Oral Mucosal Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Glossary for Narrative Writing
Periodontal Assessment and Treatment Planning Gingival description Color: o pink o erythematous o cyanotic o racial pigmentation o metallic pigmentation o uniformity Contour: o recession o clefts o enlarged papillae o cratered papillae o blunted papillae o highly rolled o bulbous o knife-edged o scalloped o stippled Consistency: o firm o edematous o hyperplastic o fibrotic Band of gingiva: o amount o quality o location o treatability Bleeding tendency: o sulcus base, lining o gingival margins Suppuration Sinus tract formation Pocket depths Pseudopockets Frena Pain Other pathology Dental Description Defective restorations: o overhangs o open contacts o poor contours Fractured cusps 1 ww.links2success.biz [email protected] 914-303-6464 Caries Deposits: o Type . plaque . calculus . stain . matera alba o Location . supragingival . subgingival o Severity . mild . moderate . severe Wear facets Percussion sensitivity Tooth vitality Attrition, erosion, abrasion Occlusal plane level Occlusion findings Furcations Mobility Fremitus Radiographic findings Film dates Crown:root ratio Amount of bone loss o horizontal; vertical o localized; generalized Root length and shape Overhangs Bulbous crowns Fenestrations Dehiscences Tooth resorption Retained root tips Impacted teeth Root proximities Tilted teeth Radiolucencies/opacities Etiologic factors Local: o plaque o calculus o overhangs 2 ww.links2success.biz [email protected] 914-303-6464 o orthodontic apparatus o open margins o open contacts o improper -

Prevalence of Oral Lesions in Complete Denture Wearers- an Original Research
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 20, Issue 1 Ser.3 (January. 2021), PP 29-33 www.iosrjournals.org Prevalence of oral lesions in complete denture wearers- An original research Prenika Sharma1*, Reecha Gupta2 1- MDS, Oral medicine and radiology 2- Professor and HOD Department of Prosthodontics, Indira Gandhi Govt. Dental College, Jammu (J&K) Abstract: Background: Complete denture patients are often associated with the various denture-related oral mucosallesions. The purpose of this study is to evaluate the prevalence ofdenture-related oral mucosal lesions in complete denture patients. Materials and Methods: The study was consisted of 225 patientshaving various denture-induced oral mucosal lesions from theoutpatient department of the department out of the 395 completedenture patients examined. Data related to gender, age, length ofdenture use, hygiene care were obtained. All the data were tabulated and analyzed. Results: In 225 complete denture patients. Denture stomatitis (60.23%) was the most commonlesion present, followed by Epulis fissuratum and angularcheilitis. The denture-induced oral mucosal lesions werefound more common in age >40 years (59.78%) and in female(52.70%) complete denture wearer patients. Conclusion: The present studies showed that oral lesions associated with wearing denture are prevalent and create health problems that impact the quality of life of dental patients. Key Words: Complete denture, denture stomatitis, Epulis fissuratum, oralmucosal lesions. --------------------------------------------------------------------------------------------------------------------------------------- Date of Submission: 26-12-2020 Date of Acceptance: 07-01-2021 --------------------------------------------------------------------------------------------------------------------------------------- I. Introduction Edentulism may be the last sequel of periodontal diseases and dental caries. In case of older adults, edentulism is essential as a correlate of self-esteem and quality of life. -

Recognition and Management of Oral Health Problems in Older Adults by Physicians: a Pilot Study
J Am Board Fam Pract: first published as 10.3122/jabfm.11.6.474 on 1 November 1998. Downloaded from BRIEF REPORTS Recognition and Management of Oral Health Problems in Older Adults by Physicians: A Pilot Study Thomas V. Jones, MD, MPH, Mitchel J Siegel, DDS, andJohn R. Schneider, A1A Oral health problems are among the most com of the nation's current and future health care mon chronic health conditions experienced by needs, the steady increase in the older adult popu older adults. Healthy People 2000, an initiative to lation, and the generally high access elderly per improve the health of America, has selected oral sons have to medical care provided by family health as a priority area. l About 11 of 100,000 physicians and internists.s,7,8 Currently there is persons have oral cancer diagnosed every year.2 very little information about the ability of family The average age at which oral cancer is diagnosed physicians or internists, such as geriatricians, to is approximately 65 years, with the incidence in assess the oral health of older patients. We con creasing from middle adulthood through the sev ducted this preliminary study to determine how enth decade of life. l-3 Even though the mortality family physicians and geriatricians compare with rate associated with oral cancer (7700 deaths an each other and with general practice dentists in nually)4 ranks among the lowest compared with their ability to recognize, diagnose, and perform other cancers, many deaths from oral cancer initial management of a wide spectrum of oral might be prevented by improved case finding and health problems seen in older adults. -

Application of Lasers in Treatment of Oral Premalignant Lesions
Symbiosis www.symbiosisonline.org www.symbiosisonlinepublishing.com Review article Journal of Dentistry, Oral Disorders & Therapy Open Access Application of Lasers in Treatment of Oral Premalignant Lesions Amaninder Singh*1, Akanksha Zutshi2, Preetkanwal Singh Ahluwalia3, Vikas Sharma4 and Vandana Razdan5 1,4oral and maxillofacial surgery, reader, National Dental College and Hospital, Dera Bassi, Punjab 2oral and maxillofacial surgery, senior lecturer, National Dental College and Hospital, Dera Bassi, Punjab 3oral and maxillofacial surgery, professor, National Dental College and Hospital, Dera Bassi, Punjab 5Pharmacology, professor, Govt. Medical College and Hospital, Jammu Received: April 03, 2018; Accepted: June 04, 2018; Published: June 11, 2018 *Corresponding author: Amaninder Singh, House No- 620, Phase- 6, mohali, 160055, E-mail address: [email protected] Abstract radiation. Laser systems and their application in dentistry and especially the basis of energy of the beam and wavelength of the emitted oral surgery are rapidly improving today. Lasers are being used as a niche tool as direct replacement for conventional approaches ClassificationGas lasers of lasers [6] CO advantages of lasers are incision of tissues, coagulation during Argon like scalpel, blades, electro surgery, dental hand piece. The specific Liquid Dyes2 canoperation be used and for treatmentpostoperative of conditions benefits likesuch lowas premalignant postoperative lesions, pain, better wound healing. For soft tissue oral surgical procedures lasers Solid -

Management of Epulis Fissuratum Using Cryosurgery - a Case Report
CASE REPORT Management of Epulis Fissuratum Using Cryosurgery - A Case Report Pradeep Sharma, Daksh Goel, Rajarshi Ghosh, Balram Garg Department of Oral and Maxillofacial Surgery, I.T.S Dental College, Ghaziabad, Uttar Pradesh, India Email for correspondence: [email protected] ABSTRACT The aim of the present case report is to present a case showing the treatment of Epulis fissuratum in relation to an ill-fitting denture treated with nitrous oxide cryosurgery. Epulis fissuratum associated with an ill-fitting denture greatly hinders mastication and produces discomfort and pain to the patient. The nitrous oxide cryosurgery can be used effectively in its management, due to its excellent hemorrhage control and post-operative healing. A 64-year- old male reported with Epulis fissuratum in the maxillary anterior vestibular sulcus, which was associated with an ill-fitting denture. Nitrous oxide cryosurgery was used for the treatment of the lesion. During the procedure, nil hemorrhage was achieved, and the post-operative healing was satisfactory. Nitrous oxide cryosurgery, hence, can be used effectively as it has the boon of achieving excellent hemostasis, good healing with minimal post-operative edema and pain, and maintaining an aseptic environment. This technique can be effectively used in the treatment of Epulis fissuratum besides it can also be used in the treatment of other oral soft tissue pathologies achieving a plethora of benefits. Key words: Epulis fissuratum, hemorrhage control, nitrous oxide cryosurgery, soft tissue lesion INTRODUCTION dentures have potential to cause oral carcinoma.[2] A poorly fitted prosthesis can give rise to a Hence, ill-fitting dentures and its sequelae should plethora of problems, notably Epulis fissuratum, not be overlooked. -

Oral Cancer in Its Early Stage, When Treatment May Be Most Effective
Clinical Showcase This month’s Clinical Showcase highlights common oral conditions that should be included in the differential diagnosis for squamous cell carcinoma or salivary gland tumours. The author sounds a cautionary note about the dangers of misdiagnosing oral lesions and reminds oral health professionals that they can detect oral cancer in its early stage, when treatment may be most effective. Clinical Showcase is a new section that features case demonstrations of clinical problems encountered in dental practice. If you would like to propose a case or recommend a clinician who could contribute to Clinical Showcase, contact editor-in-chief Dr. John O’Keefe at [email protected]. Oral Cancer John G.L. Lovas, DDS, MSc, FRCD(C) Practising dentists should concentrate on competently morbidity. Instead, radiation therapy was curative, leaving diagnosing and treating routine conditions like caries, minimal local scarring. Patients can remain completely gingivitis, periodontitis, malocclusion and tooth loss. unaware of surprisingly large intraoral lesions if the lesions However, dentists and dental hygienists are also in the best are slow-growing and asymptomatic. Unfortunately, even position to detect and diagnose relatively rare and life- when patients become aware of an intraoral lesion, they threatening oral lesions such as carcinoma. The dental team often erroneously assume that if it’s painless, it’s not danger- should therefore always maintain a high index of suspicion. ous. The patient with the mucoepidermoid carcinoma in The cases presented here highlight some of the key factors Fig. 4 had been aware of the asymptomatic swelling for essential for the early detection and most effective treat- 18 months. -

Epulis Fissuratum
Clinical Image World Journal of Oral and Maxillofacial Surgery Published: 03 Dec, 2018 Epulis Fissuratum Acevedo Ocana R1, Amez Descalzo S1, Cortes-Breton Brinkmann J2*, Delgado Gregori J1 and Sanchez Jorge MI1 1Department of Oral Surgery and Implantology, Alfonso X EI Sabio University, Spain 2Department of Oral Surgery and Implantology, Hospital Virgen de la Paloma, Spain Clinical Image A female patient aged 78 years attended the clinic pertaining to the Master’s Program in Oral Surgery, Implant Dentistry, and Periodontics at the Alfonso X Ei Sabio University (Madrid, Spain), presenting a tumor over the mandibular alveolar ridge at the midline (Figure 1). The patient did not report any family or personal antecedents of relevance. The development of the tumor appeared to be related to recent rehabilitation with implant retained overdentures retained with locator attachments (Figure 2). During intraoral exploration, a pedunculated lesion was found of fibrous consistency and whitish color with an ulcerated surface, which the patient found painful during function. It was decided to perform excisional biopsy. After obtaining informed consent from the patient, local anesthesia was applied with a supraperiosteal and perilesional infiltration technique, excision of the lesion by cold knife cone technique was performed, followed by cauterization with an electric scalpel (Figure 3 and 4). The sample was placed in a 10% formal saline for histopathological analysis. The anatomopathological report described the entity microscopically as a lesion with densely fibrous paucellular connective stroma around a vascular axis. The polypoid structure showed a covering of non-keratinized mature squamous epithelium. No signs of malignancy were observed. The pathologist’s diagnosis was of traumatic (fibroepithelial polyp) fibroma/epulis fissuratum. -
Intro to OMFS
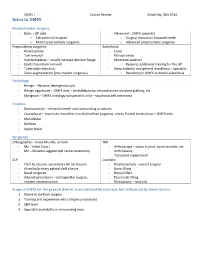
OMFS I Course Review Enoch Ng, DDS 2014 Intro to OMFS Dentoalveolar surgery - Basic – GP able - Advanced – OMFS specialist o Extraction of erupted o Surgical extraction impacted teeth o Minor preprosthetic surgeries o Advanced preprosthetic surgeries Preprosthetic surgeries Anesthesia - Alveoloplasty - Local - Tori removal - Nitrous oxide - Vestibuloplasty – usually increase denture flange - Moderate sedation - Epulis fissuratum removal o Requires additional training for the GP - Tuberosity reduction - Deep sedation and general anesthesia – specialist - Sinus augmentation (pre-implant surgeries) o Residency in OMFS or dental anesthesia Pathology - Benign – fibroma, dentigerous cyst - Benign aggressive – OMFS only – ameloblastoma, reconstruction via bone grafting, etc - Malignant – OMFS oncology subspecialist only – squamous cell carcinoma Trauma - Dentoalveolar – related to teeth and surrounding structures - Craniofacial – trauma to mandible, maxilla/midface (zygoma), orbits, frontal bones/sinus – OMFS only - Mandibular - Midface - Upper facial Surgeries Orthognathic – move Mx, Mn, or both TMJ - Mx – lefort Class I - Arthroscopy – scope in joint, inject steroids, etc - Mn – bilateral saggital split ramus osteotomy - Arthroplasty - Total joint replacement CLP Cosmetic - Cleft lip closure, secondary cleft lip closure - Blepharoplasty – eye lid surgery - Alveolar/primary palatal cleft closure - Brow lifting - Nasal surgeries - Botox/fillers - Adjunct procedures – orthognathic surgery, - Face/neck lifting implant reconstruction - Rhinoplasty -

Comparative Evaluation of SMAD-2 Expression in Oral Submucous
DOI:10.31557/APJCP.2020.21.2.399 Smad 2 Expression in Oral Submucous Fibrosis & Reactive Oral Lesions RESEARCH ARTICLE Editorial Process: Submission:06/30/2019 Acceptance:02/01/2020 Comparative Evaluation of SMAD-2 Expression in Oral Submucous Fibrosis and Reactive Oral Lesions Sravya Zagabathina1, Ramya Ramadoss1*, Harini Priya AH2, Rajkumar Krishnan1 Abstract Background: The event of fibrosis encompasses involvement of definite immunological and molecular mechanisms. As quite a lot of pro-fibrotic pathways are concerned, a multipronged approach is obligatory to cognize the fibrotic events. SMAD signaling pathway hasn’t been studied oral fibrotic events.In the progression of cramming the SMAD signaling pathway in OSMF, the first initiator protein of the pathway was considered for evaluation in the present study. Materials and Methods: A total of 100 subjects consisting of 20 controls, 40 patients with reactive lesions such as Traumatic Fibroma, Epulis Fissuratum and Gingival Hyperplasia and 40 patients with Oral Submucous Fibrosis were recruited for the study. Tissue homogenates were assayed by quantitative sandwich enzyme immunoassay technique using Human Mothers Against Decapentaplegic Homolog 2 (Smad2). Results: SMAD 2 expression values showed significant difference between control and OSMF group. However, the difference between reactive lesions with control and OSMF were not statistically significant.Conclusion: Graded increase of SMAD 2 expression from control,reactive lesions and OSMF were observed accentuating the role of SMAD signalling pathway in fibro genesis. Further this can be validated to generate effective antifibrotic targets. Keywords: SMAD- OSMF- Reactive oral lesions Asian Pac J Cancer Prev, 21 (2), 399-403 Introduction In general, the event of fibrosis encompasses involvement of definite immunological and molecular Oral sub mucous fibrosis (OSMF) is a chronic mechanisms. -

Description Concept ID Synonyms Definition
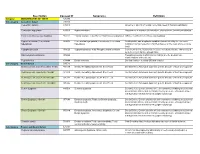
Description Concept ID Synonyms Definition Category ABNORMALITIES OF TEETH 426390 Subcategory Cementum Defect 399115 Cementum aplasia 346218 Absence or paucity of cellular cementum (seen in hypophosphatasia) Cementum hypoplasia 180000 Hypocementosis Disturbance in structure of cementum, often seen in Juvenile periodontitis Florid cemento-osseous dysplasia 958771 Familial multiple cementoma; Florid osseous dysplasia Diffuse, multifocal cementosseous dysplasia Hypercementosis (Cementation 901056 Cementation hyperplasia; Cementosis; Cementum An idiopathic, non-neoplastic condition characterized by the excessive hyperplasia) hyperplasia buildup of normal cementum (calcified tissue) on the roots of one or more teeth Hypophosphatasia 976620 Hypophosphatasia mild; Phosphoethanol-aminuria Cementum defect; Autosomal recessive hereditary disease characterized by deficiency of alkaline phosphatase Odontohypophosphatasia 976622 Hypophosphatasia in which dental findings are the predominant manifestations of the disease Pulp sclerosis 179199 Dentin sclerosis Dentinal reaction to aging OR mild irritation Subcategory Dentin Defect 515523 Dentinogenesis imperfecta (Shell Teeth) 856459 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield I 977473 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield II 976722 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; -

Oral Mucosal Lesions in a Chilean Elderly Population: a Retrospective Study with a Systematic Review from Thirteen Countries
J Clin Exp Dent. 2017;9(2):e276-83. Oral mucosal lesions in elderly people Journal section: Oral Medicine and Pathology d oi:10.4317/jced. 53427 Publication Types: Research http://dx.doi.org/10.4317/jced.53427 Oral mucosal lesions in a Chilean elderly population: A retrospective study with a systematic review from thirteen countries César Rivera 1,2, Daniel Droguett 3, María-Jesús Arenas-Márquez 4 1 Department of Basic Biomedical Sciences, Faculty of Health Sciences, University of Talca (UTALCA), Talca, Chile 2 Department of Oral Diagnosis, School of Dentistry (FOP), University of Campinas (UNICAMP), Piracicaba, São Paulo, Brazil 3 Department of Stomatology, Faculty of Health Sciences, University of Talca (UTALCA), Talca, Chile 4 Gerontology Program, Faculty of Medical Sciences, University of Campinas (UNICAMP), Campinas, São Paulo, Brazil Correspondence: Jaime Rodríguez Carvajal Building University of Talca (UTALCA) Lircay Av. S/N, Talca, Chile Zip code 3460000 [email protected] Rivera C, Droguett D, Arenas-Márquez MJ. Oral mucosal lesions in a Chilean elderly population: A retrospective study with a systematic re- view from thirteen countries. J Clin Exp Dent. 2017;9(2):e276-83. Received: 12/08/2016 http://www.medicinaoral.com/odo/volumenes/v9i2/jcedv9i2p276.pdf Accepted: 22/08/2016 Article Number: 53427 http://www.medicinaoral.com/odo/indice.htm © Medicina Oral S. L. C.I.F. B 96689336 - eISSN: 1989-5488 eMail: [email protected] Indexed in: Pubmed Pubmed Central® (PMC) Scopus DOI® System Abstract Background: The oral examination is an essential part of the multidisciplinary medical care in elderly people. Oral mucosal lesions and normal variations of oral anatomy (OMLs) are very common in this people, but few studies have examined the frequency and prevalence of these conditions worldwide and less in Chile. -

Copyrighted Material
9781405199858_1_pre.qxd 3/1/10 2:29 Page v Contents Preface vii 20 Red and purple lesions: Erythematous candidosis 36 Acute candidosis 36 1 Examination of extraoral tissues 2 Chronic candidosis 37 Head and neck 3 Denture-related stomatitis (denture sore mouth; chronic Cranial nerves 3 atrophic candidosis) 37 Limbs 3 Angular stomatitis (angular cheilitis; perleche) 37 2 Examination of mouth, jaws, temporomandibular region Median rhomboid glossitis (central papillary atrophy and salivary glands 4 of the tongue) 37 Mouth 5 21 Red and purple lesions: Angiomas 38 Jaws 5 Hemangioma 38 Temporomandibular joint (TMJ) 5 Venous lake (venous varix; senile hemangioma of lip) 38 Salivary glands 5 Lymphangioma 38 3 Investigations: Histopathology 6 22 Red and purple lesions: Proliferative vascular lesions, Mucosal biopsy 7 Kaposi sarcoma 39 Brush biopsy 7 Proliferative vascular lesions 39 Labial salivary gland biopsy 7 Kaposi sarcoma 39 4 Investigations: Microbiology 8 23 Red and purple lesions: Erythroplakia 40 5 Investigations: Imaging 10 Erythroplakia (erythroplasia) 40 6 Investigations: Blood tests 12 24 Red and purple lesions: Erythema migrans (lingual erythema Referring a patient for specialist opinion 12 migrans; benign migratory glossitis; geographical 7 Anatomical variants and developmental anomalies 14 tongue; continental tongue) 41 Fordyce spots (“Fordyce granules”) 15 25 Swellings: Hereditary conditions, drug-induced Fissured tongue (scrotal or plicated tongue) 15 swellings 42 Stafne cyst or bone cavity 15 Hereditary gingival fibromatosis (HGF)