Definition of Stroke/Brain Attack
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cory Newman Thesis 5-2021 Signed.Pdf (1.303Mb)
DocuSign Envelope ID: 4851A328-CF63-4770-A833-B4246E7E5D23 Simulating Homonymous Hemianopsia for the Care Team by Cory Newman May 2021 Presented to the Division of Science, Information Arts, and Technologies University of Baltimore In Partial Fulfillment of the Requirements for the Degree of Master of Science 5/25/2021 Approved by: ________________________________ [name, Thesis Advisor] ________________________________5/25/2021 [name, Committee Member] i DocuSign Envelope ID: 4851A328-CF63-4770-A833-B4246E7E5D23 Abstract Homonymous hemianopsia is a visual impairment that involves the bilateral loss of a complete visual field. While research has been done to ascertain the details of cause and prognosis of homonymous hemianopsia, an obvious disparity arose in the research on how to educate the supporting care team of a person with homonymous hemianopsia to maximize the creation of educational and rehabilitation plans. This research presents two studies focused on closing that gap by providing an alternative method of understanding. In the initial study 16 participants with a confirmed caregiver relationship to one or more persons with homonymous hemianopsia were surveyed on their personal knowledge of the visual impairment. These participants were asked to express any visual obstacles they have encountered, and to ascertain the availability of a device or program that could provide an interactive interpretation of how their homonymous hemianopsia patient views their surroundings. Survey results confirmed the need for a program that could easily simulate homonymous hemianopsia for the care provider. An additional usability study was completed by eight of the 16 previous participants on a mobile homonymous hemianopsia simulation application prototype. User tests showed that participants gained a significant increase in understanding of how those with a homonymous hemianopsia visual impairment view the environment. -

Cognitive Emotional Sequelae Post Stroke
11/26/2019 The Neuropsychology of Objectives 1. Identify various cognitive sequelae that may result from stroke Stroke: Cognitive & 2. Explain how stroke may impact emotional functioning, both acutely and long-term Emotional Sequelae COX HEALTH STROKE CONFERENCE BRITTANY ALLEN, PHD, ABPP, MBA 12/13/2019 Epidemiology of Stroke Stroke Statistics • > 795,000 people in the United States have a stroke • 5th leading cause of death for Americans • ~610,000 are first or new strokes • Risk of having a first stroke is nearly twice as high for blacks as whites • ~1/4 occur in people with a history of prior stroke • Blacks have the highest rate of death due to stroke • ~140,000 Americans die every year due to stroke • Death rates have declined for all races/ethnicities for decades except that Hispanics have seen • Approximately 87% of all strokes are ischemic an increase in death rates since 2013 • Costs the United States an estimated $34 billion annually • Risk for stroke increases with age, but 34% of people hospitalized for stroke were < 65 years of • Health care services age • Medicines to treat stroke • Women have a lower stroke risk until late in life when the association reverses • Missed days of work • Approximately 15% of strokes are heralded by a TIA • Leading cause of long-term disability • Reduces mobility in > 50% of stroke survivors > 65 years of age Source: Centers for Disease Control Stroke Death Rates Neuropsychological Assessment • Task Engagement • Memory • Language • Visuospatial Functioning • Attention/Concentration • Executive -

Homonymous Hemianopsia
Source: CLEVELAND CLINIC OHIO USA FACTSHEET Homonymous Hemianopsia Homonymous hemianopsia is a condition in which a person sees only one side - right or left of the visual world of each eye; results from a problem in brain function rather than a disorder of the eyes themselves. This can happen after a head or brain injury. What is homonymous hemianopsia? Homonymous hemianopsia is a condition in which a person sees only one side―right or left―of the visual world of each eye. The person may not be aware that the vision loss is happening in both eyes, not just one. Under normal circumstances, the left half of the brain processes visual information from both eyes about the right side of the world. The right side of the brain processes visual information from both eyes about the left side of the world. A visual world of someone with normal vision A visual world of someone with homonymous hemianopsia In homonymous hemianopsia, an injury to the left part of the brain results in the loss of the right half of the visual world of each eye. An injury to the right part of the brain produces loss of the left side of the visual world of each eye. This condition is created by a problem in brain function rather than a disorder of the eyes themselves. What causes homonymous hemianopsia? The most common cause of this type of vision loss is stroke. However, any disorder that affects the brain—including tumours, inflammation, and injuries--can be a cause. Source: CLEVELAND CLINIC OHIO USA It is estimated that 70% of the injuries leading to hemianopsias are due to an obstruction (blockage) of the blood supply (stroke). -

Lack of Motivation: Akinetic Mutism After Subarachnoid Haemorrhage
Netherlands Journal of Critical Care Submitted October 2015; Accepted March 2016 CASE REPORT Lack of motivation: Akinetic mutism after subarachnoid haemorrhage M.W. Herklots1, A. Oldenbeuving2, G.N. Beute3, G. Roks1, G.G. Schoonman1 Departments of 1Neurology, 2Intensive Care Medicine and 3Neurosurgery, St. Elisabeth Hospital, Tilburg, the Netherlands Correspondence M.W. Herklots - [email protected] Keywords - akinetic mutism, abulia, subarachnoid haemorrhage, cingulate cortex Abstract Akinetic mutism is a rare neurological condition characterised by One of the major threats after an aneurysmal SAH is delayed the lack of verbal and motor output in the presence of preserved cerebral ischaemia, caused by cerebral vasospasm. Cerebral alertness. It has been described in a number of neurological infarction on CT scans is seen in about 25 to 35% of patients conditions including trauma, malignancy and cerebral ischaemia. surviving the initial haemorrhage, mostly between days 4 and We present three patients with ruptured aneurysms of the 10 after the SAH. In 77% of the patients the area of cerebral anterior circulation and akinetic mutism. After treatment of the infarction corresponded with the aneurysm location. Delayed aneurysm, the patients lay immobile, mute and were unresponsive cerebral ischaemia is associated with worse functional outcome to commands or questions. However, these patients were awake and higher mortality rate.[6] and their eyes followed the movements of persons around their bed. MRI showed bilateral ischaemia of the medial frontal Cases lobes. Our case series highlights the risk of akinetic mutism in Case 1: Anterior communicating artery aneurysm patients with ruptured aneurysms of the anterior circulation. It A 28-year-old woman with an unremarkable medical history is important to recognise akinetic mutism in a patient and not to presented with a Hunt and Hess grade 3 and Fisher grade mistake it for a minimal consciousness state. -

Oct Institute
Low Vision, Visual Dysfunction and TBI – Treatment, Considerations, Adaptations Andrea Hubbard, OTD, OTR/L, LDE Objectives • In this course, participants will: 1. Learn about interventions involving specialized equipment to adapt an environment for clients with low vision. 2. Learn about the most typical low vision presentations/conditions. 3. Gain increased knowledge of eye anatomy and the visual pathway. Overview of TBI Reference: Centers for Disease Control and Prevention Overview of TBI Risk Factors for TBI Among non-fatal TBI-related injuries for 2006–2010: • Men had higher rates of TBI hospitalizations and ED visits than women. • Hospitalization rates were highest among persons aged 65 years and older. • Rates of ED visits were highest for children aged 0-4 years. • Falls were the leading cause of TBI-related ED visits for all but one age group. – Assaults were the leading cause of TBI-related ED visits for persons 15 to 24 years of age. • The leading cause of TBI-related hospitalizations varied by age: – Falls were the leading cause among children ages 0-14 and adults 45 years and older. – Motor vehicle crashes were the leading cause of hospitalizations for adolescents and persons ages 15-44 years. Reference: Centers for Disease Control and Prevention Overview of TBI Risk Factors for TBI Among TBI-related deaths in 2006–2010: • Men were nearly three times as likely to die as women. • Rates were highest for persons 65 years and older. • The leading cause of TBI-related death varied by age. – Falls were the leading cause of death for persons 65 years or older. -
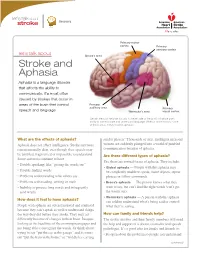
Stroke and Aphasia Aphasia Is a Language Disorder That Affects the Ability to Communicate
Recovery Primary motor cortex Primary sensory cortex let’s talk about Broca’s area Stroke and Aphasia Aphasia is a language disorder that affects the ability to communicate. It’s most often caused by strokes that occur in areas of the brain that control Primary auditory area Primary speech and language. Wernicke’s area visual cortex Certain areas of the brain (usually in the left side of the brain) influence one’s ability to communicate and understand language. When a stroke occurs in one of these areas, it may result in aphasia. What are the effects of aphasia? sender plissen.” Thousands of alert, intelligent men and Aphasia does not affect intelligence. Stroke survivors women are suddenly plunged into a world of jumbled remain mentally alert, even though their speech may communication because of aphasia. be jumbled, fragmented or impossible to understand. Are there different types of aphasia? Some survivors continue to have: Yes, there are several forms of aphasia. They include: • Trouble speaking, like “getting the words out” • Global aphasia — People with this aphasia may • Trouble finding words be completely unable to speak, name objects, repeat • Problems understanding what others say phrases or follow commands. • Problems with reading, writing or math • Broca’s aphasia — The person knows what they • Inability to process long words and infrequently want to say, but can’t find the right words (can’t get used words the words out). • Wernicke’s aphasia — A person with this aphasia How does it feel to have aphasia? can seldom understand what’s being said or control People with aphasia are often frustrated and confused what they’re saying. -

Abadie's Sign Abadie's Sign Is the Absence Or Diminution of Pain Sensation When Exerting Deep Pressure on the Achilles Tendo
A.qxd 9/29/05 04:02 PM Page 1 A Abadie’s Sign Abadie’s sign is the absence or diminution of pain sensation when exerting deep pressure on the Achilles tendon by squeezing. This is a frequent finding in the tabes dorsalis variant of neurosyphilis (i.e., with dorsal column disease). Cross References Argyll Robertson pupil Abdominal Paradox - see PARADOXICAL BREATHING Abdominal Reflexes Both superficial and deep abdominal reflexes are described, of which the superficial (cutaneous) reflexes are the more commonly tested in clinical practice. A wooden stick or pin is used to scratch the abdomi- nal wall, from the flank to the midline, parallel to the line of the der- matomal strips, in upper (supraumbilical), middle (umbilical), and lower (infraumbilical) areas. The maneuver is best performed at the end of expiration when the abdominal muscles are relaxed, since the reflexes may be lost with muscle tensing; to avoid this, patients should lie supine with their arms by their sides. Superficial abdominal reflexes are lost in a number of circum- stances: normal old age obesity after abdominal surgery after multiple pregnancies in acute abdominal disorders (Rosenbach’s sign). However, absence of all superficial abdominal reflexes may be of localizing value for corticospinal pathway damage (upper motor neu- rone lesions) above T6. Lesions at or below T10 lead to selective loss of the lower reflexes with the upper and middle reflexes intact, in which case Beevor’s sign may also be present. All abdominal reflexes are preserved with lesions below T12. Abdominal reflexes are said to be lost early in multiple sclerosis, but late in motor neurone disease, an observation of possible clinical use, particularly when differentiating the primary lateral sclerosis vari- ant of motor neurone disease from multiple sclerosis. -

VISUAL FIELD Pathway Extends from the „Front‟ to the „Back‟ of the RETINA Brain
NOTE: To change the image on this slide, select the picture and delete it. Then click the Pictures icon in the placeholde r to insert your own image. Visual Pathway Disorders Amr Hassan, MD, FEBN Associate professor of Neurology - Cairo University Optic nerve • Anatomy of visual pathway • How to examine • Visual pathway disorders • Quiz 2 Optic nerve • Anatomy of visual pathway • How to examine • Visual pathway disorders • Quiz 3 Optic nerve The Visual Pathway VISUAL FIELD Pathway extends from the „front‟ to the „back‟ of the RETINA brain. ON OC OT LGN OPTIC RADIATIONS ON = Optic Nerve OC = Optic Chiasm OT = Optic Tract LGN = Lateral Geniculate Nucleus of Thalamus VISUAL CORTEX 5 The Visual Pathway Eyes & Retina Light >> lens >> retina (inverted and reversed image). Eyes & Retina Eyes & Retina • Macula: oval region approximately 3-5 mm that surrounds the fovea, also has high visual acuity. • Fovea: central fixation point of each eye// region of the retina with highest visual acuity. Eyes & Retina • Optic disc: region where axons leaving the retina gather to form the Optic nerve. Eyes & Retina • Blind spot located 15° lateral and inferior to central fixation point of each eye. Object to be seen Peripheral Retina Central Retina (fovea in the macula lutea) 12 Photoreceptors © Stephen E. Palmer, 2002 Photoreceptors Cones • Cone-shaped • Less sensitive • Operate in high light • Color vision • Less numerous • Highly represented in the fovea >> have high spatial & temporal resolution >> they detect colors. © Stephen E. Palmer, 2002 Photoreceptors Rods • Rod-shaped • Highly sensitive • Operate at night • Gray-scale vision • More numerous than cons- 20:1, have poor spatial & temporal resolution of visual stimuli, do not detect colors >> vision in low level lighting conditions © Stephen E. -

Lacunar Stroke
Lacunar Stroke Prior to making any medical decisions, please view our disclaimer. Clinical Lacunar Syndrome Lacunar strokes tend to occur in patients with diabetes, hyperlipidemia, smoking or chronic hypertension and may be clinically silent or present as pure motor hemiparesis, pure sensory loss, or a variety of well-defined syndromes (e.g., dysarthria-clumsy hand, ataxic- hemiparesis). Descending compact white matter tracts or brainstem gray matter nuclei are injured, often producing widespread and striking initial deficits. However, the prognosis for recovery with lacunar stroke is better than with large artery territory stroke, and for this reason many centers favor using antiplatelet therapy (aspirin, clopidogrel) or conservative management rather than thrombolytic therapy for uncomplicated lacunar stroke. The risk of hemorrhagic transformation or edema in these patients is extremely low. Because initial clinical presentation may be deceiving particularly in the posterior circulation, all patients presenting with acute ischemic symptoms should undergo some form of neurovascular imaging to establish large vessel patency (CTA, MRA, ultrasound or angiography). Management Algorithm Phase 1 Additional Diagnostic Testing • Consider fasting lipids, lipoprotein (a), B12, folate, homocysteine • If suspicious of large vessel atheroma producing penetrator infarction, refer to algorithm for Large Vessel disease Prevention of Acute Recurrent Stroke • Consider antiplatelet therapy (e.g., aspirin, clopidogrel, ticlopidine, persantine, integrilin, -

• Classifications of Aphasia Expressive Vs. Receptive Fluent Vs
12/7/2018 APHASIA Aphasia is an acquired communication disorder that impairs a person’s ability to process LANGUAGE, but DOES NOT AFFECT intelligence. Aphasia impairs the ability to speak and understand others. -National Aphasia Association LANGUAGE Language is a system of communication that uses symbolism. K L U $ + M – Phonemes: perceptually distinct unit of sounds Words: sounds combined & given meaning Sentences: combination of syntax (rules) and semantics (meaning). • CLASSIFICATIONS OF APHASIA EXPRESSIVE VS. RECEPTIVE FLUENT VS. NON- FLUENT 1 12/7/2018 -NATIONAL APHASIA ASSOCIATION -COURTESY OF MY-MS.ORG MCA DISTRIBUTION -SLIDESHARE.NET 2 12/7/2018 BROCA’S APHASIA * short utterances * limited vocabulary * halting, effortful speech *mild comprehension deficits Lesion * Inferior frontal gyrus Choose Sentence Speech Coordinate Speak Idea Words Structure Sounds Articulate Pragmatics Muscles Fluently (Semantics) (Syntax) (Phonology) SAMPLE OF BROCA’S THERAPY FROM TACTUS THERAPY 3 12/7/2018 WERNICKE’S APHASIA • Comprehension is poor (auditory & reading) • Fluent, intact prosody • Logorrhea, press of speech • Neologisms, Paraphasias • Lack of awareness Lesion Temporo-Parietal, Posterior section of the superior temporal gyrus near the auditory cortex Auditory Preparation Attach Input Perception Recognition Phonological For Meaning Analysis Output WERNICKE’S APHASIA FROM TACTUS THERAPY 4 12/7/2018 GLOBAL APHASIA * severe language deficit * responds to personally relevant language * responds to non-verbal cues * some automatic speech Lesion -

Number Reading in Pure Alexiaâ
Neuropsychologia 49 (2011) 2283–2298 Contents lists available at ScienceDirect Neuropsychologia jo urnal homepage: www.elsevier.com/locate/neuropsychologia Reviews and perspectives Number reading in pure alexia—A review a,∗ b Randi Starrfelt , Marlene Behrmann a Center for Visual Cognition, Department of Psychology, Copenhagen University, O. Farimagsgade 2A, DK-1353 Copenhagen K, Denmark b Department of Psychology, Carnegie Mellon University, Pittsburgh, PA, USA a r t i c l e i n f o a b s t r a c t Article history: It is commonly assumed that number reading can be intact in patients with pure alexia, and that this Received 25 October 2010 dissociation between letter/word recognition and number reading strongly constrains theories of visual Received in revised form 31 March 2011 word processing. A truly selective deficit in letter/word processing would strongly support the hypothesis Accepted 22 April 2011 that there is a specialized system or area dedicated to the processing of written words. To date, however, Available online 4 May 2011 there has not been a systematic review of studies investigating number reading in pure alexia and so the status of this assumed dissociation is unclear. We review the literature on pure alexia from 1892 to Keywords: 2010, and find no well-documented classical dissociation between intact number reading and impaired Pure alexia letter identification in a patient with pure alexia. A few studies report strong dissociations, with number Alexia without agraphia reading less impaired than letter reading, but when we apply rigorous statistical criteria to evaluate Letter-by-letter reading Visual recognition these dissociations, the difference in performance across domains is not statistically significant. -

Journal of Neurological Disorders DOI: 10.4172/2329-6895.1000309 ISSN: 2329-6895
olog eur ica N l D f i o s l o a r n d r e u r s o J Lee, et al., J Neurol Disord 2016, 4:7 Journal of Neurological Disorders DOI: 10.4172/2329-6895.1000309 ISSN: 2329-6895 Case Report Open Access Two Cases with Cerebral Infarction in the Left Middle Frontal Lobe Presented as Gerstmann's Syndrome Eun-Ju Lee, Hye-Young Shin, Young Noh, Ki-Hyung Park, Hyeon-Mi Park, Yeong-Bae Lee, Dong-Jin Shin, Young Hee Sung and Dong Hoon Shin* Department of Neurology, Gil Hospital, Gachon University Gil Medical Center, Incheon, South Korea *Corresponding author: Dong Hoon Shin, Department of Neurology, Gil Hospital, Gachon University Gil Medical Center, South Korea, Tel: +82-32-460-3346; Fax: +83-32-460-3344; E-mail: [email protected] Rec date: Oct 08, 2016, Acc date: Oct 18, 2016, Pub date: Oct 22, 2016 Copyright: © 2016 Lee, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Gerstmann's syndrome is a neuropsychological disorder characterized by four symptoms, namely, acalculia, finger agnosia, left-right disorientation, and agraphia suggesting the presence of a lesion in the inferior parietal lobule of the dominant hemisphere, especially at the angular gyrus. Several descriptions of Gerstmann's syndrome have been reported in associated with a lesion to the left frontal lobe, but none of these reports fulfilled the full tetrad of diagnostic criteria.