Abadie's Sign Abadie's Sign Is the Absence Or Diminution of Pain Sensation When Exerting Deep Pressure on the Achilles Tendo
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Detrusor Sphincter Dyssynergia: a Review of Physiology, Diagnosis, and Treatment Strategies
Review Article Detrusor sphincter dyssynergia: a review of physiology, diagnosis, and treatment strategies John T. Stoffel Department of Urology, University of Michigan, Ann Arbor, MI, USA Correspondence to: John T. Stoffel, MD. Department of Urology, University of Michigan, Ann Arbor, MI, USA. Email: [email protected]. Abstract: Detrusor sphincter dyssynergia (DSD) is the urodynamic description of bladder outlet obstruction from detrusor muscle contraction with concomitant involuntary urethral sphincter activation. DSD is associated with neurologic conditions such as spinal cord injury, multiple sclerosis, and spina bifida and some of these neurogenic bladder patients with DSD may be at risk for autonomic dysreflexia, recurrent urinary tract infections, or upper tract compromise if the condition is not followed and treated appropriately. It is diagnosed most commonly during the voiding phase of urodynamic studies using EMG recordings and voiding cystourethrograms, although urethral pressure monitoring could also potentially be used. DSD can be sub-classified as either continuous or intermittent, although adoption of this terminology is not widespread. There are few validated oral pharmacologic treatment options for this condition but transurethral botulinum toxin injection have shown temporary efficacy in reducing bladder outlet obstruction. Urinary sphincterotomy has also demonstrated reproducible long term benefits in several studies, but the morbidity associated with this procedure can be high. Keywords: Detrusor sphincter dyssynergia (DSD); neurogenic bladder; urodynamics; external urinary sphincter (EUS) Submitted Nov 30, 2015. Accepted for publication Jan 05, 2016. doi: 10.3978/j.issn.2223-4683.2016.01.08 View this article at: http://dx.doi.org/10.3978/j.issn.2223-4683.2016.01.08 Introduction Physiology The human bladder has two functions—to store and During storage of urine, afferent nerves carry information empty urine. -

Acute Cerebellar Ataxia Associated with Intermittent ECG Pattern Similar to Wellens Syndrome and Transient Prominent QRS Anterior Forces
Acute cerebellar ataxia associated with intermittent ECG pattern similar to Wellens syndrome and transient prominent QRS anterior forces Andrés Ricardo Pérez-Riera, MD, PhD. Post-Graduates Advisor at Design of Studies and Scientific Writing Laboratory in the ABC Faculty of Medicine - ABC Foundation - Santo André – São Paulo – Brazil Raimundo Barbosa-Barros, MD. Specialist in Cardiology by the Brazilian Society of Cardiology (SBC) Specialist in Intensive Care by the Sociedade Brasileira de Terapia Intensiva Chief of the Coronary Center of the Hospital de Messejana Dr. Carlos Alberto Studart Gomes. Fortaleza - Brazil Adrian Baranchuk, MD FACC FRCPC Associate Professor of Medicine and Physiology - Cardiac Electrophysiology and Pacing - Director, EP Training Program - Kingston General Hospital - FAPC 3, 76 Stuart Street K7L 2V7, Kingston ON Queen's University - Canada Male patient, 56 years old, white, uncontrolled hypertension, was admitted to our emergency department (ED) with reports of sudden dizziness, headache of abrupt onset, nausea, vomiting and weakness in the lower limbs. Physical examination drew attention to the presence of manifestations suggestive of cerebellar syndrome: impaired coordination in the trunk or arms and legs, inability to coordinate balance, gait, extremity, uncontrolled or repetitive eye movements, (nystagmus), dyssynergia, dysmetria, dysdiadochokinesia, dysarthria (cerebellar ataxia). Normal myocardial necrosis markers and normal electrolytes ECO 1: anteroseptal-apical akinesis; LVEF = 30% ECO 2 (third day): -

Cognitive Emotional Sequelae Post Stroke
11/26/2019 The Neuropsychology of Objectives 1. Identify various cognitive sequelae that may result from stroke Stroke: Cognitive & 2. Explain how stroke may impact emotional functioning, both acutely and long-term Emotional Sequelae COX HEALTH STROKE CONFERENCE BRITTANY ALLEN, PHD, ABPP, MBA 12/13/2019 Epidemiology of Stroke Stroke Statistics • > 795,000 people in the United States have a stroke • 5th leading cause of death for Americans • ~610,000 are first or new strokes • Risk of having a first stroke is nearly twice as high for blacks as whites • ~1/4 occur in people with a history of prior stroke • Blacks have the highest rate of death due to stroke • ~140,000 Americans die every year due to stroke • Death rates have declined for all races/ethnicities for decades except that Hispanics have seen • Approximately 87% of all strokes are ischemic an increase in death rates since 2013 • Costs the United States an estimated $34 billion annually • Risk for stroke increases with age, but 34% of people hospitalized for stroke were < 65 years of • Health care services age • Medicines to treat stroke • Women have a lower stroke risk until late in life when the association reverses • Missed days of work • Approximately 15% of strokes are heralded by a TIA • Leading cause of long-term disability • Reduces mobility in > 50% of stroke survivors > 65 years of age Source: Centers for Disease Control Stroke Death Rates Neuropsychological Assessment • Task Engagement • Memory • Language • Visuospatial Functioning • Attention/Concentration • Executive -

Lack of Motivation: Akinetic Mutism After Subarachnoid Haemorrhage
Netherlands Journal of Critical Care Submitted October 2015; Accepted March 2016 CASE REPORT Lack of motivation: Akinetic mutism after subarachnoid haemorrhage M.W. Herklots1, A. Oldenbeuving2, G.N. Beute3, G. Roks1, G.G. Schoonman1 Departments of 1Neurology, 2Intensive Care Medicine and 3Neurosurgery, St. Elisabeth Hospital, Tilburg, the Netherlands Correspondence M.W. Herklots - [email protected] Keywords - akinetic mutism, abulia, subarachnoid haemorrhage, cingulate cortex Abstract Akinetic mutism is a rare neurological condition characterised by One of the major threats after an aneurysmal SAH is delayed the lack of verbal and motor output in the presence of preserved cerebral ischaemia, caused by cerebral vasospasm. Cerebral alertness. It has been described in a number of neurological infarction on CT scans is seen in about 25 to 35% of patients conditions including trauma, malignancy and cerebral ischaemia. surviving the initial haemorrhage, mostly between days 4 and We present three patients with ruptured aneurysms of the 10 after the SAH. In 77% of the patients the area of cerebral anterior circulation and akinetic mutism. After treatment of the infarction corresponded with the aneurysm location. Delayed aneurysm, the patients lay immobile, mute and were unresponsive cerebral ischaemia is associated with worse functional outcome to commands or questions. However, these patients were awake and higher mortality rate.[6] and their eyes followed the movements of persons around their bed. MRI showed bilateral ischaemia of the medial frontal Cases lobes. Our case series highlights the risk of akinetic mutism in Case 1: Anterior communicating artery aneurysm patients with ruptured aneurysms of the anterior circulation. It A 28-year-old woman with an unremarkable medical history is important to recognise akinetic mutism in a patient and not to presented with a Hunt and Hess grade 3 and Fisher grade mistake it for a minimal consciousness state. -

Foreign Accent Syndrome, a Rare Presentation of Schizophrenia in a 34-Year-Old African American Female: a Case Report and Literature Review
Hindawi Publishing Corporation Case Reports in Psychiatry Volume 2016, Article ID 8073572, 5 pages http://dx.doi.org/10.1155/2016/8073572 Case Report Foreign Accent Syndrome, a Rare Presentation of Schizophrenia in a 34-Year-Old African American Female: A Case Report and Literature Review Kenneth Asogwa,1 Carolina Nisenoff,1 and Jerome Okudo2 1 Richmond University Medical Center, 355 Bard Avenue, Staten Island, NY 10310, USA 2University of Texas School of Public Health, 1200 Pressler Street, Houston, TX 77030, USA Correspondence should be addressed to Jerome Okudo; [email protected] Received 17 October 2015; Revised 14 December 2015; Accepted 29 December 2015 AcademicEditor:ErikJonsson¨ Copyright © 2016 Kenneth Asogwa et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Foreign Accent Syndrome (FAS) is a rare phenomenon where speech is characterized by a new accent to the patient’snative language. More than 100 cases with the syndrome have been published, the majority of which were associated with observed insults of the speech center. Some other cases have been described without identifiable organic brain injury, especially in patients with psychiatric illness. This paper presents a patient with schizophrenia and FAS, without any evidence of organic brain injury. FAS recurred during psychotic exacerbation and did not reverse before transfer to a long-term psychiatric facility. The case is discussed in the context of a brief review of the syndrome. 1. Introduction had a history of paranoid schizophrenia. The patient was brought to the psychiatry emergency room by ambulance Foreign Accent Syndrome (FAS) is a rare condition where for evaluation of aggression. -
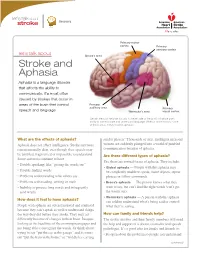
Stroke and Aphasia Aphasia Is a Language Disorder That Affects the Ability to Communicate
Recovery Primary motor cortex Primary sensory cortex let’s talk about Broca’s area Stroke and Aphasia Aphasia is a language disorder that affects the ability to communicate. It’s most often caused by strokes that occur in areas of the brain that control Primary auditory area Primary speech and language. Wernicke’s area visual cortex Certain areas of the brain (usually in the left side of the brain) influence one’s ability to communicate and understand language. When a stroke occurs in one of these areas, it may result in aphasia. What are the effects of aphasia? sender plissen.” Thousands of alert, intelligent men and Aphasia does not affect intelligence. Stroke survivors women are suddenly plunged into a world of jumbled remain mentally alert, even though their speech may communication because of aphasia. be jumbled, fragmented or impossible to understand. Are there different types of aphasia? Some survivors continue to have: Yes, there are several forms of aphasia. They include: • Trouble speaking, like “getting the words out” • Global aphasia — People with this aphasia may • Trouble finding words be completely unable to speak, name objects, repeat • Problems understanding what others say phrases or follow commands. • Problems with reading, writing or math • Broca’s aphasia — The person knows what they • Inability to process long words and infrequently want to say, but can’t find the right words (can’t get used words the words out). • Wernicke’s aphasia — A person with this aphasia How does it feel to have aphasia? can seldom understand what’s being said or control People with aphasia are often frustrated and confused what they’re saying. -

Second Edition
COVID-19 Evidence Update COVID-19 Update from SAHMRI, Health Translation SA and the Commission on Excellence and Innovation in Health Updated 4 May 2020 – 2nd Edition “What is the prevalence, positive predictive value, negative predictive value, sensitivity and specificity of anosmia in the diagnosis of COVID-19?” Executive Summary There is widespread reporting of a potential link between anosmia (loss of smell) and ageusia (loss of taste) and SARS-COV-2 infection, as an early sign and with sudden onset predominantly without nasal obstruction. There are calls for anosmia and ageusia to be recognised as symptoms for COVID-19. Since the 1st edition of this briefing (25 March 2020), there has been a significant expansion of literature on this topic, including 3 systematic reviews. Predictive value: The reported prevalence of anosmia/hyposmia and ageusia/hypogeusia in SARS-COV-2 positive patients are in the order of 36-68% and 33-71% respectively. There are reports of anosmia as the first symptom in some patients. Estimates from one study for hyposmia and hypogeusia: • Positive likelihood ratios: 4.5 and 5.8 • Sensitivity: 46% and 62% • Specificity: 90% and 89% The US Centres for Disease Control and Prevention (CDC) has added new loss or taste or smell to its list of recognised symptoms for SARS-COV-2 infection. To date, the World Health Organization has not. Conclusion: There is sufficient evidence to warrant adding loss of taste and smell to the list of symptoms for COVID-19 and promoting this information to the public. Context • Early detection of COVID-19 is key to the ongoing management of the pandemic. -

Spinocerebellar Ataxia Type 29 Due to Mutations in ITPR1: a Case Series and Review of This Emerging Congenital Ataxia Jessica L
Zambonin et al. Orphanet Journal of Rare Diseases (2017) 12:121 DOI 10.1186/s13023-017-0672-7 RESEARCH Open Access Spinocerebellar ataxia type 29 due to mutations in ITPR1: a case series and review of this emerging congenital ataxia Jessica L. Zambonin1*, Allison Bellomo2, Hilla Ben-Pazi3, David B. Everman2, Lee M. Frazer2, Michael T. Geraghty4, Amy D. Harper5, Julie R. Jones2, Benjamin Kamien6, Kristin Kernohan1,4, Mary Kay Koenig7, Matthew Lines4, Elizabeth Emma Palmer8,9, Randal Richardson10, Reeval Segel11, Mark Tarnopolsky12, Jason R. Vanstone4, Melissa Gibbons13, Abigail Collins14, Brent L. Fogel15, Care4Rare Canada Consortium, Tracy Dudding-Byth16 and Kym M. Boycott1,4 Abstract Background: Spinocerebellar ataxia type 29 (SCA29) is an autosomal dominant, non-progressive cerebellar ataxia characterized by infantile-onset hypotonia, gross motor delay and cognitive impairment. Affected individuals exhibit cerebellar dysfunction and often have cerebellar atrophy on neuroimaging. Recently, missense mutations in ITPR1 were determined to be responsible. Results: Clinical information on 21 individuals from 15 unrelated families with ITPR1 mutations was retrospectively collected using standardized questionnaires, including 11 previously unreported singletons and 2 new patients from a previously reported family. We describe the genetic, clinical and neuroimaging features of these patients to further characterize the clinical features of this rare condition and assess for any genotype-phenotype correlation for this disorder. Our cohort consisted of 9 males and 12 females, with ages ranging from 28 months to 49 years. Disease course was non-progressive with infantile-onset hypotonia and delays in motor and speech development. Gait ataxia was present in all individuals and 10 (48%) were not ambulating independently between the ages of 3–12 years of age. -

Conduction Aphasia, Sensory-Motor Integration, and Phonological Short-Term Memory – an Aggregate Analysis of Lesion and Fmri Data ⇑ Bradley R
Brain & Language 119 (2011) 119–128 Contents lists available at ScienceDirect Brain & Language journal homepage: www.elsevier.com/locate/b&l Conduction aphasia, sensory-motor integration, and phonological short-term memory – An aggregate analysis of lesion and fMRI data ⇑ Bradley R. Buchsbaum a, , Juliana Baldo b, Kayoko Okada d, Karen F. Berman e, Nina Dronkers b, ⇑ Mark D’Esposito c, Gregory Hickok d, a Rotman Research Institute, Toronto, Ontario, Canada b VA Northern California Health Care System, Center for Aphasia and Related Disorders, Martinez, CA, USA c Department of Psychology, University of California, Berkeley, CA, USA d Department of Cognitive Sciences, University of California, Irvine, CA, USA e Section on Integrative Neuroimaging, National Institute of Mental Health, Bethesda, MD, USA article info abstract Article history: Conduction aphasia is a language disorder characterized by frequent speech errors, impaired verbatim Accepted 11 December 2010 repetition, a deficit in phonological short-term memory, and naming difficulties in the presence of other- Available online 21 January 2011 wise fluent and grammatical speech output. While traditional models of conduction aphasia have typi- cally implicated white matter pathways, recent advances in lesions reconstruction methodology Keywords: applied to groups of patients have implicated left temporoparietal zones. Parallel work using functional Conduction aphasia magnetic resonance imaging (fMRI) has pinpointed a region in the posterior most portion of the left pla- Working memory num temporale, area Spt, which is critical for phonological working memory. Here we show that the Speech production region of maximal lesion overlap in a sample of 14 patients with conduction aphasia perfectly circum- Planum temporale Brain lesion scribes area Spt, as defined in an aggregate fMRI analysis of 105 subjects performing a phonological work- Sensorimotor integration ing memory task. -

Unifying the Motor & Non-Motor Features of Parkinson's Disease
Unifying the Motor & Non-motor Features of Parkinson’s Disease Ali Shalash Professor of Neurology Chair of Ain Shams Movement Disorders Group Department of Neurology, Ain Shams Univeristy Cairo, Egypt AGENDA 1. Motor and non-motor Symptoms 2. Pathophysiology of Motor & NMS 3. Relation To Disease Course 4. NMS in motor subtypes 5. Motor & NMS fluctuation 6. Treatment of Motor & NMS: links Parkinson’s Disease • PD prevalence 1 % of populations older than 65 years (Abbas et al., 2018) • From 1990 to 2015, the number of with PD patients doubled to over 6 million, and double again to over 12 million by 2040 (Dorsey et al, 2018) • Aging populations, increasing longevity, decreasing smoking rates, and the by- products of industrialization MDS Clinical Diagnostic Criteria for PD Postuma et al 2015 MDS Clinical Diagnostic Criteria for PD Postuma et al 2015 Non-motor Symptoms of PD • Neuropsychiatric symptoms • Autonomic dysfunction • Depression up to 50-70 % • Drooling • Anxiety up to 60 % • Orthostatic hypotension 30–58% • Apathy 60 % • Urinary dysfunction • Psychosis up to 40% • Erectile dysfunction • Impulse control and related disorders • Gastrointestinal dysfunction 25–67% • Dementia, 24% to 40%. • Excessive sweating • Cognitive impairment 20-25% (other • Others than dementia mainly mild cognitive impairment) • Pain 30–85% • Fatigue 50% • Disorders of sleep and wakefulness • Olfactory dysfunction 90% • • Sleep fragmentation and insomnia Ophthalmologic dysfunction • Rapid eye movement sleep behavior disorder 65 % • Excessive daytime sleepiness Pathophysiology of Motor & NMS Neuropathology of PD: Motor Symptoms Two major pathologic processes: (a) premature selective loss of dopamine neurons: 30–70% cell loss ⇢ motor symptoms. (b) the accumulation of Lewy bodies, composed of α-synuclein Poewe, W. -

Dissociation Between Awareness and Spatial Coding: Evidence from Unilateral Neglect
Dissociation between Awareness and Spatial Coding: Evidence from Unilateral Neglect Barbara Treccani1, Roberto Cubelli1, Roberta Sellaro1, Carlo Umiltà2, and Sergio Della Sala3 Downloaded from http://mitprc.silverchair.com/jocn/article-pdf/24/4/854/1777452/jocn_a_00185.pdf by MIT Libraries user on 17 May 2021 Abstract ■ Prevalent theories about consciousness propose a causal re- dissociate. A patient with left neglect, who was not aware of lation between lack of spatial coding and absence of conscious contralesional stimuli, was able to process their color and po- experience: The failure to code the position of an object is sition. However, in contrast to (ipsilesional) consciously per- assumed to prevent this object from entering consciousness. ceived stimuli, color and position of neglected stimuli were This is consistent with influential theories of unilateral neglect processed separately. We propose that individual object fea- following brain damage, according to which spatial coding of tures, including position, can be processed without attention neglected stimuli is defective, and this would keep their process- and consciousness and that conscious perception of an ob- ing at the nonconscious level. Contrary to this view, we report ject depends on the binding of its features into an integrated evidence showing that spatial coding and consciousness can percept. ■ INTRODUCTION the effects of processing of neglected stimuli on responses Awareness of a stimulus can be defined as the explicit to stimuli presented in the intact hemispace. Properties knowledge of its physical and semantic properties or sim- that can be processed implicitly include color and shape, ply of its existence. This knowledge can be demonstrated identity of alphanumerical symbols, and even the mean- by direct reports of the perception of the stimulus; for ing of words and pictures (Della Sala, van der Meulen, example, by naming it, categorizing it, or just by signaling Bestelmeyer, & Logie, 2010; Làdavas, Paladini, & Cubelli, its presence. -

Correlation of CT Cerebral Vascular Territories with Function: 3. Middle Cerebral Artery
161 Correlation of CT Cerebral Vascular Territories with Function: 3. Middle Cerebral Artery Stephen A. Berman 1 Schematic displays are presented of the cerebral territories supplied by branches of L. Anne Hayman2 the middle cerebral artery as they would appear on axial and coronal computed Vincent C. Hinck 1 tomographic (CT) scan sections. Companion diagrams of regional cortical function and a discussion of the fiber tracts are provided to simplify correlation of clinical deficits with coronal and axial CT abnormalities. This report is the third in a series designed to correlate cerebral vascular territories and functional anatomy in a form directly applicable to computed tomog raphy (CT). The illustrations are intended to simplify analysis of CT images in terms of clinical signs and symptoms and vascular territories in everyday practice. The anterior and posterior cerebral arteries have been described [1 , 2] . This report deals with the middle cerebral arterial territory. Knowledge of cerebral vascular territories can help in differentiating between infarction and other pathologic processes. For example, if the position and extent of a lesion and the usual position and extent of a vascular territory are incongruous, infarction should receive relatively low diagnostic priority and vice versa. Knowledge of vascular territories can also facilitate correct interpretation of cerebral angio grams by pinpointing specific vessels for particularly close attention. Knowledge of functional neuroanatomy applied to a patient's clinical findings can improve detection of subtle lesions by pinpointing specific areas for special attention on CT and specific vessels for attention on angiograms. Discussion The largest area of the brain that is normally supplied by the vessel(s) of the middle cerebral territory is indicated in figures 1 and 2.