Benign Tumors and Tumor-Like Lesions of the Vulva
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Skin and Breast Disease in the Differential Diagnosis of Chest Pain
Skin and breast disease in the differential diagnosis of chest pain Author Muir, Jim, Yelland, Michael Published 2010 Journal Title Medical Clinics of North America DOI https://doi.org/10.1016/j.mcna.2010.01.006 Copyright Statement © 2010 Elsevier. This is the author-manuscript version of this paper. Reproduced in accordance with the copyright policy of the publisher. Please refer to the journal's website for access to the definitive, published version. Downloaded from http://hdl.handle.net/10072/33712 Griffith Research Online https://research-repository.griffith.edu.au ARTICLE IN PRESS 1 2 Skin and Breast 3 4 Disease in the 5 6 Differential 7 8 Diagnosis of 9 10 Chest Pain 11 12 a, b ½Q2½ Q3 Jim Muir *, Michael Yelland ½Q4½ Q5 KEYWORDS 13 14 Chest pain Skin diseases Herpes zoster PROOF 15 Breast Neoplasm 16 17 18 Pain is not a symptom commonly associated with skin disease. This is especially so 19 when considering the known skin problems that have a presenting symptom of chest 20 pain that could potentially be confused with chest pain from other causes. 21 22 PAINFUL SKIN CONDITIONS 23 24 Several extremely painful and tender skin conditions present with dramatic clinical 25 signs. Inflammatory disorders such as pyoderma gangrenosum, skin malignancies, 26 both primary and secondary, acute bacterial infections such as erysipelas or cellulitis, 27 and multiple other infections are commonly extremely painful and tender. As these 28 conditions manifest with obvious skin signs such as swelling, erythema, localized 29 tenderness, fever, lymphangitis, and lymphadenopathy, there is little chance of misdi- 30 agnosis of symptoms as caused by anything other than a cutaneous pathology. -

Large Clitoridal Inclusion Cyst Following Female Genital Mutilation
Case Report 2020 iMedPub Journals Gynaecology & Obstetrics Case report www.imedpub.com ISSN 2471-8165 Vol.6 No.1:6 DOI: 10.36648/2471-8165.6.1.87 Large Clitoridal Inclusion Cyst Orisabinone IB and Oriji PC* Following Female Department of Obstetrics and Gynaecology, Federal Medical Centre, Genital Mutilation/Cutting - A Case Report Yenagoa, Bayelsa State, Nigeria Abstract *Corresponding author: Dr. Oriji PC Introduction: Epithelial inclusion cyst is a common type of cutaneous cyst that results from implantation of epidermal elements in the dermis and can occur throughout the body. It is often seen in the perineum and posterior [email protected] vaginal wall, and lined by stratified squamous epithelium. This desquamates and produces secretions to form a cystic mass. This is called clitoridal inclusion cyst when it involves the clitoris. It is usually a complication of Department of Obstetrics and female genital mutilation/ cutting. Gynaecology, Federal Medical Centre, Case presentation: She was a 27-year-old young woman, who presented to Yenagoa, Bayelsa State, Nigeria. the gynaecological clinic with a 15-year history of progressive swelling in her perineum. She was circumcised at the age of 10 years. She had surgical excision Tel: +234 803 067 7372 under anaesthesia, and was discharged home in good health condition. Conclusion: Evaluation of clitoridal inclusion cyst requires careful assessment by a good history, detailed physical examination and necessary imaging modality, Citation: Orisabinone IB, Oriji PC as this will help to rule out differential diagnosis and manage the patient better. (2020) Clitoridal Inclusion Cyst Following Female Genital Keywords: Clitoridal inclusion cyst; Female genital mutilation/cutting; Mutilation/Cutting - A Case Report. -
Detail Report
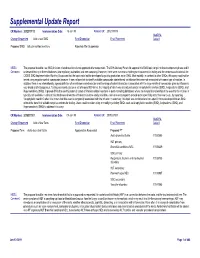
Supplemental Update Report CR Number: 2012319113 Implementation Date: 16-Jan-19 Related CR: 2012319113 MedDRA Change Requested Add a new SMQ Final Disposition Final Placement Code # Proposed SMQ Infusion related reactions Rejected After Suspension MSSO The proposal to add a new SMQ Infusion related reactions is not approved after suspension. The ICH Advisory Panel did approve this SMQ topic to go into the development phase and it Comment: underwent testing in three databases (two regulatory authorities and one company). However, there were numerous challenges encountered in testing and the consensus decision of the CIOMS SMQ Implementation Working Group was that the topic could not be developed to go into production as an SMQ. Most notably, in contrast to other SMQs, this query could not be tested using negative control compounds because it was not possible to identify suitable compounds administered via infusion that were not associated with some type of reaction. In addition, there is no internationally agreed definition of an infusion related reaction and the range of potential reactions associated with the large variety of compounds given by infusion is very broad and heterogenous. Testing was conducted on a set of around 500 terms, the majority of which was already included in Anaphylactic reaction (SMQ), Angioedema (SMQ), and Hypersensitivity (SMQ). It proved difficult to identify potential cases of infusion related reactions in post-marketing databases where the temporal relationship of the event to the infusion is typically not available. In clinical trial databases where this information is more easily available, users are encouraged to provide more specificity about the event, e.g., by reporting “Anaphylactic reaction” when it is known that this event is temporally associated with the infusion. -

A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated Through 445 Nm Diode Laser
healthcare Case Report A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated through 445 nm Diode Laser Maria Vittoria Viani 1,*, Luigi Corcione 1, Chiara Di Blasio 2, Ronell Bologna-Molina 3 , Paolo Vescovi 1 and Marco Meleti 1 1 Department of Medicine and Surgery, University of Parma, 43126 Parma, Italy; [email protected] (L.C.); [email protected] (P.V.); [email protected] (M.M.) 2 Private practice, Centro Medico Di Blasio, 43121 Parma; Italy; [email protected] 3 Faculty of Dentistry, University of the Republic, 14600 Montevideo, Uruguay; [email protected] * Correspondence: [email protected] Received: 10 June 2020; Accepted: 11 August 2020; Published: 13 August 2020 Abstract: Oral granular cell tumor (GCT) is a relatively rare, benign lesion that can easily be misdiagnosed. Particularly, the presence of pseudoepitheliomatous hyperplasia might, in some cases, lead to the hypothesis of squamous cell carcinoma. Surgical excision is the treatment of choice. Recurrence has been reported in up to 15% of cases treated with conventional surgery. Here, we reported a case of GCT of the tongue in a young female patient, which was successfully treated through 445 nm diode laser excision. Laser surgery might reduce bleeding and postoperative pain and may be associated with more rapid healing. Particularly, the vaporization effect on remnant tissues could eliminate GCT cells on the surgical bed, thus hypothetically leading to a lower rate of recurrence. In the present case, complete healing occurred in 1 week, and no recurrence was observed after 6 months. Laser surgery also allows the possibility to obtain second intention healing. -

Atypical Fibroids
Hereditary leiomyomatosis and renal cell cancer: Cutaneous lesions & atypical fibroids The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Bortoletto, Pietro, Jennifer L. Lindsey, Liping Yuan, Bradley J. Quade, Antonio R. Gargiulo, Cynthia C. Morton, Elizabeth A. Stewart, and Raymond M. Anchan. 2017. “Hereditary leiomyomatosis and renal cell cancer: Cutaneous lesions & atypical fibroids.” Case Reports in Women's Health 15 (1): 31-34. doi:10.1016/ j.crwh.2017.06.004. http://dx.doi.org/10.1016/j.crwh.2017.06.004. Published Version doi:10.1016/j.crwh.2017.06.004 Citable link http://nrs.harvard.edu/urn-3:HUL.InstRepos:35982080 Terms of Use This article was downloaded from Harvard University’s DASH repository, and is made available under the terms and conditions applicable to Other Posted Material, as set forth at http:// nrs.harvard.edu/urn-3:HUL.InstRepos:dash.current.terms-of- use#LAA Case Reports in Women's Health 15 (2017) 31–34 Contents lists available at ScienceDirect Case Reports in Women's Health journal homepage: www.elsevier.com/locate/crwh Hereditary leiomyomatosis and renal cell cancer: Cutaneous MARK lesions & atypical fibroids Pietro Bortolettoa,b,c,1, Jennifer L. Lindseya,b,1, Liping Yuand, Bradley J. Quadec,d, Antonio R. Gargiuloa,b,c, Cynthia C. Mortonb,c,d,e,f, Elizabeth A. Stewartg, ⁎ Raymond M. Anchana,b,c, a Division of Reproductive Endocrinology and Infertility, Boston, MA, USA b Department of Obstetrics, Gynecology and Reproductive Biology, -
Study to Evaluate the Safety and Effectiveness of Zostavax™ in Subjects 50 - 59 Years of Age (V211-022) - Full Text View - Clinicaltrials.Gov
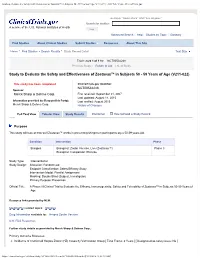
Study to Evaluate the Safety and Effectiveness of Zostavax™ in Subjects 50 - 59 Years of Age (V211-022) - Full Text View - ClinicalTrials.gov Example: "Heart attack" AND "Los Angeles" Search for studies: A service of the U.S. National Institutes of Health Advanced Search Help Studies by Topic Glossary Find Studies About Clinical Studies Submit Studies Resources About This Site Home Find Studies Search Results Study Record Detail Text Size Trial record 1 of 1 for: NCT00534248 Previous Study | Return to List | Next Study Study to Evaluate the Safety and Effectiveness of Zostavax™ in Subjects 50 - 59 Years of Age (V211-022) This study has been completed. ClinicalTrials.gov Identifier: NCT00534248 Sponsor: Merck Sharp & Dohme Corp. First received: September 21, 2007 Last updated: August 11, 2015 Information provided by (Responsible Party): Last verified: August 2015 Merck Sharp & Dohme Corp. History of Changes Full Text View Tabular View Study Results Disclaimer How to Read a Study Record Purpose This study will look at how well Zostavax™ works in preventing shingles in participants ages 50-59 years old. Condition Intervention Phase Shingles Biological: Zoster Vaccine, Live (Zostavax™) Phase 3 Biological: Comparator: Placebo Study Type: Interventional Study Design: Allocation: Randomized Endpoint Classification: Safety/Efficacy Study Intervention Model: Parallel Assignment Masking: Double Blind (Subject, Investigator) Primary Purpose: Prevention Official Title: A Phase III Clinical Trial to Evaluate the Efficacy, Immunogenicity, Safety and -

Surgical Excision of Eyelid Lesions Reference Number: CP.VP.75 Coding Implications Last Review Date: 12/2020 Revision Log
Clinical Policy: Surgical Excision of Eyelid Lesions Reference Number: CP.VP.75 Coding Implications Last Review Date: 12/2020 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description: The majority of eyelid lesions are benign, ranging from innocuous cysts and chalazion/hordeolum to nevi and papillomas. Key features that should prompt further investigation include gradual enlargement, central ulceration or induration, irregular borders, eyelid margin destruction or loss of lashes, and telangiectasia. This policy describes the medical necessity requirements for surgical excision of eyelid lesions. Policy/Criteria I. It is the policy of health plans affiliated with Centene Corporation® (Centene) that surgical excision and repair of eyelid or conjunctiva due to lesion or cyst or eyelid foreign body removal is medically necessary for any of the following indications: A. Lesion with one or more of the following characteristics: 1. Bleeding; 2. Persistent or intense itching; 3. Pain; 4. Inflammation; 5. Restricts vision or eyelid function; 6. Misdirects eyelashes or eyelid; 7. Displaces lacrimal puncta or interferes with tear flow; 8. Touches globe; 9. Unknown etiology with potential for malignancy; B. Lesions classified as one of the following: 1. Malignant; 2. Benign; 3. Cutaneous papilloma; 4. Cysts; 5. Embedded foreign bodies; C. Periocular warts associated with chronic conjunctivitis. Background The majority of eyelid lesions are benign, ranging from innocuous cysts and chalazion/hordeolum to nevi and papillomas. Key features that should prompt further investigation include gradual enlargement, central ulceration or induration, irregular borders, eyelid margin destruction or loss of lashes, and telangiectasia. Benign tumors, even though benign, often require removal and therefore must be examined carefully and the differential diagnosis of a malignant eyelid tumor considered and the method of removal planned. -

Cutaneous Melanoma Metastasizing to Leiomyoma Uteri
CASE REPORT Tumour-to-tumour Metastasis: Cutaneous Melanoma Metastasizing to Leiomyoma Uteri Jelena Amidzic1, Nenad Solajic2, Aleksandra Fejsa Levakov1, Matilda Djolai1 and Nada Vuckovic2 1Department for Histology and Embryology / Pathology2, Centre for Pathology and Histology, Clinical Centre of Vojvodina, Faculty of Medicine, University of Novi Sad, HajdukVeljkova 1-3, 21000 Novi Sad, Serbia ABSTRACT The incidence of melanoma is increasing worldwide. It is known that melanoma frequently progresses to metastatic disease. The aim of this report is to emphasise the metastatic potential of cutaneous melanoma to various body areas, as well as the ability to produce unexpected presentation of the disease. A 48-year female had a myomatous uterus and underwent hysterectomy. At the pathological examination, multiple leiomyomas were diagnosed and in one of them, the metastatic melanoma was found, the later confirmed with immunohistochemical analysis. The medical history revealed that the patient was previously operated two years back due to skin superficial spreading melanoma. The metastasis to uterine leiomyoma was the first site of distant spread. Melanoma is a type of tumour with aggressive and unpredictable behaviour, so metastases to unexpected localisations could occur. A careful examination of patient's body is mandatory, including the remote areas and even benign tumours. Key Words: Tumout-to-tumour metastasis, Melanoma, Leiomyoma. How to cite this article: Amidzic J, Solajic N, Fejsa Levakov A, Djolai M, Vuckovic N. Tumour-to-tumour metastasis: cutaneous melanoma metastasizing to leiomyoma uteri. J Coll Physicians Surg Pak 2019; 29 (Supplement 2):S112-S113. INTRODUCTION Recognised by T-cells (MART1) and polyclonal or 2 Melanoma is an aggressive, highly malignant disease monoclonal S100 protein. -

Inherited Skin Tumour Syndromes
CME GENETICS Clinical Medicine 2017 Vol 17, No 6: 562–7 I n h e r i t e d s k i n t u m o u r s y n d r o m e s A u t h o r s : S a r a h B r o w n , A P a u l B r e n n a n B a n d N e i l R a j a n C This article provides an overview of selected genetic skin con- and upper trunk. 1,2 These lesions are fibrofolliculomas, ditions where multiple inherited cutaneous tumours are a cen- trichodiscomas and acrochordons. Patients are also susceptible tral feature. Skin tumours that arise from skin structures such to the development of renal cell carcinoma, lung cysts and as hair, sweat glands and sebaceous glands are called skin pneumothoraces. 3 appendage tumours. These tumours are uncommon, but can Fibrofolliculomas and trichodiscomas clinically present as ABSTRACT have important implications for patient care. Certain appenda- skin/yellow-white coloured dome shaped papules 2–4 mm in geal tumours, particularly when multiple lesions are seen, may diameter (Fig 1 a and Fig 1 b). 4 These lesions usually develop indicate an underlying genetic condition. These tumours may in the third or fourth decade.4 In the case of fibrofolliculoma, not display clinical features that allow a secure diagnosis to be hair specific differentiation is seen, whereas in the case of made, necessitating biopsy and dermatopathological assess- trichodiscoma, differentiation is to the mesodermal component ment. -

2016 Essentials of Dermatopathology Slide Library Handout Book
2016 Essentials of Dermatopathology Slide Library Handout Book April 8-10, 2016 JW Marriott Houston Downtown Houston, TX USA CASE #01 -- SLIDE #01 Diagnosis: Nodular fasciitis Case Summary: 12 year old male with a rapidly growing temple mass. Present for 4 weeks. Nodular fasciitis is a self-limited pseudosarcomatous proliferation that may cause clinical alarm due to its rapid growth. It is most common in young adults but occurs across a wide age range. This lesion is typically 3-5 cm and composed of bland fibroblasts and myofibroblasts without significant cytologic atypia arranged in a loose storiform pattern with areas of extravasated red blood cells. Mitoses may be numerous, but atypical mitotic figures are absent. Nodular fasciitis is a benign process, and recurrence is very rare (1%). Recent work has shown that the MYH9-USP6 gene fusion is present in approximately 90% of cases, and molecular techniques to show USP6 gene rearrangement may be a helpful ancillary tool in difficult cases or on small biopsy samples. Weiss SW, Goldblum JR. Enzinger and Weiss’s Soft Tissue Tumors, 5th edition. Mosby Elsevier. 2008. Erickson-Johnson MR, Chou MM, Evers BR, Roth CW, Seys AR, Jin L, Ye Y, Lau AW, Wang X, Oliveira AM. Nodular fasciitis: a novel model of transient neoplasia induced by MYH9-USP6 gene fusion. Lab Invest. 2011 Oct;91(10):1427-33. Amary MF, Ye H, Berisha F, Tirabosco R, Presneau N, Flanagan AM. Detection of USP6 gene rearrangement in nodular fasciitis: an important diagnostic tool. Virchows Arch. 2013 Jul;463(1):97-8. CONTRIBUTED BY KAREN FRITCHIE, MD 1 CASE #02 -- SLIDE #02 Diagnosis: Cellular fibrous histiocytoma Case Summary: 12 year old female with wrist mass. -

Genetic Heterogeneity Intuberous Sclerosis: Phenotypic Correlations
J Med Genet: first published as 10.1136/jmg.27.7.418 on 1 July 1990. Downloaded from 4184 Med Genet 1990; 27: 418-421 Genetic heterogeneity in tuberous sclerosis: phenotypic correlations I M Winship, J M Connor, P H Beighton Abstract sistently present in families in whom the gene for There is increasing evidence for genetic hetero- TSC is not on 9q34. We conclude that confetti geneity in tuberous sclerosis (TSC) on the basis of depigmentation and nuchal skin tags may be clinical linkage analysis in affected kindreds. We have per- pointers to an alternative locus for TSC. formed a detailed assessment of an affected South African family in which there is no evidence of linkage to chromosome 9 markers. The affected persons have atypical clinical features, namely Tuberous sclerosis (TSC) is inherited as an autosomal prominent nuchal skin tags, a confetti pattern of dominant trait and is characterised by multisystem hypopigmentation of the skin of the lower legs, and hamartosis. The areas of predilection are the skin, absence of ungual fibromata. Further investigation central nervous system, kidneys, and heart, while of these unusual phenotypic features is warranted in other organs are less frequently affected.' Certain skin order to determine whether these lesions are con- lesions are pathognomonic of TSC (adenoma seba- ceum, periungual fibromata, shagreen patches, fibrous facial plaques). Other skin changes may be copyright. MRC Unit for Inherited Skeletal Disorders, Department suggestive (ash leaf macules) or compatible with the of Human Genetics, University of Cape Town Medical diagnosis of TSC in the appropriate clinical setting School, Observatory 7925, South Africa. -

Laparoscopic Management of a Canal of Nuck Cyst
CASE REPORT Laparoscopic Management of a Canal of Nuck Cyst Jacqueline Ho, MD, John Maa, MD, Peter Liou, MD, Jeannette Lager, MD Department of Obstetrics and Gynecology, and Reproductive Sciences, University of California San Francisco, CA (Drs. Ho, Lager). Northern California Chapter of the American College of Surgeons, and Division of General and Trauma Surgery, Marin General Hospital, Larkspur, CA (Dr. Maa). Department of Surgery, Columbia University, New York, NY (Dr. Liou). ABSTRACT The female hydrocele, also known as the canal of Nuck cyst, is a rare congenital abnormality that is the equivalent of the patent processus vaginalis in males. We are the first to report the laparoscopic excision of an entirely extraperitoneal canal of Nuck cyst. We discuss the embryology, pathophysiology, and surgical management of this atypical variant of a rare entity. Key Words: Canal of Nuck cyst, Hydrocele, Laparoscopic surgery, Processus vaginalis. Citation Ho J, Maa J, Liou P, Lager J. Laparoscopic management of a canal of nuck cyst. CRSLS e2014.002134. DOI: 10.4293/CRSLS.2014.002134. Copyright © 2014 SLS This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-ShareAlike 3.0 Unported license, which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original author and source are credited. Presented at the Abdominal Wall Reconstruction Conference, June 12–14, 2014, Washington, DC. Address correspondence to: John Maa, MD, Marin General Hospital, 5 Bon Air Road #101, Larkspur, CA 94939. E-mail: [email protected] INTRODUCTION nation, she had a palpable 5-cm cystic fluid collection lateral to the pubis in the region of her right inguinal canal.