Angiotensin-Converting Enzyme (ACE) Inhibitors
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Angiotensin-Converting Enzyme Inhibitors Or Angiotensin II Receptor Blockers and the Risk of Developing Rheumatoid Arthritis in Antihypertensive Drug Users
Jong, H.J.I. de, Vandebriel, R.J., Saldi, S.R.F., Dijk, L. van, Loveren, H. van, Cohen Tervaert, J.W., Klungel, O.H. Angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers and the risk of developing rheumatoid arthritis in antihypertensive drug users. Pharmacoepidemiology and Drug Safety: 2012, 21(8), 835-843 Postprint Version 1.0 Journal website http://dx.doi.org/10.1002/pds.3291 Pubmed link http://www.ncbi.nlm.nih.gov/pubmed/22674737 DOI 10.1002/pds.3291 This is a NIVEL certified Post Print, more info at http://www.nivel.eu Angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers and the risk of developing rheumatoid arthritis in antihypertensive drug users†‡ HILDA J. I. DE JONG1,2,3, ROB J. VANDEBRIEL1, SITI R. F. SALDI3, LISET VAN DIJK4, HENK VAN LOVEREN1,2, JAN WILLEM COHEN TERVAERT5, OLAF H. KLUNGEL3,* ABSTRACT Purpose: Angiotensin-converting enzyme (ACE) inhibitors and angiotensin II receptor blockers (ARBs) are effective in the treatment of cardiovascular disease. Next to effects on hypertension and cardiac function, these drugs have anti-inflammatory and immunomodulating properties which may either facilitate or protect against the development of autoimmunity, potentially resulting in autoimmune diseases. Therefore, we determined in the current study the association between ACE inhibitor and ARB use and incident rheumatoid arthritis (RA). Methods: A matched case–control study was conducted among patients treated with antihypertensive drugs using the Netherlands Information Network of General Practice (LINH) database in 2001–2006. Cases were patients with a first-time diagnosis of RA. Each case was matched to five controls for age, sex, and index date, which was selected 1 year before the first diagnosis of RA. -

Several Weeks Before Your Surgery, You Should Stop Taking
Several weeks before your surgery, you should stop taking: All Herbal/Vitamin Supplements & Weight loss medicines One week prior to surgery, you should stop taking: Aspirin products and Anti-inflammatory products (OTC and Prescribed) Anticoagulants or blood thinners such as Coumadin, Pradaxa, Plavix, Ticlid, and Aggrenox Night before surgery: Do not drink alcoholic beverages 24 hours prior to surgery. Alcohol may increase the depth of your anesthesia or the effect of medicines you may be given. Do not smoke after midnight prior to having surgery. Smoking can cause gastric secretions that interfere with the anesthetic during surgery. You need to be fasting or nothing to eat or drink 9 hours prior to your surgery. If your surgery is before noon, nothing to eat or drink after 11pm. If your surgery is after noon, nine hours prior to surgery you may eat a light meal (toast with clear juices such as apple juice or ginger ale). Here are some other pre-surgery instructions you need to follow: Do not take the following Blood pressure medications the night before or the morning of surgery: o Do not take ACE Inhibitors : Benazepril (Lotensin), Captopril (Capoten), Enalapril (Vasotec), Fosinpril (Monopril), Lisinopril (Prinvil, Zestril), Moexipril (Univasc or Perdix), Perindopril (Aceon), Quinapril (Accupril), Ramipril (Altace), Trandolapril (Mavik). o Do not take ARBS (Angiotenensin II Receptor Blockers): (Atacand) Candesartan, (Avapro) Irbesartan, (Benicar) Olmesartan, (Cozaar) Losartan, (Diovan) Valsartan, (Micardis) Telmisartan, (Teveten) Eprosartan The morning of surgery when you wake, take the following medications with a small sip of water: o Parkinson’s and seizure medications, blood pressure and heart medication except as indicated above.* o Do not take your diuretics or “water pills” the morning of surgery. -

Apo-Cilazapril/Hydrochlorothiazide Film Coated Tablet
New Zealand Data Sheet APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE 1. PRODUCT NAME APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE – cilazapril 5mg and hydrochlorothiazide 12.5mg film coated tablets. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Cilazapril monohydrate 5.22mg (equivalent to Cilazapril 5mg) and Hydrochlorothiazide 12.5mg Excipient(s) with known effect HYDROCHLOROTHIAZIDE contains sulphur. APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE is lactose free and gluten free. APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE contains Red Ferric Oxide (orange shade # 34690). For the full list of excipients, see section 6.1 3. PHARMACEUTICAL FORM APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE are pink, oval biconvex film-coated tablets. Each tablet is engraved “APO” on one side and “5” bisect “12.5” on the other side. Each tablet typically weighs 92mg. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE is indicated for the treatment of patients with hypertension who are not adequately controlled on monotherapy. 4.2 Dose and method of administration Standard Dosage The dosage of APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE is one tablet administered once daily. As food intake has no clinically significant influence on absorption, APO- CILAZAPRIL/HYDROCHLOROTHIAZIDE can be administered before or after meals. The dose should always be taken at about the same time of day. Special Populations Renal insufficiency When concomitant diuretic therapy is required in patients with severe renal impairment, a loop diuretic rather than a thiazide diuretic is preferred for use with cilazapril/hydrochlorothiazide; therefore, for patients with severe renal dysfunction (creatinine Please refer to Medsafe website (www.medsafe.govt.nz) for the most recent datasheet Page 1 of 22 APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE clearance <10ml/min), APO-CILAZAPRIL/HYDROCHLOROTHIAZIDE is not recommended. -

Selective Mtorc2 Inhibitor Therapeutically Blocks Breast Cancer Cell Growth and Survival
Author Manuscript Published OnlineFirst on January 22, 2018; DOI: 10.1158/0008-5472.CAN-17-2388 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Selective mTORC2 inhibitor therapeutically blocks breast cancer cell growth and survival Thomas A. Werfel1, 3, Shan Wang2, Meredith A. Jackson1, Taylor E. Kavanaugh1, Meghan Morrison Joly3, Linus H. Lee1, Donna J. Hicks3, Violeta Sanchez4, Paula Gonzalez Ericsson4, Kameron V. Kilchrist1, Somtochukwu C. Dimobi1, Samantha M. Sarett1, Dana Brantley-Sieders2, Rebecca S. Cook1,3,4* and Craig L. Duvall1* 1Department of Biomedical Engineering, Vanderbilt University, Nashville, TN 37232 USA 2Department of Medicine, Vanderbilt University Medical Center, Nashville, TN 37232.USA 3Department of Cell and Developmental Biology, Vanderbilt University School of Medicine, Nashville, TN 37232 USA 4Breast Cancer Research Program, Vanderbilt-Ingram Cancer Center, Vanderbilt University Medical Center, Nashville, TN 37232 USA Running Title: A selective mTORC2 inhibitor blocks breast cancer growth Key Words: Breast Cancer, mTOR, Rictor, RNA interference, Nanomedicine *To whom correspondence should be addressed: Craig L. Duvall, PhD Vanderbilt University School of Engineering Department of Biomedical Engineering Nashville, TN 37232 Phone: (615) 322-3598 Fax: (615) 343-7919 Email: [email protected] Rebecca S. Cook, PhD Vanderbilt University Medical Center Department of Cancer Biology Nashville, TN 37232 Phone: (615) 936-3813 Fax: (615) 936-3811 Email: [email protected] Funding. This work was supported by Specialized Program of Research Excellence (SPORE) grant NIH P50 CA098131 (VICC), Cancer Center Support grant NIH P30 CA68485 (VICC), NIH F31 CA195989-01 (MMW), NIH R01 EB019409, DOD CDMRP OR130302, NSF GFRP 1445197, and CTSA UL1TR000445 from the National Center for Advancing Translational Sciences. -

Effective Dose Range of Enalapril in Mild to Moderate Essential Hypertension
Br. J. clin. Pharmac. (1985), 19, 605-611 Effective dose range of enalapril in mild to moderate essential hypertension R. BERGSTRAND', H. HERLITZ2, SAGA JOHANSSON', G. BERGLUND2, A. VEDIN', C. WILHELMSSON', H. J. GOMEZ3, V. J. CIRILLO3 & J. A. BOLOGNESE4 'Department of Medicine, Ostra Hospital and 2Department of Medicine I, Sahlgrenska Hospital, Goteborg, Sweden and Department of 3Cardiovascular Clinical Research and 4Clinical Biostatistics, Merck Sharp & Dohme Research Laboratories, Rahway, New Jersey, USA 1 The dose-response relationship of enalapril was evaluated in a double-blind, balanced, two-period, incomplete-block study in 91 patients with mild to moderate essential hyper- tension. 2 Patients were randomly assigned to two of six treatments: placebo, 2.5, 5, 10, 20 and 40 mg/day of enalapril maleate. There were two 3-week treatment periods, each preceded by a 4-week, single-blind placebo washout. 3 Each dose of enalapril produced significant decreases in standing and supine systolic and diastolic blood pressure after 2 and 3 weeks of treatment. There were no significant changes on placebo. 4 There was a significant linear dose response relationship for both mean blood pressure and mean change from baseline in blood pressure (P < 0.01 for systolic and mean arterial pressure, and P < 0.05 for diastolic pressure). 5 Enalapril was associated with an increasing dose-response relationship across the 2.5- 40 mg/day range. The 2.5 mg/dose is effective in some patients; however, doses ¢ 10 mg/ day may be necessary to achieve satisfactory blood pressure control. Keywords enalapril angiotensin converting enzyme inhibitor dose-response relationship Introduction In recent years much interest has been focused with renal impairment treated with high doses of on angiotensin converting enzyme (ACE) in- captopril. -

A Comparison of the Tolerability of the Direct Renin Inhibitor Aliskiren and Lisinopril in Patients with Severe Hypertension
Journal of Human Hypertension (2007) 21, 780–787 & 2007 Nature Publishing Group All rights reserved 0950-9240/07 $30.00 www.nature.com/jhh ORIGINAL ARTICLE A comparison of the tolerability of the direct renin inhibitor aliskiren and lisinopril in patients with severe hypertension RH Strasser1, JG Puig2, C Farsang3, M Croket4,JLi5 and H van Ingen4 1Technical University Dresden, Heart Center, University Hospital, Dresden, Germany; 2Department of Internal Medicine, La Paz Hospital, Madrid, Spain; 31st Department of Internal Medicine, Semmelweis University, Budapest, Hungary; 4Novartis Pharma AG, Basel, Switzerland and 5Novartis Institutes for Biomedical Research, Cambridge, MA, USA Patients with severe hypertension (4180/110 mm Hg) LIS 3.4%). The most frequently reported AEs in both require large blood pressure (BP) reductions to reach groups were headache, nasopharyngitis and dizziness. recommended treatment goals (o140/90 mm Hg) and At end point, ALI showed similar mean reductions from usually require combination therapy to do so. This baseline to LIS in msDBP (ALI À18.5 mm Hg vs LIS 8-week, multicenter, randomized, double-blind, parallel- À20.1 mm Hg; mean treatment difference 1.7 mm Hg group study compared the tolerability and antihyperten- (95% confidence interval (CI) À1.0, 4.4)) and mean sitting sive efficacy of the novel direct renin inhibitor aliskiren systolic blood pressure (ALI À20.0 mm Hg vs LIS with the angiotensin converting enzyme inhibitor À22.3 mm Hg; mean treatment difference 2.8 mm Hg lisinopril in patients with severe hypertension (mean (95% CI À1.7, 7.4)). Responder rates (msDBPo90 mm Hg sitting diastolic blood pressure (msDBP)X105 mm Hg and/or reduction from baselineX10 mm Hg) were 81.5% and o120 mm Hg). -
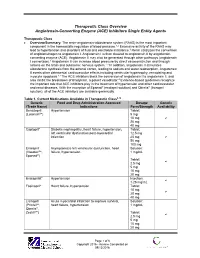
Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents
Therapeutic Class Overview Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents Therapeutic Class Overview/Summary: The renin-angiotensin-aldosterone system (RAAS) is the most important component in the homeostatic regulation of blood pressure.1,2 Excessive activity of the RAAS may lead to hypertension and disorders of fluid and electrolyte imbalance.3 Renin catalyzes the conversion of angiotensinogen to angiotensin I. Angiotensin I is then cleaved to angiotensin II by angiotensin- converting enzyme (ACE). Angiotensin II may also be generated through other pathways (angiotensin I convertase).1 Angiotensin II can increase blood pressure by direct vasoconstriction and through actions on the brain and autonomic nervous system.1,3 In addition, angiotensin II stimulates aldosterone synthesis from the adrenal cortex, leading to sodium and water reabsorption. Angiotensin II exerts other detrimental cardiovascular effects including ventricular hypertrophy, remodeling and myocyte apoptosis.1,2 The ACE inhibitors block the conversion of angiotensin I to angiotensin II, and also inhibit the breakdown of bradykinin, a potent vasodilator.4 Evidence-based guidelines recognize the important role that ACE inhibitors play in the treatment of hypertension and other cardiovascular and renal diseases. With the exception of Epaned® (enalapril solution) and Qbrelis® (lisinopril solution), all of the ACE inhibitors are available generically. Table 1. Current Medications Available in Therapeutic Class5-19 Generic Food and Drug Administration -
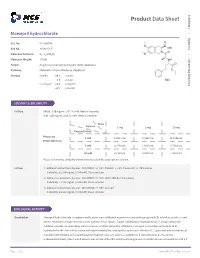

Moexipril Hydrochloride | Medchemexpress
Inhibitors Product Data Sheet Moexipril hydrochloride • Agonists Cat. No.: HY-B0378A CAS No.: 82586-52-5 Molecular Formula: C₂₇H₃₅ClN₂O₇ • Molecular Weight: 535.03 Screening Libraries Target: Angiotensin-converting Enzyme (ACE); Apoptosis Pathway: Metabolic Enzyme/Protease; Apoptosis Storage: Powder -20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month SOLVENT & SOLUBILITY In Vitro DMSO : 250 mg/mL (467.26 mM; Need ultrasonic) H2O : 100 mg/mL (186.91 mM; Need ultrasonic) Mass Solvent 1 mg 5 mg 10 mg Concentration Preparing 1 mM 1.8691 mL 9.3453 mL 18.6905 mL Stock Solutions 5 mM 0.3738 mL 1.8691 mL 3.7381 mL 10 mM 0.1869 mL 0.9345 mL 1.8691 mL Please refer to the solubility information to select the appropriate solvent. In Vivo 1. Add each solvent one by one: 10% DMSO >> 40% PEG300 >> 5% Tween-80 >> 45% saline Solubility: ≥ 2.08 mg/mL (3.89 mM); Clear solution 2. Add each solvent one by one: 10% DMSO >> 90% (20% SBE-β-CD in saline) Solubility: ≥ 2.08 mg/mL (3.89 mM); Clear solution 3. Add each solvent one by one: 10% DMSO >> 90% corn oil Solubility: ≥ 2.08 mg/mL (3.89 mM); Clear solution BIOLOGICAL ACTIVITY Description Moexipril hydrochloride is a potent orally active non-sulfhydryl angiotensin converting enzyme(ACE) inhibitor, which is used for the treatment of hypertension and congestive heart failure. Target: ACEMoexipril hydrochloride is a long-acting ACE inhibitor suitable for once-daily administration, and like some ACE inhibitors, moexipril is a prodrug and needs to be hydrolyzed in the liver into its active carboxylic metabolite, moexiprilat, to become effective [1]. -

Download Leaflet View the Patient Leaflet in PDF Format
Package leaflet: Information for the patient Fosinopril Sodium 10 mg Tablets Fosinopril Sodium 20 mg Tablets Fosinopril sodium Read all of this leaflet carefully before you start taking this medicine because it contains important information for you. - Keep this leaflet. You may need to read it again. - If you have any further questions, ask your doctor or pharmacist. - This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours. - If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4. What is in this leaflet 1. What Fosinopril is and what it is used for 2. What you need to know before you take Fosinopril 3. How to take Fosinopril 4. Possible side effects 5. How to store Fosinopril 6. Contents of the pack and other information. 1. What Fosinopril is and what is it used for Fosinopril belongs to the class of medicines called Angiotensin Converting Enzyme (ACE) inhibitors that act on the heart and blood vessels. You may have been given Fosinopril to: • lower your blood pressure if it is too high (a condition called hypertension) • help your heart pump blood around your body if you have a condition known as heart failure and are also being treated with diuretics (medicines which help to remove excess fluid from the body). 2. What you need to know before you take Fosinopril Do not take Fosinopril: • if you are allergic to fosinopril or any other ACE inhibitor, or any of the other ingredients of this medicine (listed in section 6). -

Cough Induced by Enalapril but Not by Captopril
Eur Respir J 1989, 2, 289-291 CASE REPORT Cough induced by enalapril but not by captopril H. Puolijoki*, M. Nieminen*, E. Moilanen**, L. Siitonen*, A. Lahdensuo*, P. Reinikainen*, H. Vapaatalo** Cough iruluced by enalapril but 1101 by capropril. H. Puolijoki, M Nieminen, •Tampere University Central Hospital. E. Moilanen, L. Siironen, A. Lahdensuo, P. Reinikainen, If. VapaaJalo. •• Dept of Biomedical Sciences, University of ABSTRACT: We report a 68 yr old woman with hypertension wbo Tampcre. Finland. developed a dry cough on enalaprll but not on captopril therapy. Pul monary function te!its, methacholine in halation challenges, total blood Correspondence: H. Puolijoki, Dept of Pulmonary Diseases, Turlcu University Central Hospital, SF- eoslnophiJ counts, and changes In plasma concentrations or prostaglandin 207 40 Preitila, Finland. E2 and tllromboxane 81 did not explain the difference in the adverse reaction between tbese two angiotensin converting enzyme inhibitors. Keywords: ACE inhibitors; captopril; cough; Eur Respir J., 1989, 2, 289- 291. enalapril. Received: March, 1988; accepted after revision August 9, 1988. Angiotensin converting enzyme (ACE) inhibiLors like Case History capropril and ena1april are usually well tolerated. How ever, in some patientS they may cause cough as an A 68 yr old non-smoking woman with diabetes, adverse reaction [1]. We report a female patiem who hypertension and compensated heart failure, but with developed a cough on enalapril but not on captopril no respiratory disease or abnormalities on chest X-ray, therapy. We evaluated her lung function, bronchial re developed a dry cough but no dyspnoea or posrnasal activity to methacholine, LolaJ blood eosinophi l count as drip during Lreatmem with ena1april (Renitcc®, MSD, E 20 mg·day·1) for hypertension. -

Summary of Product Characteristics
Proposed var 24 psusa cilazapril SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT [Fosinopril sodium 10 mg, tablets] [Fosinopril sodium 20 mg, tablets] 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains 10 or 20 mg fosinopril sodium. Excipient with known effect: Each tablet fosinopril sodium 10 mg contains 87 mg of lactose, anhydrous. Each tablet fosinopril sodium 20 mg contains 174 mg of lactose, anhydrous. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Tablet. The 10 mg tablets are white and shaped like a capsule with indents. On one side they are engraved with the letters “APO” and on the other side with “FOS-10”. The 20 mg tablets are white and their shape is oval. On one side they are engraved with the letters “APO” and on the other side with “FOS-20”. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications - Treatment of hypertension. - Treatment of symptomatic heart failure. 4.2 Posology and method of administration Posology Fosinopril sodium should be administered orally in a single daily dose. As with all other medicinal products taken once daily, it should be taken at approximately the same time each day. The absorption of fosinopril sodium is not affected by food. The dose should be individualised according to patient profile and blood pressure response (see section 4.4). Hypertension: Fosinopril sodium may be used as a monotherapy or in combination with other classes of antihypertensive medicinal products (see section 4.3, 4.4, 4.5 and 5.1). Hypertensive patients not being treated with diuretics: Starting dose The initial recommended dose is 10 mg once a day. -

Ace Inhibitors (Angiotensin-Converting Enzyme)
Medication Instructions Ace Inhibitors (Angiotensin-Converting Enzyme) Generic Brand Benazepril Lotensin Captopril Capoten Enalapril Vasotec Fosinopril Monopril Lisinopril Prinivil, Zestril Do not Moexipril Univasc Quinapril Accupril stop taking Ramipril Altace this medicine Trandolapril Mavik About this Medicine unless told ACE inhibitors are used to treat both high blood pressure (hypertension) and heart failure (HF). They block an enzyme that causes blood vessels to constrict. This to do so allows the blood vessels to relax and dilate. Untreated, high blood pressure can damage to your heart, kidneys and may lead to stroke or heart failure. In HF, using by your an ACE inhibitor can: • Protect your heart from further injury doctor. • Improve your health • Reduce your symptoms • Can prevent heart failure. Generic forms of ACE Inhibitors (benazepril, captopril, enalapril, fosinopril, and lisinopril) may be purchased at a lower price. There are no “generics” for Accupril, Altace Mavik, and of Univasc. Thus their prices are higher. Ask your doctor if one of the generic ACE Inhibitors would work for you. How to Take Use this drug as directed by your doctor. It is best to take these drugs, especially captopril, on an empty stomach one hour before or two hours after meals (unless otherwise instructed by your doctor). Side Effects Along with needed effects, a drug may cause some unwanted effects. Many people will not have any side effects. Most of these side effects are mild and short-lived. Check with your doctor if any of the following side effects occur: • Fever and chills • Hoarseness • Swelling of face, mouth, hands or feet or any trouble in swallowing or breathing • Dizziness or lightheadedness (often a problem with the first dose) Report these side effects if they persist: • Cough – dry or continuing • Loss of taste, diarrhea, nausea, headache or unusual fatigue • Fast or irregular heartbeat, dizziness, lightheadedness • Skin rash Special Guidelines • Sodium in the diet may cause you to retain fluid and increase your blood pressure.