Common Skin Conditions in Children
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

FIG. 4A © O O Wo 2015/042110 Al III III II II III III 1 1 II III II II III III II III
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date W O 2015/042110 A l 2 6 March 2015 (26.03.2015) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61P 37/00 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/US20 14/056021 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, ΓΝ , IR, IS, JP, KE, KG, KN, KP, KR, 17 September 2014 (17.09.2014) KZ, LA, LC, LK, LR, LS, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, OM, (25) Filing Language: English PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, SC, (26) Publication Language: English SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, ZW. (30) Priority Data: 61/880,522 20 September 2013 (20.09.2013) (84) Designated States (unless otherwise indicated, for every kind of regional protection available): ARIPO (BW, GH, (71) Applicant: CHILDREN'S MEDICAL CENTER COR¬ GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, ST, SZ, PORATION [US/US]; 55 Shattuck Street, Boston, Mas¬ TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, sachusetts 021 15 (US). -

Seborrheic Dermatitis
432 Teams Dermatology Done by: Wael Al Saleh & Abdulrahman Al-Akeel Reviewer: Wael Al Saleh & Abdulrahman Al-Akeel 9 Team Leader: Basil Al Suwaine Color Code: Original, Team’s note, Important, Doctor’s note, Not important, Old teamwork 432 Dermatology Team Lecture 9: Atopic dermatitis/ Eczema Objectives 1- To know the definition & classification of Dermatitis/Eczema 2- To recognize the primary presentation of different types of eczema 3- To understand the possible pathogenesis of each type of eczema 4- To know the scheme of managements lines P a g e | 1 432 Dermatology Team Lecture 9: Atopic dermatitis/ Eczema Introduction: A groups and spectrum of related disorders with pruritus being the hallmark of the disease, they also come with dry skin. Every atopic dermatitis is eczema but not every eczema are atopic dermatitis. Atopic dermatitis mean that the patient has eczema (excoriated skin, itching and re-onset) and atopy (atopy; the patient or one of his family has allergic rhinitis, asthma or eczema). It starts early of life (eczema can happen at any time). It classified as: - Acute, characterized by erythema, papules, vesicles, oozing, and crusting. - Subacute, clinically it is represented by erythema, scaling, and crusting. - Chronic, presents with thickening of the skin, skin markings become prominent (lichenification); pigmentation and fissuring of the skin occur. Acute on top of chronic very dry 4 years old boy with chronic, itchy, well defined brownish plaque with bleeding plaques. lichenifications. Ill defined plaques Well defined erythematous excoriated Lichenification is the hallmark for plaques on both cheeks with erosion. chronic course. P a g e | 2 432 Dermatology Team Lecture 9: Atopic dermatitis/ Eczema Dermatitis Classification of dermatitis: Atopic, more common in children Seborrheic (oily skin)- (like naso-labial folds, scalp, ears) Contact dermatitis, substance cause eczema - Allergic - Irritant Nummular, coined shape, usually in the shin. -

Xerotic Eczema
433 Dermatology Team Other type of eczema Lecture(10) Other type of eczema [email protected] 1 | P a g e 433 Dermatology Team Other type of eczema Content of lecture: To know the classification of Eczema. To recognize the primary presentation of different types of eczema. To understand the possible pathogenesis of each type of eczema. To know the scheme of managements lines. Color index: slides, doctor notes, 432 notes, Important 2 | P a g e 433 Dermatology Team Other type of eczema 1-Nummular Dermatitis: Coin shaped patches and plaques Secondary to xerosis cutis Primary symptom itch Notice the surrounding xerosis 2- Regional Eczema: A. Ear eczema B. Eyelid dermatitis Note: using of moisturizing C. Nipple eczema woreworse perorbital D. Hand eczema dermatitis. E. Diaper dermatitis F. Juvenile plantar dermatosis A- Ear Eczema Most frequently caused by seborrheic or atopic dermatitis Staph, Strep, or Psoeudomonas Earlobe is pathognomonic of nickel allergy B- Eyelid dermatitis When on one eye only, it is most frequently caused by nail polish When both eyelids are involved, consider mascara, eye shadow, eyelash cement, eyeliner, etc 3 | P a g e 433 Dermatology Team Other type of eczema C- Nipple eczema Painful fissuring, seen especially in nursing mothers. Maybe an isolated manifestation of atopic dermatitis. If persist more than 3 month, and/or unilateral, biopsy is mandatory to rule out Pagets disease . D- Hand eczema Spongiosis histologically . Irritant hand dermatitis- seen in homemakers, nurses. Resulting from excessive exposure to soaps. Pompholyx- tapioca vesicles, on sides of fingers, palms, and soles. Irritant versus allergic. Note: Adult atopic dermatitis has the greatest risk for hand dermatitis E- Juvenile plantar dermatitis Begins as a patchy symmetrical, smooth, red, glazed macules on the base of the great toes Affect age 3 to puberty. -

Dermatitis and Eczema
Dermatitis and eczema Professor Danka Švecová MD, PhD, Dept.of Dermatovenerology Faculty of Medicine, Comenius University Dermatitis and Eczema Definition • The form of epidermal intolerance reaction • Noncontagious inflammatory dermatoses • Acute case – exudative – inflammatory skin changes – redness, swelling, vesicles, oozing, crusts, itching • Chronic case – proliferative inflammatory processes – redness, epidermal thickening (acanthosis), scaling, lichenification, itching • Origin of the disease – exogenous or endogenous - toxic or allergic - noxious factors : known or unknown Dermatitis and Eczema Classification • Irritant contact dermatitis: acute and chronic • Allergic contact dermatitis (eczema): acute and chronic • Dyshidrotic dermatitis (eczema) • Atopic dermatitis (eczema) • Nummular (microbial) dermatitis (eczema) • Seborrheic dermatitis Acute irritant contact dermatitis It results from the exposure of the skin to external agents that overwhelm the normal skin barrier function • External agents → simply highly toxic →or repeated exposures to agents of low toxicity (washing hands many times daily) →or variety of predisposing intrinsic factors (atopy, ichthyosis) Epidemiology far more common than allergic contact dermatitis; toxic substances - in many work places, the home, the garden, in a variety of hobbies Acute irritant contact dermatitis Etiopathogenesis toxic reaction – tissue necrosis from a concentrated acid or base solution – damaging effect in minutes; less noxious agents – damage of the skin protective barrier Acute -

Contact Dermatitis Codes for ICD-10
Converting Contact Dermatitis Codes from ICD-9-CM to ICD-10-CM ICD10CM Irritant Contact Dermatitis Codes ICD-9 CM Contact dermatitis and other eczema due to detergents 692.0 L24.0 Irritant contact dermatitis due to detergents L24.1 …due to oils and greases 692.1 L24.2 …due to solvents 692.2 …due to drugs and medicines in contact with skin 692.3 L24.3 Irritant contact dermatitis due to cosmetics L24.4 Irritant contact dermatitis due to drugs in contact with skin L24.5 Irritant contact dermatitis due to other chemical products L24.6 Irritant contact dermatitis due to food in contact with skin L24.7 Irritant contact dermatitis due to plants, except food L24.81 Irritant contact dermatitis due to metals 692.83 L24.89 Irritant contact dermatitis due to other agents L24.9 Irritant contact dermatitis, unspecified cause Allergic contact Dermatitis Codes L23.0 Allergic contact dermatitis due to metals 692.83 L23.1 Allergic contact dermatitis due to adhesives L23.2 Allergic contact dermatitis due to cosmetics L23.3 Allergic contact dermatitis due to drugs in contact with skin L23.4 Allergic contact dermatitis due to dyes L23.5 Allergic contact dermatitis due to other chemical products L23.6 Allergic contact dermatitis due to food in contact with skin L23.7 Allergic contact dermatitis due to plants, except food L23.81 Allergic contact dermatitis due to animal (cat) (dog) dander 692.84 L23.89 Allergic contact dermatitis due to other agents 692.89 L23.9 Allergic contact dermatitis, unspecified cause L25.0 Unspecified contact dermatitis due to cosmetics -

General Aspects 14 Niels K
14_199_254* 05.11.2005 10:15 Uhr Seite 201 Chapter 14 General Aspects 14 Niels K. Veien Contents 14.1 Introduction . 201 14.4.2.1 Cement Ulcerations . 224 14.4.2.2 Pigmented Contact Dermatitis . 225 14.2 The Medical History of the Patient . 202 14.4.2.3 Caterpillar Dermatitis and Irritant Dermatitis 14.2.1 History of Hereditary Diseases . 202 from Plants and Animals . 225 14.2.2 General Medical History . 202 14.4.2.4 Head and Neck Dermatitis . 225 14.2.3 History of Previous Dermatitis . 203 14.4.2.5 Dermatitis from Transcutaneous Delivery 14.2.4 Time of Onset . 203 Systems . 225 14.2.5 History of Aggravating Factors . 204 14.4.2.6 Berloque Dermatitis . 226 14.2.6 Course of the Dermatitis . 205 14.4.2.7 Stomatitis due to Mercury or Gold Allergy . 226 14.2.7 Types of Symptoms . 205 14.5 Regional Contact Dermatitis . 226 14.3 Clinical Features of Eczematous Reactions . 206 14.5.1 Dermatitis of the Scalp . 226 14.3.1 Acute and Recurrent Dermatitis . 206 14.5.2 Dermatitis of the Face and Neck . 228 14.3.2 Chronic Dermatitis . 210 14.5.2.1 The Lips . 230 14.3.3 Nummular (Discoid) Eczema . 211 14.5.2.2 The Eyes and Eyelids . 230 14.3.4 Secondarily Infected Dermatitis . 211 14.5.2.3 The Ear . 231 14.3.5 Clinical Features of Contact Dermatitis 14.5.3 Dermatitis of the Trunk . 232 in Specific Groups of Persons . 212 14.5.3.1 The Axillary Region . -

Home Phototherapy Order Form
Physician’s Written Order for Home Phototherapy Fax to: 605-322-2475 or Email: [email protected] This form is a Prescription and Statement of Medical Necessity for Daavlin home phototherapy products Rx used for the treatment of skin conditions such as psoriasis. All fields required for insurance approval. First Name _______________________ Last Name _________________________ DOB ____/____/____ Gender: M F Address _____________________________________________ City_________________________ State_____ Zip__________ Patient Info: Patient Phone #________________________________ Alt Phone # or Email _______________________________________________ HCPCs: Product and Description: Physician Name ___________________________________ DermaPal: Hand-held treatment wand for scalp, Practice __________________________________________ E0691 spot treatment or travel. Includes comb attachment. NPI# ______________________________________________ E0691 1 Series: Small, light-weight panel for hands, face, Address _________________________________________ feet, elbows, or any other localized treatment area. City ______________________ State ____ Zip _________ 7 Series 8 Lamp: Six foot tall, multi-directional unit Info: Physician Prescribing Phone (____)______________*Fax (____)______________ Home Phototherapy Product: Home Phototherapy E0694 for large areas and/or full body treatment. * IMPORTANT: We will use this fax number to fax the Prescriber’s Dosing Guide ICD-10 Code: Description: ICD-10 Code Estimated Duration of Need: ___ Months ( -

The Itch That Rashes Cynthia Griffith MPAS, PA-C
The Itch That Rashes Cynthia Griffith MPAS, PA-C 1 Atopic Dermatitis Pityriasis Alba Nummular Eczema Dyshidrotic Eczema Lichen Simplex Chronicus Semantics: Eczema is a descriptive term not technically a diagnosis. The term refers to a group of inflammatory skin eruptions; atopic dermatitis, contact dermatitis, dyshidrotic eczema, ect. 3 Atopic Dermatitis Chronic, pruritic skin disease caused by barrier dysfunction, genetics, environment, impaired immune response. "The itch that rashes" Atopic Dermatitis Aggravators Stress, heat, sweating, and external irritants You should refrain from wearing wool as this can further irritate your skin. Emotional stress Extremes of weather. Infection Atopic Dermatitis Clinical presentation: Erythematous papules, that coalesce to form erythematous plaques that may display weeping, crusting, or scale over cheeks, forehead, scalp and extensor surfaces in toddlers and infants Atopic Dermatitis Clinical presentation: Lichenified, eczematous plaques in flexural areas of the neck, elbows, wrists, and ankles in older kids and adults Atopic Dermatitis Atopy Triad: Allergic rhinitis, Asthma, Atopic dermatitis Treatment: First line: long term emollients, short term topical steroids, antibiotics for secondary infection Second line: Topical calcineurin inhibitors - tacrolimus and pimecrolimus Food allergy may be a factor in kids with refractory AD Atopic Dermatitis Adult Patient care tips Hot baths, alkaline soaps, vigorous rubbing and scrubbing should be avoided. Water should be kept tepid and a mild cleanser (not antibiotic cleanser) should be used only on soiled skin. Soap should be used only on arm pits, genital region and scalp. Immediately after bathing while the skin is still moist apply a thin coat of Vaseline or Aquaphor to skin. Atopic Dermatitis Adult Patient care tips Humidifiers are helpful. -

Atopic Dermatitis-Eczema
432 Teams Dermatology Done by: Lama Al Faraidi Reviewer: Lama Al Tawil 11 Team Leader: Basil Al Suwaine&Lama Al Tawil Color Code: Original, Team’s note, Important, Doctor’s note, Not important, Old teamwork 432 Dermatology Team Lecture11: Atopic dermatitis-Eczema Objectives To know the definition & classification of Dermatitis/Eczema To recognize the primary presentation of different types of eczema To understand the possible pathogenesis of each type of eczema To know the scheme of managements lines P a g e | 1 432 Dermatology Team Lecture11: Atopic dermatitis-Eczema Eczema (dermatology term) – dermatitis (pathological term) Definition: inflammation of the skin What are the eczema phases? Acute eczema: erosion, oozing and vesicles Subacute eczema: Redness+ swelling, crust -+ scale +infection (most common phase) Chronic eczema: lichenification, dark pigmentation and thick papules and plaques - Scales in eczema are fine with dry itchy skin - To diagnose eczema it has to be itchy , no itchy no eczema Acute eczema Subacute eczema Chronic eczema Atopic Dermatitis Definition: chronic relapsing itchy skin disease in genetically predisposed patients. Associated diseases (Atopy): bronchial asthma, allergic rhinitis, allergic conjunctivitis (personal or family Hx of atopy including the airway involvment ) Incidence: up to 15-20 % in early childhood More in male Age of onset: (most commonly starts at infancy then at school age) 60% ------ first 2 months of life 30 %------- by age of 5 10%-------- between age 6- 20 years Improves -

Summary of Product Characteristics 1 Name of the Medicinal Product 2 Qualitative and Quantitative Composition 3 Pharmaceutical F
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Betnovate Ointment 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Betamethasone Valerate B.P. 0.122% w/w Equivalent to 0.1 w/w betamethasone For the full list of excipients, see section 6.1 3 PHARMACEUTICAL FORM Ointment 4 CLINICAL PARTICULARS 4.1 Therapeutic indications Betamethasone valerate is a potent topical corticosteroid indicated for adults, elderly and children over 1 year for the relief of the inflammatory and pruritic manifestations of steroid responsive dermatoses. These include the following: Atopic dermatitis (including infantile atopic dermatitis) Nummular dermatitis (discoid eczema) Prurigo nodularis Psoriasis (excluding widespread plaque psoriasis) Lichen simplex chronicus (neurodermatitis) and lichen planus Seborrhoeic dermatitis Irritant or allergic contact dermatitis Discoid lupus erythematosus Adjunct to systemic steroid therapy in generalised erythroderma 4.2 Posology and method of administration Route of administration: Cutaneous Ointments are especially appropriate for dry, lichenified, scaly lesions. Apply thinly and gently rub in using only enough to cover the entire affected area once or twice daily for up to 4 weeks until improvement occurs, then reduce the frequency of application or change the treatment to a less potent preparation. Allow adequate time for absorption after each application before applying an emollient. In the more resistant lesions, such as the thickened plaques of psoriasis on elbows and knees, the effect of betamethasone valerate can be enhanced, if necessary, by occluding the treatment area with polythene film. Overnight occlusion only is usually adequate to bring about a satisfactory response in such lesions; thereafter, improvement can usually be maintained by regular application without occlusion. -
Symptoms of Dyshidrotic Eczema
Eczema (EK-suh-muh) is the name for a group of conditions that cause the skin to become red, itchy and inflamed. It is also known as dermatitis. There are several types of eczema, including atopic dermatitis, contact dermatitis, dyshidrotic eczema, nummular eczema, seborrheic dermatitis and stasis dermatitis. It is possible to have more than one type of eczema at once. Eczema is not contagious. You can’t “catch it” from someone else. While the exact cause of eczema is unknown, researchers do know that people develop eczema because of a combination of genes and triggers. People with eczema tend to have an over-reactive immune system that, when triggered by something outside or inside the body, responds by producing inflammation. It is this inflammation that causes the red, itchy and painful skin symptoms common to eczema. Research also shows that some people with eczema have a mutation of the gene responsible for creating filaggrin. Filaggrin is a protein that helps our bodies maintain a healthy, protective 2 National Eczema Association barrier on the very top layer of the skin. Without enough filaggrin to build a strong skin barrier, moisture can escape and bacteria, viruses and more can enter. This is why many people with eczema have very dry and infection-prone skin. Atopic dermatitis, contact dermatitis and nummular eczema can appear almost anywhere on the body, especially the hands, feet, face and torso. Dyshidrotic eczema appears on the feet and hands. Seborrheic dermatitis happens where there are a lot of oil-producing glands like the face, scalp, back and chest. -
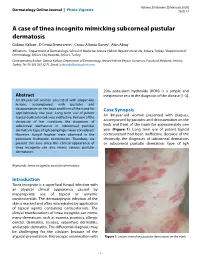
A Case of Tinea Incognito Mimicking Subcorneal Pustular Dermatosis Göknur Kalkan1, D Deniz Demirseren2, Cansu Altınöz Güney1, Akın Aktaş1
Volume 26 Number 2| February 2020| Dermatology Online Journal || Photo Vignette 26(2):13 A case of tinea incognito mimicking subcorneal pustular dermatosis Göknur Kalkan1, D Deniz Demirseren2, Cansu Altınöz Güney1, Akın Aktaş1. Affiliations: 1Department of Dermatology, School of Medicine, Ankara Yıldırım Beyazıt University, Ankara, Turkey, 2Department of Dermatology, Ankara City Hospital, Ankara, Turkey Corresponding Author: Göknur Kalkan, Department of Dermatology, AnkaraYıldırım Beyazıt University, Faculty of Medicine, Ankara, Turkey, Tel: 90-505 265 32 71, Email: [email protected] 20% potassium hydroxide (KOH) is a simple and Abstract inexpensive test in the diagnosis of the disease [1-3]. An 89-year-old woman presented with plaque-like lesions, accompanied with pustules and desquamation on the back and front of the trunk for Case Synopsis approximately one year. Long term use of potent An 89-year-old woman presented with plaques, topical corticosteroids was ineffective. Because of the chronicity of her condition, the diagnoses of accompanied by pustules and desquamation on the subcorneal dermatosis or subcorneal pustular back and front of the trunk for approximately one dermatosis type of IgA pemphigus were considered. year (Figure 1). Long term use of potent topical However, fungal hyphae were observed in the corticosteroid had been ineffective. Because of the potassium hydroxide examination. Therefore, we chronicity, the diagnoses of subcorneal dermatosis present this case since this clinical appearance of or subcorneal pustular dermatosis type of IgA tinea incognito can also mimic various pustular dermatoses. Keywords: tinea incognito, pustular dermatosis Introduction Tinea incognito is a superficial fungal infection with an atypical clinical appearance caused by inappropriate use of topical or systemic corticosteroids.