Ciliary Body Masses Inducing Cataract
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Glaucoma Related to Ocular and Orbital Tumors Sonal P
Chapter Glaucoma Related to Ocular and Orbital Tumors Sonal P. Yadav Abstract Secondary glaucoma due to ocular and orbital tumors can be a diagnostic challenge. It is an essential differential to consider in eyes with a known tumor as well as with unilateral, atypical, asymmetrical, or refractory glaucoma. Various intraocular neoplasms including iris and ciliary body tumors (melanoma, metasta- sis, lymphoma), choroidal tumors (melanoma, metastasis), vitreo-retinal tumors (retinoblastoma, medulloepithelioma, vitreoretinal lymphoma) and orbital tumors (extra-scleral extension of choroidal melanoma or retinoblastoma, primary orbital tumors) etc. can lead to raised intraocular pressure. The mechanisms for glaucoma include direct (tumor invasion or infiltration related outflow obstruction, tra- becular meshwork seeding) or indirect (angle closure from neovascularization or anterior displacement or compression of iris) or elevated episcleral venous pressure secondary to orbital tumors. These forms of glaucoma need unique diagnostic techniques and customized treatment considerations as they often pose therapeutic dilemmas. This chapter will review and discuss the mechanisms, clinical presenta- tions and management of glaucoma related to ocular and orbital tumors. Keywords: ocular tumors, secondary glaucoma, orbital tumors, angle infiltration, neovascular glaucoma, neoplastic glaucoma 1. Introduction With the advent of constantly evolving and advancing ophthalmic imaging tech- niques as well as surgical modalities in the field of ophthalmic diseases, diagnostic accuracy, and treatment outcomes of ocular as well as orbital tumors have improved remarkably over the past few years. Raised intraocular pressure (IOP) is known to be one of the presenting features or associated finding for numerous ocular as well as orbital tumors. Ocular and orbital tumors can cause secondary glaucoma due to various mechanisms. -
Commentary on the Masquerades of A
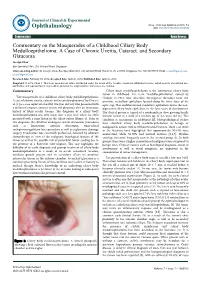
perim Ex en l & ta a l ic O p in l h t C h f Journal of Clinical & Experimental a o l m l a o n l r o Chua, J Clin Exp Ophthalmol 2016, 7:2 g u y o J Ophthalmology 10.4172/2155-9570.1000543 ISSN: 2155-9570 DOI: Commentary Open Access Commentary on the Masquerades of a Childhood Ciliary Body Medulloepithelioma: A Case of Chronic Uveitis, Cataract, and Secondary Glaucoma Jocelyn Chua* Eye Specialist Clinic, 290 Orchard Road, Singapore *Corresponding author: Dr Jocelyn Chua, Eye Specialist Clinic, 290 Orchard Road, #06-01 to 05, 238859, Singapore; Tel: +65 96897919; Email: [email protected], [email protected] Received date: February 09, 2016; Accepted date: April 20, 2016; Published date: April 25, 2016 Copyright: © 2016 Chua J. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Commentary Ciliary body medulloepithelioma is the commonest ciliary body tumor in childhood. The term “medulloepithelioma”, coined by "The masquerades of a childhood ciliary body medulloepithelioma: Grinker in 1931, best describes the origin of the tumor from the A case of chronic uveitis, cataract and secondary glaucoma" by Chua et primitive medullary epithelium located along the inner layer of the al. [1] is a case report of a healthy two year old boy who presented with optic cup. This undifferentiated medullary epithelium forms the non- a unilateral cataract, anterior uveitis and glaucoma after an innocuous pigmented ciliary body epithelium in the later years of development. -

(Diktyoma) Presenting As a Perforated, Infected Eye
Br J Ophthalmol: first published as 10.1136/bjo.61.3.229 on 1 March 1977. Downloaded from British Journal of Ophthalmology, 1977, 61, 229-232 Medulloepithelioma (diktyoma) presenting as a perforated, infected eye MOHAMED A. VIRJI Central Pathology Laboratory, Ministry of Health, Dar-es-Salaam, Tanzania SUMMARY A case of embryonal medulloepithelioma (diktyoma) presenting with perforated infected eye in a 13-year-old Black African girl is described. The tumour mass occupied most of the deformed eye, and invasion of the sclera anteriorly was seen. There was no evidence of orbital or distant tumour involvement. It is suggested that with increasing age these tumours are more likely to show frankly malignant features. Medulloepithelioma (diktyoma) is a rare neoplasm anteriorly perforated left eye, with loss of cornea, of the eye which is characterised by slow growth and purulent discharge, and a fragmenting mass of local invasion and is composed of glandular, irregular brownish-grey tissue attached mainly to neural, and mesenchymal elements (Andersen, the superior and temporal portion of the eye and 1962). It presents even rarely as an infected perfor- extending into the posterior chamber. The infection ated eye with a fungating mass replacing the ocular was controlled with systemic antibiotics and the left copyright. contents. Soudakoff (1936) reported the case of a eye was enucleated. Radiological examination of 28-year-old Chinese who had a perforated eye with the skull showed no orbital involvement, and chest tumour mass completely filling it. This paper x-rays were normal. Postoperative recovery was reports the case of a young black African girl who uneventful. -

Retinoblastoma Simulators
Retinoblastoma: Atypical Presentation & Simulators Dr. Njambi Ombaba; Paediatric Ophthalmologist, University of Nairobi Objectives • To review of typical presentation of retinoblastoma • To understand the atypical presentation • To understand the Rb simulators Presentation of retinoblastoma Growth patterns Endophytic: Inner retina, vitreous mass, no overlying vessels, pseudohypopyon Exophytic: Outer retina, SR space mass, overlying vessels, RD Diffuse: No mass, signs of inflammation/ endophthalmitis Echogenic soft tissue mass Variable shadowing – calcification Persistent on reduced gain Heterogeneous – necrosis/ haemorrhage Floating debris- vitreous seeds, increased globulin MRI- • Pre-treatment staging T1- Hyper intense to vitreous T2-Hypo intense to vitreous T1:C+Gd- homo/ heterogeneous Enhancement: Choroid & AC ON involvement Hypo intense sclera- Normal Trilateral retinoblastoma CT SCAN Typically a mass of high density Usually calcified and moderately enhancing on iodinated contrast CT has a sensitivity of 81–96%, and a higher specificity for calcification detection However, delineation of intraocular soft-tissue detail is limited. Low sensitivity for ON invasion Atypical presentation Non calcified Retinoblastoma Calcification is key to diagnosis retinoblastoma US detects calcifications in 92–95% of positive cases Non-calcified retinoblastomas: 1. Tumefaction with irregular internal structure 2. Medium reflectivity 3. Typical signs of vascularity 4. Retinal detachment with part of the retinal surface destroyed. Rare, 2% of all -

ICO Residency Curriculum 2Nd Edition and Updated Community Eye Health Section
ICO Residency Curriculum 2nd Edition and Updated Community Eye Health Section The International Council of Ophthalmology (ICO) Residency Curriculum offers an international consensus on what residents in ophthalmology should be taught. While the ICO curriculum provides a standardized content outline for ophthalmic training, it has been designed to be revised and modified, with the precise local detail for implementation left to the region’s educators. Download the Curriculum from the ICO website: icoph.org/curricula.html. www.icoph.org Copyright © International Council of Ophthalmology 2016. Adapt and translate this document for your noncommercial needs, but please include ICO credit. All rights reserved. First edition 201 6 . First edition 2006, second edition 2012, Community Eye Health Section updated 2016. International Council of Ophthalmology Residency Curriculum Introduction “Teaching the Teachers” The International Council of Ophthalmology (ICO) is committed to leading efforts to improve ophthalmic education to meet the growing need for eye care worldwide. To enhance educational programs and ensure best practices are available, the ICO focuses on "Teaching the Teachers," and offers curricula, conferences, courses, and resources to those involved in ophthalmic education. By providing ophthalmic educators with the tools to become better teachers, we will have better-trained ophthalmologists and professionals throughout the world, with the ultimate result being better patient care. Launched in 2012, the ICO’s Center for Ophthalmic Educators, educators.icoph.org, offers a broad array of educational tools, resources, and guidelines for teachers of residents, medical students, subspecialty fellows, practicing ophthalmologists, and allied eye care personnel. The Center enables resources to be sorted by intended audience and guides ophthalmology teachers in the construction of web-based courses, development and use of assessment tools, and applying evidence-based strategies for enhancing adult learning. -

Successful Treatment of Ciliary Body Medulloepithelioma with Intraocular
Stathopoulos et al. BMC Ophthalmology (2020) 20:239 https://doi.org/10.1186/s12886-020-01512-y CASE REPORT Open Access Successful treatment of ciliary body medulloepithelioma with intraocular melphalan chemotherapy: a case report Christina Stathopoulos*, Marie-Claire Gaillard, Julie Schneider and Francis L. Munier Abstract Background: Intraocular medulloepithelioma is commonly treated with primary enucleation. Conservative treatment options include brachytherapy, local resection and/or cryotherapy in selected cases. We report for the first time the use of targeted chemotherapy to treat a ciliary body medulloepithelioma with aqueous and vitreous seeding. Case presentation: A 17-month-old boy with a diagnosis of ciliary body medulloepithelioma with concomitant seeding and neovascular glaucoma in the right eye was seen for a second opinion after parental refusal of enucleation. Examination under anesthesia showed multiple free-floating cysts in the pupillary area associated with iris neovascularization and a subluxated and notched lens. Ultrasound biomicroscopy revealed a partially cystic mass adjacent to the ciliary body between the 5 and 9 o’clock meridians as well as multiple nodules in the posterior chamber invading the anterior vitreous inferiorly. Fluorescein angiography demonstrated peripheral retinal ischemia. Left eye was unremarkable. Diagnosis of intraocular medulloepithelioma with no extraocular invasion was confirmed and conservative treatment initiated with combined intracameral and intravitreal melphalan injections given according to the previously described safety-enhanced technique. Ciliary tumor and seeding totally regressed after a total of 3 combined intracameral (total dose 8.1 μg) and intravitreal (total dose 70 μg) melphalan injections given every 7–10 days. Ischemic retina was treated with cryoablation as necessary. -

Download Report Appendixes [PDF · 224
Appendices Appendix A. Selected Internet Links Appendix Table A1. Internet links for radiotherapy organizations Organization URL address Deutsche Gesellschaft fur http://www.degro.org/jsp_public/cms/index.jsp Radiooncologie European Society for Therapeutic http://www.estroweb.org/estro/index.cfm Radiology and Oncology American Society for Therapeutic http://www.astro.org/ Radiology and Oncology National Association for Proton http://www.proton-therapy.org/ Therapy Particle Therapy Cooperative http://ptcog.web.psi.ch/ Group (Accessed June 16, 2008) Appendix Table A2. Internet links for particle beam instrumentation companies Company URL address Ion Beam Applications (IBA) http://www.iba-worldwide.com/ Solutions Still River Systems Inc http://www.stillriversystems.com/ Optivus Proton Therapy http://www.optivus.com/ Siemens http://www.medical.siemens.com/ Hitachi: Proton beam Therapy http://www.pi.hitachi.co.jp/rd-eng/product/industrial-sys/accelerator- sys/proton-therapy-sys/proton-beam-therapy/index.html ACCEL Instruments http://www.proton-therapy.com/ (Accessed June 16, 2008) Appendix Table A3. Internet links for particle beam treatment centers in the USA Center/Institute URL address Francis H. Burr Proton Therapy http://www.massgeneral.org/cancer/about/providers/radiation/proton/i Center (NPTC) ndex.asp Loma Linda University Proton http://www.llu.edu/proton/index.html Therapy Center University of California, Crocker http://media.cnl.ucdavis.edu/crocker/website/default.php Nuclear Lab Midwest Proton Radiotherapy http://www.mpri.org/ Institute, Bloomington M.D. Anderson Proton Therapy http://www.mdanderson.org/care_centers/radiationonco/ptc/ Center, Houston University of Florida Proton http://www.floridaproton.org/ Therapy Institute, Jacksonville (Accessed June 16, 2008) A-1 Appendix B. -

Ocular Oncology and Pathology 2018 Hot Topics in Ocular Pathology and Oncology— an Update
Ocular Oncology and Pathology 2018 Hot Topics in Ocular Pathology and Oncology— An Update Program Directors Patricia Chévez-Barrios MD and Dan S Gombos MD In conjunction with the American Association of Ophthalmic Oncologists and Pathologists McCormick Place Chicago, Illinois Saturday, Oct. 27, 2018 Presented by: The American Academy of Ophthalmology 2018 Ocular Oncology and Pathology Subspecialty Day Advisory Committee Staff Planning Group Daniel S Durrie MD Melanie R Rafaty CMP DES, Director, Patricia Chévez-Barrios MD Associate Secretary Scientific Meetings Program Director Julia A Haller MD Ann L’Estrange, Subspecialty Day Manager Dan S Gombos MD Michael S Lee MD Carolyn Little, Presenter Coordinator Program Director Francis S Mah MD Debra Rosencrance CMP CAE, Vice R Michael Siatkowski MD President, Meetings & Exhibits Former Program Directors Kuldev Singh MD MPH Patricia Heinicke Jr, Copy Editor 2016 Carol L Shields MD Mark Ong, Designer Maria M Aaron MD Gina Comaduran, Cover Designer Patricia Chévez-Barrios MD Secretary for Annual Meeting 2014 Hans E Grossniklaus MD Arun D Singh MD ©2018 American Academy of Ophthalmology. All rights reserved. No portion may be reproduced without express written consent of the American Academy of Ophthalmology. ii Planning Group 2018 Subspecialty Day | Ocular Oncology & Pathology 2018 Ocular Oncology and Pathology Planning Group On behalf of the American Academy of Ophthalmology and the American Association of Ophthalmic Oncologists and Pathologists, it is our pleasure to welcome you to Chicago and -

Medullo-Epithelioma (Diktyoma)Of The
Brit. J. Ophthal. (I 972) 56, 362 Br J Ophthalmol: first published as 10.1136/bjo.56.4.362 on 1 April 1972. Downloaded from Medullo-epithelioma (diktyoma) of the eye M. V. SIRSAT, S. S. SHRIKHANDE, AND M. B. SAMPAT Department of Pathology, Tata Memorial Hospital, Bombay, India A medullo-epithelioma (diktyoma) is a rare malignant tumour of the eye which arises from the unpigmented epithelium of the ciliary body; diktyoma of the optic nerve with intercranial extension has also been described (Reese, I963). The name diktyoma was given by Fuchs ( I908) to indicate the net-like appearance of the tumour. We have found fifty examples of diktyoma of the ciliary body, most of them in the German literature. Three cases have been reported from India (Kesavachar and Junnarkar, I960; Nirankari, Gulati, and Chaddah, I960; Shivde, Kher, and Junnarkar, I969). The case reported below is the first to be seen at the Tata Memorial Hospital, Bombay, during the last 30 years. copyright. Case report A Hindu male child aged 5 years had shown enlargement of the right eyeball for 3 weeks. There was no history of pain or of any past major illness. He was the third child, the other children being healthy and normal. http://bjo.bmj.com/ Examination The right eyeball was found to be enlarged, with dilated capillaries over the sclera. The visual acuity was diminished. The left eye showed no abnormality. The liver and spleen were not palpable. on September 27, 2021 by guest. Protected Radiology The bony orbital walls were intact. The right optic foramen was visible. -
Differential Diagnoses Symptoms and Other Useful Lists and Tables Signs for Ophthalmologists Case Presentations
Differential Diagnoses Symptoms and other Useful Lists and Tables Signs For Ophthalmologists Case Presentations Kenn Freedman MD PhD Department of Ophthalmology and Visual Sciences Texas Tech University Health Sciences Center Lubbock, Texas USA Acknowledgments and Disclaimer The differential diagnoses and lists contained herein are not meant to be exhaustive, but are to give in most cases the most common causes of many ocular / visual symptoms, signs and situations. Included also in these lists are also some less common, but serious conditions that must be “ruled-out”. These lists have been based on years of experience, and I am grateful for God’s help in developing them. I also owe gratitude to several sources* including Roy’s classic text on Ocular Differential Diagnosis. * Please see references at end of document This presentation, of course, will continue to be a work in progress and any concerns or suggestions as to errors or omissions or picture copyrights will be considered. Please feel free to contact me at [email protected] Kenn Freedman Lubbock, Texas - October 2018 Disclaimer: The diagnostic algorithm for the diagnosis and management of Ocular or Neurological Conditions contained in this presentation is not intended to replace the independent medical or professional judgment of the physician or other health care providers in the context of individual clinical circumstances to determine a patient’s care. Use of this Presentation The lists are divided into three main areas 1. Symptoms 2. Signs from the Eight Point Eye Exam 3. Common Situations and Case Presentations The index for all of the lists is given on the following 3 pages. -

Uveal Melanoma National Guidelines
Uveal Melanoma Guidelines – Draft for Consultation Uveal Melanoma National Guidelines Draft for public consulation June 2014 This project is the independent work of the Uveal Melanoma Guideline Development Group and is funded by Melanoma Focus (http://melanomafocus.com/) um_guideline_cons_draft_v2_23_6_14 Last saved by Nancy Turnbull Date 16 June 2014 Page 1 of 93 Uveal Melanoma Guidelines – Draft for Consultation Uveal Melanoma 1. Executive Summary ......................................................................................................................... 6 1.1 Care Pathway .......................................................................................................................... 6 1.2 Recommendations .................................................................................................................. 8 1.2.1 Patient Choice and Shared decision-making .................................................................. 8 1.2.2 Service Configuration ...................................................................................................... 8 1.2.3 General Guidance............................................................................................................ 8 1.2.4 Primary management ..................................................................................................... 9 1.2.5 Prognostication ............................................................................................................. 11 1.2.6 Surveillance .................................................................................................................. -

Uveal Melanoma National Guidelines
Uveal Melanoma Guidelines January 2015 Uveal Melanoma National Guidelines January 2015 Authors: Nathan P, Cohen V, Coupland S, Curtis K, Damato B, Evans J, Fenwick S, Kirkpatrick L, Li O, Marshall E, McGuirk K, Ottensmeier C, Pearce N, Salvi S, Stedman B, Szlosarek P, Turnbull N This project is the independent work of the Uveal Melanoma Guideline Development Group and is funded by Melanoma Focus (http://melanomafocus.com/) Page 1 of 112 Uveal Melanoma Guidelines January 2015 Uveal Melanoma 1. Executive Summary ......................................................................................................................... 6 1.1 Care Pathway .......................................................................................................................... 6 1.2 Recommendations ................................................................................................................ 10 1.2.1 Patient Choice and Shared decision-making ................................................................ 10 1.2.2 Service Configuration .................................................................................................... 10 1.2.3 General Guidance.......................................................................................................... 10 1.2.4 Primary management ................................................................................................... 11 1.2.5 Prognostication ............................................................................................................. 14