35 Extrarenal Passages
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

MALE REPRODUCTIVE SYSTEM Male Reproduc�Ve System
Human Anatomy Unit 3 MALE REPRODUCTIVE SYSTEM Male Reproducve System • Gonads = testes – primary organ responsible for sperm producon – development/ maintenance of secondary sex characteriscs • Gametes = sperm Male Reproducve System Anatomy of the Testes • Tunica albuginea • Seminiferous tubules – highly coiled – sealed by the blood tess barrier – Site of sperm producon • located in tescular lobules Anatomy of the Testes Histology of the Testes • Intersal cells of Leydig – Intersal endocrinocytes – Located between seminiferous tubules – testosterone • Sertoli cells – Nursing cells or sustentacular cells – form the blood tess barrier – support sperm development Development of Sperm • Sperm formed by two processes – meiosis • Cell division resulng in cells with genecally varied cells with only one complete set of DNA (remember…our cells have two complete sets!) – spermatogenesis • morphological changes as sperm develop in tubule system • 64 days in humans – Can survive 3 days in female reproducve tract Development of Sperm The Long and Winding Road… • Seminiferous tubules • Rete tess • Epididymis • Vas deferens • Ejaculatory duct • Prostac urethra • Membranous urethra • Penile urethra The Epididymis • Sperm “swim school” • Comma shaped organ that arches over the posterior and lateral side of the tess • Stores spermatozoa unl ejaculaon or absorpon • Sperm stored for up to 2 weeks Vas Deferens • Extends from the epididymis • Passes posterior to the urinary bladder • Meets the spermac blood vessels to become the spermac cord • Enters -

1 Male Checklist Male Reproductive System Components of the Male
Male Checklist Male Reproductive System Components of the male Testes; accessory glands and ducts; the penis; and reproductive system the scrotum. Functions of the male The male reproductive system produces sperm cells that reproductive system can be transferred to the female, resulting in fertilization and the formation of a new individual. It also produces sex hormones responsible for the normal development of the adult male body and sexual behavior. Penis The penis functions as the common outlet for semen (sperm cells and glandular secretions) and urine. The penis is also the male copulatory organ, containing tissue that can fill with blood resulting in erection of the penis. Prepuce A fold of skin over the distal end of the penis. Circumcision is the surgical removal of the prepuce. Corpus spongiosum A spongy body consisting of erectile tissue. It surrounds the urethra. Sexual excitement can cause erectile tissue to fill with blood. As a result, the penis becomes erect. Glans penis The expanded, distal end of the corpus spongiosum. It is also called the head of the penis. Bulb of the penis The proximal end of the corpus spongiosum. Bulbospongiosus muscle One of two skeletal muscles surrounding the bulb of the penis. At the end of urination, contraction of the bulbospongiosus muscles forces any remaining urine out of the urethra. During ejaculation, contractions of the bulbospongiosus muscles ejects semen from the penis. Contraction of the bulbospongiosus muscles compresses the corpus spongiosum, helping to maintain an erection. Corpus cavernosum One of two spongy bodies consisting of erectile tissue that (pl., corpora cavernosa) form the sides and front of the penis. -

The Reproductive System
27 The Reproductive System PowerPoint® Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska © 2012 Pearson Education, Inc. Introduction • The reproductive system is designed to perpetuate the species • The male produces gametes called sperm cells • The female produces gametes called ova • The joining of a sperm cell and an ovum is fertilization • Fertilization results in the formation of a zygote © 2012 Pearson Education, Inc. Anatomy of the Male Reproductive System • Overview of the Male Reproductive System • Testis • Epididymis • Ductus deferens • Ejaculatory duct • Spongy urethra (penile urethra) • Seminal gland • Prostate gland • Bulbo-urethral gland © 2012 Pearson Education, Inc. Figure 27.1 The Male Reproductive System, Part I Pubic symphysis Ureter Urinary bladder Prostatic urethra Seminal gland Membranous urethra Rectum Corpus cavernosum Prostate gland Corpus spongiosum Spongy urethra Ejaculatory duct Ductus deferens Penis Bulbo-urethral gland Epididymis Anus Testis External urethral orifice Scrotum Sigmoid colon (cut) Rectum Internal urethral orifice Rectus abdominis Prostatic urethra Urinary bladder Prostate gland Pubic symphysis Bristle within ejaculatory duct Membranous urethra Penis Spongy urethra Spongy urethra within corpus spongiosum Bulbospongiosus muscle Corpus cavernosum Ductus deferens Epididymis Scrotum Testis © 2012 Pearson Education, Inc. Anatomy of the Male Reproductive System • The Testes • Testes hang inside a pouch called the scrotum, which is on the outside of the body -

The Reproductive System Thethe Reproductivereproductive Systemsystem
The Reproductive System TheThe ReproductiveReproductive SystemSystem • Gonads – primary sex organs • Testes in males • Ovaries in females • Gonads produce gametes (sex cells) and secrete hormones • Sperm – male gametes • Ova (eggs) – female gametes Slide 16.1 MaleMale ReproductiveReproductive SystemSystem Figure 16.2 Slide 16 2c MaleMale ReproductiveReproductive SystemSystem • Testes • Duct system • Epididymis • Ductus deferens • Urethra Slide 16 2a MaleMale ReproductiveReproductive SystemSystem • Accessory organs • Seminal vesicle • Prostate gland • Bulbourethral gland • External genitalia • Penis • Scrotum Slide 16 2b MaleMale ReproductiveReproductive SystemSystem Figure 16.2 Slide 16 2c TestesTestes • Coverings of the testes • Tunica albuginea – capsule that surrounds each testis Figure 16.1 Slide 16 3a TestesTestes • Coverings of the testes (continued) • Septa – extensions of the capsule that extend into the testis and divide it into lobules Figure 16.1 Slide 16 3b TestesTestes • Each lobule contains one to four seminiferous tubules • Tightly coiled structures • Function as sperm-forming factories • Empty sperm into the rete testis • Sperm travels through the rete testis to the epididymis • Interstitial cells produce androgens such as testosterone Slide 16.4 EpididymisEpididymis • Comma-shaped, tightly coiled tube • Found on the superior part of the testis and along the posterior lateral side • Functions to mature and store sperm cells (at least 20 days) • Expels sperm with the contraction of muscles in the epididymis walls to the -

Urinary Tract Eod Stage & Treatment
2/20/2020 SHRI VIDEO TRAINING SERIES 2018 DX forward Recorded 2/2020 URINARY TRACT EOD STAGE & TREATMENT PRESENTED BY LORI SOMERS, RN IOWA CANCER REGISTRY 1 BLADDER C670‐C679 EOD PRIMARY TUMOR EOD REGIONAL LYMPH NODES EOD METASTASIS 2 1 2/20/2020 EOD • General Coding instructions, 32 pg pdf • https://seer.cancer.gov/tools/staging/2018‐ EOD‐General‐Instructions.pdf • Timing rules • What to include re clinical or path findings • Rules re neoadjuvant therapy • Discrepancies between op/path 3 BLADDER EOD PRI TUMOR • Note 1: Two main types of bladder cancer – Flat (sessile) • Called in situ when tumor has not penetrated basement membrane – Papillary type • Called noninvasive when tumor has not penetrated basement membrane 4 2 2/20/2020 EOD PRI TUMOR • Note 2: Noninvasive papillary transitional carcinoma: Pathologists use many descriptive terms for noninvasive papillary TCC. Frequently the path report does not contain a definitive statement of non‐invasion. – Non‐invasion can be inferred from microscopic description – List of terms in SEER*RSA schema 5 Definite statements non‐invasion ‘for papillary TCC’ • Noninfiltrating • Noninvasive • No evidence of invasion • No extension into lamina propria • No stromal invasion • No extension into underlying supporting tissue • Neg lamina propria and superficial muscle • Neg muscle and (subepithelial) connective tissue • No infiltrative behavior/component 6 3 2/20/2020 Inferred descriptions of non‐invasion ‘for papillary TCC’ • No involvement of musc propria and no mention of subepthelium/submucosa • No statement of invasion (microscopic description present • (Underlying) tissue insufficient to judge depth of invasion • No involvement of muscularis propria • Benign deeper tissue • Microscopic description problematic (non‐invas vs superficial invas) • Frond surfaced by transitional cell • No mural infiltration • No evid of invasion (no sampled stroma) • Confined to mucosa 7 EOD PRI TUMOR Note 3: Noninvasive (in situ) flat transitional cell carcinoma: . -

The Urinary System Dr
The urinary System Dr. Ali Ebneshahidi Functions of the Urinary System • Excretion – removal of waste material from the blood plasma and the disposal of this waste in the urine. • Elimination – removal of waste from other organ systems - from digestive system – undigested food, water, salt, ions, and drugs. + - from respiratory system – CO2,H , water, toxins. - from skin – water, NaCl, nitrogenous wastes (urea , uric acid, ammonia, creatinine). • Water balance -- kidney tubules regulate water reabsorption and urine concentration. • regulation of PH, volume, and composition of body fluids. • production of Erythropoietin for hematopoieseis, and renin for blood pressure regulation. Anatomy of the Urinary System Gross anatomy: • kidneys – a pair of bean – shaped organs located retroperitoneally, responsible for blood filtering and urine formation. • Renal capsule – a layer of fibrous connective tissue covering the kidneys. • Renal cortex – outer region of the kidneys where most nephrons is located. • Renal medulla – inner region of the kidneys where some nephrons is located, also where urine is collected to be excreted outward. • Renal calyx – duct – like sections of renal medulla for collecting urine from nephrons and direct urine into renal pelvis. • Renal pyramid – connective tissues in the renal medulla binding various structures together. • Renal pelvis – central urine collecting area of renal medulla. • Hilum (or hilus) – concave notch of kidneys where renal artery, renal vein, urethra, nerves, and lymphatic vessels converge. • Ureter – a tubule that transport urine (mainly by peristalsis) from the kidney to the urinary bladder. • Urinary bladder – a spherical storage organ that contains up to 400 ml of urine. • Urethra – a tubule that excretes urine out of the urinary bladder to the outside, through the urethral orifice. -

The Role of the External Sphincter
PARAPLEGIA REFERENCES Ross, J. COSBIE, GIBBON, N. O. K. & DAMANSKI, M. (1967). B.J.S. 54, NO. 7. STAMEY, T. (1968). J. Urol. 97, (May). VINCENT, S. A. (1959). Ulster med. Jour. 28, 176. VINCENT, S. A. (1960). Lancet, 2, 292. VINCENT, S. A. (1964). Dev. Med. and Child Neurol. 6, 23. VINCENT, S. A. (1966a). Lancet, Sept., 631-632. VINCENT, S. A. (1966b). Bio-Engineering, Sept., p. 1. THE ROLE OF THE EXTERNAL SPHINCTER By J. COSBIE Ross Director of Urological Studies, University of Liverpool Introduction. It must be acknowledged that as yet no one knows the precise role of the external sphincter and there should, by right, be a question mark after the word 'sphincter'. The problem is much more complex and obscure than the simple, easily understood mechanism of the anal sphincter. However, there is much that is already known, and perhaps recent work has shed some light on the problem. First, the traditional view. In the 32nd Edition of Gray's Anatomy (1958), the description is as follows. 'The sphincter urethrae surrounds the membranous portion of the urethra, and lies deep to the inferior fascia of the urogenital diaphragm. Its superficial or inferior fibres arise in front from the transverse perineal ligament and from the neighbouring fascia. They pass backwards on each side of the urethra and converge on the perineal body for their insertion. Its deep fibres, some of which arise from the fascial sheath of the pudendal vessels and pass medially, form a continuous circular investment for the membranous urethra.' Actions. 'The muscles of both sides act together as a sphincter, compressing the membranous part of the urethra. -
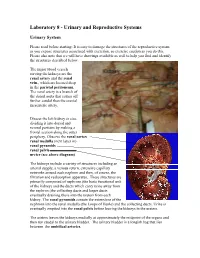
Laboratory 8 - Urinary and Reproductive Systems
Laboratory 8 - Urinary and Reproductive Systems Urinary System Please read before starting: It is easy to damage the structures of the reproductive system as you expose structures associated with excretion, so exercise caution as you do this. Please also note that we will have drawings available as well to help you find and identify the structures described below. The major blood vessels serving the kidneys are the Renal renal artery and the renal pyramid vein., which are located deep in the parietal peritoneum. The renal artery is a branch of the dorsal aorta that comes off Renal further caudal than the cranial pelvis mesenteric artery. Dissect the left kidney in situ, dividing it into dorsal and ventral portions by making a frontal section along the outer periphery. Observe the renal cortex renal medulla (next layer in) renal pyramids renal pelvis ureter (see above diagram) The kidneys include a variety of structures including an arterial supply, a venous return, extensive capillary networks around each nephron and then, of course, the filtration and reabsorption apparatus. These structures are primarily composed of nephrons (the basic functional unit of the kidney) and the ducts which carry urine away from the nephron (the collecting ducts and larger ducts eventually draining these into the ureters from each kidney. The renal pyramids contain the extensions of the nephrons into the renal medulla (the Loops of Henle) and the collecting ducts. Urine is eventually emptied into the renal pelvis before leaving the kidneys in the ureters. The ureters leaves the kidneys medially at approximately the midpoint of the organs and then run caudal to the urinary bladder. -

Transperineal Ultrasound As a Reliable Tool in the Assessment Of
www.nature.com/scientificreports OPEN Transperineal ultrasound as a reliable tool in the assessment of membranous urethra length in radical prostatectomy patients Kania Piotr1, Mieleszko Rafał1, Kuligowski Marcin1, Dudka Karol1, Kuca Monika1, Biedrzycki Jakub1, Zwolan Bartosz1, Dmowski Tadeusz1 & Salagierski Maciej 2* To evaluate the usefulness of transperineal ultrasound (TPUS) as a method of membranous urethra length (MUL) measurement and investigate whether preoperative (MULpre) and postoperative (MULpost) would be associated with the degree and time of urinary continence recovery after laparoscopic radical prostatectomy (LRP). 84 patients who underwent LRP between January 2017 and December 2018 were selected for fnal analysis. All patients had preoperative and postoperative measurement of MUL in TPUS. Urinary continence was defned as no pad or a safety pad. Recovery of continence was assessed at 1, 3, 6 and 12 months after catheter removal. We prospectively analyzed correlation of MULpre, MULpost and a percent change in membranous urethral length (MULratio) with the urinary continence status. 69 (82%) patients regained continence in the follow-up of 12 months. MULpre, MULpost and MULratio assessed in TPUS were larger in subgroups of patients who regained continence earlier and in the entire continent group. Spearman rank test showed strong correlations between MULpost and MULratio (R—0.6 and R—0.56, respectively, p < 0.0001) with the time to continence recovery in the cumulative 12 months follow-up. TPUS allowed a reliable measurement of MUL before and after LRP. MULpre, MULpost as well as MULratio are related with time to regain continence and recovery rate after LRP. Sparing longest possible sphincteric urethra, with respect to oncological outcomes is a key factor in recovering continence after prostate cancer surgery. -

Anatomy and Blood Supply of the Urethra and Penis J
3 Anatomy and Blood Supply of the Urethra and Penis J. K.M. Quartey 3.1 Structure of the Penis – 12 3.2 Deep Fascia (Buck’s) – 12 3.3 Subcutaneous Tissue (Dartos Fascia) – 13 3.4 Skin – 13 3.5 Urethra – 13 3.6 Superficial Arterial Supply – 13 3.7 Superficial Venous Drainage – 14 3.8 Planes of Cleavage – 14 3.9 Deep Arterial System – 15 3.10 Intermediate Venous System – 16 3.11 Deep Venous System – 17 References – 17 12 Chapter 3 · Anatomy and Blood Supply of the Urethra and Penis 3.1 Structure of the Penis surface of the urogenital diaphragm. This is the fixed part of the penis, and is known as the root of the penis. The The penis is made up of three cylindrical erectile bodies. urethra runs in the dorsal part of the bulb and makes The pendulous anterior portion hangs from the lower an almost right-angled bend to pass superiorly through anterior surface of the symphysis pubis. The two dor- the urogenital diaphragm to become the membranous solateral corpora cavernosa are fused together, with an urethra. 3 incomplete septum dividing them. The third and smaller corpus spongiosum lies in the ventral groove between the corpora cavernosa, and is traversed by the centrally 3.2 Deep Fascia (Buck’s) placed urethra. Its distal end is expanded into a conical glans, which is folded dorsally and proximally to cover the The deep fascia penis (Buck’s) binds the three bodies toge- ends of the corpora cavernosa and ends in a prominent ther in the pendulous portion of the penis, splitting ven- ridge, the corona. -

Urinary System: Summary Stage 2018 Coding Manual V2.0
URINARY SYSTEM BLADDER, RENAL PELVIS AND URETERS ANATOMIC STRUCTURES Table of Anatomic Structures MUCOSA MUSCULARIS PRIMARY SITE -Epithelium SEROSA PROPRIA -Lamina propria submucosa Yes, on superior Bladder (C67_) Yes Yes surface Renal pelvis (C659) Yes Yes No Ureter (C669) Yes Yes No The layers of the urinary tract include: 1. The EPITHELIAL LAYER contains no blood vessels or lymphatics 2. The BASEMENT MEMBRANE, a sheet of extracellular material, functions as a filtration barrier and a boundary involved in generating and maintaining tissue structure 3. The LAMINA PROPRIA, composed of areolar connective tissue, contains blood vessels, nerves, and, in some regions, glands. Once tumor has broken through the basement membrane into the lamina propria, it can spread by way of the lymphatics and blood vessels to other parts of the body 4. The urinary sites do NOT have a MUSCULARIS MUCOSAE, and, therefore, the lamina propria and the submucosa are difficult to separate. These terms are used interchangeably 5. The SUBMUCOSA is a thick layer of either dense or areolar connective tissue. It contains blood vessels, lymphatic vessels, nerves, and, in some regions, glands 6. The MUSCULARIS PROPRIA is composed of multiple layers of muscle tissue; it constitutes the wall of the organ 7. The SEROSA, the outermost layer covering, is a serous membrane, part of the visceral peritoneum. It covers only the superior surface of the bladder. There is no serosa on the renal pelvis or ureters. a. Where there is no serosa, the connective tissue of surrounding structures merges with the connective tissue of the urinary organs and is called ADVENTITIA. -

URINARY SYSTEM Components
Human Anatomy Unit 3 URINARY SYSTEM Components • Kidneys • Ureters • Urinary bladder • Urethra Funcons • Storage of urine – Bladder stores up to 1 L of urine • Excreon of urine – Transport of urine out of body • Regulaon: – Plasma pH – Blood volume/pressure – Plasma ion concentraons (Ca2+, Na+, K+, CL-) – Assist liver in detoxificaon, amino acid metabolism Kidney Gross Anatomy • Retroperitoneal – Anterior surface covered with peritoneum – Posterior surface directly against posterior abdominal wall • Superior surface at about T12 • Inferior surface at about L3 • Ureters enter urinary bladder posteriorly • LeT kidney 2cm superior to right – Size of liver Structure of the Kidney • Hilum = the depression along the medial border through which several structures pass – renal artery – renal vein – ureter – renal nerves Surrounding Tissue • Fibrous capsule – Innermost layer of dense irregular CT – Maintains shape, protec:on • Adipose capsule – Adipose ct of varying thickness – Cushioning and insulaon • Renal fascia – Dense irregular CT – Anchors kidney to peritoneum & abdominal wall • Paranephric fat – Outermost, adipose CT between renal fascia and peritoneum Frontal Sec:on of the Kidney • Cortex – Layer of renal :ssue in contact with capsule – Renal columns – parts of cortex that extend into the medulla between pyramids • Medulla – Striped due to renal tubules • Renal pyramids – 8-15 present in medulla of adult – Conical shape – Wide base at cor:comedullary juncon Flow of Filtrate/Urine • Collec:ng ducts – Collect from mul:ple nephrons • Minor calyx – Collect from each pyramid • Major calyx – Collect from minor calyx • Renal pelvis – Collects from calyces, passes onto • Ureter – Collects from pelvis • Urinary Bladder – Collects from ureters Histology Renal Cortex Renal Medulla Renal Tubules • Nephron – func:onal unit of the kidney.