1. Pathology of Cellular Injury and Death 1
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

General Pathologic Anatomy
МІНІСТЕРСТВО ОХОРОНИ ЗДОРОВ'Я УКРАЇНИ Харківський національний медичний університет GENERAL PATHOLOGIC ANATOMY Manual for practical classes in pathomorphology for English-speaking teachers ЗАГАЛЬНА ПАТОЛОГІЧНА АНАТОМІЯ Методичні розробки до занять з патоморфології для англомовних викладачів медичних закладів Затверджено вченою радою ХНМУ. Протокол № 15 від 15.06.2017. Харків ХНМУ 2017 1 General pathologic anatomy : мanual for practical classes in patho- morphology for English-speaking teachers / comp. I. V. Sorokina, V. D. Markovskiy, I. V. Korneyko et al. – Kharkov : KNMU, 2017. – 64 p. Compilers I. V. Sorokina V. D. Markovskiy I. V. Korneyko G. I. Gubina-Vakulik V. V. Gargin O. N. Pliten M. S. Myroshnychenko S. N. Potapov T. V. Bocharova D. I. Galata O.V. Kaluzhina Загальна патологічна анатомія : метод. розроб. до занять з пато- морфології для англомовних викладачів мед. закладів / упоряд. І. В. Сорокіна, В. Д. Марковський, І. В. Корнейко та ін. – Харків : ХНМУ, 2017. – 64 с. Упорядники I. В. Сорокіна В. Д. Марковський І. В. Корнейко Г. І. Губіна-Вакулик В. В. Гаргін О. М. Плітень М. С. Мирошниченко С. М. Потапов Т. В. Бочарова Д. І. Галата О. В. Калужина 2 Foreword Pathomorphology, one of the most important medical subjects is aimed at teaching students understanding material basis and mechanisms of the development of main pathological processes and diseases. This manual published as separate booklets is devoted to general pathological processes as well as separate nosological forms. It is intended to the English-medium students of the medical and dentistry faculties. It can be used as additional material used for individual work in class. It can also be used to master the relevant terminology and its unified teaching. -

Heart Failure • Cor Pulmonale • Hypertensive Heart Disease
DISEASES OF THE HEART - content • Cardiac hypertrophy and congestive heart failure • Cor pulmonale • Hypertensive heart disease • Ischemic heart disease • Valvular diseases • Myocardial diseases • Congenital heart diseases • Diseases of the pericardium • Cardiac neoplasms Normal values assessed by echocardiography • Free wall thickness: RV: 3-4 mm, LV: 10-11 mm • End-diastolic volume (EDV) 120 ml • End-systolic volume (ESV) 50 ml • Stroke volume (SV) 70 ml Weight: women: 300 gs, men: 350 gs HYPERTROPHY OF THE HEART • The cardiac myocytes are permanent cells (not able to enter the cell cycle) and, therefore, are not able to proliferate • Increase in work load increase in size and pumping capacity of ventricular myocytes • Weight > 400 g • Types: concentric dilative Concentric hypertrophy Pathogenesis An obstruction of outflow in systole (i.e., hypertension, aortic valve stenosis) the LV increases the end-systolic pressure pressure overload concentric remodeling and hypertrophy Morphologic features of concentric hypertrophy of LV: small lumen; markedly increased wall thickness (> 20 mm); increased mass (> 500 g) Clinical features of pressure-overloaded LV - symptomless for a long period - pump failure occurs lately - risk of sudden cardiac death Dilative hypertrophy Pathogenesis Aortic/mitral valve incompetence leads to diastolic backflow the regurgitated extra volume of blood is accepted with the dilation of the LV an increased EDV is ejected into the circulation during the next systole (volume overload) excentric remodeling and -
Pathology.Pre-Test.Pdf
Pathology PreTestTMSelf-Assessment and Review Notice Medicine is an ever-changing science. As new research and clinical experience broaden our knowledge, changes in treatment and drug therapy are required. The authors and the publisher of this work have checked with sources believed to be reliable in their efforts to provide information that is complete and generally in accord with the standards accepted at the time of publication. However, in view of the possibility of human error or changes in medical sciences, neither the authors nor the publisher nor any other party who has been involved in the preparation or publication of this work warrants that the information contained herein is in every respect accurate or complete, and they disclaim all responsibility for any errors or omissions or for the results obtained from use of the information contained in this work. Readers are encouraged to confirm the information contained herein with other sources. For example, and in particular, readers are advised to check the product information sheet included in the package of each drug they plan to administer to be certain that the information contained in this work is accurate and that changes have not been made in the recommended dose or in the contraindications for administration. This recommendation is of particular importance in connection with new or infrequently used drugs. Pathology PreTestTMSelf-Assessment and Review Twelfth Edition Earl J. Brown, MD Associate Professor Department of Pathology Quillen College of Medicine Johnson City, Tennessee New York Chicago San Francisco Lisbon London Madrid Mexico City Milan New Delhi San Juan Seoul Singapore Sydney Toronto Copyright © 2007 by The McGraw-Hill Companies, Inc. -

Coronary Thrombosis
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1935 Coronary thrombosis Joseph F. Linsman University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Linsman, Joseph F., "Coronary thrombosis" (1935). MD Theses. 568. https://digitalcommons.unmc.edu/mdtheses/568 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. -------- Ii CORONARY THROMBOSIS A ~ri:NIOR THESIS BY JOSEPH FRANCIS LINS~Mill College of Medicine, University ot N&hraska 'f "" Table of Contents Pages Introduction------------------------------------------- i-iii Historical Review ----------'...-----------------------------1-7 Ineidene• ----------------------------------------------- 8-11 Etiological Factors------------------------------------ 12-22 Relationship to Arteriosclerosis Relationship to Angina Pectoris Relationship to F.ypertension Relationship to Diabetes Relationship to Syphilis Relationship to Heredity, Physical Type, Work, Weight, and Habits Relationship to Other Diseases Pathogenesis and Pathology----------------------------23-34 SymptollS and Signs------------------------------------35-58 -
Human Pathology Slide Sets
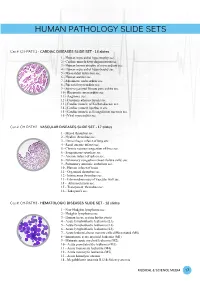
HUMAN PATHOLOGY SLIDE SETS Cat #: CH-PATH1 - CARDIAC DISEASES SLIDE SET - 16 slides 1 - Human myocardial hypertrophy sec. 2 - Cardiac muscle fatty degeneration sec. 3 - Human brown atrophy of myocardium sec. 4 - Human myocardial hypertrophy sec. 5 - Myocardial infarction sec. 6 - Human aortitis sec. 7 - Rheumatic endocarditis sec. 8 - Bacterial myocarditis sec. 9 - Semi-organized fibrous pericarditis sec. 10 - Rheumatic myocarditis sec. 11 - Angioma sec. 12 - Coronary atherosclerosis sec. 13 - Cardiac muscle of Keshan disease sec. 14 - Cardiac muscle lipofuscin sec. 15 - Cardiac muscle cell coagulation necrosis sec. 16 - Viral myocarditis sec. Cat #: CH-PATH2 - VASCULAR DISEASES SLIDE SET - 17 slides 1 - Mixed thrombus sec. 2 - Hyaline thrombus sec. 3 - Hemorrhagic infarct of lung sec. 4 - Renal anemic infarct sec. 5 - Chronic venous congestion of liver sec. 6 - Sanguineous apoplexy sec. 7 - Anemic infarct of spleen sec. 8 - Pulmonary congestion (heart-failure cells) sec. 9 - Pulmonary amniotic embolism sec. 10 - Human infarct of brain 11 - Organized thrombus sec. 12 - Intravenous thrombus sec. 13 - Fibrinoid necrosis of vascular wall sec. 14 - Atherosclerosis sec. 15 - Transparent thrombus sec. 16 - Takayasu's sec. Cat #: CH-PATH3 - HEMATOLOGIC DISEASES SLIDE SET - 12 slides 1 - Non-Hodgkin lymphoma sec. 2 - Hodgkin lymphoma sec. 3 - Human tissue system histiocytosis 4 - Acute lymphoblastic leukemia (L1) 5 - Acute lymphoblastic leukemia (L2) 6 - Acute lymphoblastic leukemia (L3) 7 - Acute leukemia bone marrow cells differentiated (M0) 8 - Immaturate acute myeloid leukemia (M1) 9 - Maturate acute myeloid leukemia (M2) 10 - Acute promyelocytic leukemia (M3) 11 - Acute monocytic leukemia (M4) 12 - Acute monocytic leukemia (M5) 13 - Acute hemolytic anemia 14 - Megaloblastic anaemia B12 deficiency anemia MEDICAL & SCIENCE MEDIA 17 Cat #: CH-PATH4 - URINARY DISEASES SLIDE SET - 27 slides 1 - Vitreous degeneration of renal arteriole sec. -

Hemodynamic Disorders Edema Elephantiasis
5/15/2020 Edema Hemodynamic Disorders • Excess accumulation of fluid in interstitial space or in serous cavity is called edema. • Types – Local edema Dr. Sadequel Islam Talukder – Generalized edema MBBS, M Phil (Pathology 1995, IPGMR) 5/15/2020 Sadequel Talukder, www.talukderbd.com 1 5/15/2020 Sadequel Talukder, www.talukderbd.com 2 • Generalized edema • Local edema – Hepatic edema – Acute inflammatory edema – Cardiac edema – Allergic edema – Renal edema – Edema due to impaired venous return of leg following – Nutritional deficiency edema • Long journey – Pregnancy edema • Long period of standing – Myxedema – Lymphedema following lymphatic obstruction – Unexplained edema • e.g. Filariasis 5/15/2020 Sadequel Talukder, www.talukderbd.com 3 5/15/2020 Sadequel Talukder, www.talukderbd.com 4 Elephantiasis • Clinical Types of Edema – Pitting edema • A non-pitting edema following lymphtaic – Non-pitting edema obstruction • Causes of edema/Pathophysiological Category • Accumulation of lymph in tissue – Increased hydrostatic pressure • Causes inflammation, fibrosis. – Decreased colloidal osmotic pressure • Fibrosis causes non-pitting edema. – Retention of salt and water – Lymphatic obstruction 5/15/2020 Sadequel Talukder, www.talukderbd.com 5 5/15/2020 Sadequel Talukder, www.talukderbd.com 6 1 5/15/2020 • Serous cavities – Peritoneal cavity - Excess accumulation of fluid is • All causes are found in hepatic edema called ascites. • Normally interstitial space and serous cavity – Pleural cavity - Excess accumulation of fluid is contains small amount of fluid. Excess amount called pleural effusion. of fluid cases edema. – Pericardial cavity - Excess accumulation of fluid is called pericardial effusion. – Synovial cavity - Excess accumulation of fluid is called synovial effusion. 5/15/2020 Sadequel Talukder, www.talukderbd.com 7 5/15/2020 Sadequel Talukder, www.talukderbd.com 8 • Anasarca – Severe generalized edema is called • Fluid comes out from vessels due to anasarca. -

Status of the Myocardium and Infarct-Related Coronary Artery in 19 Necropsy Patients with Acute Recanalization Using Pharmacolog
JACC Vol. 9. No. 4 785 April I<J 87:785- 80 I MORPHOLOGIC STUDIES Status of the Myocardium and Infarct-Related Coronary Artery in 19 Necropsy Patients With Acute Recanalization Using Pharmacologic (Streptokinase, r-Tissue Plasminogen Activator), Mechanical (Percutaneous Transluminal Coronary Angioplasty) or Combined Types of Reperfusion Therapy BRUCE F. WALLER, MD, FACC,* DONALD A. ROTHBAUM, MD, FACC,t CASS A. PINKERTON, MD, FACC,t MICHAEL J. COWLEY, MD, FACC,§ THOMAS J. LlNNEMElER, MD, FACC,t CHARLES ORR, MD, FACC,t MICHAEL IRONS, MD,t ROBIN A. HELMUTH , MD,II EDWARD R. WILLS, MD,II CHARLES AUST, MOil Indianapolis. Indiana and Richmond. Virginia In acute myocardial infarction, myocardial salvage is 14 (74%) had hemorrhagic myocardial infarction and dependent on rapid restoration of blood flow. Phar they all received pharmacologic or combined forms of macologic (streptokinase, recombinant tissue-type plas reperfusion therapy. The remaining five patients (26%) minogen activator), mechanical (percutaneous translu had nonhemorrhagic (anemic) infarction and were treated minal coronary angioplasty, guide wire perforation) or with balloon angioplasty therapy alone. Increased lu combined forms of reperfusion therap y can accomplish minal cross-sectional area was present in 8 of 9 patients this goal, but their effects on infarcted myocardium and with acute balloon angioplasty but severe coronary ath vessel occlusion site have not been compared at necropsy. erosclerotic plaque remained in 9 of 10 patients without The heart of 19 necropsy patients who had received var acute balloon angioplasty. Severe hemorrhage sur ious forms of acute reperfusion therap y was studied: rounded angioplasty sites in all four patients who also 14 had pharmacologic or combined forms of reperfusion received streptokinase or tissue-type plasminogen acti therapy (13 streptokinase and I tissue-type plasminogen vator. -

Annals of Surgery
ANNALS OF SURGERY Vol. 171 April 1970 No. 4 Neurological Complications of Carotid Artery Surgery JAi s E. BLAiN, M.D., RiciLuA D. CHAPMAN, M.D., EDWIN J. WYLIE, M.D., F.A.C.S. From the Department of Surgery, University of California School of Medicine, San Francisco, California POSTOPERATIVE stroke is the most fre- rological deficit or acute progression of an quent and most disastrous complication of old deficit occurred after 55 (9%) of these cerebrovascular reconstructive surgery. Pa- operations. In most instances postoperative tients who undergo operation on the ca- neurological deficits, when viewed retro- rotid arteries are particularly vulnerable. spectively, resulted from an unwise deci- Since prevention of stroke is the primary sion to operate or an error in surgical man- objective of most carotid artery operations, agement. In three additional patients the technics to prevent it at the time of opera- postoperative deficit was merely a gradual tion are of paramount importance. Post- progression of a preoperative deficit and operative neurological deficits in our pa- was not related to the operation. A tabula- tients who had carotid operations were re- tion of the severity of the deficits and the viewed to determine causes and to assess ultimate neurological status of the patients the value of methods designed to prevent is shown in Table 1. Visual disturbances, these deficits. dysphagia, and monoparesis are examples Six hundred thirteen endarterectomies of deficits classified as mild. Under moder- for occlusive or ulcerating lesions at the ate deficits we included hemiparesis. Se- carotid bifurcation were performed in 488 vere deficit was applied to complete uni- patients between October, 1958 and June, lateral paralysis (hemiplegia) with or 1969. -

17. Vascular Pathology III. Heart Failure 1
17. Vascular pathology III. Heart failure DISEASES OF THE HEART Content Cardiac hypertrophy and congestive heart failure Cor pulmonale Hypertensive heart disease Ischemic heart disease Valvular diseases Myocardial diseases Congenital heart diseases Diseases of the pericardium Cardiac neoplasms HYPERTROPHY OF THE HEART AND HEART FAILURE Normal values assessed by echocardiography Free wall thickness: RV: 3-4 mm, LV:10-11 mm End-diastolic volume (EDV) 120 ml, end-systolic volume (ESV) 50 ml, stroke volume (SV) 70 ml Weight: women: 300 gs, men: 350 gs Hypertrophy of the heart The cardiac myocytes are permanent cells (not able to enter the cell cycle) and, therefore, are not able to proliferate Increase in work load increase in size and pumping capacity of ventricular myocytes Weight > 400 g Types: concentric or dilative Concentric hypertrophy Pathogenesis An obstruction of outflow in systole (i.e., hypertension, aortic valve stenosis) the LV increases the end-systolic pressure pressure overload concentric remodeling and hypertrophy Morphology Concentric hypertrophy of the LV: small lumen; markedly increased wall thickness (> 20 mm); increased mass (> 500 g) Clinical features of pressure-overloaded LV Symptomless for a long period Pump failure occurs lately Risk of sudden cardiac death Dilative hypertrophy Pathogenesis Aortic/mitral valve incompetence leads to diastolic backflow the regurgitated extra volume of blood is accepted with the dilation of the LV an increased EDV is ejected into the circulation during the -

Inhalt 11..23
Contents 1 Fundamentals of Pathology Pathology .............................. 2 Signs of Death .......................... 5 Methods Equivocal Signs of Death Brain Death Disease ................................ 5 Unequivocal Signs of Death Etiology Causal Pathogenesis Statistics ............................... 5 Formal Pathogenesis Clinical Course Autopsy ................................ 5 2 Cellular Pathology Nuclear Lesions ........................ 6 Inclusions ............................. 12 Forms of Nuclei Amorphous inclusions Chromosomes Crystalline inclusions Particulate inclusions DNA Repair Defects ..................... 6 Xeroderma pigmentosum Oncofetal Lesion ....................... 12 Ribosome-lamellae complexes Chromosome Abnormalities .............. 6 Annulated lamellae layers Change in the Size of the Nucleus ........ 8 Mitochondria-lamellar-layer complexes Relation of Nucleus to Cytoplasm Nuclear Euploidy Lesions of the Smooth Endoplasmic Nuclear Polyploidy Nuclear Aneuploidy Reticulum (SER) ...................... 14 Chromatin Change ...................... 8 Quantitative Change ................... 14 Heterochromatin Condensation Proliferation of SER Dyskaryosis Atrophy of the SER Perinuclear Hyperchromatosis Morphologic Change ................... 14 Karyolysis Formation of Vesicles in the SER Inclusions .............................. 8 „Cytoplasmic Nuclei“ Cytoplasmic inclusions Inclusions ............................. 14 Paraplasmic inclusions Change in the Number of Nuclei ......... 10 Golgi Lesions ........................ -

Vascular Pathology in the Aged Human Brain
Acta Neuropathol (2010) 119:277–290 DOI 10.1007/s00401-010-0652-7 REVIEW Vascular pathology in the aged human brain Lea Tenenholz Grinberg • Dietmar Rudolf Thal Received: 24 June 2009 / Revised: 3 February 2010 / Accepted: 4 February 2010 / Published online: 14 February 2010 Ó The Author(s) 2010. This article is published with open access at Springerlink.com Abstract Cerebral atherosclerosis (AS), small vessel lesions (WMLs) and lacunar infarcts. In this review, we disease (SVD), and cerebral amyloid angiopathy (CAA) demonstrate the relationship between AS, SVD, and CAA are the most prevalent arterial disorders in the aged brain. as well as their contribution to the development of vascular Pathogenetically, AS and SVD share similar mechanisms: tissue lesions and we emphasize an important role for apoE plasma protein leakage into the vessel wall, accumulation in the pathogenesis of vessel disorders and vascular tissue of lipid-containing macrophages, and fibrosis of the vessel lesions as well as for BBB dysfunction on WML and wall. CAA, on the other hand, is characterized by the lacunar infarct development. deposition of the amyloid b-protein in the vessel wall. Despite these differences between CAA, AS and SVD, Keywords Atherosclerosis Á Small vessel disease Á apolipoprotein E (apoE) is involved in all three disorders. Cerebral amyloid angiopathy Á Brain infarction Á Such a pathogenetic link may explain the correlations Hemorrhages Á White matter lesions between AS, SVD, CAA, and Alzheimer’s disease in the brains of elderly individuals reported in the literature. In addition, AS, SVD, and CAA can lead to tissue lesions Introduction such as hemorrhage and infarction. -

Pathology of Cellular Injury and Death. Cellular Adaptations
What is disease? • A condition in which the presence of an abnormality causes a loss of normal health • Manifests in signs and symptoms subjective: e.g., pain objective: confirmed by diagnostic tests • Duration of disease: short lasting - acute long lasting - chronic • Outcome: varies; can be lethal What is pathology? • The study (logos) of suffering (pathos) • Devoted to the study of - the cause of the disease (etiology) - the mechanism(s) of disease development (pathogenesis) - the structural alterations induced in cells and tissues by the disease (morphologic change) - the functional consequences of the morphologic changes (clinical significance) • The morphologic change can be focal (localized abnormality) or diffuse Teaching program of pathology for medical students General pathology • Basic reactions of cells and tissues to abnormal stimuli, i.e. common features of various disease processes in various cells and tissues Systematic pathology • The descriptions of specific diseases as they affect given organs or organ systems The descriptions and terms used are the basis of medical language Students are expected to attend the lectures, the autopsy and histopathology practicals, and the organ demonstrations. Attendance at the practicals the attendence is always verified. There is no possibility for missed practicals to be repeated later. Students who are absent from more than 25% of the practicals, automatically fail the semester. The grade achieved in the fall-semester examinations will be calculated from the sum of the following: - the first mid-term assessment (maximum 5 points) - the second mid-term assessment (max. 5 points) - the histology examination (max. 5 points) - the autopsy examination (max. 5 points) - the final test (max.