Roles for the Uptake 2 Transporter OCT3 in Regulation Of
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Biased Allosteric Regulation of the Prostaglandin F2α Receptor: From
Biased Allosteric Regulation of the Prostaglandin F2 Receptor: From Small Molecules to Large Receptor Complexes By Eugénie Goupil Department of Pharmacology and Therapeutics McGill University, Montréal, Canada November, 2012 A thesis submitted to McGill in partial fulfillment of the requirements of the degree of Doctor of philosophy Copyright ©Eugénie Goupil, 2012 ''In theory, there is no difference between theory and practice. In practice, there is.'' -Lawrence Peter ''Yogi'' Berra ii Abstract G protein-coupled receptors (GPCRs) represent the largest family of cell surface receptors, and thus some of the most important targets for drug discovery. By binding to the orthosteric site where endogenous ligands bind, agonists and antagonists differentially modulate signals sent downstream from these receptors. New evidence suggests that GPCRs possess topographically distinct or allosteric binding sites, which may differentially modulate agonist- and antagonist-mediated responses to selectively affect distinct signalling pathways coupled to the same receptor. These sites may either positively or negatively regulate receptor activity, depending on the pathway in question, and thus can act as biased ligands, leading to functional selectivity (or ligand-directed signalling). Another way of allosterically regulating GPCR signalling is through receptor oligomerization, which has recently emerged as a common mechanism for regulating receptor function. The GPCR for prostaglandin F2 FP, is implicated in many important physiological responses, such as parturition, smooth muscle cell contraction and blood pressure regulation. Therefore, evaluating the potential use of allosteric modulators of FP to fine-tune PGF2-mediated signals, as well as generating a better understanding of its putative oligomerization partners would be of significant pharmacological and clinical interest. -

Methylphenidate Amplifies the Potency and Reinforcing Effects Of
ARTICLE Received 1 Aug 2013 | Accepted 7 Oct 2013 | Published 5 Nov 2013 DOI: 10.1038/ncomms3720 Methylphenidate amplifies the potency and reinforcing effects of amphetamines by increasing dopamine transporter expression Erin S. Calipari1, Mark J. Ferris1, Ali Salahpour2, Marc G. Caron3 & Sara R. Jones1 Methylphenidate (MPH) is commonly diverted for recreational use, but the neurobiological consequences of exposure to MPH at high, abused doses are not well defined. Here we show that MPH self-administration in rats increases dopamine transporter (DAT) levels and enhances the potency of MPH and amphetamine on dopamine responses and drug-seeking behaviours, without altering cocaine effects. Genetic overexpression of the DAT in mice mimics these effects, confirming that MPH self-administration-induced increases in DAT levels are sufficient to induce the changes. Further, this work outlines a basic mechanism by which increases in DAT levels, regardless of how they occur, are capable of increasing the rewarding and reinforcing effects of select psychostimulant drugs, and suggests that indivi- duals with elevated DAT levels, such as ADHD sufferers, may be more susceptible to the addictive effects of amphetamine-like drugs. 1 Department of Physiology and Pharmacology, Wake Forest University School of Medicine, Winston-Salem, North Carolina 27157, USA. 2 Department of Pharmacology and Toxicology, University of Toronto, Toronto, Ontario, Canada M5S1A8. 3 Department of Cell Biology, Medicine and Neurobiology, Duke University Medical Center, Durham, North Carolina 27710, USA. Correspondence and requests for materials should be addressed to S.R.J. (email: [email protected]). NATURE COMMUNICATIONS | 4:2720 | DOI: 10.1038/ncomms3720 | www.nature.com/naturecommunications 1 & 2013 Macmillan Publishers Limited. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

Differentially Affect Monoamine Transporters and Abuse Liability
Neuropsychopharmacology (2017) 42, 1950–1961 © 2017 American College of Neuropsychopharmacology. All rights reserved 0893-133X/17 www.neuropsychopharmacology.org N-Alkylated Analogs of 4-Methylamphetamine (4-MA) Differentially Affect Monoamine Transporters and Abuse Liability Ernesto Solis Jr1, John S Partilla2, Farhana Sakloth3, Iwona Ruchala4, Kathryn L Schwienteck5, 4 4 3 5 *,2 Louis J De Felice , Jose M Eltit , Richard A Glennon , S Stevens Negus and Michael H Baumann 1In Vivo Electrophysiology Unit, Behavioral Neuroscience Research Branch, Intramural Research Program, National Institute on Drug Abuse, National Institutes of Health, Baltimore, MD, USA; 2Designer Drug Research Unit, Intramural Research Program, National Institute on Drug Abuse, 3 National Institutes of Health, Baltimore, MD, USA; Department of Medicinal Chemistry, Virginia Commonwealth University, Richmond, VA, USA; 4 5 Department of Physiology and Biophysics, Virginia Commonwealth University, Richmond, VA, USA; Department of Pharmacology and Toxicology, Virginia Commonwealth University, Richmond, VA, USA Clandestine chemists synthesize novel stimulant drugs by exploiting structural templates known to target monoamine transporters for dopamine, norepinephrine, and serotonin (DAT, NET, and SERT, respectively). 4-Methylamphetamine (4-MA) is an emerging drug of – abuse that interacts with transporters, but limited structure activity data are available for its analogs. Here we employed uptake and release assays in rat brain synaptosomes, voltage-clamp current measurements in cells expressing transporters, and calcium flux assays in cells coexpressing transporters and calcium channels to study the effects of increasing N-alkyl chain length of 4-MA on interactions at DAT, NET, and SERT. In addition, we performed intracranial self-stimulation in rats to understand how the chemical modifications affect abuse liability. -

Phencyclidine: an Update
Phencyclidine: An Update U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES • Public Health Service • Alcohol, Drug Abuse and Mental Health Administration Phencyclidine: An Update Editor: Doris H. Clouet, Ph.D. Division of Preclinical Research National Institute on Drug Abuse and New York State Division of Substance Abuse Services NIDA Research Monograph 64 1986 DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Alcohol, Drug Abuse, and Mental Health Administratlon National Institute on Drug Abuse 5600 Fishers Lane Rockville, Maryland 20657 For sale by the Superintendent of Documents, U.S. Government Printing Office Washington, DC 20402 NIDA Research Monographs are prepared by the research divisions of the National lnstitute on Drug Abuse and published by its Office of Science The primary objective of the series is to provide critical reviews of research problem areas and techniques, the content of state-of-the-art conferences, and integrative research reviews. its dual publication emphasis is rapid and targeted dissemination to the scientific and professional community. Editorial Advisors MARTIN W. ADLER, Ph.D. SIDNEY COHEN, M.D. Temple University School of Medicine Los Angeles, California Philadelphia, Pennsylvania SYDNEY ARCHER, Ph.D. MARY L. JACOBSON Rensselaer Polytechnic lnstitute National Federation of Parents for Troy, New York Drug Free Youth RICHARD E. BELLEVILLE, Ph.D. Omaha, Nebraska NB Associates, Health Sciences Rockville, Maryland REESE T. JONES, M.D. KARST J. BESTEMAN Langley Porter Neuropsychiatric lnstitute Alcohol and Drug Problems Association San Francisco, California of North America Washington, D.C. DENISE KANDEL, Ph.D GILBERT J. BOTV N, Ph.D. College of Physicians and Surgeons of Cornell University Medical College Columbia University New York, New York New York, New York JOSEPH V. -

Monoamine Reuptake Inhibitors in Parkinson's Disease
Hindawi Publishing Corporation Parkinson’s Disease Volume 2015, Article ID 609428, 71 pages http://dx.doi.org/10.1155/2015/609428 Review Article Monoamine Reuptake Inhibitors in Parkinson’s Disease Philippe Huot,1,2,3 Susan H. Fox,1,2 and Jonathan M. Brotchie1 1 Toronto Western Research Institute, Toronto Western Hospital, University Health Network, 399 Bathurst Street, Toronto, ON, Canada M5T 2S8 2Division of Neurology, Movement Disorder Clinic, Toronto Western Hospital, University Health Network, University of Toronto, 399BathurstStreet,Toronto,ON,CanadaM5T2S8 3Department of Pharmacology and Division of Neurology, Faculty of Medicine, UniversitedeMontr´ eal´ and Centre Hospitalier de l’UniversitedeMontr´ eal,´ Montreal,´ QC, Canada Correspondence should be addressed to Jonathan M. Brotchie; [email protected] Received 19 September 2014; Accepted 26 December 2014 Academic Editor: Maral M. Mouradian Copyright © 2015 Philippe Huot et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The motor manifestations of Parkinson’s disease (PD) are secondary to a dopamine deficiency in the striatum. However, the degenerative process in PD is not limited to the dopaminergic system and also affects serotonergic and noradrenergic neurons. Because they can increase monoamine levels throughout the brain, monoamine reuptake inhibitors (MAUIs) represent potential therapeutic agents in PD. However, they are seldom used in clinical practice other than as antidepressants and wake-promoting agents. This review article summarises all of the available literature on use of 50 MAUIs in PD. The compounds are divided according to their relative potency for each of the monoamine transporters. -

Lysergic Acid Diethylamide (LSD) Promotes Social Behavior Through Mtorc1 in the Excitatory Neurotransmission
Lysergic acid diethylamide (LSD) promotes social behavior through mTORC1 in the excitatory neurotransmission Danilo De Gregorioa,b,1, Jelena Popicb,2,3, Justine P. Ennsa,3, Antonio Inserraa,3, Agnieszka Skaleckab, Athanasios Markopoulosa, Luca Posaa, Martha Lopez-Canula, He Qianzia, Christopher K. Laffertyc, Jonathan P. Brittc, Stefano Comaia,d, Argel Aguilar-Vallese, Nahum Sonenbergb,1,4, and Gabriella Gobbia,f,1,4 aNeurobiological Psychiatry Unit, Department of Psychiatry, McGill University, Montreal, QC, Canada, H3A 1A1; bDepartment of Biochemistry, McGill University, Montreal, QC, Canada, H3A 1A3; cDepartment of Psychology, McGill University, Montreal, QC, Canada, H3A 1B1; dDivision of Neuroscience, Vita Salute San Raffaele University, 20132 Milan, Italy; eDepartment of Neuroscience, Carleton University, Ottawa, ON, Canada, K1S 5B6; and fMcGill University Health Center, Montreal, QC, Canada, H3A 1A1 Contributed by Nahum Sonenberg, November 10, 2020 (sent for review October 5, 2020; reviewed by Marc G. Caron and Mark Geyer) Clinical studies have reported that the psychedelic lysergic acid receptor (6), but also displays affinity for the 5-HT1A receptor diethylamide (LSD) enhances empathy and social behavior (SB) in (7–9). Several studies have demonstrated that LSD modulates humans, but its mechanism of action remains elusive. Using a glutamatergic neurotransmission and, indirectly, the α-amino- multidisciplinary approach including in vivo electrophysiology, 3-hydroxy-5-methyl-4-isoxazole propionate (AMPA) receptors. optogenetics, behavioral paradigms, and molecular biology, the Indeed, in vitro studies have shown that LSD increased the ex- effects of LSD on SB and glutamatergic neurotransmission in the citatory response of interneurons in the piriform cortex following medial prefrontal cortex (mPFC) were studied in male mice. -

Narcolepsy: Current Treatment Options and Future Approaches
REVIEW Narcolepsy: current treatment options and future approaches Michel Billiard Abstract: The management of narcolepsy is presently at a turning point. Three main avenues Department of Neurology, Gui de are considered in this review: 1) Two tendencies characterize the conventional treatment of Chauliac Hospital, Montpellier, France narcolepsy. Modafi nil has replaced methylphenidate and amphetamine as the fi rst-line treat- ment of excessive daytime sleepiness (EDS) and sleep attacks, based on randomized, double blind, placebo-controlled clinical trials of modafi nil, but on no direct comparison of modafi nil versus traditional stimulants. For cataplexy, sleep paralysis, and hypnagogic hallucinations, new antidepressants tend to replace tricyclic antidepressants and selective serotonin reuptake inhibitors (SSRIs) in spite of a lack of randomized, double blind, placebo-controlled clinical trials of these compounds; 2) The conventional treatment of narcolepsy is now challenged by sodium oxybate, the sodium salt of gammahydroxybutyrate, based on a series of randomized, double-blind, placebo-controlled clinical trials and a long-term open label study. This treatment has a fairly good effi cacy and is active on all symptoms of narcolepsy. Careful titration up to an adequate level is essential both to obtain positive results and avoid adverse effects; 3) A series of new treatments are currently being tested, either in animal models or in humans, They include novel stimulant and anticataplectic drugs, endocrine therapy, and, more attractively, -

Disease-Induced Modulation of Drug Transporters at the Blood–Brain Barrier Level
International Journal of Molecular Sciences Review Disease-Induced Modulation of Drug Transporters at the Blood–Brain Barrier Level Sweilem B. Al Rihani 1 , Lucy I. Darakjian 1, Malavika Deodhar 1 , Pamela Dow 1 , Jacques Turgeon 1,2 and Veronique Michaud 1,2,* 1 Tabula Rasa HealthCare, Precision Pharmacotherapy Research and Development Institute, Orlando, FL 32827, USA; [email protected] (S.B.A.R.); [email protected] (L.I.D.); [email protected] (M.D.); [email protected] (P.D.); [email protected] (J.T.) 2 Faculty of Pharmacy, Université de Montréal, Montreal, QC H3C 3J7, Canada * Correspondence: [email protected]; Tel.: +1-856-938-8697 Abstract: The blood–brain barrier (BBB) is a highly selective and restrictive semipermeable network of cells and blood vessel constituents. All components of the neurovascular unit give to the BBB its crucial and protective function, i.e., to regulate homeostasis in the central nervous system (CNS) by removing substances from the endothelial compartment and supplying the brain with nutrients and other endogenous compounds. Many transporters have been identified that play a role in maintaining BBB integrity and homeostasis. As such, the restrictive nature of the BBB provides an obstacle for drug delivery to the CNS. Nevertheless, according to their physicochemical or pharmacological properties, drugs may reach the CNS by passive diffusion or be subjected to putative influx and/or efflux through BBB membrane transporters, allowing or limiting their distribution to the CNS. Drug transporters functionally expressed on various compartments of the BBB involve numerous proteins from either the ATP-binding cassette (ABC) or the solute carrier (SLC) superfamilies. -

Antidepressant Potential of Nitrogen-Containing Heterocyclic Moieties: an Updated Review
Review Article Antidepressant potential of nitrogen-containing heterocyclic moieties: An updated review Nadeem Siddiqui, Andalip, Sandhya Bawa, Ruhi Ali, Obaid Afzal, M. Jawaid Akhtar, Bishmillah Azad, Rajiv Kumar Department of ABSTRACT Pharmaceutical Chemistry, Depression is currently the fourth leading cause of disease or disability worldwide. Antidepressant is Faculty of Pharmacy, Jamia Hamdard approved for the treatment of major depression (including paediatric depression), obsessive-compulsive University, Hamdard disorder (in both adult and paediatric populations), bulimia nervosa, panic disorder and premenstrual Nagar, New Delhi - dysphoric disorder. Antidepressant is a psychiatric medication used to alleviate mood disorders, such as 110 062, India major depression and dysthymia and anxiety disorders such as social anxiety disorder. Many drugs produce an antidepressant effect, but restrictions on their use have caused controversy and off-label prescription a Address for correspondence: risk, despite claims of superior efficacy. Our current understanding of its pathogenesis is limited and existing Dr. Sandhya Bawa, E-mail: sandhyabawa761@ treatments are inadequate, providing relief to only a subset of people suffering from depression. Reviews of yahoo.com literature suggest that heterocyclic moieties and their derivatives has proven success in treating depression. Received : 08-02-11 Review completed : 15-02-11 Accepted : 17-02-11 KEY WORDS: Antidepressant, depression, heterocyclic epression is a chronic, recurring and potentially life- monoamine oxidase inhibitors (MAOIs, e.g. Nardil®) tricyclic D threatening illness that affects up to 20% of the population antidepressants (TCAs, e.g. Elavil). They increases the synaptic across the globe.[1] The etiology of the disease is suboptimal concentration of either two (5-HT and NE) or all three (5-HT, concentrations of the monoamine neurotransmitters serotonin NE and dopamine (DA)) neurotransmitters. -
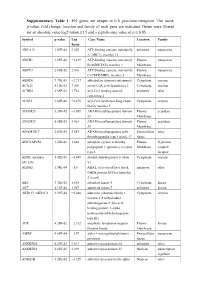
Supplementary Table 1
Supplementary Table 1. 492 genes are unique to 0 h post-heat timepoint. The name, p-value, fold change, location and family of each gene are indicated. Genes were filtered for an absolute value log2 ration 1.5 and a significance value of p ≤ 0.05. Symbol p-value Log Gene Name Location Family Ratio ABCA13 1.87E-02 3.292 ATP-binding cassette, sub-family unknown transporter A (ABC1), member 13 ABCB1 1.93E-02 −1.819 ATP-binding cassette, sub-family Plasma transporter B (MDR/TAP), member 1 Membrane ABCC3 2.83E-02 2.016 ATP-binding cassette, sub-family Plasma transporter C (CFTR/MRP), member 3 Membrane ABHD6 7.79E-03 −2.717 abhydrolase domain containing 6 Cytoplasm enzyme ACAT1 4.10E-02 3.009 acetyl-CoA acetyltransferase 1 Cytoplasm enzyme ACBD4 2.66E-03 1.722 acyl-CoA binding domain unknown other containing 4 ACSL5 1.86E-02 −2.876 acyl-CoA synthetase long-chain Cytoplasm enzyme family member 5 ADAM23 3.33E-02 −3.008 ADAM metallopeptidase domain Plasma peptidase 23 Membrane ADAM29 5.58E-03 3.463 ADAM metallopeptidase domain Plasma peptidase 29 Membrane ADAMTS17 2.67E-04 3.051 ADAM metallopeptidase with Extracellular other thrombospondin type 1 motif, 17 Space ADCYAP1R1 1.20E-02 1.848 adenylate cyclase activating Plasma G-protein polypeptide 1 (pituitary) receptor Membrane coupled type I receptor ADH6 (includes 4.02E-02 −1.845 alcohol dehydrogenase 6 (class Cytoplasm enzyme EG:130) V) AHSA2 1.54E-04 −1.6 AHA1, activator of heat shock unknown other 90kDa protein ATPase homolog 2 (yeast) AK5 3.32E-02 1.658 adenylate kinase 5 Cytoplasm kinase AK7 -

Sex Differences in Serotonergic and Dopaminergic Mediation of LSD Discrimination in Rats
Western Michigan University ScholarWorks at WMU Dissertations Graduate College 8-2017 Sex Differences in Serotonergic and Dopaminergic Mediation of LSD Discrimination in Rats Keli A. Herr Western Michigan University, [email protected] Follow this and additional works at: https://scholarworks.wmich.edu/dissertations Part of the Psychology Commons Recommended Citation Herr, Keli A., "Sex Differences in Serotonergic and Dopaminergic Mediation of LSD Discrimination in Rats" (2017). Dissertations. 3170. https://scholarworks.wmich.edu/dissertations/3170 This Dissertation-Open Access is brought to you for free and open access by the Graduate College at ScholarWorks at WMU. It has been accepted for inclusion in Dissertations by an authorized administrator of ScholarWorks at WMU. For more information, please contact [email protected]. SEX DIFFERENCES IN SEROTONERGIC AND DOPAMINERGIC MEDIATION OF LSD DISCRIMINATION IN RATS by Keli A Herr A dissertation submitted to the Graduate College in partial fulfillment of the requirements for the degree of Doctor of Philosophy Psychology Western Michigan University August 2017 Doctoral Committee: Lisa Baker, Ph.D., Chair Cynthia Pietras, Ph.D. Heather McGee, Ph.D. Missy Peet, Ph.D. SEX DIFFERENCES IN SEROTONERGIC AND DOPAMINERGIC MEDIATION OF LSD DISCRIMINATION IN RATS Keli A. Herr, Ph.D. Western Michigan University After decades of opposition, a resurgence of interest in the psychotherapeutic potential of LSD is gaining acceptance in the medical community. Future acceptance of LSD as a psychotherapeutic adjuvant may be predicated on knowledge about its neural mechanisms of action. Preclinical drug discrimination assay offers an invaluable model to determine the neural mechanisms underlying LSD’s interoceptive stimulus effects.