Keepthebeatconference 2014
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Heart Disease in Children.Pdf
Heart Disease in Children Richard U. Garcia, MD*, Stacie B. Peddy, MD KEYWORDS Congenital heart disease Children Primary care Cyanosis Chest pain Heart murmur Infective endocarditis KEY POINTS Fetal and neonatal diagnosis of congenital heart disease (CHD) has improved the out- comes for children born with critical CHD. Treatment and management of CHD has improved significantly over the past 2 decades, allowing more children with CHD to grow into adulthood. Appropriate diagnosis and treatment of group A pharyngitis and Kawasaki disease in pe- diatric patients mitigate late complications. Chest pain, syncope, and irregular heart rhythm are common presentations in primary care. Although typically benign, red flag symptoms/signs should prompt a referral to car- diology for further evaluation. INTRODUCTION The modern incidence of congenital heart disease (CHD) has been reported at 6 to 11.1 per 1000 live births.1,2 The true incidence is likely higher because many miscar- riages are due to heart conditions incompatible with life. The unique physiology of CHD, the constantly developing nature of children, the differing presenting signs and symptoms, the multiple palliative or corrective surgeries, and the constant devel- opment of new strategies directed toward improving care in this population make pe- diatric cardiology an exciting field in modern medicine. THE FETAL CIRCULATION AND TRANSITION TO NEONATAL LIFE Cardiovascular morphogenesis is a complex process that transforms an initial single- tube heart to a 4-chamber heart with 2 separate outflow tracts. Multiple and Disclosure Statement: All Authors take responsibility for all aspects of the reliability and freedom from bias of the information presented and their discussed interpretation. -

Chest Pain in Children and Adolescents Surendranath R
Article cardiology Chest Pain in Children and Adolescents Surendranath R. Veeram Objectives After completing this article, readers should be able to: Reddy, MD,* Harinder R. Singh, MD* 1. Enumerate the most common causes of chest pain in pediatric patients. 2. Differentiate cardiac chest pain from that of noncardiac cause. 3. Describe the detailed evaluation of a pediatric patient who has chest pain. Author Disclosure 4. Screen and identify patients who require a referral to a pediatric cardiologist or other Drs Veeram Reddy specialist. and Singh have 5. Explain the management of the common causes of pediatric chest pain. disclosed no financial relationships relevant Case Studies to this article. This Case 1 commentary does not During an annual physical examination, a 12-year-old girl complains of intermittent chest contain a discussion pain for the past 5 days that localizes to the left upper sternal border. The pain is sharp and of an unapproved/ stabbing, is 5/10 in intensity, increases with deep breathing, and lasts for less than 1 minute. investigative use of a The patient has no history of fever, cough, exercise intolerance, palpitations, dizziness, or commercial product/ syncope. On physical examination, the young girl is in no pain or distress and has normal vital signs for her age. Examination of her chest reveals no signs of inflammation over the sternum device. or rib cage. Palpation elicits mild-to-moderate tenderness over the left second and third costochondral junctions. The patient reports that the pain during the physical examination is similar to the chest pain she has experienced for the past 5 days. -

Chest Pain in Pediatrics
PEDIATRIC CARDIOLOGY 0031-3955/99 $8.00 + .OO CHEST PAIN IN PEDIATRICS Keith C. Kocis, MD, MS Chest pain is an alarming complaint in children, leading an often frightened and concerned family to a pediatrician or emergency room and commonly to a subsequent referral to a pediatric cardiologist. Because of the well-known associ- ation of chest pain with significant cardiovascular disease and sudden death in adult patients, medical personnel commonly share heightened concerns over pediatric patients presenting with chest pain. Although the differential diagnosis of chest pain is exhaustive, chest pain in children is least likely to be cardiac in origin. Organ systems responsible for causing chest pain in children include*: Idiopathic (12%-85%) Musculoskeletal (15%-31%) Pulmonary (12%-21%) Other (4%-21%) Psychiatric (5%-17%) Gastrointestinal (4'/0-7%) Cardiac (4%4%) Furthermore, chest pain in the pediatric population is rareZy associated with life-threatening disease; however, when present, prompt recognition, diagnostic evaluation, and intervention are necessary to prevent an adverse outcome. This article presents a comprehensive list of differential diagnostic possibilities of chest pain in pediatric patients, discusses the common causes in further detail, and outlines a rational diagnostic evaluation and treatment plan. Chest pain, a common complaint of pediatric patients, is often idiopathic in etiology and commonly chronic in nature. In one study,67 chest pain accounted for 6 in 1000 visits to an urban pediatric emergency room. In addition, chest pain is the second most common reason for referral to pediatric cardiologist^.^, 23, 78 Chest pain is found equally in male and female patients, with an average *References 13, 17, 23, 27, 32, 35, 44, 48, 49, 63-67, 74, and 78. -

Identifying and Treating Chest Pain
Identifying and Treating Chest Pain The Congenital Heart Collaborative Cardiac Chest Pain University Hospitals Rainbow Babies & Children’s Hospital Chest pain due to a cardiac condition is rare in children and and Nationwide Children’s Hospital have formed an innovative adolescents, with a prevalence of less than 5 percent. The affiliation for the care of patients with congenital heart disease cardiac causes of chest pain include inflammation, coronary from fetal life to adulthood. The Congenital Heart Collaborative insufficiency, tachyarrhythmias, left ventricular outflow tract provides families with access to one of the most extensive and obstruction and connective tissue abnormalities. experienced heart teams – highly skilled in the delivery of quality clinical services, novel therapies and a seamless continuum of care. Noncardiac Chest Pain Noncardiac chest pain is, by far, the most common cause of chest pain in children and adolescents, accounting for 95 percent of Pediatric Chest Pain concerns. Patients are often unnecessarily referred to a pediatric In pediatrics, chest pain has a variety of symptomatic levels and cardiologist for symptoms. This causes increased anxiety and causes. It can range from a sharp stab to a dull ache; a crushing distress within the family. Noncardiac causes of chest pain are or burning sensation; or even pain that travels up to the neck, musculoskeletal, pulmonary, gastrointestinal and miscellaneous. jaw and back. Chest pain can be cause for alarm in both patients The most common cause of chest pain in children and and parents, and it warrants careful examination and treatment. adolescents is musculoskeletal or chest-wall pain. Pediatric chest pain can be broadly classified as cardiac chest pain Reassurance, rest and analgesia are the primary treatments or noncardiac chest pain. -

Kounis Syndrome: a Forgotten Cause of References Chest Pain/ Cardiac Chest Pain in Children 1
382 Editöre Mektuplar Letters to the Editor Kounis syndrome: A forgotten cause of References chest pain/ Cardiac chest pain in children 1. Çağdaş DN, Paç FA. Cardiac chest pain in children. Anadolu Kardiyol Derg 2009;9:401-6. Kounis sendromu: Göğüs ağrısının unutulan bir sebebi/ 2. Coleman WL. Recurrent chest pain in children. Pediatr Clin North Am Çocuklarda kardiyak göğüs ağrısı 1984;31:1007-26. 3. Kounis NG. Kounis syndrome (allergic angina and allergic myocardial infarction): a natural paradigm? Int J Cardiol 2006; 7:7-14. Dear Editor, 4. Biteker M, Duran NE, Biteker F, Civan HA, Gündüz S, Gökdeniz T, et al. Kounis syndrome: first series in Turkish patients. Anadolu Kardiyol Derg I read with interest the article “Cardiac chest pain in children” by 2009;9:59-60. Çağdaş et al. (1) which has retrospectively evaluated 120 children 5. Biteker M. A new classification of Kounis syndrome. Int J Cardiol 2010 Jun admitted to a pediatric cardiology clinic with chest pain. Although chest 7. [Epub ahead of print]. pain in children is rarely reported to be associated with cardiac 6. Biteker M, Duran NE, Ertürk E, Aykan AC, Civan HA, et al. Kounis Syndrome diseases in the literature (2) authors have found that 52 of the patients secondary to amoxicillin/clavulanic acid use in a child. Int J Cardiol 2009;136:e3-5. (42.5%) had cardiac diseases and 28 (23.3%) of these patients’ cardiac 7. Biteker M, Ekşi Duran N, Sungur Biteker F, Ayyıldız Civan H, Kaya H, diseases were thought to directly cause their chest pain. -

Effectiveness of Screening for Life-Threatening Chest Pain in Children
Effectiveness of Screening for Life-Threatening Chest Pain in Children WHAT’S KNOWN ON THIS SUBJECT: Chest pain in children is an AUTHORS: Susan F. Saleeb, MD, Wing Yi V. Li, BA, Shira Z. extremely frequent complaint, with generally benign causes. Warren, BA, and James E. Lock, MD Referrals to cardiologists are increasing in volume, although the Department of Cardiology, Children’s Hospital Boston and frequency of cardiac causes is exceedingly low. Harvard Medical School, Harvard University, Boston, Massachusetts WHAT THIS STUDY ADDS: This study demonstrates that thorough KEY WORDS history assessments, physical examinations, and chest pain, standardized clinical assessment and management electrocardiograms can be used effectively in initial screening to plan, congenital heart disease determine when higher-level care and testing are needed. This ABBREVIATIONS technique allowed for no cardiac deaths over a 10-year period. CP—chest pain SCAMP—standardized clinical assessment and management plan ECG—electrocardiogram EST—exercise stress test SVT—supraventricular tachycardia abstract ICD-9—International Classification of Diseases, Ninth Revision www.pediatrics.org/cgi/doi/10.1542/peds.2011-0408 OBJECTIVE: We sought to determine the incidence of sudden cardiac doi:10.1542/peds.2011-0408 death among patients discharged from the cardiology clinic with pre- Accepted for publication Jul 29, 2011 sumed noncardiac chest pain (CP). Address correspondence to Susan F. Saleeb, MD, Children’s METHODS: The records of children Ͼ6 years of age who presented to Hospital Boston, Department of Cardiology, 300 Longwood Ave, Children’s Hospital Boston between January 1, 2000, and December 31, Boston, MA 02115. E-mail: [email protected] 2009, with a complaint of CP were reviewed for demographic features, PEDIATRICS (ISSN Numbers: Print, 0031-4005; Online, 1098-4275). -

Chest Pain in Children: It's Not All Heart • None
6/18/2019 Disclosures Chest Pain in Children: It's Not All Heart • none • Cathy S. Woodward, DNP, RN, PNP-AC • Professor of Pediatrics • UT Health -San Antonio Objectives Chest Pain •List the most common causes of benign chest pain in children. •Discuss the differential for children presenting with acute chest pain. •Describe the must-not-miss assessments in children with serious chest pain. Chest Pain Incidence of CP complaints •3700 kids evaluated for CP only 1% related to cardiac cause. •Musculoskeletal •Pulmonary •Gastrointestinal •Anxiety •Unknown cause 1 6/18/2019 Musculoskeletal CP •Brief sharp chest pain •Worse with deep breathing and movement •History of trauma, fall, new exercise, cough Musculoskeletal Causes of CP Slipping Rib Syndrome •31% of children who see cardiologists •Described in 1919 •Connective, bony and muscular tissue •Hypermobility of ant ends of ribs 8-10 •Precordial catch – short duration, unclear •Precipitating cause – cough, exercise, etiology trauma •Costochondritis •Pain acute and is reproducible •Trauma •Hooking maneuver • Slipping rib syndrome Pulmonary Causes of CP Pneumothorax •Chest Pain with •Asthma SOB •Pneumonia/Pleuritis •Trauma or •Chronic cough spontaneous •Pneumothorax •No breath •Acute Chest Syndrome sounds on affected side 2 6/18/2019 Acute Chest Syndrome Gastrointestinal Causes of CP •Major cause of morbidity and mortality for •Esophageal reflux – burning pain, center of children with Sickle Cell Disease – vaso chest, pain increased or decreased by certain occlusive crisis foods and body position -
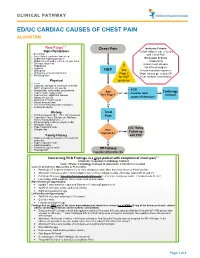
Ed/Uc Cardiac Causes of Chest Pain Algorithm
CLINICAL PATHWAY ED/UC CARDIAC CAUSES OF CHEST PAIN ALGORITHM 1,2 Red Flags Chest Pain Inclusion Criteria Signs/Symptoms Verbal children, age 2-22 yrs • Exertional with Chest Pain • Acute Onset, awakens from sleep • Substernal crushing pressure Exclusion Criteria • Radiation to shoulder, arm, neck, jaw, back Ill appearing • Syncope, dizziness Known heart disease • Palpitations • Dyspnea ! Hx of heart surgery • Orthopnea H&P See Known ingestion/exposure • Pulmonary embolus risk factors Page 2 Major trauma preceding CP • Illicit Drug Use for H&P Acute asthma exacerbation Physical guidance • Fever • Cyanosis, tachypnea, shortness of breath, WOB, abnormal breath sounds • • ECG Bradycardia, tachycardia, dysrhythmia Any Cardiology • Hypertension, hypotension Yes • Consider other • New murmur, significant murmur Red Flags? Consult • Gallop, friction rub causes of chest pain • Abnormal 2nd heart sound • Distant heart sounds • Decreased femoral/peripheral pulses No • Peripheral edema History Treat • Arthritis/vasculitis (SLE, IBD, JIA, Kawasaki) • Connective Tissue Disease (ie. Marfans, Pain Ehlers-Danlos Syndrome…) • QT-prolonging meds (ex. psych meds) • Oncologic history • Hypercoagulable state D/C Home • Dyslipidemia Pain Yes Follow up Improved? Family History with PCP • Sudden unexplained death or MI under 40 years old • Hypercoagulable state No • Cardiomyopathy • Pulmonary hypertension Off Pathway • Prolonged QT Consider Alternative Dx Concerning ECG Findings in a >2yo patient with complaint of chest pain1,2 Anschutz: In-person Cardiology -

Transthoracic Echocardiography in Children – (0523)
Medical Coverage Policy Effective Date ............................................02/15/2021 Next Review Date ......................................02/15/2022 Coverage Policy Number .................................. 0523 Transthoracic Echocardiography in Children Table of Contents Related Coverage Resources Overview .............................................................. 1 eviCore Pediatric Cardiac Imaging Guideline Coverage Policy ................................................... 1 Transthoracic Echocardiography in Adults General Background ............................................ 6 Medicare Coverage Determinations .................. 24 Coding/Billing Information .................................. 24 References ........................................................ 61 INSTRUCTIONS FOR USE The following Coverage Policy applies to health benefit plans administered by Cigna Companies. Certain Cigna Companies and/or lines of business only provide utilization review services to clients and do not make coverage determinations. References to standard benefit plan language and coverage determinations do not apply to those clients. Coverage Policies are intended to provide guidance in interpreting certain standard benefit plans administered by Cigna Companies. Please note, the terms of a customer’s particular benefit plan document [Group Service Agreement, Evidence of Coverage, Certificate of Coverage, Summary Plan Description (SPD) or similar plan document] may differ significantly from the standard benefit plans upon which -

Cardiac Chest Pain in Children
Original Investigation Özgün Araştırma 401 Cardiac chest pain in children Çocuklarda kardiyak göğüs ağrısı Deniz N. Çağdaş, F. Ayşenur Paç Section of Pediatric Cardiology, Department of Pediatrics, Türkiye Yüksek İhtisas Education and Research Hospital, Ankara, Turkey ABSTRACT Objective: Chest pain (CP) is a common cause of referral to hospital, not always directly related with cardiac diseases (CD). We investigated the causes for cardiac CP in children. Methods: A hundred and twenty children, admitted consecutively to pediatric cardiology clinic with CP, were evaluated in two groups (5-12 and 13-16 age-group) in a cross-sectional and a retrospective way. Chest X-ray, electrocardiography, and echocardiography were performed. In case of necessity, 24-hour Holter monitoring, exercise stress test, tilt-table test were performed, and hemogram, serum glucose, electrolytes were evaluated. Statistical analysis was performed using Chi-square test and risk ratio [(Odds-ratio (OR, (95% CI)] in groups were evaluated. Results: Most children with CP were older. Cardiac diseases were established in 52 (42.5%) patients. Cardiac diseases, which may cause CP (aortic stenosis, mitral valve prolapse, arrhythmias, etc.) were found in 23.3% (n=28) of patients. Compared with the younger, the risk of structural CD was found to be 2.84 times higher (OR=2.84, 95%CI 1.24-6.48, p=0.011) and risk of arrhythmia was 3.53 times higher in the elder age group (OR=3.53, 95%CI 0.93-13.38, p=0.051). When all CD were evaluated, elder children were found to have 4.12 times more risk of having CD (OR=4.12, 95%CI 1.89-9.01, p<0.0001). -

Chest Pain in Children and Adolescents Surendranath R
Chest Pain in Children and Adolescents Surendranath R. Veeram Reddy and Harinder R. Singh Pediatrics in Review 2010;31;e1 DOI: 10.1542/pir.31-1-e1 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://pedsinreview.aappublications.org/content/31/1/e1 Pediatrics in Review is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since 1979. Pediatrics in Review is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, 60007. Copyright © 2010 by the American Academy of Pediatrics. All rights reserved. Print ISSN: 0191-9601. Downloaded from http://pedsinreview.aappublications.org/ by Ben Albert on October 15, 2012 Article cardiology Chest Pain in Children and Adolescents Surendranath R. Veeram Objectives After completing this article, readers should be able to: Reddy, MD,* Harinder R. Singh, MD* 1. Enumerate the most common causes of chest pain in pediatric patients. 2. Differentiate cardiac chest pain from that of noncardiac cause. 3. Describe the detailed evaluation of a pediatric patient who has chest pain. Author Disclosure 4. Screen and identify patients who require a referral to a pediatric cardiologist or other Drs Veeram Reddy specialist. and Singh have 5. Explain the management of the common causes of pediatric chest pain. disclosed no financial relationships relevant Case Studies to this article. This Case 1 commentary does not During an annual physical examination, a 12-year-old girl complains of intermittent chest contain a discussion pain for the past 5 days that localizes to the left upper sternal border. -
Syncope and Chest Pain in the Pediatric Patient
DISCLAIMER Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this photo and/or video. If you don’t want your photo taken, please let us know. Thank you! Please DO NOT disclose any Protected Health Information (PHI) PHI includes, but is not limited to: - Patient name - Date of birth - Address - Occupation - Name of patient’s friends/family - Other identifiable features, i.e. scars, tattoos, hair/eye color Syncope and Chest Pain in the Pediatric Patient The aim of this presentation is to educate the audience about chest pain and syncope in the pediatric patient Syncope and Chest Pain in the Pediatric Patient How to Evaluate, Treat, and Reassure Conflicts of Interest There are no conflicts of interest to display Learning Objectives • The participant should be able to • The participant should know when understand causes of chest pain it is appropriate to refer to a and syncope in the pediatric subspecialist. patient. • The participant should be able to • The participant should be able to outline a treatment plan for the elucidate a history, including patient and family. certain specifics that will clarify the • The participant should be able to likely cause of the symptom. reassure the family and patient • The participant should be able to about the causes of the syncope recognize pertinent positives and and/or chest pain. negatives in the exam which will help the diagnosis. • The participant should know what, if any, testing needs to be done.