Midbrain Infarction Causing Diplopia and Atypical Neurological Symptoms: an Abducens Palsy Review
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Sensorineural Hearing Loss Due to Vertebrobasilar Artery Ischemia
logy & N ro eu u r e o N p h f y o s l i a o l n o r Ohki, J Neurol Neurophysiol 2013, S8 g u y o J Journal of Neurology & Neurophysiology ISSN: 2155-9562 DOI: 10.4172/2155-9562.S8-005 ReviewResearch Article Article OpenOpen Access Access Sensorineural Hearing Loss Due to Vertebrobasilar Artery Ischemia– Illustrative Case and Literature Review Masafumi Ohki* Department of Otolaryngology, Saitama Medical Center, Japan Abstract Acute sensorineural hearing loss is commonly caused by peripheral vestibulocochlear disorders such as sudden deafness, Meniere’s disease, and Ramsay Hunt syndrome, but is rarely due to infarction of the vertebrobasilar artery. In this report, a case of right anterior inferior cerebellar artery syndrome presenting with sudden deafness and vertigo is described in order to feature acute sensorineural hearing loss due to vertebrobasilar artery ischemia, and sensorineural hearing loss due to vertebrobasilar artery ischemia is reviewed and discussed. A 79-year-old man presented with right acute sensorineural hearing loss preceded by occasional, minute-long periods of dizziness without cranial neural symptoms other than vestibulocochlear symptoms. Magnetic resonance imaging (MRI) revealed infarction of the right anterior inferior cerebellar artery territory. The vertebrobasilar artery supplies the vestibulocochlear organ, brainstem, and cerebellum, whose abnormalities are related to vestibulocochlear symptoms. Vertigo is a major symptom associated with vertebrobasilar artery ischemia. Further, acute sensorineural hearing loss is caused by hypoperfusion of the vertebrobasilar artery. Vertigo and/or acute sensorineural hearing loss could be a prodrome of subsequent infarction of the vertebrobasilar artery territory. The artery most often responsible for acute sensorineural hearing loss is the anterior inferior cerebellar artery, whereas ischemia of the basilar artery, the posterior inferior cerebellar artery, and the superior cerebellar artery rarely cause acute sensorineural hearing loss. -

“Plugged” Anterior Inferior Cerebellar Artery Aneurysm Causing Facial Palsy, Hearing Loss, and Subarachnoid Hemorrhage Treated by a Translabyrinthine Approach
Open Access Case Report DOI: 10.7759/cureus.12282 “Plugged” Anterior Inferior Cerebellar Artery Aneurysm Causing Facial Palsy, Hearing Loss, and Subarachnoid Hemorrhage Treated by a Translabyrinthine Approach Buqing Liang 1 , Thomas Brammeier 2 , Jason Huang 1 , Ethan A. Benardete 1 1. Neurosurgery, Baylor Scott & White Medical Center - Temple, Temple, USA 2. Otolaryngology, Baylor Scott & White Medical Center - Temple, Temple, USA Corresponding author: Ethan A. Benardete, [email protected] Abstract Anterior inferior cerebellar artery (AICA) aneurysms are rare, less than 1%-2% of all intracranial aneurysms. Aneurysms of the distal AICA are even less common and can present with hearing loss and facial paralysis because of their relationship with the internal auditory canal (IAC). A 65-year-old male was followed for fluctuating left facial weakness and left-sided hearing loss for over a year. Serial magnetic resonance imaging (MRI) scans showed a mass near the left IAC, thought to be a vestibular schwannoma. Just prior to his next clinic visit, the patient deteriorated suddenly from a subarachnoid hemorrhage. Cerebral angiography revealed a 5.5 mm saccular aneurysm at the distal left AICA, which was clip ligated via a translabyrinthine (TL) approach. The patient had a good functional outcome (modified Rankin Scale [mRS] 1) after 30 days despite persistent left facial weakness. Stable obliteration of the aneurysm was demonstrated by cerebral angiography postoperatively. Distal AICA aneurysms are rare and can have a similar presentation to tumors in the cerebellar pontine angle. Because of the unique anatomy of the distal AICA, open clip ligation via a TL approach is an effective method to secure these aneurysms. -

Posterior Circulation Stroke
Posterior Circulation Stroke Sheryl Martin-Schild, MD, PhD, FANA, FAHA Stroke Medical Director for Louisiana Emergency Response Network (LERN) Medical Director of Neurology & Stroke – New Orleans East Hospital and Touro Infirmary President & CEO - Dr. Brain, Inc. Webinar #15 Posterior circulation stroke • Review anatomy – pipes, plumbing, & parenchyma • Common stroke syndromes • NIHSS exam - limitations • The 5 D’s – working through ddx • Supplemental examination • Evaluating the acutely vertiginous patient • Evaluating the patient with perceived minor stroke • Advanced imaging - pitfalls • Standard-of-care treatment options Posterior circulation stroke - Pipes Posterior circulation stroke Plumbing variation • Normal Circle of Willis • <50% population Posterior circulation stroke Plumbing variation Fetal PCA • fPCA (9.5%) is continuation of Pcomm • No communication with basilar • Partial fPCA (15%) has atretic communication with basilar artery • lack of or smaller thalamoperforators in the absence of a P1 or atretic P1 Posterior circulation stroke Plumbing variation • Dominant VA 2/3 • Persistent trigeminal artery • PCA = midbrain, thalamus, medial surface of occipital lobe, inferior and medial surfaces of temporal lobe • SCA = superior cerebellum & rostral laterodorsal pons • AICA = lateral caudal pons & part of cerebellum • PICA = lateral medulla & inferior cerebellum Common stroke syndromes associated with vessel occlusions • Posterior cerebral artery • Basilar artery • Superior cerebellar artery • Anterior inferior cerebellar artery -

Hypertension, Diabetes, Or Migraine Were Reported. Neurological
Letters to the Editor 235 J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.60.2.235 on 1 February 1996. Downloaded from recently it has become clear that hypona- for the cerebral salt wasting syndrome, espe- her left arm. Six months later she com- traemia in the cerebral salt wasting syn- cially in more severe cases. plained of numbness and weakness of her drome is accompanied by hypovolaemia.' 2 WM MULLENERS left arm and leg, from which she recovered We a Departmnenit ofNeurology, report patient with cerebral salt WIM VERHAGEN slowly. No risk factors such as arterial wasting after aneurysmal subarachnoid RHMA BARTELS hypertension, diabetes, or migraine were haemorrhage who showed remarkable Departnieiit oflNeurosurgety, reported. Neurological examination showed changes in urine production during surgery. Caniisius Wilhelnmina Hospital, Nlzjmegeni, The Netherlands a slight left sided ataxia, hemiparesis, and A 46 year old woman was admitted with hypaesthesia. Neuropsychological testing severe headache and vomiting. Physical Correspondence to: Dr WIM Verhagen, Canisius showed reduced cognitive performance and examination was unremarkable. Brain CT Wilhelmina Ziekenhuis, Department of Neurology, a deficit in and PO Box 9015, 6500 GS Niimegen, The flexibility, learning memory, showed a subarachnoid haemorrhage with Netherlands. and abnormal visual constructional abilities blood in the suprasellar cisterns and the left which were compatible with a subcortical Sylvian fissure. Two days later she devel- 1 Nelson PB, Seif SM, Maroon JC, Robinson dementia. Brain MRI showed extensive oped mild hyponatraemia and polyuria; salt AG. Hyponatremia in intracranial disease: perhaps not the syndrome of inappropriate hyperintensive confluent lesions of the pari- and fluid loss were fully compensated by secretion of antidiuretic hormone (SIADH). -

Brainstem and Multiple Cranial Nerve Syndromes
CHAPTER 21 Brainstem and Multiple Cranial Nerve Syndromes he brainstem is a compact structure, with cra- the lower motor neurons of the CN nuclei. With a nial nerve (CN) nuclei, nerve fascicles, and few exceptions, CNs innervate structures of the head T long ascending and descending tracts all and neck ipsilaterally. A process affecting the brain- closely juxtaposed. Structures and centers in the reticu- stem long tracts on one side causes clinical abnormal- lar formation control many vital functions. Brainstem ities on the opposite side of the body. For this reason, diseases are serious and often life threatening. focal brainstem lesions are characterized by “crossed” Involvement of the intricate network of neural struc- syndromes of ipsilateral CN dysfunction and contra- tures often causes a plethora of clinical findings. lateral long motor or sensory tract dysfunction. For Brainstem syndromes typically involve dysfunction of instance, in the right side of the pons, the nuclei for one or more CNs. Deficits due to dysfunction of indi- CNs VI and VII lie in proximity to the right corti- vidual nerves are covered in the preceding chapters. cospinal tract, which is destined to decussate in the This chapter discusses conditions that cause dysfunc- medulla to innervate the left side of the body. The tion beyond the distribution of a single CN, involving patient with a lesion in the right pons will have CN more than one CN, or conditions that involve brain- findings on the right, such as a sixth or seventh nerve stem structures in addition to the CN nucleus or fasci- palsy, and a hemiparesis on the left. -

Clinical Consequences of Stroke
EBRSR [Evidence-Based Review of Stroke Rehabilitation] 2 Clinical Consequences of Stroke Robert Teasell MD, Norhayati Hussein MBBS Last updated November 2013 Abstract Cerebrovascular disorders represent the third leading cause of mortality and the second major cause of long-term disability in North America (Delaney and Potter 1993). The impairments associated with a stroke exhibit a wide diversity of clinical signs and symptoms. Disability, which is multifactorial in its determination, varies according to the degree of neurological recovery, the site of the lesion, the patient's premorbid status and the environmental support systems. Clinical evidence is reviewed as it pertains to stroke lesion location (cerebral, right & left hemispheres; lacunar and brain stem), related disorders (emotional, visual spatial perceptual, communication, fatigue, etc.) and artery(s) affected. 2. Clinical Consequences of Stroke pg. 1 of 29 www.ebrsr.com Table of Contents Abstract ....................................................................................................................... 1 Table of Contents ........................................................................................................ 2 2. Clinical Consequences of Stroke ............................................................................... 3 2.1 Localization of the Stroke ............................................................................................. 3 2.2 Cerebral Hemispheres (Carotid/Anterior Circulation) ................................................... -

Acute Ischaemic Stroke: Part II. the Vertebrobasilar Circulation
Acute Ischaemic Stroke: Part II. The Vertebrobasilar Circulation L. I. G. WORTHLEY, A. W. HOLT Department of Critical Care Medicine, Flinders Medical Centre, Adelaide, SOUTH AUSTRALIA ABSTRACT Objective: To review recent advances in the management of acute ischaemic stroke in a two part presentation. Data sources: Articles and a review of studies reported from 1990 to 2000 and identified through a MEDLINE search of the English language literature on acute ischaemic stroke. Summary of review: An acute ischaemic stroke of the vertebrobasilar circulation is investigated initially with a cerebral computed tomography scan largely to differentiate it from a haemorrhagic stroke. However, cerebral magnetic resonance imaging identifies the ischaemic brainstem lesions more accurately and is often performed with MR angiography to determine the site and extent of the ischaemic vertebrobasilar lesion. Treatment with aspirin (150 - 300 mg) within the first 48 hr as well as management in a specialised unit focusing on resuscitation and prevention of complications has reduced morbidity and mortality. While therapy to improve cerebral blood flow or agents to reduce further neuronal damage have not produced consistent improvement in outcome, numerous small studies using intravenous or intraarterial thrombolytics, percutaneous transluminal angioplasty or stents have reported improved outcome in selected cases. Conclusions: An acute ischaemic stroke in the distribution of the vertebrobasilar circulation requires aspirin 150 - 300 mg daily and management in an acute stroke unit. Intra-arterial or intravenous thrombolytic therapy and percutaneous transluminal angioplasty or stents to improve cerebral blood flow (even up to 24 hours after the event) have been reported to be beneficial in selected cases. -

Assessment and Management of Facial Nerve Palsy
BMJ 2015;351:h3725 doi: 10.1136/bmj.h3725 (Published 16 September 2015) Page 1 of 5 Practice PRACTICE PRACTICE POINTER Assessment and management of facial nerve palsy 1 Liam Masterson specialty registrar, ear, nose, and throat surgery , Martin Vallis general practitioner 2 3 principal , Ros Quinlivan consultant, neuromuscular disease , Peter Prinsley consultant, ear, nose, and throat surgeon 4 1Ear, Nose, and Throat Department, Cambridge University Hospitals NHS Trust, Cambridge CB2 0QQ, UK; 2Rosedale Surgery, NHS Great Yarmouth and Waveney Clinical Commissioning Group, Lowestoft, UK; 3MRC Centre for Neuromuscular Disease, National Hospital for Neurology and Neurosurgery, London, UK; 4Ear, Nose, and Throat Department, Norfolk and Norwich University Hospital NHS Trust, Norwich, UK The facial nerve is important for both communication and When an upper motor neurone lesion is suspected, it may help expression, and impairment of its function can severely affect to determine whether this is localised to the brainstem or cerebral quality of life.1 The main concern at first presentation of a facial cortex. Brainstem disease may present with vertigo, ataxia, or nerve lesion is to exclude the possibility of a stroke or other crossed neurology signs (ipsilateral cranial nerve involvement serious cause.2 The figure⇓ outlines possible causes. Correct and contralateral hemiplegia). A cortical lesion often affects the management within the first few days may prevent long term contralateral limbs and involuntary movements of the face, such complications. as spontaneous smiling, may be spared.6 Urgent referral to How is it assessed? secondary care (neurology or acute medical unit) is needed at this stage to assess the need for thrombolysis. -

Neurovascular Anatomy (2): Posterior Circulation Anatomy
Neurovascular Anatomy (2): Posterior Circulation Anatomy Natthapon Rattanathamsakul, MD. December 28th, 2017 Contents: Neurovascular Anatomy ➢ Arterial supply of the brain ▪ Anterior circulation ▪ Posterior circulation ➢ Arterial supply of the spinal cord ➢ Venous system of the brain Neurovascular Anatomy (2): Anatomy of the Posterior Circulation ➢ Vertebral artery ➢ Basilar artery ➢ Blood supply of diencephalon, brainstem and cerebellum Vertebral Artery • Arise from the 1st part of subclavian artery • Course posteromedially to reach the transverse foramen of C6 vertebra • Run along the foramina then lie on the posterior arch of atlas (C1) • Through the dura, join with each other at pontomedullary junction Flemming KD, Jones LK. Mayo Clinic neurology board review: Basic science and psychiatry for initial certification. 2015 Vertebral Artery • Divided into 4 parts • V1: Ostium to transverse foramen of C6 • V2: Travels cephalad from C6 to C1 • V3: Lies on the posterior arch of C1 (atlas) • V4: Pierces dura, merges together at pontomedullary junction Netter FH. Atlas of human anatomy, 6th ed. 2014 Angiographic Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 Angiographic Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 MRI Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 MRI Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 MRI Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 MRI Correlation Uflacker R. Atlas of vascular anatomy: an angiographic approach, 2007 Vertebral Artery Netter FH. Atlas of human anatomy, 6th ed. 2014 Vertebral Artery Branches of vertebral artery • Muscular arteries • Segmental medullary arteries • Forming anterior & posterior spinal arteries • Meningeal arteries • Perforating branches to medulla • Anterior spinal artery • Posterior inferior cerebellar artery (PICA) Műller KI, et al. -
298.2.Full.Pdf
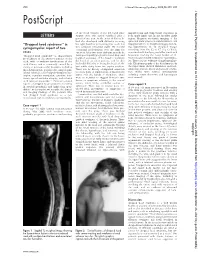
290 J Neurol Neurosurg Psychiatry 2005;76:290–300 J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.2004.047357 on 14 January 2005. Downloaded from PostScript.............................................................................................. of the small muscles of the left hand since impaired pain and temperature sensations in LETTERS August 1998. This deficit stabilised after a both upper limbs and in the shoulder girdle period of one year. At the onset of illness, he region. Magnetic resonance imaging of the had also developed mild difficulty in using spine and brain revealed a septate intrinsic cord ‘‘Dropped head syndrome’’ in his right hand for performing fine work but hypointensity in T1 weighted images, becom- this symptom remained stable. He noticed ing hyperintense in T2 weighted images syringomyelia: report of two occasional fasciculations over the arms for extending from the C2 to C7 (fig 1) levels, cases one year. After two years and nine months he associated with low lying cerebellar tonsils and ‘‘Dropped head syndrome’’ is characterised developed rapidly progressive head drop and brainstem reaching the lower border of C1. by weakness of the extensor muscles of the required assistance of the hand to maintain Brain images revealed evidence of hydrocepha- neck, with or without involvement of the the head in an erect posture, and he also lus. There was no evidence of myelomeningo- neck flexors, and is commonly caused by a had mild difficulty in lifting his head off the cele. Electromyography of the distal muscles in variety of neuromuscular disorders, including bed while rising from the supine position. the upper limbs showed fibrillation and fasci- myasthenia gravis, polymyositis, amyotrophic There was no history of impaired sensation culation potentials. -
Medial Pontomedullary Stroke Mimicking Severe Bell’S Palsy
CASE REPORT Medial Pontomedullary Stroke Mimicking Severe Bell’s Palsy: A Case Report Benjamin Boodaie, MD* *Kern Medical, Department of Emergency Medicine, Bakersfield, California Manish Amin, DO* †Kern Medical, Department of Neurology, Bakersfield, California Katayoun Sabetian, MD† ‡Ross University School of Medicine, Department of Medicine, Miramar, Florida Daniel Quesada, MD* Tyler Torrico, BIS‡ Section Editor: Austin Smith, MD Submission history: Submitted February 14, 2020; Revision received April 22, 2020; Accepted May 5, 2020 Electronically published July 20, 2020 Full text available through open access at http://escholarship.org/uc/uciem_cpcem DOI: 10.5811/cpcem.2020.5.46965 Introduction: Patients with acute unilateral upper and lower facial palsy frequently present to the emergency department fearing they have had a stroke, but many cases are benign Bell’s palsy. Case Report: We present a rare case of a medial pontomedullary junction stroke causing upper and lower hemifacial paralysis associated with severe dysphagia and contralateral face and arm numbness. Conclusion: Although rare, pontine infarct must be considered in patients who present with both upper and lower facial weakness. Unusual neurologic symptoms (namely diplopia, vertigo, or dysphagia) and signs (namely gaze palsy, nystagmus, or contralateral motor or sensory deficits) should prompt evaluation for stroke. [Clin Pract Cases Emerg Med. 2020;4(3):380–383.] Keywords: Bell’s Palsy; pontine stroke; MRI. INTRODUCTION EDs between 2005 and 2011, 0.8% received an alternative Acute facial palsy is a commonly encountered complaint diagnosis after 90-day follow-up, of which 30% was found to in the emergency department (ED) setting. Bell’s palsy be secondary to ischemic stroke or intracranial hemorrhage.4 represents approximately half of such cases.1,2 Bell’s palsy is By these numbers, approximately one in 400 ED diagnoses of defined as an idiopathic peripheral facial nerve palsy, which Bell’s palsy may be missed diagnoses of stroke. -
Double Steal Phenomenon: Emergency Department Management of Recurrent Transient Ischemic Attack
CASE REPORT Double Steal Phenomenon: Emergency Department Management of Recurrent Transient Ischemic Attack Amit R. Rawal, MD* *North Florida Regional Medical Center, Department of Emergency Medicine, Collin Bufano, DO* Gainesville, Florida Omar Saeed, MD† †University of Tennessee Health Science Center, Department of Internal Medicine, Asif A. Khan, MD‡ Memphis, Tennessee ‡North Florida Regional Medical Center, Department of Vascular and Interventional Neurology, Gainesville, Florida Section Editor: Rick A. McPheeters, DO Submission history: Submitted September 15, 2018; Revision received January 15, 2019; Accepted January 22, 2019 Electronically published February 13, 2019 Full text available through open access at http://escholarship.org/uc/uciem_cpcem DOI: 10.5811/cpcem.2019.1.40960 Double steal phenomenon is a rare condition where occlusion of the innominate (brachiocephalic) artery leads to hemodynamic changes in which blood flow is shunted from the intracranial circulation down the right vertebral artery and subsequently up the right carotid and subclavian circulation. This is a case of a 67-year-old female presenting emergently with recurrent transient ischemic attacks due to double steal phenomenon. Emergency department recognition of the double steal phenomenon and large vessel occlusion by computed tomography angiogram of the head and neck allowed for early treatment, which was critical in avoiding irreversible cerebral infarction. [Clin Pract Cases Emerg Med. 2019;3(2):144-148.] INTRODUCTION TIA. The patient described the acute onset of left-sided facial Subclavian steal syndrome is a well-documented weakness that waxed and waned, recurring several times phenomenon in which right vertebral artery flow is reversed throughout the day, and lasting 2-3 minutes at a time.