Novel Technique for Performing Retrograde Pyelogram Through A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Testosterone Replacement Therapy Is Associated with an Increased Risk of Urolithiasis
World Journal of Urology (2019) 37:2737–2746 https://doi.org/10.1007/s00345-019-02726-6 ORIGINAL ARTICLE Testosterone replacement therapy is associated with an increased risk of urolithiasis Tyler R. McClintock1 · Marie‑Therese I. Valovska2 · Nicollette K. Kwon3 · Alexander P. Cole1,3 · Wei Jiang3 · Martin N. Kathrins1 · Naeem Bhojani4 · George E. Haleblian1 · Tracey Koehlmoos5 · Adil H. Haider3,6 · Shehzad Basaria7 · Quoc‑Dien Trinh1,3 Received: 16 November 2018 / Accepted: 7 March 2019 / Published online: 23 March 2019 © Springer-Verlag GmbH Germany, part of Springer Nature 2019 Abstract Purpose To determine whether TRT in men with hypogonadism is associated with an increased risk of urolithiasis. Methods We conducted a population-based matched cohort study utilizing data sourced from the Military Health System Data Repository (a large military-based database that includes benefciaries of the TRICARE program). This included men aged 40–64 years with no prior history of urolithiasis who received continuous TRT for a diagnosis of hypogonadism between 2006 and 2014. Eligible individuals were matched using both demographics and comorbidities to TRICARE enrollees who did not receive TRT. The primary outcome was 2-year absolute risk of a stone-related event, comparing men on TRT to non-TRT controls. Results There were 26,586 pairs in our cohort. Four hundred and eighty-two stone-related events were observed at 2 years in the non-TRT group versus 659 in the TRT group. Log-rank comparisons showed this to be a statistically signifcant dif- ference in events between the two groups (p < 0.0001). This diference was observed for topical (p < 0.0001) and injection (p = 0.004) therapy-type subgroups, though not for pellet (p = 0.27). -

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Complications of Ureteroscopic Approaches, Including Incisions
18 Complications of Ureteroscopic Approaches, Including Incisions Farjaad M. Siddiq, MD and Raymond J. Leveillee, MD CONTENTS INTRODUCTION PREPARATION FOR URETEROSCOPY URETERAL ACCESS DILATION OF THE URETERAL ORIFICE: IS IT NECESSARY? COMPLICATIONS OF URETEROSCOPY URETERAL STENTS: ARE THEY NECESSARY? POSTOPERATIVE IMAGING COMPLICATIONS OF URETEROSCOPIC MANAGEMENT OF UPPER TRACT TCC COMPLICATIONS OF URETEROSCOPIC INCISIONS CONCLUSION REFERENCES SUMMARY Ureteroscopy has progressed from cystoscopic examination of a dilated ureter in a child in 1929 and the initial use of rigid ureteroscopes in the 1980s, to its current state of small caliber semirigid and flexible instruments. In this chapter the authors review complications of ureteroscopy including those associated with incisional techniques where one would anticipate a higher incidence of complications. They review the his- tory and development of modern ureteroscopes, focusing on engineering advances. Clinical points made include proper patient selection and preparation; proper use of dilators, wires, and ureteral access sheaths; and the incidence, identification, and man- agement of complications associated with ureterorenoscopy (both intraopertively and postoperatively). Key Words: Ureteroscopy; calculi; urinary stones; stricture or ureter; urothelial carcinoma; surgical complications. From: Advanced Endourology: The Complete Clinical Guide Edited by: S. Y. Nakada and M. S. Pearle © Humana Press Inc., Totowa, NJ 299 300 Siddiq and Leveillee INTRODUCTION Ureteroscopy has progressed from cystoscopic examination of a dilated ureter in a child with posterior urethral valves by Young and McKay (1) in 1929 and the initial use of a rigid ureteroscope by Perez-Castro Ellendt and Martinez-Pineiro (2,3) in the early 1980s, to its current state of small caliber semirigid and flexible instruments. -
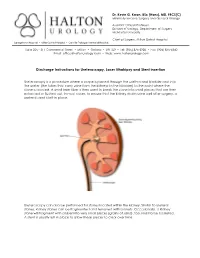
Discharge Instructions for Ureteroscopy, Laser Lithotripsy and Stent Insertion
Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Chief of Surgery, Milton District Hospital Georgetown Hospital • Milton District Hospital • Oakville Trafalgar Memorial Hospital Suite 205 - 311 Commercial Street • Milton • Ontario • L9T 3Z9 • Tel: (905) 875-3920 • Fax: (905) 875-4340 Email: [email protected] • Web: www.haltonurology.com Discharge Instructions for Ureteroscopy, Laser lithotripsy and Stent insertion Ureteroscopy is a procedure where a scope is passed through the urethra and bladder and into the ureter (the tubes that carry urine from the kidneys to the bladder) to the point where the stone is located. A small laser fiber is then used to break the stone into small pieces that are then extracted or flushed out. In most cases, to ensure that the kidney drains urine well after surgery, a ureteral stent is left in place. Ureteroscopy can also be performed for stones located within the kidney. Similar to ureteral stones, kidney stones can be fragmented and removed with baskets. Occasionally, a kidney stone will fragment with a laser into very small pieces (grains of sand), too small to be basketed. A stent is usually left in place to allow these pieces to clear over time. Ureteral Stenting: Almost always after ureteroscopy, a ureteral stent will be placed. This is a thin, hollow, plastic tube that is used temporarily to keep the ureter open and facilitates drainage of urine down to the bladder until it heals. It also allows the urine to drain and any small stone fragments to pass freely. -

Contemporary Practice Patterns of Flexible Ureteroscopy for Treating Renal Stones: Results of a Worldwide Survey
JOURNAL OF ENDOUROLOGY Volume 29, Number 11, November 2015 Ureteroscopy and Percutaneous Procedures ª Mary Ann Liebert, Inc. Pp. 1221–1230 DOI: 10.1089/end.2015.0260 Contemporary Practice Patterns of Flexible Ureteroscopy for Treating Renal Stones: Results of a Worldwide Survey Casey A. Dauw, MD,1 Laika Simeon, BA,1 Abdulrahman F. Alruwaily, MBChB,1 Francesco Sanguedolce, MD,2 John M. Hollingsworth, MD, MS,1 William W. Roberts, MD,1 Gary J. Faerber, MD,1 J. Stuart Wolf, Jr., MD,1 and Khurshid R. Ghani, MBChB, MS1 Abstract Introduction: Flexible ureteroscopy (fURS) is increasingly used in the treatment of renal stones. However, wide variations exist in technique, use, and indications. To better inform our knowledge about the contemporary state of fURS for treating renal stones, we conducted a survey of endourologists worldwide. Methods: An anonymous online questionnaire assessing fURS treatment of renal stones, consisting of 36 items, was sent to members of the Endourology Society in October 2014. Responses were collected through the SurveyMonkey system over a 3-month period. Results: Questionnaires were answered by 414 surgeons from 44 countries (response rate 20.7%). U.S. surgeons accounted for 34.4% of all respondents. fURS was routinely performed in 80.0% of institutions, with 40.0% of surgeons performing >100 cases/year. Respondents considered fURS to be first-line therapy for patients with renal stones <2 cm and lower pole calculi. A substantial minority (11.3%) preferred fURS as a primary treatment modality for renal stones >2 cm. Basket displacement for lower pole stones was routinely performed by 55.8%. -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular -

Ureteroscopy
Ureteroscopy What is a Ureteroscopy? A ureteroscopy is a “minimally invasive” procedure. This means that a urologist inserts a tube-like device with a light and a lens for viewing (ureteroscope) through the urethra (natural urinary channel) instead of making cuts. Urologists use this procedure to treat kidney stones as well as stones located in the ureter (the tube that carries urine from the kidney to the bladder.) Urologists can also use this procedure to treat patients who must remain on anticoagulation therapy. What happens during the procedure? The urologist inserts the thin ureteroscope upstream through the urethra. The ureteroscope helps deliver shock waves to the stone if necessary. No incisions are made. Once the urologist identifies the stone they break it up and remove it. It is typically an outpatient procedure meaning you go home the same day. The urologist performs it in the operating room with general anesthesia (medicine to produce loss of feeling and deep sleep) or spinal anesthesia (medication to produce loss of feeling in part of the spine) What steps should I take to prepare for the procedure? 1. Do not eat any solid food (including gum, hard candy or mints) after 12am (midnight) the night before surgery. Department of Urology - 1 - 2. Do not drink any milk products after 12am (midnight). You may drink water only and any routine medications up to 4 hours before your surgery. 3. Wear loose, simple clothing which can easily be changed. Leave all jewelry and valuables at home. 4. Bring along to the hospital a responsible adult companion who will: remain in the hospital, be available to hospital personnel during your procedure, and assist you upon discharge by driving you home with close observation of your condition. -

HAVING a URETERIC STENT What to Expect and How to Manage
You have been sent home with HAVING A URETERIC STENT What to expect and how to manage 1 INTRODUCTION In patients who have, or might have an obstruction (blockage) of the kidney, an internal drainage tube called a “stent” is commonly placed in the ureter, the tube between the kidney and the bladder. This is placed there in order to prevent of temporarily relieve the obstruction. This information sheet has been given to you to help answer some of the questions you may have about having a ureteric stent inserted. If you have any questions or concerns, please, do not hesitate to speak to a doctor or a nurse caring for you. 2 THE URINARY SYSTEM AND URETERIC STENT THE URINARY SYSTEM AND THE URETER The kidneys produce urine. Normally there are two kidneys situated in the upper part of the abdomen, towards the back. The urine formed in the kidney is carried to the bladder by a fine muscular tube called a ureter. The urinary bladder acts as a reservoir for the urine and when it is full it is emptied via the urethra. Figure 1: The urinary system HOW DOES A KIDNEY BECOME OBSTRUCTED ? Common causes of obstruction of the kidneys and ureter are: -A kidney stone or its fragments moving into the ureter, either spontaneously, or occasionally following such treatment as shock wave therapy. -Narrrowing (stricture) of the ureter anywhere along its path. This can be due. scaring of wall of the ureter, narrowing of the area where the ureter leaves from the kidney (pelvi-ueteric junction) 3 -Temporarily, following an operation or after an instrument has been inserted into the ureter and kidneys. -

Ureteroscopy and Laser Lithotripsy Is a Safe and Effective Operation to Treat Kidney Stones
URETEROSCOPY AND LASER LITHOTRIPSY Ureteroscopy and laser lithotripsy is a safe and effective operation to treat kidney stones. This is a minimally- invasive procedure where kidney stones are destroyed with a special laser, without the need for any incisions. Compared to extracorporeal shockwave lithotripsy (the destruction of stones with sound waves), ureteroscopy and laser lithotripsy is more effective with a lower need for repeat treatments. PREPARATION FOR SURGERY > Medications to avoid prior to surgery You do NOT need to stop any of your medications that affect bleeding including ASA (Aspirin/Entrophen), warfarin (Coumadin), clopidogrel (Plavix), dipyridamole (Aggrenox), ticagrelor (Brilinta), ibuprofen (Advil/Motrin) and other non-steroidal anti-inflammatories (NSAIDs), dabigatran (Pradaxa), rivaroxaban (Xarelto) and apixaban (Eliquis). If you have any questions about your medications prior to surgery, please contact your surgeon. Diet prior to surgery You may eat your normal diet up until midnight the night before your surgery. Do not eat any solid food, milk or cream after midnight the night before your surgery. You may drink up to 400 mL (1.5 cups) of water up to 3 hours before surgery. You many not drink any other fluids. You may have sips of water with your morning medications. THE SURGERY > In the operating room Ureteroscopy and laser lithotripsy is performed under a general anesthetic, meaning you will be asleep for the operation. The operation is performed using small telescopes through the urethra (the tube that allows flow of urine from the bladder). Your stone will be destroyed using a special laser. Once the stone has been destroyed, a ureteral stent (a temporary plastic tube that runs from the kidney down to the bladder) will be inserted. -

Complications of Urologic Surgery Acknowledgement
Complications of Urologic Surgery Jay D. Raman, MD, FACS Professor and Chief of Urology Penn State Health Milton S. Hershey Medical Center @urojdr Acknowledgement • J. Kellogg Parsons, MD, MHS, FACS – Professor and Endowed Chair – Moores Comprehensive Cancer Center – UC San Diego Health System © 2018 AMERICAN UROLOGICAL ASSOCIATION. ALL RIGHTS RESERVED. Disclosures • MDxHealth – Study site investigator – urine biomarker trial • Urogen Pharma Ltd – Study site investigator – Olympus trial – Strategic advisor board • American Kidney Stone Management (AKSM) – Stock ownership Resources • AUA Guidelines • AUA Core Curriculum • AUA SASP Questions • AUA Updates • Contemporary or significant publications © 2018 AMERICAN UROLOGICAL ASSOCIATION. ALL RIGHTS RESERVED. Outline (Potpourri of topics) • Nerve injury • Positional • Intra‐operative • Bowel injury • General MIS presentation • Rectal • Air embolism (MIS) Outline (Potpourri of topics) • Venous thromboembolism (VTE) • Rhabdomyolysis • Stone Surgery • Ureteroscopy (URS) • Shock wave lithotripsy (SWL) © 2018 AMERICAN UROLOGICAL ASSOCIATION. ALL RIGHTS RESERVED. Outline (Potpourri of topics) • Nerve injury • Positional • Intra‐operative • Bowel injury • General MIS presentation • Rectal • Air embolism (MIS) Positional Nerve Injury • Presentation – Immediately post‐operatively with deficits in the affected nerve distribution • Paresthesias (numbness/tingling) – sensory • Weakness – motor • Risk factors: – Improper positioning and padding – Obesity – Prolonged operative duration Mills JT et al. -

Supplemental Information
ARTICLE Supplemental Information SUPPLEMENTAL TABLE 3 Codes Used for Building Normal and Hydronephrosis Cohorts: Associated Diagnostic Codes (For Inclusion or Exclusion) Code Description Hydroureteronephrosis 591 Hydronephrosis 753.29 Other obstructive defects of renal pelvis and ureter 593.5 Hydroureter 753.22 Congenital obstruction of UVJ VUR 593.7 VUR 593.70 VUR unspecified or without reflux nephropathy 593.71 VUR with reflux nephropathy, unilateral 593.72 VUR with reflux nephropathy, bilateral 593.73 Other VUR with reflux nephropathy NOS Obstruction 593.3 Stricture or kinking of ureter 599.6 Urinary obstruction, unspecified 599.69 Urinary obstruction NOS UPJO 753.2 Unspecified obstructive defect of renal pelvis and ureter 753.21 Congenital obstruction of the UPJ 753.29 Other obstructive defect of renal pelvis and ureter UVJ obstruction 753.22 Congenital obstruction of the UVJ Ureterocele 753.23 Congenital ureterocele PUV or urethral atresia 753.6 Atresia and stenosis of urethra and bladder neck, includes PUVs NOS, not otherwise specified; UPJ, ureteropelvic junction; UVJ, ureterovesical junction. PEDIATRICS Volume 142, number 1, July 2018 1 SUPPLEMENTAL TABLE 4 Codes Used for Building Normal and Hydronephrosis Cohorts: Urological Surgical Codes for Exclusion in Building Normal Cohort CPT ICD-9 Description Pyeloplasty 50544 — Laparoscopy, surgical; pyeloplasty 50400 55.87 Pyeloplasty 50405 — Complicated pyeloplasty; secondary or congenital 50740 55.86 Ureteropyelostomy, anastomosis of ureter and renal pelvis 50750 — Ureterocalycostomy, -

Flexible Ureteroscopy for Kidney Stones (URS)
Flexible Ureteroscopy for Kidney Stones (URS) Department of Urology Patient Information WhatWhat is Ureteroscopy is Ureteroscopy or URS? or URS? Ureteroscopy involves the passage of a small fibroptic instrument called a ureteroscope through the urethra and the bladder into the ureter. The urethra is the tube from the bladder through which the urine drains out. A ureter is the tube from the kidneys which drains urine into the bladder. WhyWhy do doI need I need Ureteroscopy? Ureteroscopy? Ureteroscopy is needed to remove a stone/stones from your kidneys which have not been able to pass through the ureter normally. WhatWhat preparation preparation do I need? do I need? The procedure will be done under General Anaesthesia so you will have to attend a pre assessment clinic before your operation. You will be screened for MRSA and some baseline investigations will be performed. You will also have an x-ray done to confirm the presence of a stone. You will be asked not to eat and drink 6 hours prior to surgery. What happens on the day? You will be admitted onto the ward on the day of your procedure and be seen by an anaesthetist. You will also be seen by the surgeon who will go through with you the procedure. You will have the opportunity to ask any questions. Your surgeon will also ask you to sign a consent form. Your nurse will ask you to change into a hospital gown and remove any jewellery. You will also be asked to wear special stockings while you are in the hospital which helps to prevent Deep Vein Thrombosis.