Peripheral Nervous System the Central Nervous System Includes the Brain and Spinal Cord, While the Peripheral Nervous System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Nerve Ultrasound in Dorsal Root Ganglion Disorders: Smaller Nerves Lead to Bigger Insights
Clinical Neurophysiology 130 (2019) 550–551 Contents lists available at ScienceDirect Clinical Neurophysiology journal homepage: www.elsevier.com/locate/clinph Editorial Nerve ultrasound in dorsal root ganglion disorders: Smaller nerves lead to bigger insights See Article, pages 568–572 After decades of having to make do with electric stimulation representing the fascicles, bundled together in a large outer cable and recording (i.e. nerve conduction studies, electromyography sheath (van Alfen et al., 2018). and evoked potentials), nerve ultrasound now provides the oppor- Next, it is important to realize what the ratio between axon/ tunity to improve neurodiagnostic patient care by deploying a myelin and connective tissue in a given nerve segment is, and powerful tool to detect neuromuscular pathology in an accurate how that ratio changes from the proximal root to the distal end and patient-friendly way (Mah et al., 2018; Walker et al., 2018). branches (Schraut et al., 2016). Connective tissue elements of the Nerve ultrasound is also increasingly providing neurologists and perineurium and epineurium are relatively sparse at the very prox- clinical neurophysiologists with the opportunity to increase their imal root and plexus levels, with an average connective tissue con- insight in the pathophysiology of peripheral nervous system tent of around 25–30%. Ultrasonographically, this means that roots (PNS) pathology. In this issue of Clinical Neurophysiology, Leadbet- will always look rather black in appearance without much dis- ter and coworkers (Leadbetter et al., 2019) describe the results of cernible fascicular architecture, as the sparseness of connective tis- their study on nerve ultrasound for diagnosing sensory neuronopa- sue elements provides relatively few reflectors to create an image thy in spinocerebellar ataxia type 2 and CANVAS syndrome. -

Head Start Early Learning Outcomes Framework Ages Birth to Five
Head Start Early Learning Outcomes Framework Ages Birth to Five 2015 R U.S. Department of Health and Human Services Administration for Children and Families Office of Head Start Office of Head Start | 8th Floor Portals Building, 1250 Maryland Ave, SW, Washington DC 20024 | eclkc.ohs.acf.hhs.gov Dear Colleagues: The Office of Head Start is proud to provide you with the newly revisedHead Start Early Learning Outcomes Framework: Ages Birth to Five. Designed to represent the continuum of learning for infants, toddlers, and preschoolers, this Framework replaces the Head Start Child Development and Early Learning Framework for 3–5 Year Olds, issued in 2010. This new Framework is grounded in a comprehensive body of research regarding what young children should know and be able to do during these formative years. Our intent is to assist programs in their efforts to create and impart stimulating and foundational learning experiences for all young children and prepare them to be school ready. New research has increased our understanding of early development and school readiness. We are grateful to many of the nation’s leading early childhood researchers, content experts, and practitioners for their contributions in developing the Framework. In addition, the Secretary’s Advisory Committee on Head Start Research and Evaluation and the National Centers of the Office of Head Start, especially the National Center on Quality Teaching and Learning (NCQTL) and the Early Head Start National Resource Center (EHSNRC), offered valuable input. The revised Framework represents the best thinking in the field of early childhood. The first five years of life is a time of wondrous and rapid development and learning.The Head Start Early Learning Outcomes Framework: Ages Birth to Five outlines and describes the skills, behaviors, and concepts that programs must foster in all children, including children who are dual language learners (DLLs) and children with disabilities. -

Introduction to Arthropod Groups What Is Entomology?
Entomology 340 Introduction to Arthropod Groups What is Entomology? The study of insects (and their near relatives). Species Diversity PLANTS INSECTS OTHER ANIMALS OTHER ARTHROPODS How many kinds of insects are there in the world? • 1,000,0001,000,000 speciesspecies knownknown Possibly 3,000,000 unidentified species Insects & Relatives 100,000 species in N America 1,000 in a typical backyard Mostly beneficial or harmless Pollination Food for birds and fish Produce honey, wax, shellac, silk Less than 3% are pests Destroy food crops, ornamentals Attack humans and pets Transmit disease Classification of Japanese Beetle Kingdom Animalia Phylum Arthropoda Class Insecta Order Coleoptera Family Scarabaeidae Genus Popillia Species japonica Arthropoda (jointed foot) Arachnida -Spiders, Ticks, Mites, Scorpions Xiphosura -Horseshoe crabs Crustacea -Sowbugs, Pillbugs, Crabs, Shrimp Diplopoda - Millipedes Chilopoda - Centipedes Symphyla - Symphylans Insecta - Insects Shared Characteristics of Phylum Arthropoda - Segmented bodies are arranged into regions, called tagmata (in insects = head, thorax, abdomen). - Paired appendages (e.g., legs, antennae) are jointed. - Posess chitinous exoskeletion that must be shed during growth. - Have bilateral symmetry. - Nervous system is ventral (belly) and the circulatory system is open and dorsal (back). Arthropod Groups Mouthpart characteristics are divided arthropods into two large groups •Chelicerates (Scissors-like) •Mandibulates (Pliers-like) Arthropod Groups Chelicerate Arachnida -Spiders, -

Medical Terminology Abbreviations Medical Terminology Abbreviations
34 MEDICAL TERMINOLOGY ABBREVIATIONS MEDICAL TERMINOLOGY ABBREVIATIONS The following list contains some of the most common abbreviations found in medical records. Please note that in medical terminology, the capitalization of letters bears significance as to the meaning of certain terms, and is often used to distinguish terms with similar acronyms. @—at A & P—anatomy and physiology ab—abortion abd—abdominal ABG—arterial blood gas a.c.—before meals ac & cl—acetest and clinitest ACLS—advanced cardiac life support AD—right ear ADL—activities of daily living ad lib—as desired adm—admission afeb—afebrile, no fever AFB—acid-fast bacillus AKA—above the knee alb—albumin alt dieb—alternate days (every other day) am—morning AMA—against medical advice amal—amalgam amb—ambulate, walk AMI—acute myocardial infarction amt—amount ANS—automatic nervous system ant—anterior AOx3—alert and oriented to person, time, and place Ap—apical AP—apical pulse approx—approximately aq—aqueous ARDS—acute respiratory distress syndrome AS—left ear ASA—aspirin asap (ASAP)—as soon as possible as tol—as tolerated ATD—admission, transfer, discharge AU—both ears Ax—axillary BE—barium enema bid—twice a day bil, bilateral—both sides BK—below knee BKA—below the knee amputation bl—blood bl wk—blood work BLS—basic life support BM—bowel movement BOW—bag of waters B/P—blood pressure bpm—beats per minute BR—bed rest MEDICAL TERMINOLOGY ABBREVIATIONS 35 BRP—bathroom privileges BS—breath sounds BSI—body substance isolation BSO—bilateral salpingo-oophorectomy BUN—blood, urea, nitrogen -

The Development of a Whole-Head Human Finite- Element Model for Simulation of the Transmission of Bone-Conducted Sound
The development of a whole-head human finite- element model for simulation of the transmission of bone-conducted sound You Chang, Namkeun Kim and Stefan Stenfelt Journal Article N.B.: When citing this work, cite the original article. Original Publication: You Chang, Namkeun Kim and Stefan Stenfelt, The development of a whole-head human finite-element model for simulation of the transmission of bone-conducted sound, Journal of the Acoustical Society of America, 2016. 140(3), pp.1635-1651. http://dx.doi.org/10.1121/1.4962443 Copyright: Acoustical Society of America / Nature Publishing Group http://acousticalsociety.org/ Postprint available at: Linköping University Electronic Press http://urn.kb.se/resolve?urn=urn:nbn:se:liu:diva-133011 The development of a whole-head human finite-element model for simulation of the transmission of bone-conducted sound You Chang1), Namkeun Kim2), and Stefan Stenfelt1) 1) Department of Clinical and Experimental Medicine, Linköping University, Linköping, Sweden 2) Division of Mechanical System Engineering, Incheon National University, Incheon, Korea Running title: whole-head finite-element model for bone conduction 1 Abstract A whole head finite element model for simulation of bone conducted (BC) sound transmission was developed. The geometry and structures were identified from cryosectional images of a female human head and 8 different components were included in the model: cerebrospinal fluid, brain, three layers of bone, soft tissue, eye and cartilage. The skull bone was modeled as a sandwich structure with an inner and outer layer of cortical bone and soft spongy bone (diploë) in between. The behavior of the finite element model was validated against experimental data of mechanical point impedance, vibration of the cochlear promontories, and transcranial BC sound transmission. -

Head and Neck
DEFINITION OF ANATOMIC SITES WITHIN THE HEAD AND NECK adapted from the Summary Staging Guide 1977 published by the SEER Program, and the AJCC Cancer Staging Manual Fifth Edition published by the American Joint Committee on Cancer Staging. Note: Not all sites in the lip, oral cavity, pharynx and salivary glands are listed below. All sites to which a Summary Stage scheme applies are listed at the begining of the scheme. ORAL CAVITY AND ORAL PHARYNX (in ICD-O-3 sequence) The oral cavity extends from the skin-vermilion junction of the lips to the junction of the hard and soft palate above and to the line of circumvallate papillae below. The oral pharynx (oropharynx) is that portion of the continuity of the pharynx extending from the plane of the inferior surface of the soft palate to the plane of the superior surface of the hyoid bone (or floor of the vallecula) and includes the base of tongue, inferior surface of the soft palate and the uvula, the anterior and posterior tonsillar pillars, the glossotonsillar sulci, the pharyngeal tonsils, and the lateral and posterior walls. The oral cavity and oral pharynx are divided into the following specific areas: LIPS (C00._; vermilion surface, mucosal lip, labial mucosa) upper and lower, form the upper and lower anterior wall of the oral cavity. They consist of an exposed surface of modified epider- mis beginning at the junction of the vermilion border with the skin and including only the vermilion surface or that portion of the lip that comes into contact with the opposing lip. -
Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves
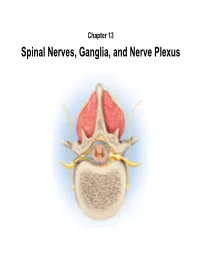
Chapter 13 Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves Posterior Spinous process of vertebra Posterior root Deep muscles of back Posterior ramus Spinal cord Transverse process of vertebra Posterior root ganglion Spinal nerve Anterior ramus Meningeal branch Communicating rami Anterior root Vertebral body Sympathetic ganglion Anterior General Anatomy of Nerves and Ganglia • Spinal cord communicates with the rest of the body by way of spinal nerves • nerve = a cordlike organ composed of numerous nerve fibers (axons) bound together by connective tissue – mixed nerves contain both afferent (sensory) and efferent (motor) fibers – composed of thousands of fibers carrying currents in opposite directions Anatomy of a Nerve Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Epineurium Perineurium Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Endoneurium Nerve Rootlets fiber Posterior root Fascicle Posterior root ganglion Anterior Blood root vessels Spinal nerve (b) Copyright by R.G. Kessel and R.H. Kardon, Tissues and Organs: A Text-Atlas of Scanning Electron Microscopy, 1979, W.H. Freeman, All rights reserved Blood vessels Fascicle Epineurium Perineurium Unmyelinated nerve fibers Myelinated nerve fibers (a) Endoneurium Myelin General Anatomy of Nerves and Ganglia • nerves of peripheral nervous system are ensheathed in Schwann cells – forms neurilemma and often a myelin sheath around the axon – external to neurilemma, each fiber is surrounded by -

Chapter 32 FOREIGN BODIES of the HEAD, NECK, and SKULL BASE
Foreign Bodies of the Head, Neck, and Skull Base Chapter 32 FOREIGN BODIES OF THE HEAD, NECK, AND SKULL BASE RICHARD J. BARNETT, MD* INTRODUCTION PENETRATING NECK TRAUMA Anatomy Emergency Management Clinical Examination Investigations OPERATIVE VERSUS NONOPERATIVE MANAGEMENT Factors in the Deployed Setting Operative Management Postoperative Care PEDIATRIC INJURIES ORBITAL FOREIGN BODIES SUMMARY CASE PRESENTATIONS Case Study 32-1 Case Study 32-2 Case Study 32-3 Case Study 32-4 Case Study 32-5 Case Study 32-6 *Lieutenant Colonel, Medical Corps, US Air Force; Chief of Facial Plastic Surgery/Otolaryngology, Eglin Air Force Base Department of ENT, 307 Boatner Road, Suite 114, Eglin Air Force Base, Florida 32542-9998 423 Otolaryngology/Head and Neck Combat Casualty Care INTRODUCTION The mechanism and extent of war injuries are sig- other military conflicts. In a study done in Croatia with nificantly different from civilian trauma. Many of the 117 patients who sustained penetrating neck injuries, wounds encountered are unique and not experienced about a quarter of the wounds were from gunshots even at Role 1 trauma centers throughout the United while the rest were from shell or bomb shrapnel.1 The States. Deployed head and neck surgeons must be injury patterns resulting from these mechanisms can skilled at performing an array of evaluations and op- vary widely, and treating each injury requires thought- erations that in many cases they have not performed in ful planning to achieve a successful outcome. a prior setting. During a 6-month tour in Afghanistan, This chapter will address penetrating neck injuries all subspecialties of otolaryngology were encountered: in general, followed specifically by foreign body inju- head and neck (15%), facial plastic/reconstructive ries of the head, face, neck, and skull base. -

Comparison of Cadaveric Human Head Mass Properties: Mechanical Measurement Vs
12 INJURY BIOMECHANICS RESEARCH Proceedings of the Thirty-First International Workshop Comparison of Cadaveric Human Head Mass Properties: Mechanical Measurement vs. Calculation from Medical Imaging C. Albery and J. J. Whitestone This paper has not been screened for accuracy nor refereed by any body of scientific peers and should not be referenced in the open literature. ABSTRACT In order to accurately simulate the dynamics of the head and neck in impact and acceleration environments, valid mass properties data for the human head must exist. The mechanical techniques used to measure the mass properties of segmented cadaveric and manikin heads cannot be used on live human subjects. Recent advancements in medical imaging allow for three-dimensional representation of all tissue components of the living and cadaveric human head that can be used to calculate mass properties. A comparison was conducted between the measured mass properties and those calculated from medical images for 15 human cadaveric heads in order to validate this new method. Specimens for this study included seven female and eight male, unembalmed human cadaveric heads (ages 16 to 97; mean = 59±22). Specimen weight, center of gravity (CG), and principal moments of inertia (MOI) were mechanically measured (Baughn et al., 1995, Self et al., 1992). These mass properties were also calculated from computerized tomography (CT) data. The CT scan data were segmented into three tissue types - brain, bone, and skin. Specific gravity was assigned to each tissue type based on values from the literature (Clauser et al., 1969). Through analysis of the binary volumetric data, the weight, CG, and MOIs were determined. -

The Peripheral Nervous System
The Peripheral Nervous System Dr. Ali Ebneshahidi Peripheral Nervous System (PNS) – Consists of 12 pairs of cranial nerves and 31 pairs of spinal nerves. – Serves as a critical link between the body and the central nervous system. – peripheral nerves contain an outermost layer of fibrous connective tissue called epineurium which surrounds a thinner layer of fibrous connective tissue called perineurium (surrounds the bundles of nerve or fascicles). Individual nerve fibers within the nerve are surrounded by loose connective tissue called endoneurium. Cranial Nerves Cranial nerves are direct extensions of the brain. Only Nerve I (olfactory) originates from the cerebrum, the remaining 11 pairs originate from the brain stem. Nerve I (Olfactory)- for the sense of smell (sensory). Nerve II (Optic)- for the sense of vision (sensory). Nerve III (Oculomotor)- for controlling muscles and accessory structures of the eyes ( primarily motor). Nerve IV (Trochlear)- for controlling muscles of the eyes (primarily motor). Nerve V (Trigeminal)- for controlling muscles of the eyes, upper and lower jaws and tear glands (mixed). Nerve VI (Abducens)- for controlling muscles that move the eye (primarily motor). Nerve VII (Facial) – for the sense of taste and controlling facial muscles, tear glands and salivary glands (mixed). Nerve VIII (Vestibulocochlear)- for the senses of hearing and equilibrium (sensory). Nerve IX (Glossopharyngeal)- for controlling muscles in the pharynx and to control salivary glands (mixed). Nerve X (Vagus)- for controlling muscles used in speech, swallowing, and the digestive tract, and controls cardiac and smooth muscles (mixed). Nerve XI (Accessory)- for controlling muscles of soft palate, pharynx and larynx (primarily motor). Nerve XII (Hypoglossal) for controlling muscles that move the tongue ( primarily motor). -

Peripheral Nervous System
Peripheral Nervous System Nervous system consists of CNS = brain and spinal cord ~90% (90 Bil) of all neurons in body are in CNS PNS = Cranial nerves and spinal nerves ~10% (10 Bil) of all neurons in body are in PNS PNS is our link to the outside world without it CNS us useless sensory deprivation hallucinations sensory (afferent) neurons ~2-3M; 6-8x’s more sensory than motor fibers motor (efferent) neurons ~350,000 efferent fibers somatic motor neurons autonomic motor neurons these neurons are bundled into nerves difference between nerve and neuron: neuron = individual nerve cell nerve = bundle of axons outside CNS surrounded by layers of connective tissue CNS PNS Axons Tracts Nerves Cell Bodies Nuclei Ganglia Nerves consist of either sensory or motor neurons or a combination of both (=mixed nerves) mixed nerves often carry both somatic and autonomic motor fibers ganglia examples: dorsal root ganglia = cell bodies of sensory neurons autonomic chain ganglia = cell bodies, dendrites & synapses of autonomic motor neurons PNS consists of 43 pairs of nerves branching from the CNS: 12 pairs of cranial nerves 31 pairs of spinal nerves Cranial Nerves 12 pairs of cranial nerves 1 structurally originate from: cerebrum: I, II midbrain: III, IV pons: V, VI, VII,VIII (pons/medulla border) medulla: IX, X, XI, XII functionally: some are sensory only: I. Olfactory [sense of smell] II. Optic [sense of sight] VIII. Vestibulocochlear [senses of hearing and balance] -injury causes deafness some are motor only: III. Oculomotor IV. Trochlear [eye movements] VI. Abducens -injury to VI causes eye to turn inward some are mixed nerves: V. -
PN1 (Midha) Microanatomy of Peripheral Nerves-Part1.Pdf
Peripheral Nerve Basics • Consist of processes of cell bodies found in the DRG, anterior horn, and autonomic ganglia • Organized by several distinct connective tissue layers – the epineurium, perineurium, and endoneurium • Vascular supply provided by the vasa nervorum Peripheral Nerve Basics • Neuronal processes bound into fascicles by perineurium • Fascicles bound into nerves by epineurium • Endoneurium is a division of the perineurium which form thin layers of connective tissue surrounding neuronal fibers in a fascicle Sural nerve in cross-section Epineurium • Loose areolar tissue with sparse, longitudinally-oriented collagen fibers • Some elastic fibers where epineurium abuts perineurium • Able to accommodate a significant amount of nerve stretching and movement • Increases in thickness where nerves cross joints • Constitutes an increasing proportion of nerves as they increase in size • Epineurial fat helps cushion nerves from compressive injury • Decreased epineurial fat found in patients with diabetes Perineurium • Cellular component composed of laminated fibroblasts of up to 15 layers in thickness which are bounded by a basal lamina • Semi-permeable: inner lamellae have tight junctions, providing a barrier to intercellular transport of macromolecules – Tight junctions can be loosened with topical anaesthetics and with osmotic change Perineurium • Exhibits a slightly positive internal pressure – Fascicular contents herniate upon perineurial injury • Under tension longitudinally – Nerve segment shortens upon transection – may complicate surgical repair as nerve can be stretched only approximately 10% before being inhibited by collagen Endoneurium • Intrafascicular connective tissue consisting of a collagenous matrix in the interstitial space • Develops into partitions of dense connective tissue between diverging fascicles and eventually becomes perineurium when the fascicles separate • Collagen fibers are longitudinally-oriented and run along nerve fibers and capillaries.