Dyshomeostatic Modulation of Ca
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Nav 1.1 Channels in Axon Initial Segments of Bipolar Cells Augment
The Journal of Neuroscience, October 9, 2013 • 33(41):16045–16059 • 16045 Systems/Circuits NaV1.1 Channels in Axon Initial Segments of Bipolar Cells Augment Input to Magnocellular Visual Pathways in the Primate Retina Theresa Puthussery,1 Sowmya Venkataramani,1 Jacqueline Gayet-Primo,1 Robert G. Smith,2 and W. Rowland Taylor1 1Casey Eye Institute, Department of Ophthalmology, Oregon Health & Science University, Portland, Oregon 97239, and 2Department of Neuroscience, University of Pennsylvania, Philadelphia, Pennsylvania 19104 In the primate visual system, the ganglion cells of the magnocellular pathway underlie motion and flicker detection and are relatively transient,whilethemoresustainedganglioncellsoftheparvocellularpathwayhavecomparativelylowertemporalresolution,butencode higher spatial frequencies. Although it is presumed that functional differences in bipolar cells contribute to the tuning of the two pathways, the properties of the relevant bipolar cells have not yet been examined in detail. Here, by making patch-clamp recordings in acuteslicesofmacaqueretina,weshowthatthebipolarcellswithinthemagnocellularpathway,butnottheparvocellularpathway,exhibit voltage-gated sodium (NaV ), T-type calcium (CaV ), and hyperpolarization-activated, cyclic nucleotide-gated (HCN) currents, and can generate action potentials. Using immunohistochemistry in macaque and human retinae, we show that NaV1.1 is concentrated in an axon initial segment (AIS)-like region of magnocellular pathway bipolar cells, a specialization not seen in transient bipolar cells of other vertebrates. In contrast, CaV3.1 channels were localized to the somatodendritic compartment and proximal axon, but were excluded from the AIS, while HCN1 channels were concentrated in the axon terminal boutons. Simulations using a compartmental model reproduced physiological results and indicate that magnocellular pathway bipolar cells initiate spikes in the AIS. Finally, we demonstrate that NaV channels in bipolar cells augment excitatory input to parasol ganglion cells of the magnocellular pathway. -

The Mineralocorticoid Receptor Leads to Increased Expression of EGFR
www.nature.com/scientificreports OPEN The mineralocorticoid receptor leads to increased expression of EGFR and T‑type calcium channels that support HL‑1 cell hypertrophy Katharina Stroedecke1,2, Sandra Meinel1,2, Fritz Markwardt1, Udo Kloeckner1, Nicole Straetz1, Katja Quarch1, Barbara Schreier1, Michael Kopf1, Michael Gekle1 & Claudia Grossmann1* The EGF receptor (EGFR) has been extensively studied in tumor biology and recently a role in cardiovascular pathophysiology was suggested. The mineralocorticoid receptor (MR) is an important efector of the renin–angiotensin–aldosterone‑system and elicits pathophysiological efects in the cardiovascular system; however, the underlying molecular mechanisms are unclear. Our aim was to investigate the importance of EGFR for MR‑mediated cardiovascular pathophysiology because MR is known to induce EGFR expression. We identifed a SNP within the EGFR promoter that modulates MR‑induced EGFR expression. In RNA‑sequencing and qPCR experiments in heart tissue of EGFR KO and WT mice, changes in EGFR abundance led to diferential expression of cardiac ion channels, especially of the T‑type calcium channel CACNA1H. Accordingly, CACNA1H expression was increased in WT mice after in vivo MR activation by aldosterone but not in respective EGFR KO mice. Aldosterone‑ and EGF‑responsiveness of CACNA1H expression was confrmed in HL‑1 cells by Western blot and by measuring peak current density of T‑type calcium channels. Aldosterone‑induced CACNA1H protein expression could be abrogated by the EGFR inhibitor AG1478. Furthermore, inhibition of T‑type calcium channels with mibefradil or ML218 reduced diameter, volume and BNP levels in HL‑1 cells. In conclusion the MR regulates EGFR and CACNA1H expression, which has an efect on HL‑1 cell diameter, and the extent of this regulation seems to depend on the SNP‑216 (G/T) genotype. -

Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model
Downloaded from http://www.jimmunol.org/ by guest on September 25, 2021 T + is online at: average * The Journal of Immunology , 34 of which you can access for free at: 2016; 197:1477-1488; Prepublished online 1 July from submission to initial decision 4 weeks from acceptance to publication 2016; doi: 10.4049/jimmunol.1600589 http://www.jimmunol.org/content/197/4/1477 Molecular Profile of Tumor-Specific CD8 Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. Waugh, Sonia M. Leach, Brandon L. Moore, Tullia C. Bruno, Jonathan D. Buhrman and Jill E. Slansky J Immunol cites 95 articles Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2016/07/01/jimmunol.160058 9.DCSupplemental This article http://www.jimmunol.org/content/197/4/1477.full#ref-list-1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material References Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2016 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 25, 2021. The Journal of Immunology Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. -

Calcium-Induced Calcium Release in Noradrenergic Neurons of the Locus Coeruleus
bioRxiv preprint doi: https://doi.org/10.1101/853283; this version posted November 23, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. Calcium-induced calcium release in noradrenergic neurons of the locus coeruleus Hiroyuki Kawano1, Sara B. Mitchell1, Jin-Young Koh1,2,3, Kirsty M. Goodman1,4, and N. Charles Harata1,* 1 Department of Molecular Physiology and Biophysics, University of Iowa Carver College of Medicine, Iowa City, IA, USA 2 Molecular Otolaryngology and Renal Research Laboratories, Department of Otolaryngology-Head and Neck Surgery, University of Iowa Carver College of Medicine, Iowa City, IA, USA 3 Department of Biomedical Engineering, University of Iowa College of Engineering, Iowa City, IA, USA 4 Department of Biology & Biochemistry, University of Bath, Bath, UK * Correspondence to: N. Charles Harata, MD, PhD Department of Molecular Physiology & Biophysics University of Iowa Carver College of Medicine 51 Newton Road, Iowa City, IA 52242, USA Phone: 1-319-335-7820 Fax: 1-319-335-7330 E-mail: [email protected] Number of words: 8620; Number of figures: 12. 1 bioRxiv preprint doi: https://doi.org/10.1101/853283; this version posted November 23, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. -
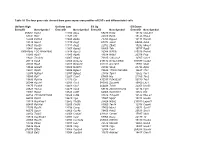

Table S1 the Four Gene Sets Derived from Gene Expression Profiles of Escs and Differentiated Cells
Table S1 The four gene sets derived from gene expression profiles of ESCs and differentiated cells Uniform High Uniform Low ES Up ES Down EntrezID GeneSymbol EntrezID GeneSymbol EntrezID GeneSymbol EntrezID GeneSymbol 269261 Rpl12 11354 Abpa 68239 Krt42 15132 Hbb-bh1 67891 Rpl4 11537 Cfd 26380 Esrrb 15126 Hba-x 55949 Eef1b2 11698 Ambn 73703 Dppa2 15111 Hand2 18148 Npm1 11730 Ang3 67374 Jam2 65255 Asb4 67427 Rps20 11731 Ang2 22702 Zfp42 17292 Mesp1 15481 Hspa8 11807 Apoa2 58865 Tdh 19737 Rgs5 100041686 LOC100041686 11814 Apoc3 26388 Ifi202b 225518 Prdm6 11983 Atpif1 11945 Atp4b 11614 Nr0b1 20378 Frzb 19241 Tmsb4x 12007 Azgp1 76815 Calcoco2 12767 Cxcr4 20116 Rps8 12044 Bcl2a1a 219132 D14Ertd668e 103889 Hoxb2 20103 Rps5 12047 Bcl2a1d 381411 Gm1967 17701 Msx1 14694 Gnb2l1 12049 Bcl2l10 20899 Stra8 23796 Aplnr 19941 Rpl26 12096 Bglap1 78625 1700061G19Rik 12627 Cfc1 12070 Ngfrap1 12097 Bglap2 21816 Tgm1 12622 Cer1 19989 Rpl7 12267 C3ar1 67405 Nts 21385 Tbx2 19896 Rpl10a 12279 C9 435337 EG435337 56720 Tdo2 20044 Rps14 12391 Cav3 545913 Zscan4d 16869 Lhx1 19175 Psmb6 12409 Cbr2 244448 Triml1 22253 Unc5c 22627 Ywhae 12477 Ctla4 69134 2200001I15Rik 14174 Fgf3 19951 Rpl32 12523 Cd84 66065 Hsd17b14 16542 Kdr 66152 1110020P15Rik 12524 Cd86 81879 Tcfcp2l1 15122 Hba-a1 66489 Rpl35 12640 Cga 17907 Mylpf 15414 Hoxb6 15519 Hsp90aa1 12642 Ch25h 26424 Nr5a2 210530 Leprel1 66483 Rpl36al 12655 Chi3l3 83560 Tex14 12338 Capn6 27370 Rps26 12796 Camp 17450 Morc1 20671 Sox17 66576 Uqcrh 12869 Cox8b 79455 Pdcl2 20613 Snai1 22154 Tubb5 12959 Cryba4 231821 Centa1 17897 -
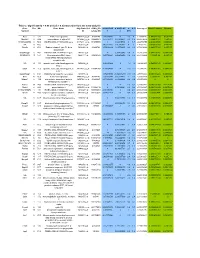
Table 2. Significant
Table 2. Significant (Q < 0.05 and |d | > 0.5) transcripts from the meta-analysis Gene Chr Mb Gene Name Affy ProbeSet cDNA_IDs d HAP/LAP d HAP/LAP d d IS Average d Ztest P values Q-value Symbol ID (study #5) 1 2 STS B2m 2 122 beta-2 microglobulin 1452428_a_at AI848245 1.75334941 4 3.2 4 3.2316485 1.07398E-09 5.69E-08 Man2b1 8 84.4 mannosidase 2, alpha B1 1416340_a_at H4049B01 3.75722111 3.87309653 2.1 1.6 2.84852656 5.32443E-07 1.58E-05 1110032A03Rik 9 50.9 RIKEN cDNA 1110032A03 gene 1417211_a_at H4035E05 4 1.66015788 4 1.7 2.82772795 2.94266E-05 0.000527 NA 9 48.5 --- 1456111_at 3.43701477 1.85785922 4 2 2.8237185 9.97969E-08 3.48E-06 Scn4b 9 45.3 Sodium channel, type IV, beta 1434008_at AI844796 3.79536664 1.63774235 3.3 2.3 2.75319499 1.48057E-08 6.21E-07 polypeptide Gadd45gip1 8 84.1 RIKEN cDNA 2310040G17 gene 1417619_at 4 3.38875643 1.4 2 2.69163229 8.84279E-06 0.0001904 BC056474 15 12.1 Mus musculus cDNA clone 1424117_at H3030A06 3.95752801 2.42838452 1.9 2.2 2.62132809 1.3344E-08 5.66E-07 MGC:67360 IMAGE:6823629, complete cds NA 4 153 guanine nucleotide binding protein, 1454696_at -3.46081884 -4 -1.3 -1.6 -2.6026947 8.58458E-05 0.0012617 beta 1 Gnb1 4 153 guanine nucleotide binding protein, 1417432_a_at H3094D02 -3.13334396 -4 -1.6 -1.7 -2.5946297 1.04542E-05 0.0002202 beta 1 Gadd45gip1 8 84.1 RAD23a homolog (S. -

Potassium Channels in Epilepsy
Downloaded from http://perspectivesinmedicine.cshlp.org/ on September 28, 2021 - Published by Cold Spring Harbor Laboratory Press Potassium Channels in Epilepsy Ru¨diger Ko¨hling and Jakob Wolfart Oscar Langendorff Institute of Physiology, University of Rostock, Rostock 18057, Germany Correspondence: [email protected] This review attempts to give a concise and up-to-date overview on the role of potassium channels in epilepsies. Their role can be defined from a genetic perspective, focusing on variants and de novo mutations identified in genetic studies or animal models with targeted, specific mutations in genes coding for a member of the large potassium channel family. In these genetic studies, a demonstrated functional link to hyperexcitability often remains elusive. However, their role can also be defined from a functional perspective, based on dy- namic, aggravating, or adaptive transcriptional and posttranslational alterations. In these cases, it often remains elusive whether the alteration is causal or merely incidental. With 80 potassium channel types, of which 10% are known to be associated with epilepsies (in humans) or a seizure phenotype (in animals), if genetically mutated, a comprehensive review is a challenging endeavor. This goal may seem all the more ambitious once the data on posttranslational alterations, found both in human tissue from epilepsy patients and in chronic or acute animal models, are included. We therefore summarize the literature, and expand only on key findings, particularly regarding functional alterations found in patient brain tissue and chronic animal models. INTRODUCTION TO POTASSIUM evolutionary appearance of voltage-gated so- CHANNELS dium (Nav)andcalcium (Cav)channels, Kchan- nels are further diversified in relation to their otassium (K) channels are related to epilepsy newer function, namely, keeping neuronal exci- Psyndromes on many different levels, ranging tation within limits (Anderson and Greenberg from direct control of neuronal excitability and 2001; Hille 2001). -
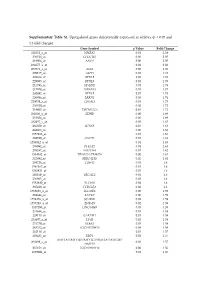
Supplementary Table S1. Upregulated Genes Differentially
Supplementary Table S1. Upregulated genes differentially expressed in athletes (p < 0.05 and 1.3-fold change) Gene Symbol p Value Fold Change 221051_s_at NMRK2 0.01 2.38 236518_at CCDC183 0.00 2.05 218804_at ANO1 0.00 2.05 234675_x_at 0.01 2.02 207076_s_at ASS1 0.00 1.85 209135_at ASPH 0.02 1.81 228434_at BTNL9 0.03 1.81 229985_at BTNL9 0.01 1.79 215795_at MYH7B 0.01 1.78 217979_at TSPAN13 0.01 1.77 230992_at BTNL9 0.01 1.75 226884_at LRRN1 0.03 1.74 220039_s_at CDKAL1 0.01 1.73 236520_at 0.02 1.72 219895_at TMEM255A 0.04 1.72 201030_x_at LDHB 0.00 1.69 233824_at 0.00 1.69 232257_s_at 0.05 1.67 236359_at SCN4B 0.04 1.64 242868_at 0.00 1.63 1557286_at 0.01 1.63 202780_at OXCT1 0.01 1.63 1556542_a_at 0.04 1.63 209992_at PFKFB2 0.04 1.63 205247_at NOTCH4 0.01 1.62 1554182_at TRIM73///TRIM74 0.00 1.61 232892_at MIR1-1HG 0.02 1.61 204726_at CDH13 0.01 1.6 1561167_at 0.01 1.6 1565821_at 0.01 1.6 210169_at SEC14L5 0.01 1.6 236963_at 0.02 1.6 1552880_at SEC16B 0.02 1.6 235228_at CCDC85A 0.02 1.6 1568623_a_at SLC35E4 0.00 1.59 204844_at ENPEP 0.00 1.59 1552256_a_at SCARB1 0.02 1.59 1557283_a_at ZNF519 0.02 1.59 1557293_at LINC00969 0.03 1.59 231644_at 0.01 1.58 228115_at GAREM1 0.01 1.58 223687_s_at LY6K 0.02 1.58 231779_at IRAK2 0.03 1.58 243332_at LOC105379610 0.04 1.58 232118_at 0.01 1.57 203423_at RBP1 0.02 1.57 AMY1A///AMY1B///AMY1C///AMY2A///AMY2B// 208498_s_at 0.03 1.57 /AMYP1 237154_at LOC101930114 0.00 1.56 1559691_at 0.01 1.56 243481_at RHOJ 0.03 1.56 238834_at MYLK3 0.01 1.55 213438_at NFASC 0.02 1.55 242290_at TACC1 0.04 1.55 ANKRD20A1///ANKRD20A12P///ANKRD20A2/// -

The Metabotropic Glutamate Receptor Mglur1 Regulates the Voltage-Gated Potassium Channel Kv1.2 Through Agonist-Dependent and Agonist-Independent Mechanisms
University of Vermont ScholarWorks @ UVM Graduate College Dissertations and Theses Dissertations and Theses 2019 The etM abotropic glutamate receptor mGluR1 regulates the voltage-gated potassium channel Kv1.2 through agonist-dependent and agonist- independent mechanisms Sharath Chandra Madasu University of Vermont Follow this and additional works at: https://scholarworks.uvm.edu/graddis Part of the Cell Biology Commons, Neuroscience and Neurobiology Commons, and the Pharmacology Commons Recommended Citation Madasu, Sharath Chandra, "The eM tabotropic glutamate receptor mGluR1 regulates the voltage-gated potassium channel Kv1.2 through agonist-dependent and agonist-independent mechanisms" (2019). Graduate College Dissertations and Theses. 982. https://scholarworks.uvm.edu/graddis/982 This Dissertation is brought to you for free and open access by the Dissertations and Theses at ScholarWorks @ UVM. It has been accepted for inclusion in Graduate College Dissertations and Theses by an authorized administrator of ScholarWorks @ UVM. For more information, please contact [email protected]. THE METABOTROPIC GLUTAMATE RECEPTOR MGLUR1 REGULATES THE VOLTAGE-GATED POTASSIUM CHANNEL KV1.2 THROUGH AGONIST-DEPENDENT AND AGONIST-INDEPENDENT MECHANISMS. A Dissertation Presented by Sharath Chandra Madasu to The Faculty of the Graduate College of The University of Vermont In Partial Fulfillment of the Requirements for the Degree of Doctor of Philosophy Specializing in Cellular Molecular and Biomedical Science January, 2019 Defense Date: September 27, 2018 Dissertation Examination Committee: Anthony D. Morielli, PhD., Advisor John Green, PhD., Chairperson Karen Lounsbury, Ph.D. Benedek Erdos, PhD. Cynthia J. Forehand, Ph.D., Dean of the Graduate College ABSTRACT The voltage gated potassium channel Kv1.2 plays a key role in the central nervous system and mutations in Kv1.2 cause neurological disorders such as epilepsies and ataxias. -

Chronic Social Isolation Reduces 5-HT Neuronal Activity Via Upregulated SK3 Calcium-Activated Potassium Channels Derya Sargin1, David K Oliver1, Evelyn K Lambe1,2,3*
SHORT REPORT Chronic social isolation reduces 5-HT neuronal activity via upregulated SK3 calcium-activated potassium channels Derya Sargin1, David K Oliver1, Evelyn K Lambe1,2,3* 1Department of Physiology, University of Toronto, Toronto, Canada; 2Department of Obstetrics and Gynaecology, University of Toronto, Toronto, Canada; 3Department of Psychiatry, University of Toronto, Toronto, Canada Abstract The activity of serotonin (5-HT) neurons is critical for mood regulation. In a mouse model of chronic social isolation, a known risk factor for depressive illness, we show that 5-HT neurons in the dorsal raphe nucleus are less responsive to stimulation. Probing the responsible cellular mechanisms pinpoints a disturbance in the expression and function of small-conductance Ca2+-activated K+ (SK) channels and reveals an important role for both SK2 and SK3 channels in normal regulation of 5-HT neuronal excitability. Chronic social isolation renders 5-HT neurons insensitive to SK2 blockade, however inhibition of the upregulated SK3 channels restores normal excitability. In vivo, we demonstrate that inhibiting SK channels normalizes chronic social isolation- induced anxiety/depressive-like behaviors. Our experiments reveal a causal link for the first time between SK channel dysregulation and 5-HT neuron activity in a lifelong stress paradigm, suggesting these channels as targets for the development of novel therapies for mood disorders. DOI: 10.7554/eLife.21416.001 Introduction *For correspondence: evelyn. Major depression is a prevalent and debilitating disease for which standard treatments remain inef- [email protected] fective. Social isolation has long been implicated as a risk factor for depression in humans Competing interests: The (Cacioppo et al., 2002,2006; Holt-Lunstad et al., 2010) and induces anxiety- and depressive-like authors declare that no behaviors in rodents (Koike et al., 2009; Wallace et al., 2009; Dang et al., 2015; Shimizu et al., competing interests exist. -

Apamin As a Selective Blocker of the Calcium-Dependent Potassium
Proc. NatL Acad. Sci. USA Vol. 79, pp. 1308-1312, February 1982 Neurobiology Apamin as a selective blocker of the calcium-dependent potassium channel in neuroblastoma cells: Voltage-clamp and biochemical characterization of the toxin receptor (receptor binding/neuroblastoma cell differentiation) M. HUGUES, G. ROMEY, D. DUVAL, J. P. VINCENT, AND M. LAZDUNSKI Centre de Biochimie du Centre National de la Recherche Scientifique, Facult, des Sciences, Parc Valrose, 06034 Nice Cedex, France Communicated by Jean-Marie P. Lehn, October 13, 1981 ABSTRACT This paper describes the interaction of apamin, MATERIALS AND METHODS a bee venom neurotoxin, with the mouse neuroblastoma cell mem- brane. Voltage-clamp analyses have shown thatapamin atlowcon- Cultures of Neuroblastoma Cells. Neuroblastoma cells centrations specifically blocks the Ca2"-dependent K+ channel in (clone N1E 115) were grown as described (12); they were in- differentiated neuroblastoma cells. Binding experiments with duced to differentiate in the presence of1% fetal calfserum and highly radiolabeled toxin indicate that the dissociation constant of 1.5% dimethyl sulfoxide. the apamin-receptor complex in differentiated neuroblastoma lodination ofApamin. Apamin was purified as described (13). cells is 15-22 pM and the maximal binding capacity is 12 fmol/ There is no tyrosine residue in the sequence, but there is his- mg ofprotein. The receptor is destroyed by proteases, suggesting tidine residue that is not essential for activity (4) and that can that it is a protein.The binding capacity ofneuroblastoma cells for be iodinated. It has been found that the previously radiolabeled apamin dramatically increases during the transition described to prepare "2I-labeled apamin ('p9rocedureI-apamin) (14) could from the nondifferentiated to the differentiated state. -

Transcriptomic Analysis of Native Versus Cultured Human and Mouse Dorsal Root Ganglia Focused on Pharmacological Targets Short
bioRxiv preprint doi: https://doi.org/10.1101/766865; this version posted September 12, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-ND 4.0 International license. Transcriptomic analysis of native versus cultured human and mouse dorsal root ganglia focused on pharmacological targets Short title: Comparative transcriptomics of acutely dissected versus cultured DRGs Andi Wangzhou1, Lisa A. McIlvried2, Candler Paige1, Paulino Barragan-Iglesias1, Carolyn A. Guzman1, Gregory Dussor1, Pradipta R. Ray1,#, Robert W. Gereau IV2, # and Theodore J. Price1, # 1The University of Texas at Dallas, School of Behavioral and Brain Sciences and Center for Advanced Pain Studies, 800 W Campbell Rd. Richardson, TX, 75080, USA 2Washington University Pain Center and Department of Anesthesiology, Washington University School of Medicine # corresponding authors [email protected], [email protected] and [email protected] Funding: NIH grants T32DA007261 (LM); NS065926 and NS102161 (TJP); NS106953 and NS042595 (RWG). The authors declare no conflicts of interest Author Contributions Conceived of the Project: PRR, RWG IV and TJP Performed Experiments: AW, LAM, CP, PB-I Supervised Experiments: GD, RWG IV, TJP Analyzed Data: AW, LAM, CP, CAG, PRR Supervised Bioinformatics Analysis: PRR Drew Figures: AW, PRR Wrote and Edited Manuscript: AW, LAM, CP, GD, PRR, RWG IV, TJP All authors approved the final version of the manuscript. 1 bioRxiv preprint doi: https://doi.org/10.1101/766865; this version posted September 12, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity.