IRAK1: Oncotarget in MDS and AML
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
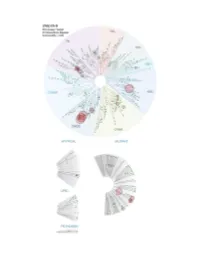
Profiling Data
Compound Name DiscoveRx Gene Symbol Entrez Gene Percent Compound Symbol Control Concentration (nM) JNK-IN-8 AAK1 AAK1 69 1000 JNK-IN-8 ABL1(E255K)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317I)-nonphosphorylated ABL1 87 1000 JNK-IN-8 ABL1(F317I)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317L)-nonphosphorylated ABL1 65 1000 JNK-IN-8 ABL1(F317L)-phosphorylated ABL1 61 1000 JNK-IN-8 ABL1(H396P)-nonphosphorylated ABL1 42 1000 JNK-IN-8 ABL1(H396P)-phosphorylated ABL1 60 1000 JNK-IN-8 ABL1(M351T)-phosphorylated ABL1 81 1000 JNK-IN-8 ABL1(Q252H)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(Q252H)-phosphorylated ABL1 56 1000 JNK-IN-8 ABL1(T315I)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(T315I)-phosphorylated ABL1 92 1000 JNK-IN-8 ABL1(Y253F)-phosphorylated ABL1 71 1000 JNK-IN-8 ABL1-nonphosphorylated ABL1 97 1000 JNK-IN-8 ABL1-phosphorylated ABL1 100 1000 JNK-IN-8 ABL2 ABL2 97 1000 JNK-IN-8 ACVR1 ACVR1 100 1000 JNK-IN-8 ACVR1B ACVR1B 88 1000 JNK-IN-8 ACVR2A ACVR2A 100 1000 JNK-IN-8 ACVR2B ACVR2B 100 1000 JNK-IN-8 ACVRL1 ACVRL1 96 1000 JNK-IN-8 ADCK3 CABC1 100 1000 JNK-IN-8 ADCK4 ADCK4 93 1000 JNK-IN-8 AKT1 AKT1 100 1000 JNK-IN-8 AKT2 AKT2 100 1000 JNK-IN-8 AKT3 AKT3 100 1000 JNK-IN-8 ALK ALK 85 1000 JNK-IN-8 AMPK-alpha1 PRKAA1 100 1000 JNK-IN-8 AMPK-alpha2 PRKAA2 84 1000 JNK-IN-8 ANKK1 ANKK1 75 1000 JNK-IN-8 ARK5 NUAK1 100 1000 JNK-IN-8 ASK1 MAP3K5 100 1000 JNK-IN-8 ASK2 MAP3K6 93 1000 JNK-IN-8 AURKA AURKA 100 1000 JNK-IN-8 AURKA AURKA 84 1000 JNK-IN-8 AURKB AURKB 83 1000 JNK-IN-8 AURKB AURKB 96 1000 JNK-IN-8 AURKC AURKC 95 1000 JNK-IN-8 -

Targeting Myddosome Signaling in Waldenström’S
Author Manuscript Published OnlineFirst on August 20, 2018; DOI: 10.1158/1078-0432.CCR-17-3265 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. IRAK 1/4 Inhibition in Waldenström’s Ni, H. et al. Targeting Myddosome Signaling in Waldenström’s Macroglobulinemia with the Interleukin-1 Receptor- associated Kinase 1/4 Inhibitor R191 Haiwen Ni1,2,#, Fazal Shirazi2,#, Veerabhadran Baladandayuthapani3, Heather Lin3, Isere Kuiatse2, Hua Wang2, Richard J. Jones2, Zuzana Berkova2, Yasumichi Hitoshi4, Stephen M. Ansell5, Steven P. Treon6, Sheeba K. Thomas2, Hans C. Lee2, Zhiqiang Wang2, R. Eric Davis2, and Robert Z. Orlowski2,7,* 1Department of Hematology, The Affiliated Hospital of Nanjing University of Traditional Chinese Medicine, Nanjing, JangSu, China; 2Department of Lymphoma and Myeloma, The University of Texas MD Anderson Cancer Center, Houston, TX; 3Department of Biostatistics, The University of Texas MD Anderson Cancer Center, Houston, TX; 4Rigel, South San Francisco, CA; The 5Division of Hematology, Mayo Clinic, Rochester, MN; The 6Dana Farber Cancer Institute, Harvard Medical School, Boston, MA. 7Department of Experimental Therapeutics, The University of Texas MD Anderson Cancer Center, Houston, TX #Indicates that these authors contributed equally. Address correspondence to: Dr. Robert Z. Orlowski, The University of Texas MD Anderson Cancer Center, Department of Lymphoma and Myeloma, 1515 Holcombe Blvd., Unit 429, Houston, TX 77030-4009, E-mail: [email protected], Telephone 713-794-3234, Fax 713- 563-5067 Page 1 Downloaded from clincancerres.aacrjournals.org on September 24, 2021. © 2018 American Association for Cancer Research. Author Manuscript Published OnlineFirst on August 20, 2018; DOI: 10.1158/1078-0432.CCR-17-3265 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. -

Targeting Cyclin-Dependent Kinase 9 and Myeloid Cell Leukaemia 1 in MYC-Driven B-Cell Lymphoma
Targeting cyclin-dependent kinase 9 and myeloid cell leukaemia 1 in MYC-driven B-cell lymphoma Gareth Peter Gregory ORCID ID: 0000-0002-4170-0682 Thesis for Doctor of Philosophy September 2016 Sir Peter MacCallum Department of Oncology The University of Melbourne Doctor of Philosophy Submitted in total fulfilment of the degree of Abstract Aggressive B-cell lymphomas include diffuse large B-cell lymphoma, Burkitt lymphoma and intermediate forms. Despite high response rates to conventional immuno-chemotherapeutic approaches, an unmet need for novel therapeutic by resistance to chemotherapy and radiotherapy. The proto-oncogene MYC is strategies is required in the setting of relapsed and refractory disease, typified frequently dysregulated in the aggressive B-cell lymphomas, however, it has proven an elusive direct therapeutic target. MYC-dysregulated disease maintains a ‘transcriptionally-addicted’ state, whereby perturbation of A significant body of evidence is accumulating to suggest that RNA polymerase II activity may indirectly antagonise MYC activity. Furthermore, very recent studies implicate anti-apoptotic myeloid cell leukaemia 1 (MCL-1) as a critical survival determinant of MYC-driven lymphoma. This thesis utilises pharmacologic and genetic techniques in MYC-driven models of aggressive B-cell lymphoma to demonstrate that cyclin-dependent kinase 9 (CDK9) and MCL-1 are oncogenic dependencies of this subset of disease. The cyclin-dependent kinase inhibitor, dinaciclib, and more selective CDK9 inhibitors downregulation of MCL1 are used -

Eradicating Chronic Myeloid Leukemia Stem Cells by IRAK1/4 Inhibitors
Eradicating chronic myeloid leukemia stem cells by IRAK1/4 inhibitors Yosuke Tanaka ( [email protected] ) The Institute of Medical Science, The University of Tokyo Tsuyoshi Fukushima The Institute of Medical Science, The University of Tokyo Keiko Mikami The Institute of Medical Science, The University of Tokyo Shun Tsuchiya Juntendo University Moe Tamura The Institute of Medical Science, The University of Tokyo Keito Adachi The Institute of Medical Science, The University of Tokyo Terumasa Umemoto Kumamoto University https://orcid.org/0000-0003-0423-9003 Naoki Watanabe Juntendo University Soji Morishita Juntendo University https://orcid.org/0000-0003-1081-0130 Misa Imai Juntendo University Masayoshi Nagasawa Juntendo University Marito Araki Juntendo University https://orcid.org/0000-0002-3502-5000 Hitoshi Takizawa International Research Center for Medical Sciences, Kumamoto University https://orcid.org/0000-0002- 5276-5430 Tomofusa Fukuyama The Institute of Medical Science, The University of Tokyo, Tokyo https://orcid.org/0000-0002-0709- 3188 Chrystelle Lamagna Rigel Esteban Masuda Rigel Ryoji Ito Central Institute for Experimental Animals https://orcid.org/0000-0003-2903-2332 Susumu Goyama The Institute of Medical Science, The University of Tokyo Norio Komatsu Juntendo University Tomoiku Takaku Juntendo University Toshio Kitamura The Institute of Medical Science, The University of Tokyo Article Keywords: chronic myeloid leukemia, leukemia stem cells, imatinib, IRAK1/4, PD-L1 Posted Date: May 20th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-449398/v1 -

A Comparative Survey of Functional Footprints of EGFR Pathway Mutations in Human Cancers
Oncogene (2014) 33, 5078–5089 & 2014 Macmillan Publishers Limited All rights reserved 0950-9232/14 www.nature.com/onc ORIGINAL ARTICLE A comparative survey of functional footprints of EGFR pathway mutations in human cancers A Lane1,4, A Segura-Cabrera1,4 and K Komurov1,2,3 Genes functioning in epidermal growth factor receptor (EGFR) signaling pathways are among the most frequently activated oncogenes in human cancers. We have conducted a comparative analysis of functional footprints (that is, effect on signaling and transcriptional landscapes in cells) associated with oncogenic and tumor suppressor mutations in EGFR pathway genes in human cancers. We have found that mutations in the EGFR pathway differentially have an impact on signaling and metabolic pathways in cancer cells in a mutation- and tissue-selective manner. For example, although signaling and metabolic profiles of breast tumors with PIK3CA or AKT1 mutations are, as expected, highly similar, they display markedly different, sometimes even opposite, profiles to those with ERBB2 or EGFR amplifications. On the other hand, although low-grade gliomas and glioblastomas, both brain cancers, driven by EGFR amplifications are highly functionally similar, their functional footprints are significantly different from lung and breast tumors driven by EGFR or ERBB2. Overall, these observations argue that, contrary to expectations, the mechanisms of tumorigenicity associated with mutations in different genes along the same pathway, or in the same gene across different tissues, may be highly different. We present evidence that oncogenic functional footprints in cancer cell lines have significantly diverged from those in tumor tissues, which potentially explains the discrepancy of our findings with the current knowledge. -

Activity Across Human Cell Types Different Requirements for IRAK1/4
Immune Complex-Mediated Cell Activation from Systemic Lupus Erythematosus and Rheumatoid Arthritis Patients Elaborate Different Requirements for IRAK1/4 Kinase This information is current as Activity across Human Cell Types of October 7, 2021. Eugene Y. Chiang, Xin Yu and Jane L. Grogan J Immunol 2011; 186:1279-1288; Prepublished online 15 December 2010; doi: 10.4049/jimmunol.1002821 Downloaded from http://www.jimmunol.org/content/186/2/1279 Supplementary http://www.jimmunol.org/content/suppl/2010/12/15/jimmunol.100282 Material 1.DC1 http://www.jimmunol.org/ References This article cites 53 articles, 23 of which you can access for free at: http://www.jimmunol.org/content/186/2/1279.full#ref-list-1 Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision by guest on October 7, 2021 • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology Immune Complex-Mediated Cell Activation from Systemic Lupus Erythematosus and Rheumatoid Arthritis Patients Elaborate Different Requirements for IRAK1/4 Kinase Activity across Human Cell Types Eugene Y. -

Supplemental Digital Content (Sdc) Sdc, Materials
SUPPLEMENTAL DIGITAL CONTENT (SDC) SDC, MATERIALS AND METHODS Animals This study used 9-12 week old male C57BL/6 mice (Jackson Laboratory, Bar Harbor, ME). This study conformed to the National Institutes of Health guidelines and was conducted under animal protocols approved by the University of Virginia’s Institutional Animal Care and Use Committee. Murine DCD Lung Procedure Mice were anesthetized by isoflurane inhalation and euthanized by cervical dislocation followed by a 60-minute period of “no-touch” warm ischemia. Mice then underwent extended median sternotomy and midline cervical exposure followed by intubation for the initiation of mechanical ventilation at 120 strokes/minute with room air. The left atrium was vented via an atriotomy followed by infusion of the lungs with 3 mL 4°C Perfadex® solution (Vitrolife Inc., Denver, CO) supplemented with THAM Solution (Vitrolife, Kungsbacka, Sweden), estimating weight-based volume recommendations for pulmonary artery perfusion (140mL/kg) (1). The chest was then packed with ice and the trachea occluded by silk-suture tie at tidal volume (7µL/g body weight) prior to cold static preservation (CSP) for 60 minutes at 4°C. Mice were then randomized into three experimental groups: 1) CSP alone with no EVLP, 2) EVLP with Steen solution and 3) EVLP with Steen solution supplemented with the highly selective A2AR agonist, ATL1223 (30nM, Lewis and Clark Pharmaceuticals, Charlottesville, VA). Mice treated with ATL1223 during EVLP also received ATL1223 treatment (30nM) during the Perfadex flush prior to CSP whereas the EVLP group received vehicle (DMSO) during the flush. CSP lungs, which did not undergo EVLP, underwent immediate functional assessment after re-intubation as described below. -

Snapshot: Pathways of Antiviral Innate Immunity Lijun Sun, Siqi Liu, and Zhijian J
SnapShot: Pathways of Antiviral Innate Immunity Lijun Sun, Siqi Liu, and Zhijian J. Chen Department of Molecular Biology, HHMI, UT Southwestern Medical Center, Dallas, TX 75390-9148, USA 436 Cell 140, February 5, 2010 ©2010 Elsevier Inc. DOI 10.1016/j.cell.2010.01.041 See online version for legend and references. SnapShot: Pathways of Antiviral Innate Immunity Lijun Sun, Siqi Liu, and Zhijian J. Chen Department of Molecular Biology, HHMI, UT Southwestern Medical Center, Dallas, TX 75390-9148, USA Viral diseases remain a challenging global health issue. Innate immunity is the first line of defense against viral infection. A hallmark of antiviral innate immune responses is the production of type 1 interferons and inflammatory cytokines. These molecules not only rapidly contain viral infection by inhibiting viral replication and assembly but also play a crucial role in activating the adaptive immune system to eradicate the virus. Recent research has unveiled multiple signaling pathways that detect viral infection, with several pathways detecting the presence of viral nucleic acids. This SnapShot focuses on innate signaling pathways triggered by viral nucleic acids that are delivered to the cytosol and endosomes of mammalian host cells. Cytosolic Pathways Many viral infections, especially those of RNA viruses, result in the delivery and replication of viral RNA in the cytosol of infected host cells. These viral RNAs often contain 5′-triphosphate (5′-ppp) and panhandle-like secondary structures composed of double-stranded segments. These features are recognized by members of the RIG-I-like Recep- tor (RLR) family, which includes RIG-I, MDA5, and LGP2 (Fujita, 2009; Yoneyama et al., 2004). -

Inhibition of ERK 1/2 Kinases Prevents Tendon Matrix Breakdown Ulrich Blache1,2,3, Stefania L
www.nature.com/scientificreports OPEN Inhibition of ERK 1/2 kinases prevents tendon matrix breakdown Ulrich Blache1,2,3, Stefania L. Wunderli1,2,3, Amro A. Hussien1,2, Tino Stauber1,2, Gabriel Flückiger1,2, Maja Bollhalder1,2, Barbara Niederöst1,2, Sandro F. Fucentese1 & Jess G. Snedeker1,2* Tendon extracellular matrix (ECM) mechanical unloading results in tissue degradation and breakdown, with niche-dependent cellular stress directing proteolytic degradation of tendon. Here, we show that the extracellular-signal regulated kinase (ERK) pathway is central in tendon degradation of load-deprived tissue explants. We show that ERK 1/2 are highly phosphorylated in mechanically unloaded tendon fascicles in a vascular niche-dependent manner. Pharmacological inhibition of ERK 1/2 abolishes the induction of ECM catabolic gene expression (MMPs) and fully prevents loss of mechanical properties. Moreover, ERK 1/2 inhibition in unloaded tendon fascicles suppresses features of pathological tissue remodeling such as collagen type 3 matrix switch and the induction of the pro-fbrotic cytokine interleukin 11. This work demonstrates ERK signaling as a central checkpoint to trigger tendon matrix degradation and remodeling using load-deprived tissue explants. Tendon is a musculoskeletal tissue that transmits muscle force to bone. To accomplish its biomechanical function, tendon tissues adopt a specialized extracellular matrix (ECM) structure1. Te load-bearing tendon compart- ment consists of highly aligned collagen-rich fascicles that are interspersed with tendon stromal cells. Tendon is a mechanosensitive tissue whereby physiological mechanical loading is vital for maintaining tendon archi- tecture and homeostasis2. Mechanical unloading of the tissue, for instance following tendon rupture or more localized micro trauma, leads to proteolytic breakdown of the tissue with severe deterioration of both structural and mechanical properties3–5. -

Xo PANEL DNA GENE LIST
xO PANEL DNA GENE LIST ~1700 gene comprehensive cancer panel enriched for clinically actionable genes with additional biologically relevant genes (at 400 -500x average coverage on tumor) Genes A-C Genes D-F Genes G-I Genes J-L AATK ATAD2B BTG1 CDH7 CREM DACH1 EPHA1 FES G6PC3 HGF IL18RAP JADE1 LMO1 ABCA1 ATF1 BTG2 CDK1 CRHR1 DACH2 EPHA2 FEV G6PD HIF1A IL1R1 JAK1 LMO2 ABCB1 ATM BTG3 CDK10 CRK DAXX EPHA3 FGF1 GAB1 HIF1AN IL1R2 JAK2 LMO7 ABCB11 ATR BTK CDK11A CRKL DBH EPHA4 FGF10 GAB2 HIST1H1E IL1RAP JAK3 LMTK2 ABCB4 ATRX BTRC CDK11B CRLF2 DCC EPHA5 FGF11 GABPA HIST1H3B IL20RA JARID2 LMTK3 ABCC1 AURKA BUB1 CDK12 CRTC1 DCUN1D1 EPHA6 FGF12 GALNT12 HIST1H4E IL20RB JAZF1 LPHN2 ABCC2 AURKB BUB1B CDK13 CRTC2 DCUN1D2 EPHA7 FGF13 GATA1 HLA-A IL21R JMJD1C LPHN3 ABCG1 AURKC BUB3 CDK14 CRTC3 DDB2 EPHA8 FGF14 GATA2 HLA-B IL22RA1 JMJD4 LPP ABCG2 AXIN1 C11orf30 CDK15 CSF1 DDIT3 EPHB1 FGF16 GATA3 HLF IL22RA2 JMJD6 LRP1B ABI1 AXIN2 CACNA1C CDK16 CSF1R DDR1 EPHB2 FGF17 GATA5 HLTF IL23R JMJD7 LRP5 ABL1 AXL CACNA1S CDK17 CSF2RA DDR2 EPHB3 FGF18 GATA6 HMGA1 IL2RA JMJD8 LRP6 ABL2 B2M CACNB2 CDK18 CSF2RB DDX3X EPHB4 FGF19 GDNF HMGA2 IL2RB JUN LRRK2 ACE BABAM1 CADM2 CDK19 CSF3R DDX5 EPHB6 FGF2 GFI1 HMGCR IL2RG JUNB LSM1 ACSL6 BACH1 CALR CDK2 CSK DDX6 EPOR FGF20 GFI1B HNF1A IL3 JUND LTK ACTA2 BACH2 CAMTA1 CDK20 CSNK1D DEK ERBB2 FGF21 GFRA4 HNF1B IL3RA JUP LYL1 ACTC1 BAG4 CAPRIN2 CDK3 CSNK1E DHFR ERBB3 FGF22 GGCX HNRNPA3 IL4R KAT2A LYN ACVR1 BAI3 CARD10 CDK4 CTCF DHH ERBB4 FGF23 GHR HOXA10 IL5RA KAT2B LZTR1 ACVR1B BAP1 CARD11 CDK5 CTCFL DIAPH1 ERCC1 FGF3 GID4 HOXA11 -

Targeting IRAK1 in T-Cell Acute Lymphoblastic Leukemia
Targeting IRAK1 in T-Cell acute lymphoblastic leukemia Charles Dussiau, Amélie Trinquand, Ludovic Lhermitte, Mehdi Latiri, Mathieu Simonin, Agata Cieslak, Nawel Bedjaoui, Patrick Villarèse, Els Verhoeyen, Hervé Dombret, et al. To cite this version: Charles Dussiau, Amélie Trinquand, Ludovic Lhermitte, Mehdi Latiri, Mathieu Simonin, et al.. Tar- geting IRAK1 in T-Cell acute lymphoblastic leukemia. Oncotarget, Impact journals, 2015, 6 (22), pp.18956-65. inserm-01820237 HAL Id: inserm-01820237 https://www.hal.inserm.fr/inserm-01820237 Submitted on 21 Jun 2018 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. www.impactjournals.com/oncotarget/ Oncotarget, Vol. 6, No. 22 Targeting IRAK1 in T-Cell acute lymphoblastic leukemia Charles Dussiau1,*, Amélie Trinquand1,*, Ludovic Lhermitte1, Mehdi Latiri1, Mathieu Simonin1, Agata Cieslak1, Nawel Bedjaoui1, Patrick Villarèse1, Els Verhoeyen2,3, Hervé Dombret4, Norbert Ifrah5, Elizabeth Macintyre1, Vahid Asnafi1 1 Université Paris Descartes Sorbonne Cité, Institut Necker-Enfants Malades (INEM), Institut National -

Lipopolysaccharide Signaling in Endothelial Cells
Laboratory Investigation (2006) 86, 9–22 & 2006 USCAP, Inc All rights reserved 0023-6837/06 $30.00 www.laboratoryinvestigation.org Lipopolysaccharide signaling in endothelial cells Shauna M Dauphinee1,2 and Aly Karsan1,2,3,4 1Department of Medical Biophysics, British Columbia Cancer Agency, Vancouver, British Columbia, Canada; 2Experimental Medicine Program, University of British Columbia, Vancouver, British Columbia, Canada; 3Department of Pathology and Laboratory Medicine, British Columbia Cancer Agency, Vancouver, British Columbia, Canada and 4Department of Pathology and Laboratory Medicine, University of British Columbia, Vancouver, British Columbia, Canada Sepsis is the systemic immune response to severe bacterial infection. The innate immune recognition of bacterial and viral products is mediated by a family of transmembrane receptors known as Toll-like receptors (TLRs). In endothelial cells, exposure to lipopolysaccharide (LPS), a major cell wall constituent of Gram- negative bacteria, results in endothelial activation through a receptor complex consisting of TLR4, CD14 and MD2. Recruitment of the adaptor protein myeloid differentiation factor (MyD88) initiates an MyD88-dependent pathway that culminates in the early activation of nuclear factor-jB (NF-jB) and the mitogen-activated protein kinases. In parallel, a MyD88-independent pathway results in a late-phase activation of NF-jB. The outcome is the production of various proinflammatory mediators and ultimately cellular injury, leading to the various vascular sequelae of sepsis.