The Abnormal Presentation of Complicated Appendicitis Goubeaux C* and Adams J Removed
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Acute Abdomen
Acute abdomen: Shaking down the Acute abdominal pain can be difficult to diagnose, requiring astute assessment skills and knowledge of abdominal anatomy 2.3 ANCC to discover its cause. We show you how to quickly and accurately CONTACT HOURS uncover the clues so your patient can get the help he needs. By Amy Wisniewski, BSN, RN, CCM Lehigh Valley Home Care • Allentown, Pa. The author has disclosed that she has no significant relationships with or financial interest in any commercial companies that pertain to this educational activity. NIE0110_124_CEAbdomen.qxd:Deepak 26/11/09 9:38 AM Page 43 suspects Determining the cause of acute abdominal rapidly, indicating a life-threatening process, pain is often complex due to the many or- so fast and accurate assessment is essential. gans in the abdomen and the fact that pain In this article, I’ll describe how to assess a may be nonspecific. Acute abdomen is a patient with acute abdominal pain and inter- general diagnosis, typically referring to se- vene appropriately. vere abdominal pain that occurs suddenly over a short period (usually no longer than What a pain! 7 days) and often requires surgical interven- Acute abdominal pain is one of the top tion. Symptoms may be severe and progress three symptoms of patients presenting in www.NursingMadeIncrediblyEasy.com January/February 2010 Nursing made Incredibly Easy! 43 NIE0110_124_CEAbdomen.qxd:Deepak 26/11/09 9:38 AM Page 44 the ED. Reasons for acute abdominal pain Visceral pain can be divided into three Your patient’s fall into six broad categories: subtypes: age may give • inflammatory—may be a bacterial cause, • tension pain. -

Missed Appendicitis Diagnosis: a Case Report Jocelyn Cox, Bphed, DC1 Guy Sovak, Phd2
ISSN 0008-3194 (p)/ISSN 1715-6181 (e)/2015/294–299/$2.00/©JCCA 2015 Missed appendicitis diagnosis: A case report Jocelyn Cox, BPhEd, DC1 Guy Sovak, PhD2 Objective: The purpose of this case report is to highlight Objectif : Cette étude de cas vise à souligner la nécessité and emphasize the need for an appropriate and thorough d’une liste appropriée et détaillée de diagnostics list of differential diagnoses when managing patients, as différentiels lors de la gestion des patients, car il n’est it is insufficient to assume cases are mechanical, until pas suffisant de supposer que les cas sont d’ordre proven non-mechanical. There are over 250,000 cases mécanique, jusqu’à la preuve du contraire. Il y a plus de of appendicitis annually in the United States. Of these 250 000 cas d’appendicite par an aux États-Unis. Parmi cases, <50% present with classic signs and symptoms of ces cas, < 50 % présentent des signes et des symptômes pain in the right lower quadrant, mild fever and nausea. classiques de douleur dans le quadrant inférieur droit, It is standard for patients who present with appendicitis de fièvre légère et de nausées. Il est normal qu’un to be managed operatively with a laparoscopic patient qui se présente avec une appendicite soit géré appendectomy within 24 hours, otherwise the risk of par une intervention chirurgicale (appendicectomie complications such as rupture, infection, and even death par laparoscopie) dans les 24 heures, sinon le risque increases dramatically. de complications, telles que rupture, infection et décès, Clinical Features: This is a retrospective case report augmente considérablement. -

Imaging of Acute Appendicitis in Adults and Children
Diagnostic Imaging Imaging of Acute Appendicitis in Adults and Children Bearbeitet von Caroline KEYZER, Pierre Alain Gevenois 1. Auflage 2011. Buch. IX, 256 S. Hardcover ISBN 978 3 642 17871 9 Format (B x L): 19,3 x 26 cm Gewicht: 688 g Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete > Radiologie, Bildgebende Verfahren Zu Inhaltsverzeichnis schnell und portofrei erhältlich bei Die Online-Fachbuchhandlung beck-shop.de ist spezialisiert auf Fachbücher, insbesondere Recht, Steuern und Wirtschaft. Im Sortiment finden Sie alle Medien (Bücher, Zeitschriften, CDs, eBooks, etc.) aller Verlage. Ergänzt wird das Programm durch Services wie Neuerscheinungsdienst oder Zusammenstellungen von Büchern zu Sonderpreisen. Der Shop führt mehr als 8 Millionen Produkte. Clinical Presentation of Acute Appendicitis: Clinical Signs—Laboratory Findings—Clinical Scores, Alvarado Score and Derivate Scores David J. Humes and John Simpson Contents Abstract Appendicectomy is the most commonly performed 1 Clinical Presentation ............................................... 14 emergency operation worldwide with a lifetime risk 1.1 History........................................................................ 14 of appendicitis of 8.6% in males and 6.7% in 15 1.2 Examination ............................................................... females (Flum and Koepsell 2002; Addiss et al. 2 Laboratory Investigations....................................... 16 1990). The diagnosis of acute appendicitis is 3 Scoring Systems ...................................................... -

Positive Psoas Sign in a Disabled Child-Not Always Appendicitis, Seldomly Due to Duodenal Perforation by Sharp Foreign Body
Case Report Published: 01 Aug, 2019 SF Journal of Radiology and Clinical Diagnosis Positive Psoas Sign in a Disabled Child-Not Always Appendicitis, Seldomly due to Duodenal Perforation by Sharp Foreign Body Klein E1*, Merhav G1, Kassis I2 and Ilivitzki A1 1Department of Radiology, Rambam Health Care Campus, Haaliya Hashniya 8 st, Haifa, Israel 2Pediatric Infectious Disease Unit, Rambam Health Care Campus, Haaliya Hashniya 8 st, Haifa, Israel Abstract We present a rare cause for "positive psoas sign" secondary to duodenal perforation by an ingested wooden skewer in a disabled 13 years old male. The unreliable clinical evaluation made the appreciation of a "positive psoas sign" obscured. We highlight the possible occurrence of this pathology in young or disabled children, and the importance of CT leading to this diagnosis, with the utilization of multiplane MIP reconstructions. This case also points that the psoas muscle is a long structure in the retroperitoneum, and irritation of its upper most part may also present as positive psoas sign. Keywords: Psoas sign; Psoasabscess; Skewer; Perforation; Missed diagnosis Case Report A 13 years old male is seen in the pediatric emergency room (ER) due to new onset of limp on the right lower limb, nausea and agitation. His past medical history consists of prematurity with severe psychomotor delay including mental retardation as a sequalae. Past surgical history consists of fundoplication procedure due to diaphragmatic hernia and feeding jejunostomy which was thereafter closed. Medical history was negative for any recent illness with fever, nothing to support food poisoning OPEN ACCESS or any trauma. Physical examination revealed a positive psoas sign, with no tenderness upon deep palpation of the abdomen, and additional point tenderness upon palpation of the distal femur. -

Abdominal Pain
10 Abdominal Pain Adrian Miranda Acute abdominal pain is usually a self-limiting, benign condition that irritation, and lateralizes to one of four quadrants. Because of the is commonly caused by gastroenteritis, constipation, or a viral illness. relative localization of the noxious stimulation to the underlying The challenge is to identify children who require immediate evaluation peritoneum and the more anatomically specific and unilateral inner- for potentially life-threatening conditions. Chronic abdominal pain is vation (peripheral-nonautonomic nerves) of the peritoneum, it is also a common complaint in pediatric practices, as it comprises 2-4% usually easier to identify the precise anatomic location that is produc- of pediatric visits. At least 20% of children seek attention for chronic ing parietal pain (Fig. 10.2). abdominal pain by the age of 15 years. Up to 28% of children complain of abdominal pain at least once per week and only 2% seek medical ACUTE ABDOMINAL PAIN attention. The primary care physician, pediatrician, emergency physi- cian, and surgeon must be able to distinguish serious and potentially The clinician evaluating the child with abdominal pain of acute onset life-threatening diseases from more benign problems (Table 10.1). must decide quickly whether the child has a “surgical abdomen” (a Abdominal pain may be a single acute event (Tables 10.2 and 10.3), a serious medical problem necessitating treatment and admission to the recurring acute problem (as in abdominal migraine), or a chronic hospital) or a process that can be managed on an outpatient basis. problem (Table 10.4). The differential diagnosis is lengthy, differs from Even though surgical diagnoses are fewer than 10% of all causes of that in adults, and varies by age group. -

Belly Pain and Vomiting: NO YES Perforation When to Worry? Hemmorrhage Hematoma Judith J
ABDOMINAL PAIN TRAUMA?? Belly Pain and Vomiting: NO YES Perforation When to Worry? Hemmorrhage Hematoma Judith J. Stellar, MSN, CRNP AGE?? Contusion Surgery Clinical Nurse Specialist ACUTE CHRONIC The Children’s Hospital of Philadelphia Peritonitis GER, Milk Allergy, Obstruction SCC, IBD Rectal Bleeding Constipation Functional Disorders INFANTS: Birth to 1 Year NEWBORNS TWO TO FIVE YEARS – Anomalies of the GI tract Gastroenteritis – NEC Constipation – Perforation Appendicitis – Volvulus UTI INFANTS up to 1 year Intussusception – Colic, Constipation Volvulus – Gastroenteristis Trauma – UTI Sickle Cell – Incarcerated Hernia HSP – Intussusception Pharyngitis – Volvulus – Hirschsprung’s Disease SCHOOL AGE: 6 to 11 Years ADOLESCENTS: 12 to 18 yrs. Appendicitis Appendicitis Gastroenteritis Ovarian / Testicular Constipation Torsion Functional pain IBD UTI Gastroenteritis Trauma Constipation Sickle Cell Dysmenorrhea HSP Mittelscherz Mesenteric Adenitis PID 1 Is All Belly Pain The Same? STEPWISE APPROACH Visceral Pain HISTORY – Irritation to viscus tension, stretching, ischemia – Visceral pain fibers: bilateral, unmyelinated, enter – Medical, Surgical, Family spinal cord at various levels REVIEW OF SYSTEMS – Pain: dull, poorly localized and midline Parietal Pain – Sequence of events, Extra-intestinal – From the body wall, peritoneum symptoms, Growth failure, Weight loss, – Myelinated fibers to specific dorsal root ganglia Recent illness – Pain: sharp, intense, localized THOROUGH PHYSICAL EXAM – Aggravated -

Abdominal Pain
Abdominal Pain With Dr Sanjay Warrier, Consultant Breast Surgeon at Royal Prince Alfred Hospital Case 1 – You are in the emergency department where a 50 year old man has just presented with abdominal pain 1. Initial approach: Analgesia aids assessment o Ensure there are appropriate lines inserted and analgesia is charted to manage pain Subjective assessment o General examination of the patient – how well/unwell are they? Objective assessment o Review the patient’s vital signs (if abnormal, go through ABC assessment and escalate as appropriate) 2. History: Assess the pain (Site, Onset, Character, Radiation, Associated symptoms, Timing, Exacerbating and Relieving factors, Severity) Associated symptoms should include dysuria, diarrhoea, nausea, vomiting Past medical history Past surgical history Embryology o Foregut . Gives rise to oesophagus, stomach, proximal duodenum, liver, gallbladder, pancreas, spleen . Supplied by coeliac trunk . Pain typically referred to epigastrium o Midgut . Gives rise to distal duodenum, jejunum, ileum, caecum, appendix, ascending colon, proximal 2/3 of transverse colon . Supplied by branches of superior mesenteric artery . Pain typically referred to the umbilical region o Hindgut . Gives rise to distal 1/3 of transverse colon, descending colon, rectum and upper anal canal . Supplied by branches of inferior mesenteric artery . Pain typically referred to suprapubic region o Visceral midgut pain typically commences as vague pain felt in the umbilical region. As it involves the parietal peritoneal it will become sharper in nature and be localised over the affected organ Summarised by Dr Abhijit Pal, Resident, RPAH. December 2014 3. Examination: Appropriate exposure and position (exposed abdomen, patient supine, arms by side) Inspection (previous surgical scars, abdominal breathing, guarding) Palpation (move systematically through all 9 quadrants superficially and then deeply) 4. -

Abdominal Pain
DESCHUTES COUNTY ADULT JAIL SO-501 L. Shane Nelson, Sheriff Standing Order Facility Provider: December 6, 2017 STANDING ORDER ABDOMINAL PAIN 1. Assessment a. History i. Location, duration, pattern of pain (constant or intermittent) ii. When did it start and anything precipitating/leading up to the start of the pain? iii. Anything tried to make the pain better? Did it work? Anything that makes the pain worse (does passing stool/flatus improve the pain?) iv. History of abdominal surgeries? v. LMP for female inmates, chance she is pregnant? vi. Last BM vii. Associated symptoms: nausea, vomiting, diarrhea, constipation, loss of appetite, fever, vaginal bleeding, vaginal discharge, penile discharge, testicular pain, hematuria, dysuria, black tarry stools, bloody stools, coffee-ground emesis. b. Exam (exam is best done without asking the inmate if he/she has pain in various areas, if there is pain it will be evident upon exam. This is an objective exam, so n) i. Ask inmate to move to exam table, observe movements from chair to a laying down position – someone in pain will have difficulty doing this and it will be evident, especially with using abdominal muscles to get to a laying down position. Also, observe inmate when gets up from the exam table. Any visible signs of pain with these movements and ambulation? ii. Auscultate bowel sounds prior to any palpation iii. Observe abdomen, is it distended, flat, obese? iv. Palpate all areas of the abdomen separately with knees bent – epigastric, LUQ, RUQ, LLQ, RLQ, umbilical, suprapubic – where is pain the worst? Is it generalized in all quadrants? v. -

Chapter 5 – Gastrointestinal System
CHAPTER 5 – GASTROINTESTINAL SYSTEM First Nations and Inuit Health Branch (FNIHB) Clinical Practice Guidelines for Nurses in Primary Care. The content of this chapter was revised October 2011. Table of Contents ASSESSMENT OF THE GASTROINTESTINAL SYSTEM ......................................5–1 EXAMINATION OF THE ABDOMEN ........................................................................5–2 COMMON PROBLEMS OF THE GASTROINTESTINAL SYSTEM .........................5–4 Anal Fissure .......................................................................................................5–4 Constipation .......................................................................................................5–5 Dehydration (Hypovolemia) ...............................................................................5–8 Diarrhea ...........................................................................................................5–11 Diverticular Disease .........................................................................................5–15 Diverticulitis ......................................................................................................5–15 Diverticulosis ....................................................................................................5–16 Dyspepsia ........................................................................................................5–17 Gallbladder Disease .........................................................................................5–18 Biliary Colic ......................................................................................................5–21 -
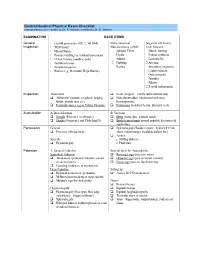
Gastrointestinal Physical Exam Checklist Learnpediatrics.Com – Written by Dr
Gastrointestinal Physical Exam Checklist Learnpediatrics.com – written by Dr. R. Acedillo, modified by Dr. E. Statham EXAMINATION OSCE ITEMS General Growth parameters (HC, L, Wt, BMI) Extra-intestinal Stigmata of Chronic Inspection Well/Unwell Manifestations of IBD: Liver Disease: Mental Status Aphtous Ulcers Muscle wasting Posture (writhing vs. minimal movement) Uveitis Palmar erythema Colour (icterus, jaundice, pale) Arthritis Leukonychia Nutritional status Clubbing Asterixis Peripheral edema Rashes Strawberry angiomas Rashes (eg. Dermatitis Herpetiformis) Caput medusae Gynecomastia Jaundice Edema Parotid enlargement Inspection Abdominal Scars (surgical – risk for Bowel obstruction) Abdominal contours (scaphoid, bulging Skin abnormalities (abdominal wall veins, flanks, protuberant, etc) hemangiomas) Peristaltic waves (eg in. Pyloric Stenosis) Protrusions (umbilical hernia, diastasis recti) Auscultation A. Bowel Sounds B. Vascular Sounds (Presence vs absence) Bruits (aorta, iliac, femoral, renal) Quality (Frequency and Pitch [high?]) Bruits/venous hums around palpable liver mass (if applicable) Percussion General: Splenomegaly (Traube’s space - below left 6th rib, Presence of tenderness above costal margin, medial to axillary line) Ascites Specific: o Shifting dullness Hepatomegaly o Fluid wave Palpation A. General Palpation Special tests for Appendicitis Superficial Palpation Rovsing’s sign (pressure wave) Tenderness (peritoneal irritation, somatic Obturator sign (pain on hip int. rotation) or -

Acute Surgical
Acute Surgical When a patient presents to the ED with acute abdominal The Basics pain, the emergency physician’s role in taking a history, performing an exam, selecting the appropriate imaging modality, and calling for surgical consultation, if needed, cannot be underestimated. The authors review the most common etiologies of acute surgical abdomen and the emergency physician’s pivotal responsibility in ensuring the best outcomes. Brian H. Campbell, MD, and Moss H. Mendelson, MD bdominal pain is a common complaint depending on the capabilities of the home institu- seen in emergency departments nation- tion. This article reviews key points in the evaluation wide. According to the CDC, stomach of adult patients with abdominal pain, discusses dis- and abdominal pain are the leading rea- ease processes that require emergent surgical evalu- Asons for visits to the ED, accounting for 6.8% of ation and treatment, and highlights the importance all visits in 2006.1 An adult patient with an acute of facilitating early surgical intervention. Although abdomen generally appears ill and has abnormal there are many causes of abdominal pain, this article findings on physical exam. Many of these patients will focus on etiologies that often lead to an acute need immediate surgery, as several of the underlying surgical abdomen, ie, those cases in which a patient disease processes that result in an acute abdomen needs emergent evaluation and treatment and likely are associated with high morbidity and/or mortal- requires emergent operative treatment. ity. The emergency physician must rapidly identify those patients who require early surgical interven- HISTORY tion and appropriately resuscitate them, order the Every clinician learns that history is the key to di- necessary tests, consult the surgical team early on, agnosing most illness, and this is especially true for and notify surgical staff or arrange for a transfer, patients with abdominal pain.