Esophagus & Thymus
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vagus Nerve (CN X) That Supply All of the Thoracic and Abdominal Viscera, Except the Descending and Sigmoid Colons and Other Pelvic Viscera
DR. HAYTHEM ALI ALSAYIGH Assistant prof. BOARD CLINICAL SURGICAL ANATOMY F.I.M.B.S.-MB.CH,B COLLEGE OF MEDICINE –UNIVERSITY OF BABYLON III. Autonomic Nervous System in the Thorax Is composed of motor, or efferent, nerves through which cardiac muscle, smooth muscle , and glands are innervated. Involves two neurons: preganglionic and postganglionic. It may include general visceral afferent (GVA) fibers because they run along with general visceral efferent (GVE) fibers . Consists of sympathetic (or thoracolumbar outflow) and parasympathetic (or craniosacral outflow)systems. Consists of cholinergic fibers (sympathetic preganglionic, parasympathetic preganglionic, and postganglionic) that use acetylcholine as the neurotransmitter and adrenergic fibers (sympathetic postganglionic) that use norepinephrine as the neurotransmitter (except those to sweat glands [cholinergic]). A. Sympathetic nervous system Enables the body to cope with crises or emergencies and thus often is referred to as the fight-or-flight division. Contains preganglionic cell bodies that are located in the lateral horn or intermediolateral cell column of the spinal cord segments between T1 and L2. Has preganglionic fibers that pass through the white rami communicantes and enter the sympathetic chain ganglion, where they synapse. Has postganglionic fibers that join each spinal nerve by way of the gray rami communicantes and supply the blood vessels, hair follicles (arrector pili muscles), and sweat glands. Increases the heart rate , dilates the bronchial lumen , and dilates the coronary arteries. 1. Sympathetic trunk Is composed primarily of ascending and descending preganglionic sympathetic fibers and visceral afferent fibers, and contains the cell bodies of the postganglionic sympathetic (GVE) fibers. Descends in front of the neck of the ribs and the posterior intercostal vessels. -

Adaptive Immune Systems
Immunology 101 (for the Non-Immunologist) Abhinav Deol, MD Assistant Professor of Oncology Wayne State University/ Karmanos Cancer Institute, Detroit MI Presentation originally prepared and presented by Stephen Shiao MD, PhD Department of Radiation Oncology Cedars-Sinai Medical Center Disclosures Bristol-Myers Squibb – Contracted Research What is the immune system? A network of proteins, cells, tissues and organs all coordinated for one purpose: to defend one organism from another It is an infinitely adaptable system to combat the complex and endless variety of pathogens it must address Outline Structure of the immune system Anatomy of an immune response Role of the immune system in disease: infection, cancer and autoimmunity Organs of the Immune System Major organs of the immune system 1. Bone marrow – production of immune cells 2. Thymus – education of immune cells 3. Lymph Nodes – where an immune response is produced 4. Spleen – dual role for immune responses (especially antibody production) and cell recycling Origins of the Immune System B-Cell B-Cell Self-Renewing Common Progenitor Natural Killer Lymphoid Cell Progenitor Thymic T-Cell Selection Hematopoetic T-Cell Stem Cell Progenitor Dendritic Cell Myeloid Progenitor Granulocyte/M Macrophage onocyte Progenitor The Immune Response: The Art of War “Know your enemy and know yourself and you can fight a hundred battles without disaster.” -Sun Tzu, The Art of War Immunity: Two Systems and Their Key Players Adaptive Immunity Innate Immunity Dendritic cells (DC) B cells Phagocytes (Macrophages, Neutrophils) Natural Killer (NK) Cells T cells Dendritic Cells: “Commanders-in-Chief” • Function: Serve as the gateway between the innate and adaptive immune systems. -

Cells, Tissues and Organs of the Immune System
Immune Cells and Organs Bonnie Hylander, Ph.D. Aug 29, 2014 Dept of Immunology [email protected] Immune system Purpose/function? • First line of defense= epithelial integrity= skin, mucosal surfaces • Defense against pathogens – Inside cells= kill the infected cell (Viruses) – Systemic= kill- Bacteria, Fungi, Parasites • Two phases of response – Handle the acute infection, keep it from spreading – Prevent future infections We didn’t know…. • What triggers innate immunity- • What mediates communication between innate and adaptive immunity- Bruce A. Beutler Jules A. Hoffmann Ralph M. Steinman Jules A. Hoffmann Bruce A. Beutler Ralph M. Steinman 1996 (fruit flies) 1998 (mice) 1973 Discovered receptor proteins that can Discovered dendritic recognize bacteria and other microorganisms cells “the conductors of as they enter the body, and activate the first the immune system”. line of defense in the immune system, known DC’s activate T-cells as innate immunity. The Immune System “Although the lymphoid system consists of various separate tissues and organs, it functions as a single entity. This is mainly because its principal cellular constituents, lymphocytes, are intrinsically mobile and continuously recirculate in large number between the blood and the lymph by way of the secondary lymphoid tissues… where antigens and antigen-presenting cells are selectively localized.” -Masayuki, Nat Rev Immuno. May 2004 Not all who wander are lost….. Tolkien Lord of the Rings …..some are searching Overview of the Immune System Immune System • Cells – Innate response- several cell types – Adaptive (specific) response- lymphocytes • Organs – Primary where lymphocytes develop/mature – Secondary where mature lymphocytes and antigen presenting cells interact to initiate a specific immune response • Circulatory system- blood • Lymphatic system- lymph Cells= Leukocytes= white blood cells Plasma- with anticoagulant Granulocytes Serum- after coagulation 1. -
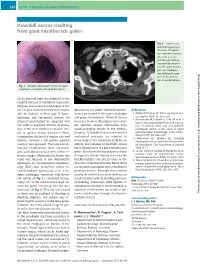
Downhill Varices Resulting from Giant Intrathoracic Goiter
E40 UCTN – Unusual cases and technical notes Downhill varices resulting from giant intrathoracic goiter Fig. 2 Sagittal com- puted tomography of the chest. The goiter was immense, reaching the aortic arch, sur- rounding the trachea and partially compres- sing the upper esopha- gus. The esophagus was additionally com- pressed by anterior spinal spondylophytes. Fig. 1 Multiple submucosal veins in the upper esophagus, consistent with downhill varices. An 82-year-old man was admitted to the hospital because of substernal chest pain, dyspnea, and occasional dysphagia to sol- ids. His past medical history was remark- geal varices are called “downhill varices”, References able for diabetes mellitus type II, hyper- as they are located in the upper esophagus 1 Kotfila R, Trudeau W. Extraesophageal vari- – lipidemia, and Parkinson’s disease. On and project downwards. Downhill varices ces. Dig Dis 1998; 16: 232 241 2 Basaranoglu M, Ozdemir S, Celik AF et al. A occur as a result of shunting in cases of up- physical examination he appeared frail case of fibrosing mediastinitis with obstruc- but with no apparent distress. Examina- per systemic venous obstruction from tion of superior vena cava and downhill tion of the neck showed no masses, stri- space-occupying lesions in the medias- esophageal varices: a rare cause of upper dor or jugular venous distension. Heart tinum [2,3]. Downhill varices as a result of gastrointestinal hemorrhage. J Clin Gastro- – examination disclosed a regular rate and mediastinal processes are reported to enterol 1999; 28: 268 270 3 Calderwood AH, Mishkin DS. Downhill rhythm; however a 2/6 systolic ejection occur in up to 50% of patients [3,4]. -

Selective Venous Sampling for Primary Hyperparathyroidism: How to Perform an Examination and Interpret the Results with Reference to Thyroid Vein Anatomy
Jpn J Radiol DOI 10.1007/s11604-017-0658-3 INVITED REVIEW Selective venous sampling for primary hyperparathyroidism: how to perform an examination and interpret the results with reference to thyroid vein anatomy Takayuki Yamada1 · Masaya Ikuno1 · Yasumoto Shinjo1 · Atsushi Hiroishi1 · Shoichiro Matsushita1 · Tsuyoshi Morimoto1 · Reiko Kumano1 · Kunihiro Yagihashi1 · Takuyuki Katabami2 Received: 11 April 2017 / Accepted: 28 May 2017 © Japan Radiological Society 2017 Abstract Primary hyperparathyroidism (pHPT) causes and brachiocephalic veins for catheterization of the thyroid hypercalcemia. The treatment for pHPT is surgical dis- veins and venous anastomoses. section of the hyperfunctioning parathyroid gland. Lower rates of hypocalcemia and recurrent laryngeal nerve injury Keywords Primary hyperparathyroidism · Localization · imply that minimally invasive parathyroidectomy (MIP) is Thyroid vein · Venous sampling safer than bilateral neck resection. Current trends in MIP use can be inferred only by reference to preoperative locali- zation studies. Noninvasive imaging studies (typically pre- Introduction operative localization studies) show good detection rates of hyperfunctioning glands; however, there have also been Primary hyperparathyroidism (pHPT) is a common endocrine cases of nonlocalization or discordant results. Selective disease. Most patients have one adenoma, but double adeno- venous sampling (SVS) is an invasive localization method mas have been reported in up to 15% of cases [1]. Approxi- for detecting elevated intact parathyroid -

Under the Human Keratin 14 Promoter Expressed Autoimmune Disease to an Antigen a Spontaneous CD8 T Cell-Dependent
A Spontaneous CD8 T Cell-Dependent Autoimmune Disease to an Antigen Expressed Under the Human Keratin 14 Promoter This information is current as Maureen A. McGargill, Dita Mayerova, Heather E. Stefanski, of September 26, 2021. Brent Koehn, Evan A. Parke, Stephen C. Jameson, Angela Panoskaltsis-Mortari and Kristin A. Hogquist J Immunol 2002; 169:2141-2147; ; doi: 10.4049/jimmunol.169.4.2141 http://www.jimmunol.org/content/169/4/2141 Downloaded from References This article cites 44 articles, 23 of which you can access for free at: http://www.jimmunol.org/content/169/4/2141.full#ref-list-1 http://www.jimmunol.org/ Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication by guest on September 26, 2021 *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2002 by The American Association of Immunologists All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology A Spontaneous CD8 T Cell-Dependent Autoimmune Disease to an Antigen Expressed Under the Human Keratin 14 Promoter1 Maureen A. McGargill,*‡ Dita Mayerova,*‡ Heather E. -

Anatomy of the Anterior Vagus Nerve: an Anatomic Description and Its Application in Surgery Leopoldo M
ogy: iol Cu ys r h re P n t & R y e s Anatomy & Physiology: Current m e Baccaro et al., Anat Physiol 2013, 3:2 o a t r a c n h DOI: 10.4172/2161-0940.1000121 A Research ISSN: 2161-0940 Research Article Open Access Anatomy of the Anterior Vagus Nerve: An Anatomic Description and its Application in Surgery Leopoldo M. Baccaro*, Cristian N. Lucas, Marcos R. Zandomeni, María V. Selvino and Eduardo F. Albanese Universidad del Salvador, School of Medicine, Tucumán 1845/49, Buenos Aires, Argentina Abstract Objective: Anatomic study of human corpses in order to obtain specific measurements of the anterior vagus nerve for its application in the surgical field. Methods: After analyzing the literature, dissections were performed on 15 human corpses, provided by the Universidad del Salvador. Descriptions were made of our observations. Results: The most frequently found structure in esophageal hiatus was a plexus. The cardial branch was present in 100% of the dissections. There were a constant number of gastric branches, between five and seven. The hepatic branch originated from the plexus in the majority of the cadavers. The distance between first and last branch points was variable. No relationship between the hepatic branch and left hepatic artery was observed. Conclusions: The structure most commonly found in the esophageal hiatus was the terminal plexus of the anterior vagus nerve. The hepatic branch most frequently originated directly from this plexus, although in a considerable number of cases its origin was found either proximal or distal to this structure. We could not confirm the literature stating the relationship between the hepatic branch and the left hepatic artery through our studies. -

Anatomy & Embryology of Thyroid & Parathyroid
ANATOMY & EMBRYOLOGY OF THYROID & PARATHYROID By Prof . Saeed Abuel Makarem & Associate Prof. Sanaa Alshaarawy 1 OBJECTIVES Ò By the end of the lecture, the student should be able to: Ò Describe the shape, position, relations and structure of the thyroid gland. Ò List the blood supply & lymphatic drainage of the thyroid gland. Ò List the nerves endanger with thyroidectomy operation. Ò Describe the shape, position, blood supply & lymphatic drainage of the parathyroid glands. Ò Describe the development of the thyroid & parathyroid glands. Ò Describe the most common congenital anomalies of the thyroid gland. 2 Before we go to the thyroid What are the parts of the deep fascia or deep cervical fascia of the neck? It is divided mainly into 3 layers: 1- Investing layer. 2- Pretracheal layer. 3- Prevertebral layer. 3 Ò Endocrine, butterfly Thyroid gland shaped gland. Ò Consists of right & left lobes. Ò The 2 lobes are connected to each other by a narrow isthmus, which overlies the 2nd ,3rd & 4th tracheal rings. Ò It is surrounded by a facial sheath derived from the pretracheal layer of the deep cervical fascia. 4 Thyroid gland Ò Each lobe is pear- shaped, with its apex reaches up to the oblique line of thyroid cartilage. Ò Its base lies at the level of 4th or 5th tracheal rings. Ò Inside the pretracheal facial capsule, there is another C.T capsule. Ò So, it s surrounded by 2 membranes. 5 Each lobe is pear shape, with its apex directed upward as far as the Anterior oblique line of the thyroid cartilage; its base lies at the 4th or 5th tracheal ring. -

An Unusual Origin and Course of the Thyroidea Ima Artery, with Absence of Inferior Thyroid Artery Bilaterally
Surgical and Radiologic Anatomy (2019) 41:235–237 https://doi.org/10.1007/s00276-018-2122-1 ANATOMIC VARIATIONS An unusual origin and course of the thyroidea ima artery, with absence of inferior thyroid artery bilaterally Doris George Yohannan1 · Rajeev Rajan1 · Akhil Bhuvanendran Chandran1 · Renuka Krishnapillai1 Received: 31 May 2018 / Accepted: 21 October 2018 / Published online: 25 October 2018 © Springer-Verlag France SAS, part of Springer Nature 2018 Abstract We report an unusual origin and course of the thyroidea ima artery in a male cadaver. The ima artery originated from the right subclavian artery very close to origin of the right vertebral artery. The artery coursed anteriorly between the common carotid artery medially and internal jugular vein laterally. It then coursed obliquely, from below upwards, from lateral to medial superficial to common carotid artery, to reach the inferior pole of the right lobe of thyroid and branched repeatedly to supply the anteroinferior and posteroinferior aspects of both the thyroid lobes and isthmus. The superior thyroid arteries were normal. Both the inferior thyroid arteries were absent. The unusual feature of this thyroidea ima artery is its origin from the subclavian artery close to vertebral artery origin, the location being remarkably far-off from the usual near midline position, and the oblique and relatively superficial course. This report is a caveat to neck surgeons to consider such a superficially running vessel to be a thyroidea ima artery. Keywords Thyroid vascular anatomy · Thyroidea ima artery · Artery of Neubauer · Blood supply of thyroid · Variations Introduction (1.1%), transverse scapular (1.1%), or pericardiophrenic or thyrocervical trunk [8, 10]. -

Thymus Growth an Epithelial Progenitor Pool Regulates
An Epithelial Progenitor Pool Regulates Thymus Growth William E. Jenkinson, Andrea Bacon, Andrea J. White, Graham Anderson and Eric J. Jenkinson This information is current as of October 1, 2021. J Immunol 2008; 181:6101-6108; ; doi: 10.4049/jimmunol.181.9.6101 http://www.jimmunol.org/content/181/9/6101 Downloaded from References This article cites 35 articles, 16 of which you can access for free at: http://www.jimmunol.org/content/181/9/6101.full#ref-list-1 Why The JI? Submit online. http://www.jimmunol.org/ • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average by guest on October 1, 2021 Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2008 by The American Association of Immunologists All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology An Epithelial Progenitor Pool Regulates Thymus Growth1 William E. Jenkinson, Andrea Bacon, Andrea J. White, Graham Anderson, and Eric J. Jenkinson2 Thymic epithelium provides an essential cellular substrate for T cell development and selection. Gradual age-associated thymic atrophy leads to a reduction in functional thymic tissue and a decline in de novo T cell generation. -

Anatomy of Esophagus Anatomy of Esophagus
DOI: 10.5772/intechopen.69583 Provisional chapter Chapter 1 Anatomy of Esophagus Anatomy of Esophagus Murat Ferhat Ferhatoglu and Taner Kıvılcım Murat Ferhat Ferhatoglu and Taner Kıvılcım Additional information is available at the end of the chapter Additional information is available at the end of the chapter http://dx.doi.org/10.5772/intechopen.69583 Abstract Anatomy knowledge is the basic stone of healing diseases. Arteries, veins, wall structure, nerves, narrowing, curves, relations with other organs are very important to understand eso- phagial diseases. In this chapter we aimed to explain anatomical fundementals of oesophagus. Keywords: anatomy, esophagus, parts of esophagus, blood supply of esophagus, innervation of esophagus 1. Introduction Esophagus is a muscular tube-like organ that originates from endodermal primitive gut, 25–28 cm long, approximately 2 cm in diameter, located between lower border of laryngeal part of pharynx (Figure 1) and cardia of stomach. Start and end points of esophagus correspond to 6th cervi- cal vertebra and 11th thoracic vertebra topographically, and the gastroesophageal junction cor- responds to xiphoid process of sternum. Five cm of esophagus is in the neck, and it descends over superior mediastinum and posterior mediastinum approximately 17–18 cm, continues for 1–1.5 cm in diaphragm, ending with 2–3 cm of esophagus in abdomen (Figure 2) [1, 2]. Sex, age, physi- cal condition, and gender affect the length of esophagus. A newborn’s esophagus is 18 cm long, and it begins and ends one or two vertebra higher than in adult. Esophagus lengthens to 22 cm long by age 3 years and to 27 cm by age 10 years [3, 4]. -

Pre-Clinical Efficacy and Safety Evaluation of Human Amniotic Fluid-Derived Stem Cell Injection in a Mouse Model of Urinary Incontinence
http://dx.doi.org/10.3349/ymj.2015.56.3.648 Original Article pISSN: 0513-5796, eISSN: 1976-2437 Yonsei Med J 56(3):648-657, 2015 Pre-Clinical Efficacy and Safety Evaluation of Human Amniotic Fluid-Derived Stem Cell Injection in a Mouse Model of Urinary Incontinence Jae Young Choi,1* So Young Chun,2* Bum Soo Kim,1 Hyun Tae Kim,1 Eun Sang Yoo,1 Yun-Hee Shon,2 Jeong Ok Lim,2 Seok Joong Yun,3 Phil Hyun Song,4 Sung Kwang Chung,1 James J Yoo,2,5 and Tae Gyun Kwon1,2 1Department of Urology, School of Medicine, Kyungpook National University, Daegu; 2Joint Institute for Regenerative Medicine, Kyungpook National University Hospital, Daegu; 3Department of Urology, College of Medicine, Chungbuk National University, Cheongju; 4Department of Urology, College of Medicine, Yeungnam University, Daegu, Korea; 5Wake Forest Institute for Regenerative Medicine, Wake Forest University School of Medicine, Winston-Salem, NC, USA. Received: March 31, 2014 Purpose: Stem cell-based therapies represent new promises for the treatment of Revised: August 10, 2014 urinary incontinence. This study was performed to assess optimized cell passage Accepted: August 13, 2014 number, cell dose, therapeutic efficacy, feasibility, toxicity, and cell trafficking for Corresponding author: Dr. Tae Gyun Kwon, the first step of the pre-clinical evaluation of human amniotic fluid stem cell (hAF- Department of Urology, School of Medicine, Kyungpook National University, SC) therapy in a urinary incontinence animal model. Materials and Methods: 130 Dongdeok-ro, Jung-gu, The proper cell passage number was analyzed with hAFSCs at passages 4, 6, and Daegu 700-721, Korea.