Anatomical Variations in the Emergence
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Tentorium Cerebelli: the Bridge Between the Central and Peripheral Nervous System, Part 2
Open Access Review Article DOI: 10.7759/cureus.5679 Tentorium Cerebelli: the Bridge Between the Central and Peripheral Nervous System, Part 2 Bruno Bordoni 1 , Marta Simonelli 2 , Maria Marcella Lagana 3 1. Cardiology, Foundation Don Carlo Gnocchi, Milan, ITA 2. Osteopathy, French-Italian School of Osteopathy, Pisa, ITA 3. Radiology, IRCCS Fondazione Don Carlo Gnocchi Onlus, Milan, ITA Corresponding author: Bruno Bordoni, [email protected] Abstract The tentorium cerebelli is a meningeal portion in relation to the skull, the nervous system, and the cervical tract. In this second part, the article discusses the systematic tentorial relationships, such as the central and cervical neurological connections, the venous circulation and highlights possible clinical alterations that could cause pain. To understand the function of anatomy, we should always remember that every area of the human body is never a segment, but a functional continuum. Categories: Physical Medicine & Rehabilitation, Anatomy, Osteopathic Medicine Keywords: tentorium cerebelli, fascia, pain, venous circulation, neurological connections, cranio Introduction And Background Cervical neurological connections The ansa cervicalis characterizes the first cervical roots and connects all anterior cervical nerve exits with the inferior floor of the oral cavity, the trigeminal system, the respiratory control system, and the sympathetic system. The descending branch of the hypoglossal nerve anastomoses with C1, forming the ansa hypoglossi or ansa cervicalis superior [1]. The inferior root of the ansa cervicalis, also known as descendens cervicalis, is formed by ascendant fibers from spinal nerves C2-C3 and occasionally fibers C4, lying anteriorly to the common carotid artery (it passes laterally or medially to the internal jugular vein upon anatomical variations) [1]. -

Human Anatomy
Human Anatomy د.فراس عبد الرحمن Lec.13 The neck Overview The neck is the area of the body between the base of the cranium superiorly and the suprasternal notch and the clavicles inferiorly. The neck joins the head to the trunk and limbs, serving as a major conduit for structures passing between them. Many important structures are crowded together in the neck, such as muscles, arteries, veins, nerves, lymphatics, thyroid and parathyroid glands, trachea, larynx, esophagus, and vertebrae. Carotid/jugular blood vessels are the major structures commonly injured in penetrating wounds of the neck. The brachial plexuses of nerves originate in the neck and pass inferolaterally to enter the axillae and continue to supply the upper limbs. Lymph from structures in the head and neck drains into cervical lymph nodes. Skin of the Neck The natural lines of cleavage of the skin (Wrinkle lines) are constant and run almost horizontally around the neck. This is important clinically because an incision along a cleavage line will heal as a narrow scar, whereas one that crosses the lines will heal as a wide or heaped-up scar. Fasciae of the Neck The neck is surrounded by a superficial cervical fascia that lies deep to the skin and invests the platysma muscle (a muscle of facial expression). A second deep cervical fascia tightly invests the neck structures and is divided into three layers. Superficial Cervical Fascia The superficial fascia of the neck forms a thin layer that encloses the platysma muscle. Also embedded in it are the cutaneous nerves, the superficial veins, and the superficial lymph nodes. -

Protection of Supraclavicular Nerve in the Surgical Procedures of Clavicle Fracture Fixation
Protection of Supraclavicular Nerve in the Surgical Procedures of Clavicle Fracture Fixation Abulaiti Abula First Aliated Hospital of Xinjiang Medical University Yanshi Liu First Aliated Hospital of Xinjiang Medical University Kai Liu First Aliated Hospital of Xinjiang Medical University Feiyu Cai First Aliated Hospital of Xinjiang Medical University Alimujiang Abulaiti First Aliated Hospital of Xinjiang Medical University Xiayimaierdan Maimaiti First Aliated Hospital of Xinjiang Medical University Peng Ren First Aliated Hospital of Xinjiang Medical University Aihemaitijiang yusufu ( [email protected] ) First Aliated Hospital of Xinjiang Medical University Research Article Keywords: Clavicle fracture, Open reduction and internal xation, Supraclavicular nerve injury Posted Date: May 27th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-549126/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/13 Abstract Background: The present study was to evaluate the clinical effectiveness of the protection of the supraclavicular nerve in the treatment of clavicle fracture using fracture reduction and percutaneous external locking plate xation or open reduction and internal xation (ORIF). Methods: A total of 27 patients suffered clavicle fracture and underwent fracture reduction and external or internal xation with reserved clavicular epithelial nerve in our department from January 2015 to January 2020 were retrospectively collected, including 19 males and 8 females with a mean age of 42 years (range 21 to 57 years). Among them, 17 patients were treated with the fracture reduction and percutaneous external locking plate xation, while the other 10 patients were treated with ORIF. The sensory function of the affected shoulder area and the superior lateral thoracic area after surgery was collected and analyzed, as well as the satisfaction rate after the xation was removed. -

A Comprehensive Review of Anatomy and Regional Anesthesia Techniques of Clavicle Surgeries
vv ISSN: 2641-3116 DOI: https://dx.doi.org/10.17352/ojor CLINICAL GROUP Received: 31 March, 2021 Research Article Accepted: 07 April, 2021 Published: 10 April, 2021 *Corresponding author: Dr. Kartik Sonawane, Uncovering secrets of the Junior Consultant, Department of Anesthesiol- ogy, Ganga Medical Centre & Hospitals, Pvt. Ltd. Coimbatore, Tamil Nadu, India, E-mail: beauty bone: A comprehensive Keywords: Clavicle fractures; Floating shoulder sur- gery; Clavicle surgery; Clavicle anesthesia; Procedure review of anatomy and specific anesthesia; Clavicular block regional anesthesia techniques https://www.peertechzpublications.com of clavicle surgeries Kartik Sonawane1*, Hrudini Dixit2, J.Balavenkatasubramanian3 and Palanichamy Gurumoorthi4 1Junior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 2Fellow in Regional Anesthesia, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 3Senior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 4Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India Abstract The clavicle is the most frequently fractured bone in humans. General anesthesia with or without Regional Anesthesia (RA) is most frequently used for clavicle surgeries due to its complex innervation. Many RA techniques, alone or in combination, have been used for clavicle surgeries. These include interscalene block, cervical plexus (superficial and deep) blocks, SCUT (supraclavicular nerve + selective upper trunk) block, and pectoral nerve blocks (PEC I and PEC II). The clavipectoral fascial plane block is also a safe and simple option and replaces most other RA techniques due to its lack of side effects like phrenic nerve palsy or motor block of the upper limb. -

Communications of Transverse Cervical Cutaneous Nerve with the Cervical Branch of Facial Nerve and Its Variant Nerve Endings
ogy: iol Cu ys r h re P n t & R y e s Anatomy & Physiology: Current m e Sirasanagandla et al., Anatom Physiol 2013, 3:1 o a t r a c n h DOI: 10.4172/2161-0940.1000114 A Research ISSN: 2161-0940 Case Report Open Access Communications of Transverse Cervical Cutaneous Nerve with the Cervical Branch of Facial Nerve and its Variant Nerve Endings Deep in the Parotid Gland Srinivasa Rao Sirasanagandla*, Swamy Ravindra S, Sapna Marpalli and Satheesha Nayak B Department of Anatomy, Melaka Manipal Medical College, Manipal University, Madhav Nagar, Manipal, Karnataka, India Abstract Anastomoses between the transverse cervical cutaneous nerve and the cervical branch of facial nerve are regularly present. The anatomic locations of these anastomoses were poorly documented in the literature. During regular dissection, we came across two of such anastomoses: one of the two anastomoses was identified posterior to submandibular gland, and the other was noted within the parenchyma of the parotid gland. Prior knowledge of anatomic locations of these anastomoses is clinically important as it allows a method for identification and preservation of the cervical branch of the facial nerve as well as a starting point for retrograde facial nerve dissections. In addition, few terminal nerve endings of transverse cervical cutaneous nerve were seen along the retromandibular vein, ducts and some were penetrating the interlobular septa of parotid gland. The functional significance of anatomic variations of its nerve terminal ends deep in the gland is yet to be evaluated. Keywords: Anastomoses; Transverse cervical cutaneous nerve; (TCCN) and supraclavicular nerves pierce the fascia to supply the skin. -
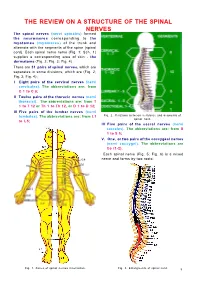
The Review on a Structure of the Spinal Nerves
THE REVIEW ON A STRUCTURE OF THE SPINAL NERVES The spinal nerves (nervi spinales) formed the neuromeres corresponding to the myotomes (myomeres) of the trunk and alternate with the segments of the spine (spinal cord). Each spinal nerve nerve (Fig. 1; Sch. 1) supplies a corresponding area of skin - the dermatome (Fig. 2; Fig. 3; Fig. 4). There are 31 pairs of spinal nerves, which are separates in some divisions, which are (Fig. 2; Fig. 3; Fig. 4): I Eight pairs of the cervical nerves (nervi cervicales). The abbreviations are: from С 1 to С 8; II Twelve pairs of the thoracic nerves (nervi thoracici). The abbreviations are: from T 1 to T 12 or Th 1 to Th 12, or D 1 to D 12; III Five pairs of the lumbar nerves (nervi lumbales). The abbreviations are: from L1 Fig. 2. Relations between vertebrae and segments of spinal cord. to L5; IV Five pairs of the sacral nerves (nervi sacrales). The abbreviations are: from S 1 to S 5; V. One, or two pairs of the coccygeal nerves (nervi coccygei). The abbreviations are Co (1-2). Each spinal nerve (Fig. 5; Fig. 6) is a mixed nerve and forms by two roots: Fig. 1. Zones of spinal nerves innervation. Fig. 3. Enlargments of spinal cord. 5 Fig. 4. Structure of the areas of spinal plexuses innervation. 1 the sensory, or the posterior root (radix subdural space. The roots unite and form the dorsalis seu posterior, seu sensorius spinal nerve (nervus spinalis). Since both nervi spinalis), which arise from the spinal roots are joined the spinal nerves continued as cord in the region of the posterior lateral mixed nerves. -

A Case of the Human Sternocleidomastoid Muscle Additionally Innervated by the Hypoglossal Nerve
Okajimas Folia Anat. Jpn., 69(6): 361-368, March, 1993 A Case of the Human Sternocleidomastoid Muscle Additionally Innervated by the Hypoglossal Nerve By Masahiro KOIZUMI, Masaharu HORIGUCHI, Shin'ichi SEKIYA, Sumio ISOGAI and Masato NAKANO Department of Anatomy, Iwate Medical University School of Medicine. Morioka, 020 Japan -Received for Publication, October 19, 1992- Key Words: Sternocleidomastoid muscle, Hypoglossal nerve, Superior sternoclavicular muscle (Hyrtl), Dual nerve supply, Gross anatomy Summary: An anomalous nerve supply from the hypoglossal nerve (XII) to the sternocleidomastoid muscle (SM) was observed in the right neck of an 82-year-old Japanese female. This nerve branch arose from the hypoglossal nerve at the origin of the superior root of the ansa cervicalis. The nerve fiber analysis revealed that this branch consisted of fibers from the hypoglossal nerve, the first and the second cervical nerves and had the same component as the superior root of the ansa cervicalis. SM appeared quite normal and the most part was innervated by the accessory nerve and a branch from the cervical plexus. The anomalous branch from XII supplied the small deep area near the anterior margin of the middle of the sternomastoid portion of SM. It is reasonable to think that the small deep area of SM, which was innervated by the anomalous branch from XII, occurs as the result of fusion of the muscular component from infrahyoid muscles. If the muscular component does not fuse with SM, it is thought to appear as an aberrant muscle such as the superior sternoclavicular muscle (Hyrtl) which is also supplied from a branch of the superior root of the ansa cervicalis. -

Original Article Supraclavicular Nerves Protection During Open Reduction and Internal Fixation
Int J Clin Exp Med 2017;10(5):8558-8565 www.ijcem.com /ISSN:1940-5901/IJCEM0038714 Original Article Supraclavicular nerves protection during open reduction and internal fixation Ting Li*, Jun He*, Junguo Wu, Guang Qian, Lei Geng, Hanwei Huang, Minghai Wang Department of Orthopedics, The Fifth People’s Hospital of Shanghai, Fudan University, Shanghai, China. *Co-first authors. Received July 15, 2016; Accepted November 29, 2016; Epub May 15, 2017; Published May 30, 2017 Abstract: Our study was to verify whether the approach of protecting supraclavicular nerve could effectively reduce the discomfort caused by iatrogenic injury to the supraclavicular nerve. A total of 37 patients with unilateral midcla- vicular fractures were enrolled and randomly assigned into the experimental group (patients received meticulous dissection by specially preservation of supraclavicular nerves with diameter > 0.5 mm during open reduction and internal fixation (ORIF)) and control group (patients received conventional ORIF). One year follow-up was performed after operation. Clinical outcomes including intraoperative and postoperative parameters were compared between groups. For the intraoperative parameters, no significant difference was found between groups in operative time (P = 0.074). However, the blood loss (P = 0.004) was significantly decreased and incision length (P = 0.008) was significantly longerin experimental group compared with control group. For postoperative parameters, the time of bone healing was similar between groups (P = 0.856). However, the degree and range of skin numbness were sig- nificantly decreased by specially preservation of supraclavicular nerves during ORIF compared with conventional ORIF at two weeks and one year after operation (P < 0.05). -

Posterior Triangle
POSTERIOR TRIANGLE BY DR . M.MD. MUSTAFA SHARIFF DEPT OF ANATOMY SENIOR LECTURER SRMDC & H POSTERIOR TRIANGLE • This is a triangular depressed space present above the middle one third of clavicle and behind the sternocleidomastoid muscle. POSTERIOR TRIANGLE OFNECK • Boundaries • – Infront – posterior border of sternocleidomastoid muscle • Behind – anterior border of trapezius • Base – Superior surface of middle 1/3rd of clavicle • Apex – Superior nuchal line where sternocleidomastoid and trapezius muscles meet • Roof – Skin, superficial fascia (platysma), investing layer of deep cervical fascia STERNOCLEIDOMASTOID MUSCLE (SCM) Origin: • Sternal head --- manubrium • Clavicular head --- medial 1/3 of clavicle Insertion: • Mastoid process and lateral ½ of superior nuchal line Action: • When muscle of one side contracts, the head is tilted to the same side and chin is rotated to opposite side. • When muscles of both side contract the head and neck are flexed Nerve supply: • Spinal part accessory nerve , ventral rami of spinal nerves C2,C3 TRAPEZIUS MUSCLE Origin: ✓ Superior nuchal line, ext. occipital protuberance, lig. nuchae, spines of C7 – T12 Insertion: ✓ Lateral 1/3 of clavicle, acromion, spine of scapula Functions: ✓ Elevation of scapula (sup. fibers), ✓ Depression of scapula (inf. fibers), ✓ Retraction of scapula (middle fibers), ✓ Superior rotation of glenoid fossa of scapula (sup. + inferior fibers). ROOF OF THE POSTERIOR TRIANGLE • The ROOF of the posterior triangle is the platysma m. and the investing layer of deep cervical fascia. Investing layer of deep cervical fascia • The platysma is a muscle of facial expression and will be Platysma m. discussed later. Roof is pierced by : Nerves : ✓ Lesser occipital, Anterior ✓ Great auricular,Superior ✓ Transverse cutaneous nerve of the neck, Posterior ✓ Supraclavicular nerves, Inferior • The FLOOR of the post. -

The LATIN LANGUAGE and Bases of Medical Terminology
The LATIN LANGUAGE and Bases of Medical Terminology The LATIN LANGUAGE and Bases of Medical Terminology ОДЕСЬКИЙ ДЕРЖАВНИЙ МЕДИЧНИЙ УНІВЕРСИТЕТ THE ODESSA STATE MEDICAL UNIVERSITY Áiáëiîòåêà ñòóäåíòà-ìåäèêà Medical Student’s Library Започатковано 1999 р. на честь 100-річчя Одеського державного медичного університету (1900–2000 рр.) Initiated in 1999 to mark the Centenary of the Odessa State Medical University (1900–2000) 2 THE LATIN LANGUAGE AND BASES OF MEDICAL TERMINOLOGY Practical course Recommended by the Central Methodical Committee for Higher Medical Education of the Ministry of Health of Ukraine as a manual for students of higher medical educational establishments of the IV level of accreditation using English Odessa The Odessa State Medical University 2008 3 BBC 81.461я73 UDC 811.124(075.8)61:001.4 Authors: G. G. Yeryomkina, T. F. Skuratova, N. S. Ivashchuk, Yu. O. Kravtsova Reviewers: V. K. Zernova, doctor of philological sciences, professor of the Foreign Languages Department of the Ukrainian Medical Stomatological Academy L. M. Kim, candidate of philological sciences, assistant professor, the head of the Department of Foreign Languages, Latin Language and Bases of Medical Terminology of the Vinnitsa State Medical University named after M. I. Pyrogov The manual is composed according to the curriculum of the Latin lan- guage and bases of medical terminology for medical higher schools. Designed to study the bases of general medical and clinical terminology, it contains train- ing exercises for the class-work, control questions and exercises for indivi- dual student’s work and the Latin-English and English-Latin vocabularies (over 2,600 terms). For the use of English speaking students of the first year of study at higher medical schools of IV accreditation level. -

Communication of the Anterior Branch of the Great Auricular Nerve with the Cervical Branch of Facial Nerve and Its Variant Nerve Endings Deep in the Parotid Gland
Int. J. Morphol., 30(3):840-842, 2012. Communication of the Anterior Branch of the Great Auricular Nerve with the Cervical Branch of Facial Nerve and its Variant Nerve Endings Deep in the Parotid Gland Comunicación del Ramo Anterior del Nervio Auricular Mayor con el Ramo Cervical del Nervio Facial y sus Terminaciones Nerviosas Profundas Variantes en la Glándula Parótida *Srinivasa Rao Sirasanagandla; *Satheesha Nayak B.; **Kumar M. R. Bhat & *Swamy Ravindra S. RAO, S. S.; NAYAK, B. S.; BHAT, K. M. R. & RAVINDRA, S. S. Communication of the anterior branch of the great auricular nerve with the cervical branch of facial nerve and its variant nerve endings deep in the parotid gland. Int. J. Morphol., 30(3):840-842, 2012. SUMMARY: The communications between the branches of cervical plexus and cervical branch of facial nerve are common and are well known. However, this communication usually occurs between the transverse cervical nerve and cervical branch of facial nerve. During routine dissection classes for the Medical undergraduate students, we came across an anatomical variant of anterior division of great auricular nerve. This variation was found in a 60-year-old male cadaver of South Indian origin and it was unilateral. The great auricular nerve arose from the loop of ventral rami of C2 and C3 spinal nerves and divided into anterior and posterior branches. The anterior branch ran obliquely upwards and forwards on the surface of the sternocleidomastoid muscle along with the external jugular vein towards the apex of parotid gland and divided into many branches. One of these branches gave a communicating branch to cervical branch of facial nerve outside the parotid gland. -

5. Upper Extremity Neuroanatomy
5. UPPER EXTREMITY compartments of the NEUROANATOMY arm). The brachial plexus divisions INTRODUCTION pass posterior to the mid-point of Regional anesthesia of the upper extremity in- the clavicle through volves two major nerve plexuses, the cervical plexus the cervico-axillary and the brachial plexus. A detailed understanding of canal. the anatomy of these nerve plexuses and surrounding • Three cords. The structures is essential for the safe and successful prac- divisions coalesce tice of regional anesthesia in this area of the body. to form three cords. The anterior CERVICAL PLEXUS divisions of the superior and middle The cervical plexus is formed from a series of nerve trunk form the loops between adjacent anterior rami of cervical nerve lateral cord. The roots C1 through C4. The cervical plexus is deep to the anterior division of sternocleidomastoid muscle and medial to the scalene the inferior trunk muscles. The deep branches of the plexus are motor becomes the medial nerves. They include the phrenic nerve (diaphragm cord. The posterior muscle) and the ansa cervicalis nerve (omohyoid, divisions of all sternothyroid, and sternohyoid muscles). The named three trunks unite nerves of the superficial cervical plexus are branches to form the posterior from the loops and emerge from the middle of the ster- Figure 5-1. Dissection of the superficial cervical plexus in the posterior triangle cord. The cords are nocleidomastoid muscle (Figure 5-1): BRACHIAL PLEXUS named based on their relationship to the axillary artery (as this • Lesser occipital nerve (C2): innervates the skin The brachial plexus is formed from the five roots neurovascular bundle passes in its sheath into posterior to the ear.