Human Anatomy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Weakness, Dysphagia, and Stridor After Botulinum Toxin Injections
CASE REPORT Too Much of a Good Thing: Weakness, Dysphagia, and Stridor After Botulinum Toxin Injections Steven Dominguez, MD, MPH; Marek Dobke, MD, PhD; Steven Dominguez Jr, BS A 68-year-old woman presented with diminished ability to raise her head, difficulty swallowing, and intermittent stridor 5 days after receiving 225 IU of onabotulinumtoxinA. Case of treatment, the patient was under the care A 68-year-old woman presented to the ED of a plastic surgeon; thereafter, she sought 5 days after receiving onabotulinumtoxinA treatment at a physician-owned medical cosmetic injections for wrinkles of the face spa because it offered onabotulinumtoxi- and neck. She stated that she was unable nA at a lower price. The injections at the to raise her head while in a supine position medical spa were administered by a physi- and that her head felt heavy when standing. cian assistant (PA). The patient stated that She also experienced spasms and strain although the PA had steadily increased the of the posterior cervical neck muscles. In dose of onabotulinumtoxinA to maintain addition, the patient described a constant the desired aesthetic effect, this was the need to swallow forcefully throughout the first time she had experienced any side ef- day, and felt an intermittent heavy sensa- fects from the treatment. tion over her larynx that was associated The ED staff contacted the medical with stridor. She noted these symptoms spa provider, who reviewed the patient’s began 5 days after the onabotulinumtoxi- medical record over the telephone. The nA injections and had peaked 2 days prior PA stated that he had been the only practi- to presentation. -

Protection of Supraclavicular Nerve in the Surgical Procedures of Clavicle Fracture Fixation
Protection of Supraclavicular Nerve in the Surgical Procedures of Clavicle Fracture Fixation Abulaiti Abula First Aliated Hospital of Xinjiang Medical University Yanshi Liu First Aliated Hospital of Xinjiang Medical University Kai Liu First Aliated Hospital of Xinjiang Medical University Feiyu Cai First Aliated Hospital of Xinjiang Medical University Alimujiang Abulaiti First Aliated Hospital of Xinjiang Medical University Xiayimaierdan Maimaiti First Aliated Hospital of Xinjiang Medical University Peng Ren First Aliated Hospital of Xinjiang Medical University Aihemaitijiang yusufu ( [email protected] ) First Aliated Hospital of Xinjiang Medical University Research Article Keywords: Clavicle fracture, Open reduction and internal xation, Supraclavicular nerve injury Posted Date: May 27th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-549126/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/13 Abstract Background: The present study was to evaluate the clinical effectiveness of the protection of the supraclavicular nerve in the treatment of clavicle fracture using fracture reduction and percutaneous external locking plate xation or open reduction and internal xation (ORIF). Methods: A total of 27 patients suffered clavicle fracture and underwent fracture reduction and external or internal xation with reserved clavicular epithelial nerve in our department from January 2015 to January 2020 were retrospectively collected, including 19 males and 8 females with a mean age of 42 years (range 21 to 57 years). Among them, 17 patients were treated with the fracture reduction and percutaneous external locking plate xation, while the other 10 patients were treated with ORIF. The sensory function of the affected shoulder area and the superior lateral thoracic area after surgery was collected and analyzed, as well as the satisfaction rate after the xation was removed. -

A Comprehensive Review of Anatomy and Regional Anesthesia Techniques of Clavicle Surgeries
vv ISSN: 2641-3116 DOI: https://dx.doi.org/10.17352/ojor CLINICAL GROUP Received: 31 March, 2021 Research Article Accepted: 07 April, 2021 Published: 10 April, 2021 *Corresponding author: Dr. Kartik Sonawane, Uncovering secrets of the Junior Consultant, Department of Anesthesiol- ogy, Ganga Medical Centre & Hospitals, Pvt. Ltd. Coimbatore, Tamil Nadu, India, E-mail: beauty bone: A comprehensive Keywords: Clavicle fractures; Floating shoulder sur- gery; Clavicle surgery; Clavicle anesthesia; Procedure review of anatomy and specific anesthesia; Clavicular block regional anesthesia techniques https://www.peertechzpublications.com of clavicle surgeries Kartik Sonawane1*, Hrudini Dixit2, J.Balavenkatasubramanian3 and Palanichamy Gurumoorthi4 1Junior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 2Fellow in Regional Anesthesia, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 3Senior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 4Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India Abstract The clavicle is the most frequently fractured bone in humans. General anesthesia with or without Regional Anesthesia (RA) is most frequently used for clavicle surgeries due to its complex innervation. Many RA techniques, alone or in combination, have been used for clavicle surgeries. These include interscalene block, cervical plexus (superficial and deep) blocks, SCUT (supraclavicular nerve + selective upper trunk) block, and pectoral nerve blocks (PEC I and PEC II). The clavipectoral fascial plane block is also a safe and simple option and replaces most other RA techniques due to its lack of side effects like phrenic nerve palsy or motor block of the upper limb. -

Communications of Transverse Cervical Cutaneous Nerve with the Cervical Branch of Facial Nerve and Its Variant Nerve Endings
ogy: iol Cu ys r h re P n t & R y e s Anatomy & Physiology: Current m e Sirasanagandla et al., Anatom Physiol 2013, 3:1 o a t r a c n h DOI: 10.4172/2161-0940.1000114 A Research ISSN: 2161-0940 Case Report Open Access Communications of Transverse Cervical Cutaneous Nerve with the Cervical Branch of Facial Nerve and its Variant Nerve Endings Deep in the Parotid Gland Srinivasa Rao Sirasanagandla*, Swamy Ravindra S, Sapna Marpalli and Satheesha Nayak B Department of Anatomy, Melaka Manipal Medical College, Manipal University, Madhav Nagar, Manipal, Karnataka, India Abstract Anastomoses between the transverse cervical cutaneous nerve and the cervical branch of facial nerve are regularly present. The anatomic locations of these anastomoses were poorly documented in the literature. During regular dissection, we came across two of such anastomoses: one of the two anastomoses was identified posterior to submandibular gland, and the other was noted within the parenchyma of the parotid gland. Prior knowledge of anatomic locations of these anastomoses is clinically important as it allows a method for identification and preservation of the cervical branch of the facial nerve as well as a starting point for retrograde facial nerve dissections. In addition, few terminal nerve endings of transverse cervical cutaneous nerve were seen along the retromandibular vein, ducts and some were penetrating the interlobular septa of parotid gland. The functional significance of anatomic variations of its nerve terminal ends deep in the gland is yet to be evaluated. Keywords: Anastomoses; Transverse cervical cutaneous nerve; (TCCN) and supraclavicular nerves pierce the fascia to supply the skin. -
The Review on a Structure of the Spinal Nerves
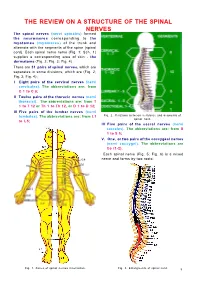
THE REVIEW ON A STRUCTURE OF THE SPINAL NERVES The spinal nerves (nervi spinales) formed the neuromeres corresponding to the myotomes (myomeres) of the trunk and alternate with the segments of the spine (spinal cord). Each spinal nerve nerve (Fig. 1; Sch. 1) supplies a corresponding area of skin - the dermatome (Fig. 2; Fig. 3; Fig. 4). There are 31 pairs of spinal nerves, which are separates in some divisions, which are (Fig. 2; Fig. 3; Fig. 4): I Eight pairs of the cervical nerves (nervi cervicales). The abbreviations are: from С 1 to С 8; II Twelve pairs of the thoracic nerves (nervi thoracici). The abbreviations are: from T 1 to T 12 or Th 1 to Th 12, or D 1 to D 12; III Five pairs of the lumbar nerves (nervi lumbales). The abbreviations are: from L1 Fig. 2. Relations between vertebrae and segments of spinal cord. to L5; IV Five pairs of the sacral nerves (nervi sacrales). The abbreviations are: from S 1 to S 5; V. One, or two pairs of the coccygeal nerves (nervi coccygei). The abbreviations are Co (1-2). Each spinal nerve (Fig. 5; Fig. 6) is a mixed nerve and forms by two roots: Fig. 1. Zones of spinal nerves innervation. Fig. 3. Enlargments of spinal cord. 5 Fig. 4. Structure of the areas of spinal plexuses innervation. 1 the sensory, or the posterior root (radix subdural space. The roots unite and form the dorsalis seu posterior, seu sensorius spinal nerve (nervus spinalis). Since both nervi spinalis), which arise from the spinal roots are joined the spinal nerves continued as cord in the region of the posterior lateral mixed nerves. -

319: Platysmaplasty: a Surgical Resolution of "Turkey Neck"
Platysmaplasty A surgical resolution for the “turkey neck” by Nydia Morales,I Morales, CST CST The term “turkey neck” refers to the lateral ptosis of the frontal neck derma. This can occur when the platysma muscles separate, a result of natural weak- ening of the ligaments in the cervical region, as well as excessive lipid build- up. Other causes of this condition include genetics, bone loss and decline of skin elasticity—possibly from weight loss. It is most commonly regarded as a factor of aging, although sun exposure and smoking may also contribute. or patients who are interested in reducing the loose look of sagging skin in the neck area under the jaw line, a platys- LEARNING OBJECTIVES maplasty, or neck lift, is an option. It can be performed in F ▲ conjunction with a face lift, but it is often performed as a Review the relevant anatomy for this stand-alone procedure. This article examines the surgical options procedure for resolving turkey neck, as well as alternatives to surgery. ▲ Examine the set-up and surgical ETIOLOGY AND ANATOMY positioning for this procedure The platysma muscle is one of a pair of plate-like, wide muscles at the side of the neck. It arises from the fascia covering the supe- ▲ Compare and contrast the differences rior parts of the pectoralis major and the deltoideus. It crosses between an in-office procedure and a the clavicle and rises obliquely and medially along the side of typical OR procedure the neck. The platysma covers the external jugular vein as the vein descends from the angle of the mandible to the clavicle. -

Esthetic Shaping of the Neck/Positive Side Effects on the Gingiva’ Warren Roberts, DMD
Dental Facial Aesthetics ‘Aesthetic shaping of the neck/positive side effects on the gingiva’ Warren Roberts, DMD This article discusses the relationship between Platysma, a large muscle of the face and neck, and the periodontium of the lower teeth. The article explores the relationship between the contraction of the platysma muscle during its repeated use as a muscle of facial expression, the pull of labial mandibular frenums and the development of gingival recession. The use of Botox Cosmetic to soften the action of this muscle is suggested as a minimally invasive therapy in preventing gingival recession. t is now widely recognized that there is a critical ongoing maintenance problem as well as contributing to relationship between the muscles of facial expression, facial tooth loss. Traditionally gingival recession has been attributed soft tissue contours and dental smile design (1). Among other to aggressive tooth brushing or flossing, untreated Ifactors, the amount of upper incisor display is influenced by periodontal disease, occlusal dysfunction, abfraction, genetics the volume of the cheeks, the fullness of the lips and even and age. There may be another factor that has been the activity of muscles in the glabellar region. All the muscles overlooked. Current treatment for lack of gingival of facial expression are interconnected (2). The aging soft attachment often involves surgical intervention through tissue of the face must be included in the diagnosis prior to various grafting procedures (Fig. 2 & 3). Subsequently, the definitive cosmetic dental treatment as the final restorative frenums are often still observable exerting a downward pull approach needs to take into account other facial esthetic (Fig. -

Original Article Supraclavicular Nerves Protection During Open Reduction and Internal Fixation
Int J Clin Exp Med 2017;10(5):8558-8565 www.ijcem.com /ISSN:1940-5901/IJCEM0038714 Original Article Supraclavicular nerves protection during open reduction and internal fixation Ting Li*, Jun He*, Junguo Wu, Guang Qian, Lei Geng, Hanwei Huang, Minghai Wang Department of Orthopedics, The Fifth People’s Hospital of Shanghai, Fudan University, Shanghai, China. *Co-first authors. Received July 15, 2016; Accepted November 29, 2016; Epub May 15, 2017; Published May 30, 2017 Abstract: Our study was to verify whether the approach of protecting supraclavicular nerve could effectively reduce the discomfort caused by iatrogenic injury to the supraclavicular nerve. A total of 37 patients with unilateral midcla- vicular fractures were enrolled and randomly assigned into the experimental group (patients received meticulous dissection by specially preservation of supraclavicular nerves with diameter > 0.5 mm during open reduction and internal fixation (ORIF)) and control group (patients received conventional ORIF). One year follow-up was performed after operation. Clinical outcomes including intraoperative and postoperative parameters were compared between groups. For the intraoperative parameters, no significant difference was found between groups in operative time (P = 0.074). However, the blood loss (P = 0.004) was significantly decreased and incision length (P = 0.008) was significantly longerin experimental group compared with control group. For postoperative parameters, the time of bone healing was similar between groups (P = 0.856). However, the degree and range of skin numbness were sig- nificantly decreased by specially preservation of supraclavicular nerves during ORIF compared with conventional ORIF at two weeks and one year after operation (P < 0.05). -

Posterior Triangle
POSTERIOR TRIANGLE BY DR . M.MD. MUSTAFA SHARIFF DEPT OF ANATOMY SENIOR LECTURER SRMDC & H POSTERIOR TRIANGLE • This is a triangular depressed space present above the middle one third of clavicle and behind the sternocleidomastoid muscle. POSTERIOR TRIANGLE OFNECK • Boundaries • – Infront – posterior border of sternocleidomastoid muscle • Behind – anterior border of trapezius • Base – Superior surface of middle 1/3rd of clavicle • Apex – Superior nuchal line where sternocleidomastoid and trapezius muscles meet • Roof – Skin, superficial fascia (platysma), investing layer of deep cervical fascia STERNOCLEIDOMASTOID MUSCLE (SCM) Origin: • Sternal head --- manubrium • Clavicular head --- medial 1/3 of clavicle Insertion: • Mastoid process and lateral ½ of superior nuchal line Action: • When muscle of one side contracts, the head is tilted to the same side and chin is rotated to opposite side. • When muscles of both side contract the head and neck are flexed Nerve supply: • Spinal part accessory nerve , ventral rami of spinal nerves C2,C3 TRAPEZIUS MUSCLE Origin: ✓ Superior nuchal line, ext. occipital protuberance, lig. nuchae, spines of C7 – T12 Insertion: ✓ Lateral 1/3 of clavicle, acromion, spine of scapula Functions: ✓ Elevation of scapula (sup. fibers), ✓ Depression of scapula (inf. fibers), ✓ Retraction of scapula (middle fibers), ✓ Superior rotation of glenoid fossa of scapula (sup. + inferior fibers). ROOF OF THE POSTERIOR TRIANGLE • The ROOF of the posterior triangle is the platysma m. and the investing layer of deep cervical fascia. Investing layer of deep cervical fascia • The platysma is a muscle of facial expression and will be Platysma m. discussed later. Roof is pierced by : Nerves : ✓ Lesser occipital, Anterior ✓ Great auricular,Superior ✓ Transverse cutaneous nerve of the neck, Posterior ✓ Supraclavicular nerves, Inferior • The FLOOR of the post. -

Anatomy Module 3. Muscles. Materials for Colloquium Preparation
Section 3. Muscles 1 Trapezius muscle functions (m. trapezius): brings the scapula to the vertebral column when the scapulae are stable extends the neck, which is the motion of bending the neck straight back work as auxiliary respiratory muscles extends lumbar spine when unilateral contraction - slightly rotates face in the opposite direction 2 Functions of the latissimus dorsi muscle (m. latissimus dorsi): flexes the shoulder extends the shoulder rotates the shoulder inwards (internal rotation) adducts the arm to the body pulls up the body to the arms 3 Levator scapula functions (m. levator scapulae): takes part in breathing when the spine is fixed, levator scapulae elevates the scapula and rotates its inferior angle medially when the shoulder is fixed, levator scapula flexes to the same side the cervical spine rotates the arm inwards rotates the arm outward 4 Minor and major rhomboid muscles function: (mm. rhomboidei major et minor) take part in breathing retract the scapula, pulling it towards the vertebral column, while moving it upward bend the head to the same side as the acting muscle tilt the head in the opposite direction adducts the arm 5 Serratus posterior superior muscle function (m. serratus posterior superior): brings the ribs closer to the scapula lift the arm depresses the arm tilts the spine column to its' side elevates ribs 6 Serratus posterior inferior muscle function (m. serratus posterior inferior): elevates the ribs depresses the ribs lift the shoulder depresses the shoulder tilts the spine column to its' side 7 Latissimus dorsi muscle functions (m. latissimus dorsi): depresses lifted arm takes part in breathing (auxiliary respiratory muscle) flexes the shoulder rotates the arm outward rotates the arm inwards 8 Sources of muscle development are: sclerotome dermatome truncal myotomes gill arches mesenchyme cephalic myotomes 9 Muscle work can be: addacting overcoming ceding restraining deflecting 10 Intrinsic back muscles (autochthonous) are: minor and major rhomboid muscles (mm. -

Communication of the Anterior Branch of the Great Auricular Nerve with the Cervical Branch of Facial Nerve and Its Variant Nerve Endings Deep in the Parotid Gland
Int. J. Morphol., 30(3):840-842, 2012. Communication of the Anterior Branch of the Great Auricular Nerve with the Cervical Branch of Facial Nerve and its Variant Nerve Endings Deep in the Parotid Gland Comunicación del Ramo Anterior del Nervio Auricular Mayor con el Ramo Cervical del Nervio Facial y sus Terminaciones Nerviosas Profundas Variantes en la Glándula Parótida *Srinivasa Rao Sirasanagandla; *Satheesha Nayak B.; **Kumar M. R. Bhat & *Swamy Ravindra S. RAO, S. S.; NAYAK, B. S.; BHAT, K. M. R. & RAVINDRA, S. S. Communication of the anterior branch of the great auricular nerve with the cervical branch of facial nerve and its variant nerve endings deep in the parotid gland. Int. J. Morphol., 30(3):840-842, 2012. SUMMARY: The communications between the branches of cervical plexus and cervical branch of facial nerve are common and are well known. However, this communication usually occurs between the transverse cervical nerve and cervical branch of facial nerve. During routine dissection classes for the Medical undergraduate students, we came across an anatomical variant of anterior division of great auricular nerve. This variation was found in a 60-year-old male cadaver of South Indian origin and it was unilateral. The great auricular nerve arose from the loop of ventral rami of C2 and C3 spinal nerves and divided into anterior and posterior branches. The anterior branch ran obliquely upwards and forwards on the surface of the sternocleidomastoid muscle along with the external jugular vein towards the apex of parotid gland and divided into many branches. One of these branches gave a communicating branch to cervical branch of facial nerve outside the parotid gland. -

Advanced Neuroanatomic Understanding of the Shoulder and Implications for Pain Management
Advanced Neuroanatomic Understanding of The Shoulder and Implications for Pain Management Maxim S. Eckmann, MD Professor/Clinical, Department of Anesthesiology Executive Director of Pain Medicine University of Texas Health Science Center at San Antonio Disclosures ▪ Employment ▪ University of Texas Health Science Center at San Antonio ▪ Research Support ▪ Avanos Medical Inc – cadaver donation ▪ Fellowship Education Grants ▪ Abbot ▪ Boston Scientific ▪ Medtronic ▪ Speaker Panel / Course Director ▪ Dannemiller, Inc. ▪ American Society of Regional Anesthesia and Pain Medicine ▪ Investments ▪ Insight Dental Systems ▪ iKare MTRC (Behavioral Health) Leveraging Increasingly Peripheral Nerve Blockade in Acute and Chronic Pain Gains and Losses ISB (interscalene block); STB (superior trunk block); LPB (lumbar plexus block); ACB (adductor canal block); Road Map: Joint Analgesia Progression LFCN (lateral femoral cutaneous nerve); IPACK (infiltration between popliteal artery and capsule of knee); PECS (pectoralis block) Plexus Level Peripheral Nerve, Plane Level *,** Articular Level** Field** Suprascap* Sup Cerv Plx Articular Ns ISB Shoulder Axillary* PECS I,II ? SS, Ax, LP, STB*? Lateral Pec* (adjunct)* SubScap… Femoral Joint / ACB** / Knee Neuraxial LPB Sciatic Genicular Ns Wound IPACK** Obturator Injection Femoral “3-in-1” LPB Articular Ns Hip Sciatic ?Quad Fem / SPB Fem / Obt Obturator Sup Glut * Diaphragm Sparing **Motor Movement Sparing Proximal: Progressive loss of: o Dermatome o Cutaneous, muscular anesthesia. Distal: o Myotome/Sclerotome o Osteotome/Capsulotome o Osteotome/Capsulotome Progressive gain of: o Motor Block o Motor function o Motor preservation Evolving understanding: Shoulder Joint Selected Developments in Regional Anesthesia for the Upper Extremity and Shoulder • Axillary (brachial plexus) block • Interscalene Block • Complications Interscalene Block Development and Complications • Multiple Approaches (e.g. Anterolateral, Posterior, etc.) • Single Injection and Continuous Techniques 1.