Spinal Nerves Spinal Nerves
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -

Anatomical Study of the Superior Cluneal Nerve and Its Estimation of Prevalence As a Cause of Lower Back Pain in a South African Population
Anatomical study of the superior cluneal nerve and its estimation of prevalence as a cause of lower back pain in a South African population by Leigh-Anne Loubser (10150804) Dissertation to be submitted in full fulfilment of the requirements for the degree Master of Science in Anatomy In the Faculty of Health Science University of Pretoria Supervisor: Prof AN Van Schoor1 Co-supervisor: Dr RP Raath2 1 Department of Anatomy, University of Pretoria 2 Netcare Jakaranda Hospital, Pretoria 2017 DECLARATION OF ORIGINALITY UNIVERSITY OF PRETORIA The Department of Anatomy places great emphasis upon integrity and ethical conduct in the preparation of all written work submitted for academic evaluation. While academic staff teach you about referencing techniques and how to avoid plagiarism, you too have a responsibility in this regard. If you are at any stage uncertain as to what is required, you should speak to your lecturer before any written work is submitted. You are guilty of plagiarism if you copy something from another author’s work (e.g. a book, an article, or a website) without acknowledging the source and pass it off as your own. In effect, you are stealing something that belongs to someone else. This is not only the case when you copy work word-for-word (verbatim), but also when you submit someone else’s work in a slightly altered form (paraphrase) or use a line of argument without acknowledging it. You are not allowed to use work previously produced by another student. You are also not allowed to let anybody copy your work with the intention of passing if off as his/her work. -
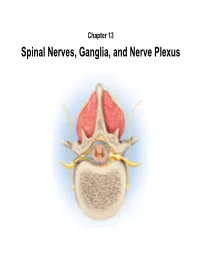
Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves
Chapter 13 Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves Posterior Spinous process of vertebra Posterior root Deep muscles of back Posterior ramus Spinal cord Transverse process of vertebra Posterior root ganglion Spinal nerve Anterior ramus Meningeal branch Communicating rami Anterior root Vertebral body Sympathetic ganglion Anterior General Anatomy of Nerves and Ganglia • Spinal cord communicates with the rest of the body by way of spinal nerves • nerve = a cordlike organ composed of numerous nerve fibers (axons) bound together by connective tissue – mixed nerves contain both afferent (sensory) and efferent (motor) fibers – composed of thousands of fibers carrying currents in opposite directions Anatomy of a Nerve Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Epineurium Perineurium Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Endoneurium Nerve Rootlets fiber Posterior root Fascicle Posterior root ganglion Anterior Blood root vessels Spinal nerve (b) Copyright by R.G. Kessel and R.H. Kardon, Tissues and Organs: A Text-Atlas of Scanning Electron Microscopy, 1979, W.H. Freeman, All rights reserved Blood vessels Fascicle Epineurium Perineurium Unmyelinated nerve fibers Myelinated nerve fibers (a) Endoneurium Myelin General Anatomy of Nerves and Ganglia • nerves of peripheral nervous system are ensheathed in Schwann cells – forms neurilemma and often a myelin sheath around the axon – external to neurilemma, each fiber is surrounded by -

Herpes Zoster by Lesia Dropulic, MD
Herpes Zoster Lesia Dropulic Jeffrey Cohen Laboratory of Infectious Diseases, NIAID Varicella (Chickenpox) Centers for Disease Control and Prevention Zoster (Shingles) Centers for Disease Control and Prevention Zoster is Due to Reactivation of Varicella from the Nervous System Blood Adapted from Kimberlin and Whitley NEJM 2007 VZV DNA is Present In Neurons in Ganglia Years After Chickenpox Ganglia latently infected with VZV Subject No. Neurons No. (%) neurons Median VZV DNA Number Tested positive for VZV copies/positive cell Wang et al J Virol 2005 History of Zoster • Zoster: Greek for girdle • Shingles: Latin (cingere) girdle Partial encircling of the trunk with rash First Cell Culture of Varicella-Zoster Virus (March 19, 1949) Thomas Weller in Varicella-Zoster Virus, Cambridge Press 2000 Varicella- Zoster Virus Straus et al. Ann Intern Med 1988 Epidemiology of Zoster • About 99% of adults >40 yo infected with varicella-zoster, thus all older adults at risk • About 1 million cases in the US each year • Rates appear to be increasing • 50% of persons of live to age 85 will develop zoster, 5% may get a second case Risk Factors for Zoster • Age- the major risk factor for healthy persons (long duration since exposure to virus) • Immune compromise- T cell immunity: transplant recipients, leukemia, lymphoma; HIV increases the risk up to 50 fold • Age and immune compromise- reduced VZV-specific T cell immunity Varicella-Zoster Virus: Site of Latency • Varicella-zoster virus is latent in dorsal root ganglia (along the spine) or cranial nerve -

The Neuroanatomy of Female Pelvic Pain
Chapter 2 The Neuroanatomy of Female Pelvic Pain Frank H. Willard and Mark D. Schuenke Introduction The female pelvis is innervated through primary afferent fi bers that course in nerves related to both the somatic and autonomic nervous systems. The somatic pelvis includes the bony pelvis, its ligaments, and its surrounding skeletal muscle of the urogenital and anal triangles, whereas the visceral pelvis includes the endopelvic fascial lining of the levator ani and the organ systems that it surrounds such as the rectum, reproductive organs, and urinary bladder. Uncovering the origin of pelvic pain patterns created by the convergence of these two separate primary afferent fi ber systems – somatic and visceral – on common neuronal circuitry in the sacral and thoracolumbar spinal cord can be a very dif fi cult process. Diagnosing these blended somatovisceral pelvic pain patterns in the female is further complicated by the strong descending signals from the cerebrum and brainstem to the dorsal horn neurons that can signi fi cantly modulate the perception of pain. These descending systems are themselves signi fi cantly in fl uenced by both the physiological (such as hormonal) and psychological (such as emotional) states of the individual further distorting the intensity, quality, and localization of pain from the pelvis. The interpretation of pelvic pain patterns requires a sound knowledge of the innervation of somatic and visceral pelvic structures coupled with an understand- ing of the interactions occurring in the dorsal horn of the lower spinal cord as well as in the brainstem and forebrain. This review will examine the somatic and vis- ceral innervation of the major structures and organ systems in and around the female pelvis. -

A Step Towards Stereotactic Navigation During Pelvic Surgery: 3D Nerve Topography
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Erasmus University Digital Repository Surgical Endoscopy and Other Interventional Techniques https://doi.org/10.1007/s00464-018-6086-3 A step towards stereotactic navigation during pelvic surgery: 3D nerve topography A. R. Wijsmuller1,2 · C. Giraudeau3 · J. Leroy4 · G. J. Kleinrensink5 · E. Rociu6 · L. G. Romagnolo7 · A. G. F. Melani7,8,9 · V. Agnus2 · M. Diana3 · L. Soler3 · B. Dallemagne2 · J. Marescaux2 · D. Mutter2 Received: 10 May 2017 / Accepted: 1 February 2018 © The Author(s) 2018. This article is an open access publication Abstract Background Long-term morbidity after multimodal treatment for rectal cancer is suggested to be mainly made up by nerve- injury-related dysfunctions. Stereotactic navigation for rectal surgery was shown to be feasible and will be facilitated by highlighting structures at risk of iatrogenic damage. The aim of this study was to investigate the ability to make a 3D map of the pelvic nerves with magnetic resonance imaging (MRI). Methods A systematic review was performed to identify a main positional reference for each pelvic nerve and plexus. The nerves were manually delineated in 20 volunteers who were scanned with a 3-T MRI. The nerve identifiability rate and the likelihood of nerve identification correctness were determined. Results The analysis included 61 studies on pelvic nerve anatomy. A main positional reference was defined for each nerve. On MRI, the sacral nerves, the lumbosacral plexus, and the obturator nerve could be identified bilaterally in all volunteers. The sympathetic trunk could be identified in 19 of 20 volunteers bilaterally (95%). -

Disc Pathology Lumbar Dermatomes
Lumbar Dermatomes: Disc Pathology Lumbar Dermatomes In this example, nerve root pain is due to disc pathology. Dermatomes are regions of altered sensation from irritated or damaged nerve roots. Symptoms that follow a dermatome (numbness, tingling or pain) may indicate a pathology that involves the related nerve root. These symptoms can follow the entire dermatome or just part of it. When symptoms cover more than one dermatome it may suggest more severe pathology and involvement of more than one nerve root. Disc Pathology: Lumbar Disc Pathology has various presentations. 1. Normal Disc 2. Internal Disc Disorder: Small tear at the inner part of the outer third of the disc where the annulus is innervated. 3. Outer Disc Disorder: Larger tear that extends to the outer part of the annulus. Discography is a good way to diagnose the morphology of the disc and establish the disc as a pain generator. 4. Protrusion: Small disc bulge and the outer layers of the annulus are intact 5. Prolapse: Large disc bulge that breaks through the layers of the annulus but not the posterior longitudinal ligament (PLL). 6. Extrusion: Large disc bulge that breaks through the layers of the annulus and the PLL. This often causes pain in a multitude of dermatomes. 7. Sequestration (not shown; rare): Disc fragment breaks away from the rest of the discs. 1. Sizer PS Jr, Phelps V, Matthijs O. Pain generators of the lumbar spine. Pain Pract. 2001;1(3):255‐ 273. 2. Sizer PS Jr, Phelps V, Dedrick G, Matthijs O. Differential diagnosis and management of spinal nerve root‐related pain. -

35. Lumbar Plexus. Sacral Plexus. Coccygeal Plexus
GUIDELINES Students’ independent work during preparation to practical lesson Academic discipline HUMAN ANATOMY Topic LUMBAR PLEXUS. SACRAL PLEXUS. COCCYGEAL PLEXUS 1. Relevance of the topic Lumbar, sacral and coccygeal plexuses innervate the skin of the abdomen, lower back and lower extremities and all the muscles of the lower limbs. Acquired knowledge is the basis for many fields of practical medicine, such as neurology, surgery and traumatology. 2. Specific objectives After the lesson the student should know and be able to: - describe the sources of the formation of the lumbar plexus; - classify the nerves of the lumbar plexus; - to be able to demonstrate and define the branches of the lumbar plexus; - describe sources of sacral plexus formation; - classify sacral plexus nerves; - be able to demonstrate and identify short and long branches of the sacral plexus; - describe the sources of formation coccygeal plexus; - classify coccygeal plexus nerves; - be able to demonstrate and identify branches of coccygeal plexus; - to explain the innervation of muscles and skin in the areas of the lower back and lower extremity. 3. Basic level of preparation For practical this lesson a student should know and be able: - to know the anatomy of the spine, pelvis, lower extremities; - to analyze and show large and small pelvis, their bones; - to analyze and demonstrate bones and joints of the lower limbs; - to demonstrate muscles of the abdomen, perineum, pelvic girdle and lower limbs; - to know the anatomy (external and internal structure) of the spinal cord; - to know the spinal nerve anatomy. 4. Tasks for independent work during preparation for the classes 4.1. -

Management of Metastatic Tumors Invading the Peripheral Nervous System
Neurosurg Focus 22 (6):E14, 2007 Management of metastatic tumors invading the peripheral nervous system JOHN GACHIANI, M.D.,1 DANIEL H. KIM, M.D.,3 ADRIANE NELSON, M.D.,2 AND DAVID KLINE, M.D.1 Departments of 1Neurosurgery and 2Pathology, Louisiana State University Health Sciences Center; 3Department of Neurosurgery, Ochsner Clinic Foundation, New Orleans, Louisiana Object. The authors present the results of a retrospective review of 37 surgically treated metastases to nerve (malignant peripheral non–neural sheath nerve tumors). Tumor frequencies, presentations, management, and prognosis are discussed. Methods. Thirty-seven patients who were treated for metastases to nerve between 1969 and 2006 at the Louisiana State University Health Sciences Center were identified in a review of patient records. Notes regarding patient history and physical examination findings were reviewed to provide informa- tion on presenting symptoms and signs. Imaging and histopathological examination results were also reviewed. Cases were analyzed depending on the primary tumor and the location of metastasis. Results. There included 37 surgically treated lesions, 16 of which originated in the breast and 10 of which originated in the lung. In two cases melanomas had metastasized to nerve, and one tumor each had metastasized from the bladder, rectum, skin, head and neck, and thyroid, and from a primary Ewing sarcoma. There was a single lymphoma that had metastasized to the radial nerve and one chor- doma and one osteosarcoma, each of which had metastasized to the brachial plexus. Conclusions. The nervous system is involved in numerous ways by oncological process. Direct involvement of the peripheral nervous system occurs mostly from direct extension, although it occa- sionally occurs because of distant spread from the primary tumor to nerve. -

Curative Efficacy of Low Frequency Electrical Stimulation in Preventing
Li et al. World Journal of Surgical Oncology (2019) 17:141 https://doi.org/10.1186/s12957-019-1689-2 RESEARCH Open Access Curative efficacy of low frequency electrical stimulation in preventing urinary retention after cervical cancer operation Huan Li1,2†, Can-Kun Zhou4†, Jing Song1,2, Wei-Ying Zhang1,2, Su-Mei Wang1,2, Yi-Ling Gu1,2, Kang Wang1,2, Zhe Ma1,2, Yan Hu1,2, Ai-Min Xiao1,2, Jian-Liu Wang3 and Rui-Fang Wu1,2* Abstract Background: To evaluate the clinical significance of low-frequency electrical stimulation in preventing urinary retention after radical hysterectomy. Methods: A total of 91 women with stage IA2–IB2 cervical cancer, who were treated with radical hysterectomy and lymphadenectomy from January 2009 to December 2012, were enrolled into this study and were randomly divided into two groups: trail group (48 cases) and control group (43 cases). Traditional bladder function training and low- frequency electrical stimulation were conducted in the trail group, while patients in the control group were only treated by traditional bladder training. The general condition, rate of urinary retention, and muscle strength grades of pelvic floor muscle in the perioperative period were compared between these two groups. Results: The incidence of postoperative urinary retention in the electrical stimulation group was 10.41%, significantly lower than that in the control group (44.18%), and the difference was statistically significant (P < 0.01). The duration of postoperative fever and use of antibiotics were almost the same between these two groups. Eleven days after surgery, the difference in grades of the pelvic floor muscle between these two groups was not statistically significant. -

Unit #2 - Abdomen, Pelvis and Perineum
UNIT #2 - ABDOMEN, PELVIS AND PERINEUM 1 UNIT #2 - ABDOMEN, PELVIS AND PERINEUM Reading Gray’s Anatomy for Students (GAFS), Chapters 4-5 Gray’s Dissection Guide for Human Anatomy (GDGHA), Labs 10-17 Unit #2- Abdomen, Pelvis, and Perineum G08- Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) G09A- Peritoneum, GI System Overview and Foregut (Dr. Albertine) G09B- Arteries, Veins, and Lymphatics of the GI System (Dr. Albertine) G10A- Midgut and Hindgut (Dr. Albertine) G10B- Innervation of the GI Tract and Osteology of the Pelvis (Dr. Albertine) G11- Posterior Abdominal Wall (Dr. Albertine) G12- Gluteal Region, Perineum Related to the Ischioanal Fossa (Dr. Albertine) G13- Urogenital Triangle (Dr. Albertine) G14A- Female Reproductive System (Dr. Albertine) G14B- Male Reproductive System (Dr. Albertine) 2 G08: Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) At the end of this lecture, students should be able to master the following: 1) Overview a) Identify the functions of the anterior abdominal wall b) Describe the boundaries of the anterior abdominal wall 2) Surface Anatomy a) Locate and describe the following surface landmarks: xiphoid process, costal margin, 9th costal cartilage, iliac crest, pubic tubercle, umbilicus 3 3) Planes and Divisions a) Identify and describe the following planes of the abdomen: transpyloric, transumbilical, subcostal, transtu- bercular, and midclavicular b) Describe the 9 zones created by the subcostal, transtubercular, and midclavicular planes c) Describe the 4 quadrants created -
Spinal Nerves and Reflexes
Central Nervous System - Spinal Nerves and Reflexes Chapter 13B Spinal Nerves - Number There are 31 pairs of spinal nerves…a total of 62 nerves. Spinal cord is located in the vertebral canal. Spinal nerves exit vertebral column through intervertebral foramina. Intervertebral foramen Vertebral canal Spinal Nerves Interneuron Sensory neuron Sensory fiber Spinal nerve Motor neuron Motor fiber All spinal nerves are mixed nerves….contain sensory and motor fibers. Spinal Nerves - Supply N V C2–C3 C2 C 3 C3 C4 Spinal nerves go to skin, muscles and some T2 C4 C5 T3 T1 of the internal organs. T4 T2 T5 C5 T3 T T 6 4 T7 T5 T8 Dermatomes: areas of the skin that is T2 T6 T9 T T2 T7 10 connected to a specific spinal nerve. T11 T8 T12 T9 C L1 6 T10 L2 T T L3 1 11 L4 C Myotomes: specific muscles that are C6 L 7 T12 5 L1 supplied by a specific spinal nerve. S4S L 3 2 S2 C8 C8 T L3 L1 1 1 S5 C7 S1 L5 L4 S2 L2 KEY L5 L Spinal cord regions 3 = Cervical = Thoracic S = Lumbar 1 = Sacral L4 ANTERIOR POSTERIOR Spinal Nerves - Branches Spinal nerve Dorsal Dorsal root Dorsal root ganglion ramus Spinal nerve Ventral Dorsal horn ramus Ventral Ventral root horn Rami communicantes After exiting vertebral column, EACH spinal nerve splits into branches, called rami: 1. Dorsal ramus: contains nerves that serve the dorsal portions of the trunk- carry visceral motor, somatic motor, and sensory information to and from the skin and muscles of the back.