Update in Acute and Preventive Treatment of Migraine 偏頭痛之急性
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Comparing the Effect of Venlafaxine and the Combination of Nortriptyline and Propranolol in the Prevention of Migraine
Comparing the Effect of Venlafaxine and the Combination of Nortriptyline and Propranolol in the Prevention of Migraine Arash Mosarrezaii1, Mohammad Reza Amiri Nikpour1, Ata Jabarzadeh2 1Department of Neurology, Imam Khomeini Hospital, Urmia University of Medical Sciences, Urmia, Iran, 2Medical Student, Urmia University of Medical Sciences, Urmia, Iran Abstract Background: Migraine is a debilitating neurological condition, which can be categorized into episodic and chronic groups based on its clinical pattern. Avoiding the risk factors exacerbating migraine is not enough to reduce the frequency and severity of migraine headaches, and in the case of non-receiving proper drug treatment, episodic migraines have the potential to become chronic, which increases the risk of cardiovascular complications RESEARCH ARTICLE and leaves great impact on the quality of life of patients and increasing the health-care costs. The objective of this research was to compare the effects of venlafaxine (VFL) and nortriptyline and propranolol in preventing migraines. Methods: This research is an interventional study performed on 60 patients with migraine admitted to the neurological clinic. Patients were visited at 3 time intervals. In each stage, the variables of headache frequency, headache severity, nausea, vomiting, and drowsiness were recorded. Data were analyzed using SPSS 23 software. Results: VFL drug with a daily dose of 37.5 mg is not only more tolerable in the long term but also leaves better effect in reducing the frequency and severity of headaches compared to the combination of nortriptyline and propranolol. Conclusion: VFL is an appropriate, effective, and tolerable alternative to migraine treatment. Key words: Migraine, nortriptyline, propranolol, venlafaxine INTRODUCTION Patients with CM are less likely to have full-time job than patients with episodic type, and they are at risk of job igraine is known as a common incapacity, anxiety, chronic pain, and depression 2 times neurological disorder and causes more than patients with episodic migraine. -
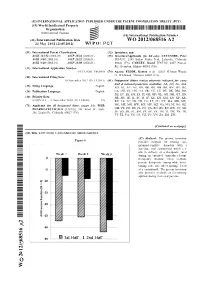
WO 2012/068516 A2 24 May 20 12 (24.05.2012) W P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2012/068516 A2 24 May 20 12 (24.05.2012) W P O P C T (51) International Patent Classification: (72) Inventors; and A61K 31/352 (2006.01) A61P 25/24 (2006.01) (75) Inventors/Applicants (for US only): LETENDRE, Peter A61K 9/48 (2006.01) A61P 25/22 (2006.01) [US/US]; 2389 Indian Peaks Trail, Lafayette, Colorado A61K 9/20 (2006.01) A61P 25/00 (2006.01) 80026 (US). CARLEY, David [US/US]; 2457 Pioneer Rd., Evanston, Illinois 60201 (US). (21) International Application Number: PCT/US201 1/061490 (74) Agents: FEDDE, Kenton et al; 18325 AUenton Woods Ct, Wildwood, Missouri 63069 (US). (22) International Filing Date: 18 November 201 1 (18.1 1.201 1) (81) Designated States (unless otherwise indicated, for every kind of national protection available): AE, AG, AL, AM, (25) Language: English Filing AO, AT, AU, AZ, BA, BB, BG, BH, BR, BW, BY, BZ, (26) Publication Language: English CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, HN, (30) Priority Data: HR, HU, ID, IL, IN, IS, JP, KE, KG, KM, KN, KP, KR, 61/415,33 1 18 November 2010 (18. 11.2010) US KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, (71) Applicant (for all designated States except US): PIER MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, PHARMACEUTICALS [US/US]; 901 Front St., Suite OM, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SC, SD, 201, Louisville, Colorado 80027 (US). -

Current Awareness in Clinical Toxicology Editors: Damian Ballam Msc and Allister Vale MD
Current Awareness in Clinical Toxicology Editors: Damian Ballam MSc and Allister Vale MD January 2017 CONTENTS General Toxicology 11 Metals 38 Management 21 Pesticides 39 Drugs 23 Chemical Warfare 41 Chemical Incidents & 33 Plants 41 Pollution Chemicals 33 Animals 42 CURRENT AWARENESS PAPERS OF THE MONTH 2015 Annual Report of the American Association of Poison Control Centers' National Poison Data System (NPDS): 33rd Annual Report Mowry JB, Spyker DA, Brooks DE, Zimmerman A, Schauben JL. Clin Toxicol 2016; 54: 924-1109. Introduction This is the 33rd Annual Report of the American Association of Poison Control Centers' (AAPCC) National Poison Data System (NPDS). As of 1 January 2015, 55 of the nation's poison centers (PCs) uploaded case data automatically to NPDS. The upload interval was 9.52 [7.40, 13.6] (median [25%, 75%]) minutes, creating a near real-time national exposure and information database and surveillance system. Methods We analyzed the case data tabulating specific indices from NPDS. The methodology was similar to that of previous years. Where changes were introduced, the differences are identified. Poison center cases with medical outcomes of death were evaluated by a team of medical and clinical toxicologist reviewers using an ordinal scale of 1-6 to assess the Relative Contribution to Fatality (RCF) of the exposure. Results In 2015, 2,792,130 closed encounters were logged by NPDS: 2,168,371 human exposures, 55,516 animal exposures, 560,467 information calls, 7657 human confirmed nonexposures, Current Awareness in Clinical Toxicology is produced monthly for the American Academy of Clinical Toxicology by the Birmingham Unit of the UK National Poisons Information Service, with contributions from the Cardiff, Edinburgh, and Newcastle Units. -

French Guidelines for the Diagnosis and Management of Migraine in Adults and Children
French Guidelines for the Diagnosis and Management of Migraine in Adults and Children Gilles Gkraud, MD,l Michel Lank-i-Minet, MD,’ Christian Lucas, MD,3 and Dominique Valade, MD,4 on behalf of the French Society for the Study of Migraine Headache (SFEMC) lDepartment of Neurology, Rangueil Hospital, Toulouse, 2Pain Centel; Pasteur Hospital, Nice, 3Depurtment of Neurology, Sulengro Hospital, Lille, and 4Heuduche Emergency Centel; Lur-iboisi&e Hospital, Paris, France ABSTRACT Background: The French Recommendations for Clinical Practice: Diagnosis and Therapy of Migraine are guidelines concerning the overall management of patients with migraine, including diagnostic and therapeutic strategies and assessment of disability Objective: This article summarizes the guidelines as they apply to adults and children, and proposes future direction for steps toward optimal treatment of migraine in patients in France. Methods: The recommendations were categorized into 3 levels of proof (A-C) according to the National Agency for Accreditation and Evaluation in Health (ANAES) methodology and were based on a professional consensus reached among members of the Working Group and the Guidelines Review Group of the ANAES. Results: The International Headache Society diagnostic criteria for migraine should be used in routine clinical practice. Recommended agents for the treatment of migraine in adults include nonsteroidal anti-inflammatory drugs, acetylsalicylic acid (ASA) monotherapy or in combination with metoclopramide, acetaminophen monotherapy, triptans, ergotamine tartrate, and dihydroergotamine mesylate. Patients should use the medication as early as possible after the onset of migraine headache. For migraine prophylaxis in adults, the following can be used: propranolol, metoprolol, oxetorone, or amitriptyline as first-line treatment, and pizotifen, flunarizine, valproate sodium, or topiramate as second-line treatment. -

BMJ Open Is Committed to Open Peer Review. As Part of This Commitment We Make the Peer Review History of Every Article We Publish Publicly Available
BMJ Open is committed to open peer review. As part of this commitment we make the peer review history of every article we publish publicly available. When an article is published we post the peer reviewers’ comments and the authors’ responses online. We also post the versions of the paper that were used during peer review. These are the versions that the peer review comments apply to. The versions of the paper that follow are the versions that were submitted during the peer review process. They are not the versions of record or the final published versions. They should not be cited or distributed as the published version of this manuscript. BMJ Open is an open access journal and the full, final, typeset and author-corrected version of record of the manuscript is available on our site with no access controls, subscription charges or pay-per-view fees (http://bmjopen.bmj.com). If you have any questions on BMJ Open’s open peer review process please email [email protected] BMJ Open Pediatric drug utilization in the Western Pacific region: Australia, Japan, South Korea, Hong Kong and Taiwan Journal: BMJ Open ManuscriptFor ID peerbmjopen-2019-032426 review only Article Type: Research Date Submitted by the 27-Jun-2019 Author: Complete List of Authors: Brauer, Ruth; University College London, Research Department of Practice and Policy, School of Pharmacy Wong, Ian; University College London, Research Department of Practice and Policy, School of Pharmacy; University of Hong Kong, Centre for Safe Medication Practice and Research, Department -

The Organic Chemistry of Drug Synthesis
THE ORGANIC CHEMISTRY OF DRUG SYNTHESIS VOLUME 3 DANIEL LEDNICER Analytical Bio-Chemistry Laboratories, Inc. Columbia, Missouri LESTER A. MITSCHER The University of Kansas School of Pharmacy Department of Medicinal Chemistry Lawrence, Kansas A WILEY-INTERSCIENCE PUBLICATION JOHN WILEY AND SONS New York • Chlchester • Brisbane * Toronto • Singapore Copyright © 1984 by John Wiley & Sons, Inc. All rights reserved. Published simultaneously in Canada. Reproduction or translation of any part of this work beyond that permitted by Section 107 or 108 of the 1976 United States Copyright Act without the permission of the copyright owner is unlawful. Requests for permission or further information should be addressed to the Permissions Department, John Wiley & Sons, Inc. Library of Congress Cataloging In Publication Data: (Revised for volume 3) Lednicer, Daniel, 1929- The organic chemistry of drug synthesis. "A Wiley-lnterscience publication." Includes bibliographical references and index. 1. Chemistry, Pharmaceutical. 2. Drugs. 3. Chemistry, Organic—Synthesis. I. Mitscher, Lester A., joint author. II. Title. [DNLM 1. Chemistry, Organic. 2. Chemistry, Pharmaceutical. 3. Drugs—Chemical synthesis. QV 744 L473o 1977] RS403.L38 615M9 76-28387 ISBN 0-471-09250-9 (v. 3) Printed in the United States of America 10 907654321 With great pleasure we dedicate this book, too, to our wives, Beryle and Betty. The great tragedy of Science is the slaying of a beautiful hypothesis by an ugly fact. Thomas H. Huxley, "Biogenesis and Abiogenisis" Preface Ihe first volume in this series represented the launching of a trial balloon on the part of the authors. In the first place, wo were not entirely convinced that contemporary medicinal (hemistry could in fact be organized coherently on the basis of organic chemistry. -

(12) United States Patent (10) Patent No.: US 8.242,110 B2 Deregnaucourt Et Al
USOO824211 OB2 (12) United States Patent (10) Patent No.: US 8.242,110 B2 Deregnaucourt et al. (45) Date of Patent: Aug. 14, 2012 (54) USE OF ANTIHISTAMINEAGENTS FOR THE FOREIGN PATENT DOCUMENTS PREVENTIVE OR EARLY TREATMENT OF FR 2802 101 A1 6, 2001 INFLAMMATORY SYNDROMES, IN JP 4-89428 A 3, 1992 PARTICULAR THOSE TRIGGERED BY JP 2001-151677 A 6, 2001 TOGAVIRUSES WO WO-96,04787 A1 2, 1996 (75) Inventors: Jean Deregnaucourt, Paris (FR): OTHER PUBLICATIONS Etienne Andre, Seyssinet-Pariset (FR): Wilson, Annals of Rheumatic Diseases, 1953; 12(1):38-39.* Jacky Tisne-Versailles, Castres (FR) Storms, Journal of Allergy and Clinical Immunology, 2004; 114:S146-153.* (73) Assignee: Pierre Fabre Medicament, Satake et al., Journal of Cardiovascular Pharmacology, Boulogne-Billancourt (FR) 1994:23(4):669-673 (abstract only).* Toovey et al., Travel Medicine and Infectious Disease, vol.2, No. 3-4, (*) Notice: Subject to any disclaimer, the term of this 2004, pp. 189-191. patent is extended or adjusted under 35 Suhrbier et al., Current Opinion in Rheumatology, vol. 16, No. 4. U.S.C. 154(b) by 809 days. 2004, pp. 374-379. Stocks et al., Australian Family Physician, vol. 26, No. 6, Jun. 1997. (21) Appl. No.: 12/224,830 pp. 710-717. Paganin et al., Presse Medicale 2006, vol. 35. No. 4 II, 2006, pp. (22) PCT Filed: Mar. 9, 2007 641-646. Ware et al., Medical Care, vol. 34, No. 3, 1996, pp. 220-233. (86). PCT No.: PCT/EP2007/052237 Bruce et al., The Journal of Rheumatology, vol. 30, No. 1, 2003, pp. -

Oxetorone Fumarate
624 Antimigraine Drugs Adverse Effects and Precautions otifen had a similar chemical structure to the tricyclic antidepres- As for Sumatriptan, p.625. sants it might antagonise the actions of adrenergic neurone O blockers in a similar manner. Naratriptan should not be used in patients with severe 1. Bailey RR. Antagonism of debrisoquine sulphate by pizotifen hepatic or renal impairment (creatinine clearance less (Sandomigran). N Z Med J 1976; 1: 449. than 15 mL/minute) and should be used with caution in mild or moderate renal or hepatic impairment. Patients O Pharmacokinetics with hypersensitivity to sulfonamides may theoretical- CHCH2CH2N(CH3)2 Pizotifen is well absorbed from the gastrointestinal ly exhibit a similar reaction to naratriptan. tract, peak plasma concentrations occurring about 5 (oxetorone) hours after a single oral dose. Over 90% is bound to Medication-overuse headache. For a report of an associa- plasma proteins. Pizotifen undergoes extensive metab- tion between naratriptan and medication-overuse headache, see Profile olism. Over half of a dose is excreted in the urine, under Adverse Effects of Sumatriptan, p.626. Oxetorone fumarate is an antihistamine and serotonin antagonist chiefly as metabolites; a significant proportion is ex- used orally in the treatment of migraine (p.616) and cluster head- creted in the faeces. The primary metabolite of pizo- Interactions ache (p.616) in doses of up to 180 mg daily. Oxetorone was re- As for Sumatriptan, p.626. ported to have induced hyperplastic changes in breast tissue and tifen (N-glucuronide conjugate) has a long elimination the uterine endometrium of rodents. half-life of about 23 hours. -

Microsoft Word
AUTORISES INTERDITS AC. ACETYLSALICYLIQUE AC. MEFENAMIQUE AC. CLAVULANIQUE AC. NALIDIXIQUE AC. FUSIDIQUE AC. PIPEMIDIQUE AC. NIFLUMIQUE AC. PIROMIDIQUE AC. OXOLINIQUE ACITRETINE AC. TIAPROFENIQUE ADRAFINIL AC. TIENILIQUE ALCOOL AC. TRANEXAMIQUE ALIZAPRIDE ACAMPROSATE ALLOPURINOL ACEBUTOLOL ALMINOPROFENE ACETAZOLAMIDE ALPRAZOLAM ACICLOVIR ALVERINE ACTH AMBROXOL ADRENALINE AMIDOPYRINE ALFENTANIL AMINEPTINE ALFUZOSINE AMINOGLUTHETIMIDE ALIMEMAZINE AMIODARONE AMANTADINE AMISULPRIDE AMFEPRAMONE AMOBARBITAL AMIKACINE ANDROGENES AMILORIDE ARTICAINE AMITRIPTYLINE ASTEMIZOLE AMLODIPINE BACLOFENE AMOXAPINE BARBITURIQUES AMOXICILLINE BENFLUOREX AMPHOTERICINE B BENZBROMARONE APTOCAINE BENZYL THIOURACILE ATENOLOL BEPRIDIL ATRACURIUM BETAHISTINE ATROPINE BIPERIDENE AZATHIOPRINE BISOPROLOL BENAZEPRIL BROMOCRIPTINE BENSERAZIDE BUPIVACAINE (*) BETA-ALANINE BUSPIRONE BETAXOLOL CAPTOPRIL BEZAFIBRATE CARBAMAZEPINE BLEOMYCINE CEFACLOR BROMAZEPAM CEFPODOXIME BROMURE CEFUROXIME BUFLOMEDIL CHLORAMPHENICOL BUPRENORPHINE CHLORMEZANONE BUTACAINE CHLOROQUINE (*) BUTYLHYOSCINE CIBENZOLINE CARBIMAZOLE CICLETANINE CARPIPRAMINE CIPROFIBRATE CEFIXIME CLINDAMYCINE CEFOTAXIME CLOBAZAM CEFTAZIDIME CLOFIBRATE CEFTRIAXONE CLOMETHIAZOLE CELIPROLOL CLOMIFENE CERIVASTATINE CLONIDINE CETIRIZINE CLORAZEPATE CHLORAL HYDRATE CLOTIAZEPAM CHLORDIAZEPOXIDE CYCLOPHOSPHAM 1 DE CHLORPROMAZINE CYPROTERONE CICLOSPORINE DANAZOL CILAZAPRIL DAPSONE CIMETIDINE DENORAL® CIPROFLOXACINE DEXFENFLURAMINE CISAPRIDE DEXTROMORAMIDE CITALOPRAM DEXTROPROPOXYPHENE CLARITHROMYCINE DIAZEPAM CLIDINIUM DIHYDRALAZINE -

Drugs to Avoid in 2017
OUTLOOK 2017 Update A more recent version is available online at english.prescrire.org Use the “Search” function with keywords “drugs to avoid (Prescrire's annual review)” Towards better patient care: drugs to avoid in 2017 ABSTRACT harm-benefit balance, and the trial design must be relevant. Tailored supportive care is the best ● To help healthcare professionals and patients option when there are no available treatments choose high-quality treatments that minimise the capable of improving prognosis or quality of life, risk of adverse effects, in early 2017 we updated beyond their placebo effect. the list of drugs that Prescrire advises health pro- Rev Prescrire 2017; 37 (400): 137-148 fessionals and patients to avoid. ● Prescrire’s assessments of the harm-benefit bal- ance of new drugs and indications are based on a his is Prescrire’s fifth consecutive annual rigorous procedure that includes a systematic and review of “drugs to avoid” (1,2). The drugs reproducible literature search, identification of Tlisted here are clearly more dangerous than patient-relevant outcomes, prioritisation of the sup- beneficial and should therefore not be used. The porting data based on the strength of evidence, aim is to help health professionals choose safe, comparison with standard treatments, and an anal- effective treatments and thereby avoid harming ysis of both known and potential adverse effects. their patients. ● This fifth annual review of drugs to avoid has been extended to cover all drugs examined by A reliable, rigorous and independent Prescr ire between 2010 and 2016 and authorised methodology in the European Union, whereas previous reviews only considered drugs marketed in France. -

Council of Europe Committee of Ministers (Partial
COUNCIL OF EUROPE COMMITTEE OF MINISTERS (PARTIAL AGREEMENT IN THE SOCIAL AND PUBLIC HEALTH FIELD) RESOLUTION AP (82) 2 ON THE CLASSIFICATION OF MEDICINES WHICH ARE OBTAINABLE ONLY ON MEDICAL PRESCRIPTION (Adopted by the Committee of Ministers on 2 June 1982 at the 348th meeting of the Ministers' Deputies and superseding Resolution AP (77) 1) AND APPENDIX containing the list of medicines adopted by the Public Health Committee (Partial Agreement) updated to 31 October 1982 RESOLUTION AP (82) 2 ON THE CLASSIFICATION OF MEDICINES WHICH ARE OBTAINABLE ONLY ON MEDICAL PRESCRIPTION 1 (Adopted by the Committee of Ministers on 2 June 1982 at the 348th meeting of the Ministers' Deputies) The Representatives on the Committee of Ministers of Belgium, France, the Federal Republic of Germany, Italy, Luxembourg, the Netherlands, the United Kingdom of Great Britain and Northern Ireland, these states being parties to the Partial Agreement in the social and public health field, and the Representatives of Austria, Denmark, Ireland and Switzerland, states which have participated in the public health activities carried out within the above-mentioned Partial Agreement since 1 October 1974, 2 April 1968, 23 September 1969 and 5 May 1964, respectively, Considering that, under the terms of its Statute, the aim of the Council of Europe is to achieve a greater unity between its Members for the purpose of safeguarding and realising the ideals and principles which are their common heritage and facilitating their economic and social progress; Having regard to the -

WO 2012/107573 Al 16 August 2012 (16.08.2012) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2012/107573 Al 16 August 2012 (16.08.2012) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 9/00 (2006.01) A61K 47/14 (2006.01) kind of national protection available): AE, AG, AL, AM, A61K 47/06 (2006.0V) A61K 9/70 (2006.01) AO, AT, AU, AZ, BA, BB, BG, BH, BR, BW, BY, BZ, A61 47/10 (2006.0V) CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, HN, (21) Number: International Application HR, HU, ID, IL, IN, IS, JP, KE, KG, KM, KN, KP, KR, PCT/EP2012/052337 KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, (22) International Filing Date: MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, 10 February 2012 (10.02.2012) OM, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, (25) Filing Language: English TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, ZW. (26) Publication Language: English (84) Designated States (unless otherwise indicated, for every (30) Priority Data: kind of regional protection available): ARIPO (BW, GH, 61/441,346 10 February 201 1 (10.02.201 1) US GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, MD, RU, (71) Applicant (for all designated States except US): Moberg TJ, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, Derma AB [SE/SE]; Gustavslundsvagen 42, 5 tr, S-167 51 DK, EE, ES, FI, FR, GB, GR, HR, HU, IE, IS, IT, LT, LU, Bromma (SE).