Where Is the True Location of the Femoral Piriform Fossa?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Entry Point Related Outcome in Antegrade Femoral Nailing Experimental and Clinical Studies
C.M.S. Moein Ansari experimental and clinical studies clinical and experimental Entry Point Related Outcome Outcome Related Point Entry in Antegrade Femoral Nailing Femoral Antegrade in Entry Point Related Outcome in Antegrade Femoral Nailing experimental and clinical studies C.M.S. Ansari Moein Entry Point Related Outcome in Antegrade Femoral Nailing experimental and clinical studies C.M.S. Ansari Moein ENTRY POINT RELATED OUTCOME IN ANTEGRADE FEMORAL NAILING Experimental and clinical studies C.M.S. Ansari Moein The Robert Mathys Foundation, Bettlach, Switzerland and the AO Foundation, Davos, Switzerland financially supported the studies presented in this thesis. Kind contribution for the publication of this thesis by: Erasmus Medical Centre Dept. of Surgery Trauma Research Unit Erasmus MC (TRUE) Parnassia Academy ABN AMRO Bank PsyQ Maatschap Plastische Chirurgie Midden Brabant THP Financial Guidance Post Notariaat Cover illustration by Rob Veen Printing and lay-out by Optima Grafische Communicatie, Rotterdam, The Netherlands ISBN 978-94-6169-867-4 © 2016. Copyright by CMS Ansari Moein Entry Point Related Outcome in Antegrade Femoral Nailing experimental and clinical studies Entreeplaats gerelateerde uitkomst van antegrade mergpen ostheosynthese bij femurfracturen experimentele en klinische studies Proefschrift ter verkrijging van de graad van doctor aan de Erasmus Universiteit Rotterdam op gezag van de rector magnificus Prof. Dr. H.A.P. Pols en volgens besluit van het College voor Promoties De openbare verdediging zal plaatsvinden op vrijdag 20 mei 2016 om 13.30 uur door Chloé Mahsima Ansari Moein geboren te Tehran, Iran Promotiecommissie promotoren: Prof. dr. M.H.J. Verhofstad Prof. dr. H.J. Ten Duis overige leden: Prof. -

A New Caenagnathid Dinosaur from the Upper Cretaceous Wangshi
www.nature.com/scientificreports OPEN A new caenagnathid dinosaur from the Upper Cretaceous Wangshi Group of Shandong, China, with Received: 12 October 2017 Accepted: 7 March 2018 comments on size variation among Published: xx xx xxxx oviraptorosaurs Yilun Yu1, Kebai Wang2, Shuqing Chen2, Corwin Sullivan3,4, Shuo Wang 5,6, Peiye Wang2 & Xing Xu7 The bone-beds of the Upper Cretaceous Wangshi Group in Zhucheng, Shandong, China are rich in fossil remains of the gigantic hadrosaurid Shantungosaurus. Here we report a new oviraptorosaur, Anomalipes zhaoi gen. et sp. nov., based on a recently collected specimen comprising a partial left hindlimb from the Kugou Locality in Zhucheng. This specimen’s systematic position was assessed by three numerical cladistic analyses based on recently published theropod phylogenetic datasets, with the inclusion of several new characters. Anomalipes zhaoi difers from other known caenagnathids in having a unique combination of features: femoral head anteroposteriorly narrow and with signifcant posterior orientation; accessory trochanter low and confuent with lesser trochanter; lateral ridge present on femoral lateral surface; weak fourth trochanter present; metatarsal III with triangular proximal articular surface, prominent anterior fange near proximal end, highly asymmetrical hemicondyles, and longitudinal groove on distal articular surface; and ungual of pedal digit II with lateral collateral groove deeper and more dorsally located than medial groove. The holotype of Anomalipes zhaoi is smaller than is typical for Caenagnathidae but larger than is typical for the other major oviraptorosaurian subclade, Oviraptoridae. Size comparisons among oviraptorisaurians show that the Caenagnathidae vary much more widely in size than the Oviraptoridae. Oviraptorosauria is a clade of maniraptoran theropod dinosaurs characterized by a short, high skull, long neck and short tail. -

Percutaneous Reduction Techniques
AAOS 2016 Specialty Day Orthopaedic Trauma Associacion (OTA) Percutaneous Reduction Techniques Christian Krettek Trauma Department, Hannover Medical School, Germany [email protected] www.mhh-unfallchirurgie.de Short segment tibial fractures can be stabilized using different implants like plates, screws, external fixators and nails. This syllabus deals mainly with reduction techniques in the context of the use of intramedullary nails. 1.1 PREOPERATIVE PLANNING AND MANAGEMENT 1.1.1 Primary shortening and secondary overdistraction eases definitive nailing In the acute setting primary shortening of a shaft fracture is a helpful strategy to de- crease soft tissue tension and intra-compartmental pressure. However, reduction gets more difficult and more time consuming, the longer the fracture is kept in a shortened position. The concept of primary shortening (acute phase) and secondary (after 3 or 4 days) overdistraction eases definitive nailing. Using a electro-mechanical load cell, our group has compared the reduction forces in patients undergoing femoral nailing after Damage Control in shortend vs overdistracted fracture configuration. In the overdistrac- tion group, the reduction forces were lower (200 N +/-43.1 N vs. 336 N +/- 51.9 N, p = 0.007) and the reduction time was shorter (5.8 min +/-4.0 min vs. 28.3 min +/-21.8 min, p = 0.056). It was concluded, that DCO with the fracture shortened leads to higher restrai- ning forces & prolonged reduction time. Overdistraction should be performed as soon as possible under careful soft-tissue monitoring [1a, 2a]. Primary shortening and secondary overdistraction eases definitive nailing Example of a femoral shaft fracture stabilized in shortening first with an external fixator. -

Congenital Abnormalities of the Femur
Arch Dis Child: first published as 10.1136/adc.36.188.410 on 1 August 1961. Downloaded from CONGENITAL ABNORMALITIES OF THE FEMUR BY P. A. RING From the Royal College of Surgeons (RECEIVED FOR PUBLICATION NOVEMBER 25, 1960) Congenital defects of the femur vary from simple tion of its incidence is difficult to obtain, but it hypoplasia of the bone to complete absence. appears to be the commonest congenital defect Classification of these defects has been suggested causing major abnormalities of limb growth. by Nilsonne (1928) and by Mouchet and Ibos (1928), but neither has met with general acceptance. In more recent years Golding (1939, 1948) has demon- Clinical Features strated the close association of the short femur with There is no evidence that this is a familial disorder, congenital coxa vara, and has emphasized that and careful inquiry of the parents has revealed no these are variations of the same underlying abnor- evidence of other congenital disorders within the mality. The clinical distinction between the various immediate family. The history of the pregnancy types of femoral defect is important as a guide to and delivery has failed to indicate any significant the prognosis of limb development. infection or abnormality at this time. In most From an examination of patients with congenital patients the abnormality is apparent at birth, but abnormalities of the femur the following classifica- where the inequality of leg length is slight, the by copyright. tion is suggested: diagnosis may not be made until the child begins to 1. Simple femoral hypoplasia. walk. To ordinary clinical testing the abnormality 2. -

Periprosthetic Fractures
Periprosthetic Fractures SRS 2017 Stephen R Smith Orthopaedic Surgeon Northeast Nebraska Orthopaedics P C Norfolk Nebraska SRS 2017 Periprosthetic Fractures Fractures around Joint Replacements Mostly Lower Limb Knee Arthroplasty 700,000/ yr. Hip Arthroplasty 350,000/yr. Shoulder Arthroplasty ? 60,000/yr. Elbow Arthroplasty ? 20,000/yr. Periprosthetic Fractures Incidence Increasing due Increasing Demand and High Demands of Older Patients Projections 2025 2,000,000 (2 million) Knee Replacements 750,000 Total Hip Replacements Periprosthetic Fractures Risk Factors Mechanical Patient Factors Implant Loosening Rheumatoid Arthritis Chronic Steroid Use Neurologic Osteolysis Disease/Disorders Osteoporosis Osteopenia Femoral Notching Female Gender (Above TKA) Increasing Age SRS 2017 Periprosthetic Fractures Incidence Hip Intraoperative Acetabulum Cemented 0.2% Uncemented 0.4% During Impaction Under reaming> 2mm, Osteoporosis, Dysplasia Radiation Periprosthetic Fractures Incidence Hip Intraoperative Primary 0.1-5% Classification Osteoporosis,Cementless, Technique, Revision, Minimally Invasive, Revision 3-21% Periprosthetic Fractures Risk Factors DON’T FALL Remove Loose Rugs Minimize Stair Use Rail Stay Home in Bad Weather!!! Use Common Sense SRS 2017 Periprosthetic Fractures Risk Factors This Is Ice DON’T FALL Remove Loose Rugs Minimize Stair Use Rail Stay Home in Bad Weather!!! Use Common Sense SRS 2017 Periprosthetic Fractures Incidence Knee Intraoperative ?? Occasional Medial Femoral Condyle Often Tibial Crack after Stem Impaction Postoperative -

Clinical Anatomy of the Lower Extremity
Государственное бюджетное образовательное учреждение высшего профессионального образования «Иркутский государственный медицинский университет» Министерства здравоохранения Российской Федерации Department of Operative Surgery and Topographic Anatomy Clinical anatomy of the lower extremity Teaching aid Иркутск ИГМУ 2016 УДК [617.58 + 611.728](075.8) ББК 54.578.4я73. К 49 Recommended by faculty methodological council of medical department of SBEI HE ISMU The Ministry of Health of The Russian Federation as a training manual for independent work of foreign students from medical faculty, faculty of pediatrics, faculty of dentistry, protocol № 01.02.2016. Authors: G.I. Songolov - associate professor, Head of Department of Operative Surgery and Topographic Anatomy, PhD, MD SBEI HE ISMU The Ministry of Health of The Russian Federation. O. P.Galeeva - associate professor of Department of Operative Surgery and Topographic Anatomy, MD, PhD SBEI HE ISMU The Ministry of Health of The Russian Federation. A.A. Yudin - assistant of department of Operative Surgery and Topographic Anatomy SBEI HE ISMU The Ministry of Health of The Russian Federation. S. N. Redkov – assistant of department of Operative Surgery and Topographic Anatomy SBEI HE ISMU THE Ministry of Health of The Russian Federation. Reviewers: E.V. Gvildis - head of department of foreign languages with the course of the Latin and Russian as foreign languages of SBEI HE ISMU The Ministry of Health of The Russian Federation, PhD, L.V. Sorokina - associate Professor of Department of Anesthesiology and Reanimation at ISMU, PhD, MD Songolov G.I K49 Clinical anatomy of lower extremity: teaching aid / Songolov G.I, Galeeva O.P, Redkov S.N, Yudin, A.A.; State budget educational institution of higher education of the Ministry of Health and Social Development of the Russian Federation; "Irkutsk State Medical University" of the Ministry of Health and Social Development of the Russian Federation Irkutsk ISMU, 2016, 45 p. -

Fracture of the Lesser Trochanter As a Sign of Undiagnosed Tumor Disease in Adults Christian Herren*, Christian D
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Springer - Publisher Connector Herren et al. Eur J Med Res (2015) 20:72 DOI 10.1186/s40001-015-0167-8 CASE REPORT Open Access Fracture of the lesser trochanter as a sign of undiagnosed tumor disease in adults Christian Herren*, Christian D. Weber, Miguel Pishnamaz, Thomas Dienstknecht, Philipp Kobbe, Frank Hildebrand and Hans‑Christoph Pape Abstract Isolated avulsion fractures of the pelvic ring are rare and occur predominantly in adolescent athletes. Isolated fractures of the lesser trochanter are reported to be pathognomic for tumor diseases in adults. We present a case of a female patient with an isolated avulsion of the lesser trochanter after treatment by her chiropractor. After staging exami‑ nation, we determine the diagnosis of a left-sided carcinoma of the mamma. Additional imaging shows multiple metastases in liver, spine and pelvis. Palliative therapy has started over the course of time. We suggest, on suspicion of a malignant metastatic process, further investigation. Keywords: Fracture, Lesser trochanter, Metastatic, Tumor disease Background described unexplained weight loss of 5 kg in 4 months. Isolated fractures of the lesser trochanter are uncommon Sporadic onset of night sweats was also reported. She had and have been reported predominantly in adolescent ath- no other musculoskeletal or constitutional diseases in her letes [1]. This injury is caused by severe impact, usually medical history. Physical examination showed tenderness in context of contact sports and following a forceful and in the right groin, almost preserved passive mobility of sudden muscle contraction of the iliopsoas with avulsion the right hip joint in the full range of motion. -
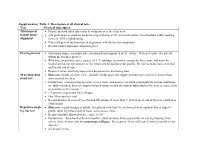
Supplementary Table 1: Description of All Clinical Tests Test Protocol
Supplementary Table 1: Description of all clinical tests Test Protocol description Tibiofemoral • Palpate & mark tibial tuberosity & midpoint over the talus neck frontal plane • Ask participant to stand on footprint map with foot at 10° external rotation, feet shoulder width, looking alignment forward, 50% weightbearing • Place callipers of inclinometer in alignment with the the two landmarks • Record varus/valgus direction in degrees Herrington test • Participant supine on plinth, knee positioned and supported in 20° of knee flexion (to place the patella within the trochlea groove) • With knee in position, place a piece of 1” Leukotape (or similar) across the knee joint, and mark the medial and lateral epicondyles of the femur and mid-point of the patella. Be sure to make note of medial and lateral end of tape • Repeat 3 times, attaching tape to this document for measuring later 30 second chair • Shoes on, middle of chair, feet ~ shoulder width apart and slightly behind knees with feet flat on floor, stand test arms crossed on chest • Instructions “stand up keeping arms across chest, and ensure you stand completely up so hips and knees are fully extended; then sit completely back down, so that the bottom fully touches the seat, as many times as possible in 30 seconds,” • 1-2 practice repetitions for technique • One 30-second test trial • Record number of correctly performed full stands (if more than ½ of way up at end of the test, counted as a full stand) Repetitive single • Shoes on, seated on edge of plinth, foot placed with heel 10 cm forward from a plumb line at edge of leg rise test plinth, other leg held at side of body, arms across chest. -

Endoscopic Repair of Full-Thickness Gluteus Medius Tears Benjamin G
Endoscopic Repair of Full-Thickness Gluteus Medius Tears Benjamin G. Domb, M.D., and Dominic S. Carreira, M.D. Abstract: Tears in the gluteus medius and minimus tendons recently have emerged as an important cause of chronic greater trochanteric pain syndrome. Increasing recognition of the gluteal insertion as a cause of chronic pain and weakness, as well as technologic advances in endoscopic hip surgery, has made gluteal insertional repair a rapidly emerging technique in minimally invasive surgery of the hip. We present an endoscopic double-row technique for gluteal insertional repair that allows for visualization, debridement, and repair, re-creating the normal footprint. ears in the gluteus medius and minimus tendons most patients respond favorably.7 A survey of French Trecently have emerged as an important cause of surgeons reporting the results of open repairs in 29 chronic greater trochanteric pain syndrome. Histori- patients showed 12 excellent results, 6 good outcomes, cally, pain over the greater trochanter was presumed and 11 poor outcomes.9 Endoscopic techniques have solely to be due to bursitis, but several studies have included gluteal debridement or repairs, bursectomy, challenged this and shown gluteus tears as a source of and iliotibial band release.10 Voos et al.11 described pain.1 Degenerative tears occur more often than acute a technique of endoscopic repair of the gluteal insertion tears,2,3 and gluteus medius tears occur more often with complete relief of symptoms in 10 patients. The than gluteus minimus tears.4,5 Tears at the insertion of advantages and limitations of endoscopic repair of the the gluteus medius can be intrasubstance, partial, or gluteus medius are described in Table 1. -

Thigh Muscles
Lecture 14 THIGH MUSCLES ANTERIOR and Medial COMPARTMENT BY Dr Farooq Khan Aurakzai PMC Dated: 03.08.2021 INTRODUCTION What are the muscle compartments? The limbs can be divided into segments. If these segments are cut transversely, it is apparent that they are divided into multiple sections. These are called fascial compartments, and are formed by tough connective tissue septa. Compartments are groupings of muscles, nerves, and blood vessels in your arms and legs. INTRODUCTION to the thigh Muscles The musculature of the thigh can be split into three sections by intermuscular septas in to; Anterior compartment Medial compartment and Posterior compartment. Each compartment has a distinct innervation and function. • The Anterior compartment muscle are the flexors of hip and extensors of knee. • The Medial compartment muscle are adductors of thigh. • The Posterior compartment muscle are extensor of hip and flexors of knee. Anterior Muscles of thigh The muscles in the anterior compartment of the thigh are innervated by the femoral nerve (L2-L4), and as a general rule, act to extend the leg at the knee joint. There are three major muscles in the anterior thigh –: • The pectineus, • Sartorius and • Quadriceps femoris. In addition to these, the end of the iliopsoas muscle passes into the anterior compartment. ANTERIOR COMPARTMENT MUSCLE 1. SARTORIUS Is a long strap like and the most superficial muscle of the thigh descends obliquely Is making one of the tendon of Pes anserinus . In the upper 1/3 of the thigh the med margin of it makes the lat margin of Femoral triangle. Origin: Anterior superior iliac spine. -
Bones of the Lower Limb Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Bones of the Lower Limb Doctors Notes Notes/Extra explanation Editing File Objectives Classify the bones of the three regions of the lower limb (thigh, leg and foot). Memorize the main features of the – Bones of the thigh (femur & patella) – Bones of the leg (tibia & Fibula) – Bones of the foot (tarsals, metatarsals and phalanges) Recognize the side of the bone. ﻻ تنصدمون من عدد ال رشائح نصها رشح زائد وملخصات واسئلة Some pictures in the original slides have been replaced with other pictures which are more clear BUT they have the same information and labels. Terminology (Team 434) شيء مرتفع /Eminence a small projection or bump Terminology (Team 434) Bones of thigh (Femur and Patella) Femur o Articulates (joins): (1) above with Acetabulum of hip bone to form the hip joint, (2) below with tibia and patella to form the knee joint. Body of femur (shaft) o Femur consists of: I. Upper end. II. Shaft. III. Lower end. Note: All long bones consist of three things: 1- upper/proximal end posterior 2- shaft anterior 3- lower/distal end I. Upper End of Femur The upper end contains: A. Head B. Neck C. Greater trochanter & D. Lesser trochanter A. Head: o Articulates (joins) with acetabulum of hip bone to form the hip joint. o Has a depression in the center called Fovea Capitis. o The fovea capitis is for the attachment of ligament of the head of Femur. o An artery called Obturator Artery passes along this ligament to supply head of Femur. B. Neck: o Connects head to the shaft. -
The Greater Trochanter Triangle
Occasional piece Br J Sports Med: first published as 10.1136/bjsm.2007.042325 on 19 November 2008. Downloaded from The greater trochanter triangle; a pathoanatomic approach to the diagnosis of chronic, proximal, lateral, lower pain in athletes E C Falvey,1 A Franklyn-Miller,1 P R McCrory2 1 Centre for Health, Exercise and ABSTRACT THE GREATER TROCHANTER TRIANGLE Sports Medicine, School of Chronic pain experienced in the proximal, lateral, lower The specific anatomical landmarks and borders of Physiotherapy, Faculty of Medicine, Dentistry and Health limb may arise from the femoro-acetabular joint, from the the greater trochanter triangle are set out in fig 1. Sciences The University of muscles and tendons that act upon it, from any of the Melbourne, Victoria 3010 structures that traverse the area, and from more remote Australia and Olympic Park structures such as the lumbar spine. Sports Medicine Centre, The aetiology of pathology in this area is not confined to Olympic Boulevard, Melbourne 3004, Australia; 2 Centre for either trauma or overuse. As a result many different Health, Exercise and Sports sporting activities may have a causal role. Medicine University of Without a clear clinical/pathological diagnosis, the Melbourne, Australia subsequent management of chronic groin pain is difficult. Correspondence to: The combination of complex anatomy, variability of Eanna C Falvey, Centre for presentation and the non-specific nature of the signs and Health, Exercise and Sports symptoms makes the diagnostic process problematic. Medicine, School of Physiotherapy, Faculty of The paper proposes a novel educational model based on Medicine, Dentistry and Health pathoanatomic concepts.