Keycard M11 21 22.Qxd
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Elbow Checklist
Workbook Musculoskeletal Ultrasound September 26, 2013 Shoulder Checklist Long biceps tendon Patient position: Facing the examiner Shoulder in slight medial rotation; elbow in flexion and supination Plane/ region: Transverse (axial): from a) intraarticular portion to b) myotendinous junction (at level of the pectoralis major tendon). What you will see: Long head of the biceps tendon Supraspinatus tendon Transverse humeral ligament Subscapularis tendon Lesser tuberosity Greater tuberosity Short head of the biceps Long head of the biceps (musculotendinous junction) Humeral shaft Pectoralis major tendon Plane/ region: Logitudinal (sagittal): What you will see: Long head of biceps; fibrillar structure Lesser tuberosity Long head of the biceps tendon Notes: Subscapularis muscle and tendon Patient position: Facing the examiner Shoulder in lateral rotation; elbow in flexion/ supination Plane/ region: longitudinal (axial): full vertical width of tendon. What you will see: Subscapularis muscle, tendon, and insertion Supraspinatus tendon Coracoid process Deltoid Greater tuberosity Lesser tuberosity Notes: Do passive medial/ lateral rotation while examining Plane/ region: Transverse (sagittal): What you will see: Lesser tuberosity Fascicles of subscapularis tendon Supraspinatus tendon Patient position: Lateral to examiner Shoulder in extension and medial rotation Hand on ipsilateral buttock Plane/ region: Longitudinal (oblique sagittal) Identify the intra-articular portion of biceps LH in the transverse plane; then -

Intramuscular Neural Distribution of the Sartorius Muscles: Treating Spasticity with Botulinum Neurotoxin
Intramuscular Neural Distribution of the Sartorius Muscles: Treating Spasticity With Botulinum Neurotoxin Kyu-Ho Yi Yonsei University Ji-Hyun Lee Yonsei University Kyle Seo Modelo Clinic Hee-Jin Kim ( [email protected] ) Yonsei University Research Article Keywords: botulinum neurotoxin, spasticity, sartorius muscle, Sihler’s staining Posted Date: January 6th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-129928/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/14 Abstract This study aimed to detect the idyllic locations for botulinum neurotoxin injection by analyzing the intramuscular neural distributions of the sartorius muscles. A altered Sihler’s staining was conducted on sartorius muscles (15 specimens). The nerve entry points and intramuscular arborization areas were measured as a percentage of the total distance from the most prominent point of the anterior superior iliac spine (0%) to the medial femoral epicondyle (100%). Intramuscular neural distribution were densely detected at 20–40% and 60–80% for the sartorius muscles. The result suggests that the treatment of sartorius muscle spasticity requires botulinum neurotoxin injections in particular locations. These locations, corresponding to the locations of maximum arborization, are suggested as the most safest and effective points for botulinum neurotoxin injection. Introduction Spasticity is a main contributor to functional loss in patients with impaired central nervous system, such as in stroke, cerebral palsy, multiple sclerosis, traumatic brain injury, spinal cord injury, and others 1. Sartorius muscle, as a hip and knee exor, is one of the commonly involved muscles, and long-lasting spasticity of the muscle results in abnormalities secondary to muscle hyperactivity, affecting lower levels of functions, such as impairment of gait. -

Pes Anserinus Syndrome
DEPARTMENT OF ORTHOPEDIC SURGERY SPORTS MEDICINE Marc R. Safran, MD Professor, Orthopaedic Surgery Chief, Division of Sports Medicine PES ANSERINUS SYNDROME DESCRIPTION The pes anserinus is the tendon insertion of 3 muscles of the thigh into the upper leg (tibia), just below the knee to the inner side of the front of the leg. Where the tendon attaches to bone, there is a bursa sac between the bone and the tendon. The bursa functions like a water balloon to reduce friction and wear of the tendon against the bone. With this syndrome there is inflammation and pain of the bursa (bursitis), tendon (tendinitis), or both. FREQUENT SIGNS AND SYMPTOMS Pain, tenderness, swelling, warmth and/or redness over the pes anserinus bursa and tendon on the front inner leg just 2-3 inches below the knee. The pain is usually slight when beginning to exercise and is worse as the activity continues. Pain with running or bending the knee against resistance Crepitation (a crackling sound) when the tendon or bursa is moved or touched CAUSES Strain from sudden increase in amount or intensity of activity or overuse of the lower extremity usually in the endurance athlete or the athlete just beginning to run. May also be due to direct trauma to the upper leg. RISK INCREASES WITH Endurance sports (distance runs, triathlons) Beginning a training program Sports that require pivoting, cutting (sudden change of direction while running), jumping and deceleration. Incorrect training techniques that include excessive hill running, recent large increases in mileage, inadequate time for rest between workouts.. Poor physical conditioning (strength/flexibility) Inadequate warm-up prior to practice or play Knock knees Arthritis of the knee. -

Burt Klos MD Phd Stephan Konijnenberg MD Ultrasound Imaging and Conservative Treatment Follow up Presenter Disclosure Information
Burt Klos MD PhD Stephan Konijnenberg MD Ultrasound imaging and conservative treatment follow up Presenter Disclosure Information Burt Klos disclosed no conflict of interest. Musculoskeletal Ultrasound • US Cuff /bursa • Knee Bakers Cyst • Knee Tendinitis Ultrasound positions prone , supine , hyperflexion Tendon imaging MRI vs MSU Static Dynamic Overview Focus Recognition Learning curve Less detail Interactive Relative value of MRI sports injury • KSSTA 2017 MRI is not reliable in diagnosing of concomitant anterolateral ligament and anterior cruciate ligament injuries of the knee • BM. Devitt et al AUS • KSSTA 2017 High prevalence of Segond Avulsion in MS ultrasound not found with MRI • Klos , Konijnenberg NL Courtesy C vd Hart * * Sport tendon injuries • Achilles tendon • Patella tendon • Pes anserinus Pes anserinus tendino/bursitis IA pathology (hydrops) Osteofyt impingement Endotorsion /Hyperpronation / Overload Researchgate.net femur tibia Ultrasound injection • Image-guided versus blind corticosteroid • injections in adults with shoulder pain: A systematic review • Edmund Soh 2011 BMC • statistically significant greater improvement in shoulder pain and function at 6 weeks after injection with MS Ultrasound • Sinus tarsi US guided injections Mayo Clinic 2010 • MSU 90 % accurate • Blinded injections 35 % accurate • J of Clinical ultrasound 2018 tibia • Pes anserinus bursa injection : • Blind versus US guided injection • 4/ 22 accurate placement in blind . Pes anserinus bursa injection Patella tendinopathy Patella tendinopathy • Tendon -

Anserine Bursitis an Under-Diagnosed, Easily Treatable Cause of Knee Pain He Anserine Bursa Was Initially Called the No-Name-No-Fame by Suzan M
perspectives on pain ADDRESSING PATIENT NEEDS Anserine bursitis An under-diagnosed, easily treatable cause of knee pain he anserine bursa was initially called the no-name-no-fame BY SUZAN M. ATTAR, MD tbursa. The term anserine bur- sitis presently in use was coined by Moshcowitz in 1937, when he first pelvic area, which results in angu- lateral ligament injury or from pes described the condition.1 lation at the knee joint, putting anserine tendonitis. Certain provo- The anserine bursa is located more pressure on the pes anserine cative manoeuvres, however, may medially, 6 cm below the joint line attachment. Secondary causes in- help: between the attachment of the med- clude medial compartment osteo- • tenderness that extends from ial collateral ligament and the con- arthritis of the knee, obesity, direct the anserine bursal area to the joined tendon (see Figures 1 and 2). trauma, abnormal gait, tight ham- joint line is more likely due to Pes anserinus means “goose’s foot” strings and, less commonly, over- inflammation or injury of the and is the anatomic location of the use injury, as in athletics.4 medial collateral ligament conjoined tendons formed by gracilis, • the supine valgus stress test, sartorius and semitendinosus mus- Clinical symptoms which is used to determine the cles in the knee.2 This article will pro- Pain is localized to a well-defined integrity of the medial collateral vide an overview, including the clinical area on the medial knee region over ligament, should not aggravate presentation and management. the upper tibia. Patients often point the pain of anserine bursitis to the spot with one finger. -

Pelvis. Muscles of the Lower Limb. Walking
Pelvis. Muscles of the lower limb. Walking Sándor Katz M.D.,Ph.D. Pelvis Pelvic ligaments Pelvis Hip muscles: iliopsoas (psoas major and iliacus) iliacus Origin: psoas major: vertebral bodies of the T12-L4 vertebrae and costal processes of the L1-5 vertebrae iliacus: iliac fossa Insertion: lesser trochanter Action: flexion of the hip joint; lateral flexion of the lumbar spine Innervation:spinal nerves and femoral nerve Hip muscles - gluteus maximus • Origin: dorsal to the posterior gluteal line of the ilium, sacrum and thoracolumbar fascia • Insertion: gluteal tuberosity, iliotibial tract • Action: Hip joint: adbuction-adduction, extension and lateral rotation. Knee joint: stabilisation when the knee is extended. • Innervation: inferior gluteal nerve Hip muscles - gluteus medius • Origin: between the anterior and posterior gluteal lines of the ilium • Insertion: greater trochanter • Action: abduction and rotation. • Innervation: superior gluteal nerve Hip muscles - gluteus minimus • Origin: between the anterior and inferior gluteal lines of the ilium • Insertion: greater trochanter • Action: abduction and rotation. • Innervation: superior gluteal nerve Hip muscles Piriformis • Origin: 2nd-4th sacral pelvic foramina • Insertion: tip of the greater trochanter • Action: abduction and lateral rotation. • Innervation: sciatic nerve Obturator internus • Origin: inner surface o f t h e o b t u r a t o r foramen and obturator membrane • I n s e r t i o n : trochanteric fossa • Action: adduction and lateral rotation. • Innervation: sacral plexus Obturator externus • Origin: outer surface o f t h e o b t u r a t o r foramen and obturator membrane • I n s e r t i o n : trochanteric fossa • Action: adduction and lateral rotation. -
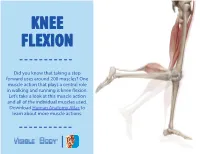
Did You Know That Taking a Step Forward Uses Around 200 Muscles? One Muscle Action That Plays a Central Role in Walking and Running Is Knee Flexion
KNEE FLEXION Did you know that taking a step forward uses around 200 muscles? One muscle action that plays a central role in walking and running is knee flexion. Let’s take a look at this muscle action and all of the individual muscles used. Download Human Anatomy Atlas to learn about more muscle actions. KNEE CAP KNEE MCL ACL OVERVIEW The knee is one of the largest joints in the human body. It provides shock absorption during walking and running, and allows flexion and extension. The knee’s stability is maintained MEDIAL by different ligaments like the MENISCUS anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament LCL PCL LATERAL MENISCUS (MCL), medial meniscus, lateral meniscus, lateral collateral ligament (LCL). ANTERIOR VIEW POSTERIOR VIEW KNEE EXTENSION KNEE FLEXION KNEE FLEXION OVERVIEW Knee flexion is the action of the knee bending the leg towards the buttock. The reverse of this action, when the lower leg is straightened, is called knee extension. Sartorius MUSCLES Gracilis OF Semitendinosus KNEE FLEXION Semimembranosus Biceps Femoris (Long Head) Biceps Femoris (Short Head) There are 8 main muscles used in knee flexion. We will take a look at each one Gastrocnemius and their individual origins, insertions, innervation, and blood supply points. Achilles Tendon SARTORIUS The sartorius is the longest muscle in the body. It is located in the anterior compartment of the thigh and assists in the movements of the hip, thigh, knee, and lower leg. Origin: Ilium (anterior superior iliac spine) Insertion: -

Thigh Muscles
Lecture 14 THIGH MUSCLES ANTERIOR and Medial COMPARTMENT BY Dr Farooq Khan Aurakzai PMC Dated: 03.08.2021 INTRODUCTION What are the muscle compartments? The limbs can be divided into segments. If these segments are cut transversely, it is apparent that they are divided into multiple sections. These are called fascial compartments, and are formed by tough connective tissue septa. Compartments are groupings of muscles, nerves, and blood vessels in your arms and legs. INTRODUCTION to the thigh Muscles The musculature of the thigh can be split into three sections by intermuscular septas in to; Anterior compartment Medial compartment and Posterior compartment. Each compartment has a distinct innervation and function. • The Anterior compartment muscle are the flexors of hip and extensors of knee. • The Medial compartment muscle are adductors of thigh. • The Posterior compartment muscle are extensor of hip and flexors of knee. Anterior Muscles of thigh The muscles in the anterior compartment of the thigh are innervated by the femoral nerve (L2-L4), and as a general rule, act to extend the leg at the knee joint. There are three major muscles in the anterior thigh –: • The pectineus, • Sartorius and • Quadriceps femoris. In addition to these, the end of the iliopsoas muscle passes into the anterior compartment. ANTERIOR COMPARTMENT MUSCLE 1. SARTORIUS Is a long strap like and the most superficial muscle of the thigh descends obliquely Is making one of the tendon of Pes anserinus . In the upper 1/3 of the thigh the med margin of it makes the lat margin of Femoral triangle. Origin: Anterior superior iliac spine. -

Pes Anserinus Structural Framework and Constituting Tendons Are Grossly Aberrant in Nigerian Population
Hindawi Publishing Corporation Anatomy Research International Volume 2015, Article ID 483186, 9 pages http://dx.doi.org/10.1155/2015/483186 Research Article Pes Anserinus Structural Framework and Constituting Tendons Are Grossly Aberrant in Nigerian Population J. O. Ashaolu,1,2 T. S. Osinuga,1 V. O. Ukwenya,3 E. O. Makinde,1 and A. J. Adekanmbi1 1 Department of Anatomy, Faculty of Basic Medical Sciences, College of Health Sciences, Bowen University, Iwo 284, Osun State, Nigeria 2Department of Anatomy, Faculty of Basic Medical Sciences, College of Health Sciences, University of Ilorin, Ilorin 1515, Kwara State, Nigeria 3Department of Anatomy, Faculty of Basic Medical Sciences, College of Medicine, Ekiti State University, Ado-Ekiti 5363, Ekiti State, Nigeria Correspondence should be addressed to J. O. Ashaolu; [email protected] Received 6 May 2015; Revised 15 June 2015; Accepted 16 June 2015 Academic Editor: Robert J. Spinner Copyright © 2015 J. O. Ashaolu et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. We evaluated the morphological framework of the pes anserinus in both knees of ten Nigerian cadavers and we observed high degree of variability in its morphology and location. The pes anserinus inserted specifically on the superior half of the media border of the tibia, as far inferiorly as 124.44 mm to the tibial tuberosity (prolonged insertion). The insertion was also joined to the part of tibia close to the tibia tuberosity (90%) and to the fascia cruris (10%). -

Anserine Syndrome
Artigo de revisÃO A síndrome anserina Milton Helfenstein Jr1 e Jorge Kuromoto2 RESUMO Dor no joelho é uma condição comum na clínica diária e a patologia anserina, também conhecida como pata de ganso, tem sido considerada uma das principais causas. O diagnóstico tem sido realizado de maneira eminentemente clínica, o que tem gerado equívocos. Os pacientes queixam-se tipicamente de dor na parte medial do joelho, com sensibilidade na porção ínferomedial. Estudos de imagem têm sido realizados para esclarecer se tais pacientes possuem bursite, tendinite ou ambos os distúrbios na região conhecida como pata de ganso. Entretanto, o defeito estrutural responsável pelos sintomas permanece desconhecido, motivo pelo qual preferimos intitular como “Síndrome Anserina”. O diabetes mellitus é um fator predisponente bem reconhecido. O sobrepeso e a osteoartrite de joelho parecem ser fatores adicionais de risco, contudo, seus papéis na gênese da moléstia ainda não são bem entendidos. O tratamento atual inclui anti-inflamatório, fisioterapia e infiltração de corticoide, com evolução muito variável, que oscila entre 10 dias e 36 meses. A falta de conhecimento sobre a etiofisiopatologia e dados epidemiológicos exige futuros estudos para esse frequente e intrigante distúrbio. Palavras-chave: bursite anserina, tendinite da pata de ganso, síndrome da bursite/tendinite anserina, pata de ganso. INTRODUÇÃO A síndrome tem sido evidenciada em atletas corredores de longa distância.3 O diabetes mellitus (DM) tem sido identifi- A inserção combinada dos tendões dos músculos sartório, grácil cado em uma substancial proporção desses pacientes.4 Casos e semitendinoso, a cerca de 5 cm distalmente da porção medial considerados como bursite crônica foram documentados em da articulação do joelho, forma uma estrutura que se assemelha artrite reumatoide e em osteoartrite.5,6 à membrana natatória do ganso, razão pela qual os anatomistas A etiologia também inclui trauma, retração da musculatura a denominaram de “pata de ganso”, ou, do latim, pes anserinus. -

1 Knee Muscle Power Deficits “Patellofemoral Pain Syndrome
1 Knee Muscle Power Deficits “Patellofemoral Pain Syndrome” ICD-9-CM: 719.46 Pain in joint - lower leg Diagnostic Criteria History: Anterior knee pain Precipitated by trauma (subluxation), unaccustomed weight bearing activities, or prolonged sitting Worsens with bent knee sitting and activities – especially squatting, climbing stairs, or running Physical Exam: Limited medial patellar glide and/or excessive lateral patellar glide – with pain at end range of one or both of these glides (may need to vary the amount of knee flexion to elicit symptoms) Biomechanical abnormalities (such as pronatory disorders, patella malalignment, VMO/quadriceps weakness, tight lateral retinaculum and myofascia excessive lateral tracking excessive Q angle, hip muscle length and strength imbalances Patella Lateral Glide Patella Medial Glide Cues Assess glides at varying degrees of knee flexion - up to about 30° Determine motion availability Determine symptom responses at end range - be sure to use a strong force if mild- moderate forces are asymptomatic Ben Cornell PT, Joe Godges PT Loma Linda U DPT Program KPSoCal Ortho PT Residency 2 "Patellar Tendinitis" ICD-9-CM: 726.64 Patellar tendinitis Diagnostic Criteria History: Anterior knee pain. Pain associated with repetitive use of extensor mechanism (e.g., jumping, kicking) Physical Exam: Symptoms reproduced with palpation to inferior pole of patella, or patella tendon insertion at the tibial tuberosity Patellar Tendon Palpation/Provocation Cues: P= Patella 1= Inferior Pole 2= Superior Pole 3= Tibial Tuberosity -

Snapping Pes Anserinus Caused by Gracilis Tendon: a New Mechanism
J Korean Soc Radiol 2019;80(5):969-974 Case Report https://doi.org/10.3348/jksr.2019.80.5.969 pISSN 1738-2637 / eISSN 2288-2928 Received July 19, 2018 Revised October 4, 2018 Accepted December 19, 2018 Snapping Pes Anserinus *Corresponding author Tae Eun Kim, MD Department of Radiology, Daegu Fatima Hospital, Caused By Gracilis Tendon: 99 Ayang-ro, Dong-gu, Daegu 41199, Korea. A New Mechanism Proposed Tel 82-53-940-7161 Fax 82-53-954-7417 by Dynamic Knee E-mail [email protected] This is an Open Access article distributed under the terms of the Creative Commons Attribu- Ultrasonography tion Non-Commercial License 두덩정강건에 의해서 발생하는 거위발 근육의 퉁김현상: (https://creativecommons.org/ licenses/by-nc/4.0) which permits 역동적 무릎 초음파 검사에 근거한 새로운 기전 unrestricted non-commercial use, distribution, and reproduc- tion in any medium, provided the Hyun Seok Oh, MD , Tae Eun Kim, MD* original work is properly cited. Department of Radiology, Daegu Fatima Hospital, Daegu, Korea ORCID iDs Tae Eun Kim https:// Snapping pes anserinus is the main extra-articular cause of snapping on the medial side of the orcid.org/0000-0002-9874-0247 Hyun Seok Oh knee. There are limited articles that describe the mechanism of the condition, especially only https:// when flexion of the knee. We report a case of snapping pes anserinus in a 23-year-old skier, which orcid.org/0000-0003-0036-2792 was reproduced on only active flexion of both knees in the posteromedial aspect of the tibia, with pain for 6 years, diagnosed using dynamic ultrasonography for elucidating a new mecha- nism of the gracilis tendon.