HIP THIGH KNEE Ultrasound – Fundamental
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Knee Flow Chart Acute
Symptom chart for acute knee pain START HERE Did the knee pain begin Does the knee joint You may have a fracture or Stop what you are doing immediately and go to a hospital emergency room YES YES suddenly, with an injury, appear deformed, or dislocated patella. or an orthopedic surgeon specializing in knee problems. slip, fall, or collision? out of position? If possible, splint the leg to limit the movement of the knee until you reach NO the doctor. Do not put any weight on the knee. Use a wheelchair, a cane, or NO crutch to prevent putting any weight on the leg, which might cause further damage to the joint. GO TO FLOW CHART #2 Go to an orthopedic surgeon Stop what you are doing. Continuing activity despite the feeling that the knee ON CHRONIC KNEE Did you hear a “pop” YES immediately, you may have is unstable can cause additional damage to other ligaments, meniscus , and PROBLEMS THAT DEVELOP and does your knee feel torn your anterior cruciate, or cartilage. Try ice on the knee to control swelling. Take anti-in ammatories OR WORSEN OVER TIME. unstable or wobbly? other ligaments in the knee. like Advil or Nuprin until your doctor’s appointment. About a third of ligament tears get better with exercises, a third may need a brace, and a third may need sur gery. NO Use R•I•C•E for sore knees Does your knee hurt YES You may have damaged the articular Try anti-in ammatories, as directed on the bottle, for two days to reduce R: Rest as you bend it? cartilage on the bottom of the the chronic in ammation. -

Iliopsoas Tendonitis/Bursitis Exercises
ILIOPSOAS TENDONITIS / BURSITIS What is the Iliopsoas and Bursa? The iliopsoas is a muscle that runs from your lower back through the pelvis to attach to a small bump (the lesser trochanter) on the top portion of the thighbone near your groin. This muscle has the important job of helping to bend the hip—it helps you to lift your leg when going up and down stairs or to start getting out of a car. A fluid-filled sac (bursa) helps to protect and allow the tendon to glide during these movements. The iliopsoas tendon can become inflamed or overworked during repetitive activities. The tendon can also become irritated after hip replacement surgery. Signs and Symptoms Iliopsoas issues may feel like “a pulled groin muscle”. The main symptom is usually a catch during certain movements such as when trying to put on socks or rising from a seated position. You may find yourself leading with your other leg when going up the stairs to avoid lifting the painful leg. The pain may extend from the groin to the inside of the thigh area. Snapping or clicking within the front of the hip can also be experienced. Do not worry this is not your hip trying to pop out of socket but it is usually the iliopsoas tendon rubbing over the hip joint or pelvis. Treatment Conservative treatment in the form of stretching and strengthening usually helps with the majority of patients with iliopsoas bursitis. This issue is the result of soft tissue inflammation, therefore rest, ice, anti- inflammatory medications, physical therapy exercises, and/or injections are effective treatment options. -
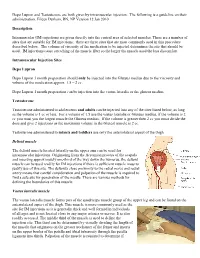
An Intramuscular Injection Is an Injection Given Directly Into The
Depo Lupron and Testosterone are both given by intramuscular injection. The following is a guideline on their administration. Eileen Durham, RN, NP Version 12 Jan 2010 Description Intramuscular (IM) injections are given directly into the central area of selected muscles. There are a number of sites that are suitable for IM injections; there are three sites that are most commonly used in this procedure described below. The volume of viscosity of the medication to be injected determines the site that should be used. IM injections cause stretching of the muscle fiber so the larger the muscle used the less discomfort. Intramuscular Injection Sites Depo Lupron Depo Lupron 3 month preparation should only be injected into the Gluteus medius due to the viscosity and volume of the medication approx. 1.5 – 2 cc. Depo Lupron 1 month preparation can be injection into the vastus lateralis or the gluteus medius. Testosterone Testosterone administered to adolescents and adults can be injected into any of the sites listed below, as long as the volume is 1 cc or less. For a volume of 1.5 use the vastus lateralis or Gluteus medius, if the volume is 2 cc you must you the largest muscle the Gluteus medius. If the volume is greater then 2 cc you must divide the dose and give 2 injections as the maximum volume in the Gluteal muscle is 2 cc. Testosterone administered to infants and toddlers use only the anteriolateral aspect of the thigh. Deltoid muscle The deltoid muscle located laterally on the upper arm can be used for intramuscular injections. -

Bacterial Meningitis and Multiple Abscess Formation in the Iliopsoas
Yamada et al. Renal Replacement Therapy (2018) 4:22 https://doi.org/10.1186/s41100-018-0163-x CASEREPORT Open Access Bacterial meningitis and multiple abscess formation in the iliopsoas, erector spinae, and vastus lateralis muscle in a maintenance hemodialysis patient treated with continuous epidural anesthesia for herpes zoster-related pain control: a case report and review of the literature Shunsuke Yamada1, Narihito Tatsumoto1, Noriko Nakamura1, Kosuke Masutani1, Toshiro Maeda2, Takanari Kitazono1 and Kazuhiko Tsuruya1,3* Abstract Background: Infection is the second leading cause of mortality in patients who undergo maintenance hemodialysis. In this population, impairment in both cellular and humoral immunity contributes to the increased incidence of infection and infection-related hospitalization. However, these artificial devices occasionally enhance the risk of deep organ infection including muscle abscess, frequently leading to disability and mortality in hemodialysis patients. Case presentation: A 54-year-old male undergoing maintenance hemodialysis was hospitalized because of the acute onset pain in the back and bilateral legs and declining consciousness which started at 7 days after the treatment of herpes zoster-related neuralgia with continuous epidural anesthesia. Physical examination revealed purulent discharge from the insertion site of the catheter. Serum biochemical tests showed increased inflammatory response and malnutrition. Magnetic resonance imaging revealed meningitis and multiple abscesses in the iliopsoas, erector spinae, gluteus medius, and vastus lateralis muscles, where conventional antibiotic treatment often fails to cure. Staphylococcus aureus was detected in the cerebrospinal fluid. Combination of intravenous antibiotics treatment and aggressive open surgical drainage of the muscle abscesses finally cured meningitis and multiple deep muscle abscesses in this patient. -

The Anatomy of the Posterolateral Aspect of the Rabbit Knee
Journal of Orthopaedic Research ELSEVIER Journal of Orthopaedic Research 2 I (2003) 723-729 www.elsevier.com/locate/orthres The anatomy of the posterolateral aspect of the rabbit knee Joshua A. Crum, Robert F. LaPrade *, Fred A. Wentorf Dc~~ur/niiviiof Orthopuer/ic Surgery. Unicrrsity o/ Minnesotu. MMC 492, 420 Dcluwur-c Si. S. E., Minnwpoli,s, MN 55455, tiSA Accepted 14 November 2002 Abstract The purpose of this study was to determine the anatomy of the posterolateral aspect of the rabbit knee to serve as a basis for future in vitro and in vivo posterolateral knee biomechanical and injury studies. Twelve nonpaired fresh-frozen New Zealand white rabbit knees were dissected to determine the anatomy of the posterolateral corner. The following main structures were consistently identified in the rabbit posterolateral knee: the gastrocnemius muscles, biceps femoris muscle, popliteus muscle and tendon, fibular collateral ligament, posterior capsule, ligament of Wrisberg, and posterior meniscotibial ligament. The fibular collateral ligament was within the joint capsule and attached to the femur at the lateral epi- condyle and to the fibula at the midportion of the fibular head. The popliteus muscle attached to the medial edge of the posterior tibia and ascended proximally to give rise to the popliteus tendon, which inserted on the proximal aspect of the popliteal sulcus just anterior to the fibular collateral ligament. The biceps femoris had no attachment to the fibula and attached to the anterior com- partment fascia of the leg. This study increased our understanding of these structures and their relationships to comparative anatomy in the human knee. -

The Influence of Altered Lower-Extremity Kinematics on Patellofemoral Joint Dysfunction: a Theoretical Perspective
The Influence of Altered Lower-Extremity Kinematics on Patellofemoral Joint Dysfunction: A Theoretical Perspective Christopher M. Powers, PT, PhD 1 Although patellofemoral pain (PFP) is recognized as being one of the most common disorders of It has been recognized by sev- the lower extremity, treatment guidelines and underlying rationales remain vague and controver- eral authors that the patel- sial. The premise behind most treatment approaches is that PFP is the result of abnormal patellar lofemoral joint may be influenced CLINICAL COMMENTARY tracking and/or patellar malalignment. Given as such, interventions typically focus on the joint by the segmental interactions of itself and have traditionally included strengthening the vastus medialis oblique, taping, bracing, the lower extremity.6,7,21,27,34,45 Ab- soft tissue mobilization, and patellar mobilization. More recently, it has been recognized that the normal motion(s) of the tibia and patellofemoral joint and, therefore, PFP may be influenced by the interaction of the segments and femur in the transverse and frontal joints of the lower extremity. In particular, abnormal motion of the tibia and femur in the transverse and frontal planes may have an effect on patellofemoral joint mechanics. With this in planes are believed to have an mind, interventions aimed at controlling hip and pelvic motion (proximal stability) and ankle/foot effect on patellofemoral joint me- motion (distal stability) may be warranted and should be considered when treating persons with chanics and therefore PFP. An un- patellofemoral joint dysfunction. The purpose of this paper is to provide a biomechanical derstanding of how lower- overview of how altered lower-extremity mechanics may influence the patellofemoral joint. -

Acellular Dermal Graft Augmentation in Quadriceps Tendon Rupture Repair
INNOVATIONS IN PRACTICE Acellular dermal graft augmentation in quadriceps tendon rupture repair Ross M. Wilkins INTRODUCTION cific pain and swelling of the knee indicative of other more nstability of the knee from failure of the extensor frequent soft-tissue maladies such as ligament rupture, mechanism is a debilitating problem. Extensor mechan- partial tears, and the presence of intact medial and lateral 19 ism failure frequently is the result of patellar tendon patellar retinacula and iliotibial band. The purpose of this I retrospective review was to describe a ‘‘stent’’ augmentation rupture, quadriceps tendon rupture, patellar fracture or avulsion of the patellar tendon.1,2 Such failures have method for rupture of the quadriceps tendon and evaluate been linked to underlying pathologies such as diabetes the effects of quadriceps tendon augmentation in both the mellitus, gout, corticosteroid use, autoimmune inflamma- presence and absence of a TKA. tory diseases, hyperthyroidism, obesity and end-stage renal disease.3--8 Often, the treatment of this problem is com- MATERIALS AND METHODS pounded by the presence of a total knee arthroplasty (TKA) Eight knees in seven patients were treated using acellular or the need for a TKA.7 Depending on the root cause of the human dermal matrix, (AHDM; GRAFT JACKETs Matrix, instability, there are a variety of ways to treat this soft-tissue Wright Medical Technology, Arlington TN) for chronic insufficiency. Historically, problems of the extensor me- quadriceps tendon rupture at a single institution. Four chanism have been operatively treated using primary repair, of these patients presented with a TKA, with one patient tendon autografts, fascia, extensor mechanism allografts, having had bilateral TKA. -

Strain Assessment of Deep Fascia of the Thigh During Leg Movement
Strain Assessment of Deep Fascia of the Thigh During Leg Movement: An in situ Study Yulila Sednieva, Anthony Viste, Alexandre Naaim, Karine Bruyere-Garnier, Laure-Lise Gras To cite this version: Yulila Sednieva, Anthony Viste, Alexandre Naaim, Karine Bruyere-Garnier, Laure-Lise Gras. Strain Assessment of Deep Fascia of the Thigh During Leg Movement: An in situ Study. Frontiers in Bioengineering and Biotechnology, Frontiers, 2020, 8, 15p. 10.3389/fbioe.2020.00750. hal-02912992 HAL Id: hal-02912992 https://hal.archives-ouvertes.fr/hal-02912992 Submitted on 7 Aug 2020 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. fbioe-08-00750 July 27, 2020 Time: 18:28 # 1 ORIGINAL RESEARCH published: 29 July 2020 doi: 10.3389/fbioe.2020.00750 Strain Assessment of Deep Fascia of the Thigh During Leg Movement: An in situ Study Yuliia Sednieva1, Anthony Viste1,2, Alexandre Naaim1, Karine Bruyère-Garnier1 and Laure-Lise Gras1* 1 Univ Lyon, Université Claude Bernard Lyon 1, Univ Gustave Eiffel, IFSTTAR, LBMC UMR_T9406, Lyon, France, 2 Hospices Civils de Lyon, Hôpital Lyon Sud, Chirurgie Orthopédique, 165, Chemin du Grand-Revoyet, Pierre-Bénite, France Fascia is a fibrous connective tissue present all over the body. -

Elbow Checklist
Workbook Musculoskeletal Ultrasound September 26, 2013 Shoulder Checklist Long biceps tendon Patient position: Facing the examiner Shoulder in slight medial rotation; elbow in flexion and supination Plane/ region: Transverse (axial): from a) intraarticular portion to b) myotendinous junction (at level of the pectoralis major tendon). What you will see: Long head of the biceps tendon Supraspinatus tendon Transverse humeral ligament Subscapularis tendon Lesser tuberosity Greater tuberosity Short head of the biceps Long head of the biceps (musculotendinous junction) Humeral shaft Pectoralis major tendon Plane/ region: Logitudinal (sagittal): What you will see: Long head of biceps; fibrillar structure Lesser tuberosity Long head of the biceps tendon Notes: Subscapularis muscle and tendon Patient position: Facing the examiner Shoulder in lateral rotation; elbow in flexion/ supination Plane/ region: longitudinal (axial): full vertical width of tendon. What you will see: Subscapularis muscle, tendon, and insertion Supraspinatus tendon Coracoid process Deltoid Greater tuberosity Lesser tuberosity Notes: Do passive medial/ lateral rotation while examining Plane/ region: Transverse (sagittal): What you will see: Lesser tuberosity Fascicles of subscapularis tendon Supraspinatus tendon Patient position: Lateral to examiner Shoulder in extension and medial rotation Hand on ipsilateral buttock Plane/ region: Longitudinal (oblique sagittal) Identify the intra-articular portion of biceps LH in the transverse plane; then -

Knee Joint Distraction Compared with Total Knee Arthroplasty a RANDOMISED CONTROLLED TRIAL
KNEE Knee joint distraction compared with total knee arthroplasty A RANDOMISED CONTROLLED TRIAL J. A. D. van der Woude, Aims K. Wiegant, Knee joint distraction (KJD) is a relatively new, knee-joint preserving procedure with the R. J. van Heerwaarden, goal of delaying total knee arthroplasty (TKA) in young and middle-aged patients. We S. Spruijt, present a randomised controlled trial comparing the two. P. J. E m ans , Patients and Methods S. C. Mastbergen, The 60 patients ≤ 65 years with end-stage knee osteoarthritis were randomised to either F. P. J. G. Lafeber KJD (n = 20) or TKA (n = 40). Outcomes were assessed at baseline, three, six, nine, and 12 months. In the KJD group, the joint space width (JSW) was radiologically assessed, From UMC Utrecht, representing a surrogate marker of cartilage thickness. Utrecht, The Netherlands Results In total 56 patients completed their allocated treatment (TKA = 36, KJD = 20). All patient reported outcome measures improved significantly over one year (p < 0.02) in both groups. J. A. D. van der Woude, MD, At one year, the TKA group showed a greater improvement in only one of the 16 patient- PhD, Resident in Orthopaedic Surgery, Limb and Knee related outcome measures assessed (p = 0.034). Outcome Measures in Rheumatology- Reconstruction Unit, Department of Orthopaedic Osteoarthritis Research Society International clinical response was 83% after TKA and 80% Surgery after KJD. A total of 12 patients (60%) in the KJD group sustained pin track infections. In the R. J. van Heerwaarden, MD, PhD, Orthopaedic Surgeon, KJD group both mean minimum (0.9 mm, standard deviation (SD) 1.1) and mean JSW (1.2 mm, Limb and Knee Reconstruction Unit, Department of SD 1.1) increased significantly (p = 0.004 and p = 0.0003). -

Intramuscular Neural Distribution of the Sartorius Muscles: Treating Spasticity with Botulinum Neurotoxin
Intramuscular Neural Distribution of the Sartorius Muscles: Treating Spasticity With Botulinum Neurotoxin Kyu-Ho Yi Yonsei University Ji-Hyun Lee Yonsei University Kyle Seo Modelo Clinic Hee-Jin Kim ( [email protected] ) Yonsei University Research Article Keywords: botulinum neurotoxin, spasticity, sartorius muscle, Sihler’s staining Posted Date: January 6th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-129928/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/14 Abstract This study aimed to detect the idyllic locations for botulinum neurotoxin injection by analyzing the intramuscular neural distributions of the sartorius muscles. A altered Sihler’s staining was conducted on sartorius muscles (15 specimens). The nerve entry points and intramuscular arborization areas were measured as a percentage of the total distance from the most prominent point of the anterior superior iliac spine (0%) to the medial femoral epicondyle (100%). Intramuscular neural distribution were densely detected at 20–40% and 60–80% for the sartorius muscles. The result suggests that the treatment of sartorius muscle spasticity requires botulinum neurotoxin injections in particular locations. These locations, corresponding to the locations of maximum arborization, are suggested as the most safest and effective points for botulinum neurotoxin injection. Introduction Spasticity is a main contributor to functional loss in patients with impaired central nervous system, such as in stroke, cerebral palsy, multiple sclerosis, traumatic brain injury, spinal cord injury, and others 1. Sartorius muscle, as a hip and knee exor, is one of the commonly involved muscles, and long-lasting spasticity of the muscle results in abnormalities secondary to muscle hyperactivity, affecting lower levels of functions, such as impairment of gait. -

A Cadaver Research
Journal of Arthroscopy and Joint Surgery 6 (2019) 114e116 Contents lists available at ScienceDirect Journal of Arthroscopy and Joint Surgery journal homepage: www.elsevier.com/locate/jajs Tensile strength comparison between hamstring tendon, patellar tendon, quadriceps tendon and peroneus longus tendon: A cadaver research * Krisna Y. Phatama a, , Mohamad Hidayat a, Edi Mustamsir a, Ananto Satya Pradana a, Brian Dhananjaya b, Surya Iman Muhammad b a Orthopaedic and Traumatology Department, Lower Extremity and Adult Reconstruction Division, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No.2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia b Orthopaedic and Traumatology Department, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No. 2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia article info abstract Article history: Knee ligament injury is a frequent occurrence. Ligament reconstruction using tendon graft is the best Received 6 December 2018 therapy recommendation in the case of severe knee ligament injury. Tendon graft that is oftenly used are Accepted 15 February 2019 hamstring tendon, patellar tendon (BPTB), quadriceps tendon and peroneus longus tendon have been Available online 19 February 2019 proposed as tendon graft donor. Biomechanically, tensile strength from tendon graft is the main factor that greatly contributes to the success of ligament reconstruction procedure. Numerous researches have Keywords: been done to calculate tensile strengths of hamstring and patellar tendon, but there has not been a Ligament reconstruction research done yet on the comparison of the tensile strengths of peroneus longus tendon, hamstring, Tendon graft Tensile strength patellar tendon and quadriceps tendon. This research will strive to record the tensile strengths of per- oneus longus tendon, hamstring, patellar tendon and quadriceps tendon as well as their comparison.