Ocular Emergencies for the Primary Care Optometrist
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Non-Invasive Evaluation of Cerebrospinal Fluid Pressure in Ocular Hypertension
perim Ex en l & ta a l ic O p in l h t C h f Journal of Clinical & Experimental a o l m l a o n l r o Xie et al., J Clin Exp Ophthalmol 2017, 8:4 g u y o J Ophthalmology DOI: 10.4172/2155-9570.1000672 ISSN: 2155-9570 Research Article Open Access Non-invasive Evaluation of Cerebrospinal Fluid Pressure in Ocular Hypertension: The Beijing Intracranial and Intraocular Pressure Study Xiaobin Xie1,2, Weiwei Chen3,4, Zhen Li5, Ravi Thomas3,6,7, Yong Li8, Junfang Xian8, Diya Yang4, Huaizhou Wang4, Jun Feng1, Shoukang Zhang1, Lixia Zhang1, Ruojin Ren9 and Ningli Wang3,4* 1Eye Hospital of China Academy of Chinese Medical Sciences, Beijing, China 2Post-doctoral Research Station Affiliated to the Chinese Academy of Chinese Medical Sciences, Beijing, China 3Beijing Institute of Ophthalmology, Beijing Tongren Eye Center, Beijing Tongren Hospital, Capital Medical University, China 4Beijing Tongren Eye Center, Beijing Ophthalmology and Visual Sciences Key Laboratory, Beijing Tongren Hospital, Capital Medical University, Beijing, China 5Department of Ophthalmology, Xuanwu Hospital, Capital Medical University, Beijing, China 6Queensland Eye Institute, 140 Melbourne Street, South Brisbane 4101, Queensland, Australia 7University of Queensland, Brisbane, Australia 8Department of Radiology, Beijing Tongren Hospital, Capital Medical University, Beijing, China 9State University of New York College of Optometry, New York, United States *Corresponding author: Ningli Wang, Beijing Tongren Eye Center, Beijing Tongren Hospital, Capital Medical University, Beijing Ophthalmology and Visual Sciences Key Laboratory, Dongjiaominxiang Street, Dongcheng District, Beijing 100730, China, Tel: +8610-5826-9968; Fax: +8610-5826-9920; E-mail: [email protected] Received date: July 19, 2017; Accepted date: August 10, 2017; Published date: June 30, 2017 Copyright: © 2017 Xie X, et al. -
Cone Interaction with Progressive Macular Dysfunction
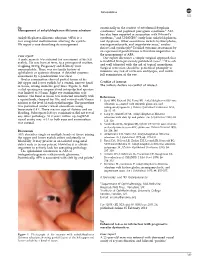
Correspondence 823 Sir, occasionally in the context of ectodermal dysplasia Management of ankyloblepharon filiforme adnatum syndromes3 and popliteal pterygium syndrome.4 AFA has also been reported in association with Edward’s Ankyloblepharon filiforme adnatum (AFA) is a syndrome,5 and CHANDS6 (curly hair, ankyloblepharon, rare congenital malformation affecting the eyelids. nail dysplasia). Other associations include hydrocephalus, We report a case describing its management. meningomyelocoele, and imperforate anus,7 cardiac defects and syndactyly.4 Detailed systemic assessment by an experienced paediatrician is therefore imperative in Case report the management of AFA. Our report illustrates a simple surgical approach that A male neonate was referred for assessment of his left is modified from previously published cases.1,2,4 It is safe eyelids. He was born at term, to a primigravid mother, and well tolerated with the aid of topical anaesthesia. weighing 3150 g. Pregnancy and delivery were Surgical correction should be performed promptly to unremarkable. There was no family history of minimise any risk of occlusion amblyopia, and enable ophthalmic or systemic disease. A detailed systemic full examination of the eye. assessment by a paediatrician was clear. Ocular examination showed partial fusion of his left upper and lower eyelids by a central, narrow band Conflict of interest of tissue, arising from the grey lines (Figure 1). Full The authors declare no conflict of interest. eyelid opening was impaired and interpalpebral aperture was limited to 3.5 mm. Right eye examination was normal. The band of tissue was retracted anteriorly with References a squint hook, clamped for 10 s, and excised with Vannas 1 Scott MH, Richard JM, Farris BK. -

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

Neurotrophic Keratopathy and Diabetes Mellitus a Lockwood Et Al 838
Eye (2006) 20, 837–839 & 2006 Nature Publishing Group All rights reserved 0950-222X/06 $30.00 www.nature.com/eye 1 1 2 Neurotrophic A Lockwood , M Hope-Ross and P Chell CASE SERIES keratopathy and diabetes mellitus Abstract no history of previous corneal trauma or herpes simplex infection. Ocular examination revealed Diabetes mellitus is frequently associated a best-corrected visual acuity of 6/12 in both with microvascular complications such as eyes. There was an epithelial irregularity retinopathy, nephropathy, and peripheral extending across the inferonasal quadrant of the neuropathy. Neurotrophic keratopathy occurs right cornea. A diagnosis of exposure in response to a neuropathy of the ophthalmic keratopathy was made. She was treated with division of the trigeminal nerve. Rarely has artificial tears and a month later the epithelium diabetic neurotrophic keratopathy been had healed. A year later, an epithelial defect in described. This paper discusses the the same area was seen at follow-up. Again she ophthalmic histories of three patients who was asymptomatic and the visual acuity was presented with diabetic neurotrophic unchanged. Decreased corneal sensation was keratopathy. In one patient the corneal noted using a cotton swab to touch the ulceration was the sole presenting feature of peripheral and central cornea. A diagnosis of his diabetes. We discuss the need for increased diabetic neurotrophic keratopathy was made. vigilance in the ophthalmic community for She was treated with ocular lubricants. After suspecting diabetes in patients with 6 months, the defect had increased in size to unexplained corneal epithelial disease. 5.5 mm. There was associated corneal Eye (2006) 20, 837–839. -

Optical Coherence Tomography (OCT) Anterior Segment of the Eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: optical_coherence_tomography_(OCT)_anterior_segment_of_the_eye Origination: 2/2010 Last CAP Review: 6/2021 Next CAP Review: 6/2022 Last Review: 6/2021 Description of Procedure or Service Optical Coherence Tomography Optical coherence tomography (OCT) is a noninvasive, high-resolution imaging method that can be used to visualize ocular structures. OCT creates an image of light reflected from the ocular structures. In this technique, a reflected light beam interacts with a reference light beam. The coherent (positive) interference between the 2 beams (reflected and reference) is measured by an interferometer, allowing construction of an image of the ocular structures. This method allows cross-sectional imaging a t a resolution of 6 to 25 μm. The Stratus OCT, which uses a 0.8-μm wavelength light source, was designed to evaluate the optic nerve head, retinal nerve fiber layer, and retinal thickness in the posterior segment. The Zeiss Visante OCT and AC Cornea OCT use a 1.3-μm wavelength light source designed specifically for imaging the a nterior eye segment. Light of this wa velength penetrates the sclera, a llowing high-resolution cross- sectional imaging of the anterior chamber (AC) angle and ciliary body. The light is, however, typically blocked by pigment, preventing exploration behind the iris. Ultrahigh resolution OCT can achieve a spatial resolution of 1.3 μm, allowing imaging and measurement of corneal layers. Applications of OCT OCT of the anterior eye segment is being eva luated as a noninvasive dia gnostic and screening tool with a number of potential a pplications. -

Refractive Surgery Faqs. Refractive Surgery the OD's Role in Refractive
9/18/2013 Refractive Surgery Refractive Surgery FAQs. Help your doctor with refractive surgery patient education Corneal Intraocular Bill Tullo, OD, FAAO, LASIK Phakic IOL Verisys Diplomate Surface Ablation Vice-President of Visian PRK Clinical Services LASEK CLE – Clear Lens Extraction TLC Laser Eye Centers Epi-LASIK Cataract Surgery AK - Femto Toric IOL Multifocal IOL ICRS - Intacs Accommodative IOL Femtosecond Assisted Inlays Kamra The OD’s role in Refractive Surgery Refractive Error Determine the patient’s interest Myopia Make the patient aware of your ability to co-manage surgery Astigmatism Discuss advancements in the field Hyperopia Outline expectations Presbyopia/monovision Presbyopia Enhancements Risks Make a recommendation Manage post-op care and expectations Myopia Myopic Astigmatism FDA Approval Common Use FDA Approval Common Use LASIK: 1D – 14D LASIK: 1D – 8D LASIK: -0.25D – -6D LASIK: -0.25D – -3.50D PRK: 1D – 13D PRK: 1D – 6D PRK: -0.25D – -6D PRK: -0.25D – -3.50D Intacs: 1D- 3D Intacs: 1D- 3D Intacs NONE Intacs: NONE P-IOL: 3D- 20D P-IOL: 8D- 20D P-IOL: NONE P-IOL: NONE CLE/CAT: any CLE/CAT: any CLE/CAT: -0.75D - -3D CLE/CAT: -0.75D - -3D 1 9/18/2013 Hyperopia Hyperopic Astigmatism FDA Approval Common Use FDA Approval Common Use LASIK: 0.25D – 6D LASIK: 0.25D – 4D LASIK: 0.25D – 6D LASIK: 0.25D – 4D PRK: 0.25D – 6D PRK: 0.25D – 4D PRK: 0.25D – 6D PRK: 0.25D – 4D Intacs: NONE Intacs: NONE Intacs: NONE Intacs: NONE P-IOL: NONE P-IOL: NONE P-IOL: NONE P-IOL: -

Bilateral Acute Angle Closure Glaucoma After Hyperopic LASIK Correction
Saudi Journal of Ophthalmology (2009) 23, 215– 217 King Saud University Saudi Journal of Ophthalmology www.ksu.edu.sa www.sciencedirect.com CASE REPORT Bilateral acute angle closure glaucoma after hyperopic LASIK correction Essam A. Osman, MD *, Ahmed A. Alsaleh, MD, Turki Al Turki, MD, Saleh A. AL Obeidan, MD Department of Ophthalmology, College of Medicine, King Saud University, Riyadh, Saudi Arabia Received 25 May 2009; accepted 13 July 2009 Available online 24 October 2009 KEYWORDS Abstract Acute angle closure glaucoma is unexpected complication following laser in situ ker- Acute glaucoma; atomileusis (LASIK). We are reporting a 49-years-old lady that was presented to the emergency Hyperopia; department with acute glaucoma in both eyes soon after LASIK correction. Diagnosis was made LASIK on detailed clinical history and examination, slit lamp examination, intraocular pressure measure- ment and gonioscopy. Laser iridotomy in both eyes succeeded in controlling the attack and normal- izing the intraocular pressure (IOP) more than 6 months of follow-up. Prophylactic laser iridotomy is essential for narrow angle patients before LASIK surgery if refractive laser surgery is indicated. ª 2009 King Saud University. All rights reserved. 1. Introduction Paciuc et al. reported a case of unilateral acute angle clo- sure glaucoma 1 year after hyperopic LASIK correction (Paci- Primary angle closure glaucoma (PACG) is a vision-threaten- uc et al., 2000). However, we are reporting a case of bilateral ing type of glaucoma. A high prevalence of PACG has been re- acute glaucoma soon after LASIK correction. LASIK surgery ported in the Asian region (Kunimatsu, 2007). Angle closure is the most popular form of laser eye surgery, in which an oph- glaucoma soon after LASIK procedure is an unexpected thalmic surgeon reshapes the cornea using an excimer laser complication. -

Comparison of Retinal Vessel Diameter Between Open-Angle Glaucoma Patients with Initial Parafoveal Scotoma and Peripheral Nasal Step
Comparison of Retinal Vessel Diameter Between Open-Angle Glaucoma Patients With Initial Parafoveal Scotoma and Peripheral Nasal Step EUNJOO YOO, CHUNGKWON YOO, TAE-EUN LEE, AND YONG YEON KIM PURPOSE: To compare retinal vessel diameters (RVDs) LTHOUGH INTRAOCULAR PRESSURE (IOP) IS THE between open-angle glaucoma (OAG) patients with most important and only known modifiable risk initial parafoveal scotoma (PFS) and those with initial pe- A factor for glaucoma,1–4 not all patients with ripheral nasal step (PNS). glaucoma show elevated IOP. The Collaborative Normal- DESIGN: Retrospective, cross-sectional study. Tension Glaucoma study reported that 20% of the patients METHODS: We enrolled 151 eyes of 151 patients with with normal-tension glaucoma (NTG) show visual field OAG (83 with normal-tension glaucoma [NTG] and 68 (VF) deterioration, even after a 30% IOP reduction from with primary open-angle glaucoma [POAG]). The pa- baseline.2 Accumulating evidence indicates that, in addi- tients were categorized into the PFS and PNS groups ac- tion to mechanical factors, vascular pathology plays a role cording to the location of the initial visual field (VF) in open-angle glaucoma (OAG). The relationships between defect. Clinical characteristics and RVD indices—central glaucoma and vascular factors, such as migraine,5,6 optic retinal arteriolar equivalent (CRAE) and central retinal disc hemorrhage,7,8 and vasospasm,9 are well established. venular equivalent (CRVE)—were compared between Furthermore, many reports have suggested that glaucoma it- the groups. Subgroup analyses were conducted in the self is associated with the retinal vasculature. A previous NTG and POAG groups. study showed that retinal vessel diameter (RVD) decreases RESULTS: Forty-six patients had PFS and 105 had significantly with increasing glaucoma stage, independently PNS. -

Bioptics with LASIK Flap First for the Treatment of High Ametropia
Bioptics With LASIK Flap First for the Treatment of High Ametropia Merab L. Dvali, MD, PhD; Nana A. Tsinsadze, MD, PhD; Bella V. Sirbiladze, MD, PhD ioptics, fi rst described by Zaldivar et al,1 is the treat- ABSTRACT ment of refractive error using phakic intraocular PURPOSE: To report the safety and predictability of an B lens (IOL) implantation and excimer laser corneal alternate sequence of the bioptics procedure. ablation. Candidates for this procedure included patients with high refractive errors (with astigmatism) that surpass METHODS: In this prospective study of 50 eyes, pha- the treatment range for excimer laser refractive surgery and kic intraocular lenses (IOLs) and pseudophakic IOLs were patients whose corneal thickness will not allow full treat- implanted, followed by LASIK. The corneal fl ap was cre- ment of refractive error. ated, followed by lens implantation 3 days later. Laser ablation was performed to the stromal bed 3 months Over time, the defi nition of bioptics has expanded to in- later. Fifty eyes with varying degrees of refractive clude phakic, pseudophakic, and clear lens extraction cases error (range of manifest refraction spherical equivalent followed by surgery on the corneal plane. Phakic or pseudo- [MRSE], Ϫ19.50 to ϩ8.50 diopters [D]) were treated. phakic surgery followed by refractive surgery is the most com- Follow-up ranged from 3 months to 4 years postopera- mon form of bioptics.2 In this procedure, the lens is implanted tively. to correct the majority of refractive error followed by LASIK RESULTS: No intra- or postoperative complications performed at least 3 months postoperatively to correct the re- occurred. -

The Use of Anterior-Segment Optical-Coherence Tomography for the Assessment of the Iridocorneal Angle and Its Alterations: Update and Current Evidence
Journal of Clinical Medicine Review The Use of Anterior-Segment Optical-Coherence Tomography for the Assessment of the Iridocorneal Angle and Its Alterations: Update and Current Evidence Giacinto Triolo 1,* , Piero Barboni 2,3, Giacomo Savini 4, Francesco De Gaetano 1, Gaspare Monaco 1, Alessandro David 1 and Antonio Scialdone 1 1 Ophthalmic Institute, ASST Fatebenefratelli-Sacco, 20121 Milan, Italy; [email protected] (F.D.G.); [email protected] (G.M.); [email protected] (A.D.); [email protected] (A.S.) 2 San Raffaele Scientific Institute, University Vita-Salute, 20133 Milan, Italy; [email protected] 3 Studio Oculistico D’Azeglio, 40123 Bologna, Italy 4 G.B. Bietti Foundation I.R.C.C.S., 00198 Rome, Italy; [email protected] * Correspondence: [email protected] Abstract: The introduction of anterior-segment optical-coherence tomography (AS-OCT) has led to improved assessments of the anatomy of the iridocorneal-angle and diagnoses of several mechanisms of angle closure which often result in raised intraocular pressure (IOP). Continuous advancements in AS-OCT technology and software, along with an extensive research in the field, have resulted in a wide range of possible parameters that may be used to diagnose and follow up on patients with this spectrum of diseases. However, the clinical relevance of such variables needs to be explored thoroughly. The aim of the present review is to summarize the current evidence supporting the use of AS-OCT for the diagnosis and follow-up of several iridocorneal-angle and anterior-chamber Citation: Triolo, G.; Barboni, P.; alterations, focusing on the advantages and downsides of this technology. -

Corneal Ulcers in Cats
Corneal Ulcers in Cats 803-808-7387 www.gracepets.com The cornea is the clear, shiny membrane that makes up the surface of the eyeball. It is much like a clear window. To understand a corneal ulcer, you must first understand how the cornea is constructed. The cornea is comprised of three layers. The most superficial or outermost layer is the epithelium. This layer is comprised of many, very thin layers of cells, similar to an onion’s skin. Below the epithelium is the stroma and the deepest layer is Descemet's membrane. Because all of these layers are clear, it is not possible to see them without special stains and a microscope. Erosion through a few layers of the epithelium is called a corneal erosion or corneal abrasion. A corneal ulcer is an erosion through the entire epithelium and down into the stroma. If the erosion goes through the epithelium and stroma to the level of Descemet's membrane, a descemetocele exists. If Descemet's membrane ruptures, the liquid inside the eyeball leaks out and the eye collapses. What causes corneal ulcers? There are several causes for corneal ulcers in cats. The most common is trauma. An ulcer may result from blunt trauma, such as a cat rubbing its eye on a carpet, or due to a laceration, such as a cat-claw scratch. The second most common cause is chemical burn of the cornea. This may happen when irritating shampoo or dip gets in the eye. Less common causes of corneal ulcers include bacterial infections, viral infections, and other diseases. -

Congenital Ocular Anomalies in Newborns: a Practical Atlas
www.jpnim.com Open Access eISSN: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2020;9(2):e090207 doi: 10.7363/090207 Received: 2019 Jul 19; revised: 2019 Jul 23; accepted: 2019 Jul 24; published online: 2020 Sept 04 Mini Atlas Congenital ocular anomalies in newborns: a practical atlas Federico Mecarini1, Vassilios Fanos1,2, Giangiorgio Crisponi1 1Neonatal Intensive Care Unit, Azienda Ospedaliero-Universitaria Cagliari, University of Cagliari, Cagliari, Italy 2Department of Surgery, University of Cagliari, Cagliari, Italy Abstract All newborns should be examined for ocular structural abnormalities, an essential part of the newborn assessment. Early detection of congenital ocular disorders is important to begin appropriate medical or surgical therapy and to prevent visual problems and blindness, which could deeply affect a child’s life. The present review aims to describe the main congenital ocular anomalies in newborns and provide images in order to help the physician in current clinical practice. Keywords Congenital ocular anomalies, newborn, anophthalmia, microphthalmia, aniridia, iris coloboma, glaucoma, blepharoptosis, epibulbar dermoids, eyelid haemangioma, hypertelorism, hypotelorism, ankyloblepharon filiforme adnatum, dacryocystitis, dacryostenosis, blepharophimosis, chemosis, blue sclera, corneal opacity. Corresponding author Federico Mecarini, MD, Neonatal Intensive Care Unit, Azienda Ospedaliero-Universitaria Cagliari, University of Cagliari, Cagliari, Italy; tel.: (+39) 3298343193; e-mail: [email protected].