Circular RNA Expression Profiles in Pediatric Ependymomas Ulvi Ahmadov1, Meile M
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

Circular RNA Hsa Circ 0005114‑Mir‑142‑3P/Mir‑590‑5P‑ Adenomatous
ONCOLOGY LETTERS 21: 58, 2021 Circular RNA hsa_circ_0005114‑miR‑142‑3p/miR‑590‑5p‑ adenomatous polyposis coli protein axis as a potential target for treatment of glioma BO WEI1*, LE WANG2* and JINGWEI ZHAO1 1Department of Neurosurgery, China‑Japan Union Hospital of Jilin University, Changchun, Jilin 130033; 2Department of Ophthalmology, The First Hospital of Jilin University, Jilin University, Changchun, Jilin 130021, P.R. China Received September 12, 2019; Accepted October 22, 2020 DOI: 10.3892/ol.2020.12320 Abstract. Glioma is the most common type of brain tumor APC expression with a good overall survival rate. UALCAN and is associated with a high mortality rate. Despite recent analysis using TCGA data of glioblastoma multiforme and the advances in treatment options, the overall prognosis in patients GSE25632 and GSE103229 microarray datasets showed that with glioma remains poor. Studies have suggested that circular hsa‑miR‑142‑3p/hsa‑miR‑590‑5p was upregulated and APC (circ)RNAs serve important roles in the development and was downregulated. Thus, hsa‑miR‑142‑3p/hsa‑miR‑590‑5p‑ progression of glioma and may have potential as therapeutic APC‑related circ/ceRNA axes may be important in glioma, targets. However, the expression profiles of circRNAs and their and hsa_circ_0005114 interacted with both of these miRNAs. functions in glioma have rarely been studied. The present study Functional analysis showed that hsa_circ_0005114 was aimed to screen differentially expressed circRNAs (DECs) involved in insulin secretion, while APC was associated with between glioma and normal brain tissues using sequencing the Wnt signaling pathway. In conclusion, hsa_circ_0005114‑ data collected from the Gene Expression Omnibus database miR‑142‑3p/miR‑590‑5p‑APC ceRNA axes may be potential (GSE86202 and GSE92322 datasets) and explain their mecha‑ targets for the treatment of glioma. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
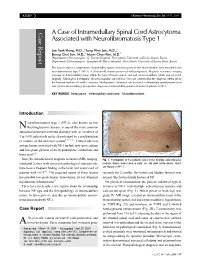
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Investigation of the Underlying Hub Genes and Molexular Pathogensis in Gastric Cancer by Integrated Bioinformatic Analyses
bioRxiv preprint doi: https://doi.org/10.1101/2020.12.20.423656; this version posted December 22, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Investigation of the underlying hub genes and molexular pathogensis in gastric cancer by integrated bioinformatic analyses Basavaraj Vastrad1, Chanabasayya Vastrad*2 1. Department of Biochemistry, Basaveshwar College of Pharmacy, Gadag, Karnataka 582103, India. 2. Biostatistics and Bioinformatics, Chanabasava Nilaya, Bharthinagar, Dharwad 580001, Karanataka, India. * Chanabasayya Vastrad [email protected] Ph: +919480073398 Chanabasava Nilaya, Bharthinagar, Dharwad 580001 , Karanataka, India bioRxiv preprint doi: https://doi.org/10.1101/2020.12.20.423656; this version posted December 22, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract The high mortality rate of gastric cancer (GC) is in part due to the absence of initial disclosure of its biomarkers. The recognition of important genes associated in GC is therefore recommended to advance clinical prognosis, diagnosis and and treatment outcomes. The current investigation used the microarray dataset GSE113255 RNA seq data from the Gene Expression Omnibus database to diagnose differentially expressed genes (DEGs). Pathway and gene ontology enrichment analyses were performed, and a proteinprotein interaction network, modules, target genes - miRNA regulatory network and target genes - TF regulatory network were constructed and analyzed. Finally, validation of hub genes was performed. The 1008 DEGs identified consisted of 505 up regulated genes and 503 down regulated genes. -

Risk-Adapted Therapy for Young Children with Embryonal Brain Tumors, High-Grade Glioma, Choroid Plexus Carcinoma Or Ependymoma (Sjyc07)
SJCRH SJYC07 CTG# - NCT00602667 Initial version, dated: 7/25/2007, Resubmitted to CPSRMC 9/24/2007 and 10/6/2007 (IRB Approved: 11/09/2007) Activation Date: 11/27/2007 Amendment 1.0 dated January 23, 2008, submitted to CPSRMC: January 23, 2008, IRB Approval: March 10, 2008 Amendment 2.0 dated April 16, 2008, submitted to CPSRMC: April 16, 2008, (IRB Approval: May 13, 2008) Revision 2.1 dated April 29, 2009 (IRB Approved: April 30, 2009 ) Amendment 3.0 dated June 22, 2009, submitted to CPSRMC: June 22, 2009 (IRB Approved: July 14, 2009) Activated: August 11, 2009 Amendment 4.0 dated March 01, 2010 (IRB Approved: April 20, 2010) Activated: May 3, 2010 Amendment 5.0 dated July 19, 2010 (IRB Approved: Sept 17, 2010) Activated: September 24, 2010 Amendment 6.0 dated August 27, 2012 (IRB approved: September 24, 2012) Activated: October 18, 2012 Amendment 7.0 dated February 22, 2013 (IRB approved: March 13, 2013) Activated: April 4, 2013 Amendment 8.0 dated March 20, 2014. Resubmitted to IRB May 20, 2014 (IRB approved: May 22, 2014) Activated: May 30, 2014 Amendment 9.0 dated August 26, 2014. (IRB approved: October 14, 2014) Activated: November 4, 2014 Un-numbered revision dated March 22, 2018. (IRB approved: March 27, 2018) Un-numbered revision dated October 22, 2018 (IRB approved: 10-24-2018) RISK-ADAPTED THERAPY FOR YOUNG CHILDREN WITH EMBRYONAL BRAIN TUMORS, HIGH-GRADE GLIOMA, CHOROID PLEXUS CARCINOMA OR EPENDYMOMA (SJYC07) Principal Investigator Amar Gajjar, M.D. Division of Neuro-Oncology Department of Oncology Section Coordinators David Ellison, M.D., Ph.D. -
Meningioma ACKNOWLEDGEMENTS
AMERICAN BRAIN TUMOR ASSOCIATION Meningioma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Meningioma Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit advocacy organization dedicated solely to brain tumor research. For nearly 45 years, the ABTA has been providing comprehensive resources that support the complex needs of brain tumor patients and caregivers, as well as the critical funding of research in the pursuit of breakthroughs in brain tumor diagnosis, treatment and care. To learn more about the ABTA, visit www.abta.org. We gratefully acknowledge Santosh Kesari, MD, PhD, FANA, FAAN chair of department of translational neuro- oncology and neurotherapeutics, and Marlon Saria, MSN, RN, AOCNS®, FAAN clinical nurse specialist, John Wayne Cancer Institute at Providence Saint John’s Health Center, Santa Monica, CA; and Albert Lai, MD, PhD, assistant clinical professor, Adult Brain Tumors, UCLA Neuro-Oncology Program, for their review of this edition of this publication. This publication is not intended as a substitute for professional medical advice and does not provide advice on treatments or conditions for individual patients. All health and treatment decisions must be made in consultation with your physician(s), utilizing your specific medical information. Inclusion in this publication is not a recommendation of any product, treatment, physician or hospital. COPYRIGHT © 2017 ABTA REPRODUCTION WITHOUT PRIOR WRITTEN PERMISSION IS PROHIBITED AMERICAN BRAIN TUMOR ASSOCIATION Meningioma INTRODUCTION Although meningiomas are considered a type of primary brain tumor, they do not grow from brain tissue itself, but instead arise from the meninges, three thin layers of tissue covering the brain and spinal cord. -
“Where Hope Springs Eternal”
BASIC FACTS ABOUT EPENDYMOMA “Where hope springs eternal” Pediatric Brain Tumor Foundation of the United States A Resource for Families ACKNOWLEDGEMENTS The Pediatric Brain Tumor Foundation of the United States wishes to thank Ian Pollack, MD, Department of Neurosurgery, Children’s Hospital of Pittsburgh, Pittsburgh, PA, for the scientific review of this publication. SOURCES Statistical data in this publication was obtained from the Central Brain Tumor Registry of the United States (CBTRUS) and the World Health Organization Classification of Tumors, 2000. DISCLAIMER The Pediatric Brain Tumor Foundation of the United States does not engage in rendering medical advice or professional medical services. Information contained in this publication is NOT intended to be a substitute for medical care and should not be used for the diagnosing or the treatment of a brain tumor or any other health problem. If you have or even suspect you have a problem concerning your health or that of someone else, you should consult with your healthcare provider. The materials provided by the Pediatric Brain Tumor Foundation of the United States are compiled based on current information at the time that they were written. Medical research concerning disease and treatments is an ongoing process. We endeavor to keep our materials current. However, you should contact your doctors and medical institutions to seek the most current information available. COPYRIGHT Copyright© 2002 by the Pediatric Brain Tumor Foundation of the United States, Inc. The contents of this publication have been prepared for the exclusive use of the Pediatric Brain Tumor Foundation of the United States. It may not be reproduced in part or in its entirety without the written permission of the Pediatric Brain Tumor Foundation of the United States. -

Long-Term Follow-Up of Coexisting Meningioma and Intramedullary Ependymoma As a Collision Tumor in the Spinal Cord: a Case Report
Case Report Clinics in Surgery Published: 31 Jan, 2019 Long-Term Follow-Up of Coexisting Meningioma and Intramedullary Ependymoma as a Collision Tumor in the Spinal Cord: A Case Report Masatoshi Teraguchi1*, Mamoru Kawakami1, Shinichi Nakao2, Daisuke Fukui3 and Yukihiro Nakagawa1 1Spine Care Center, Wakayama Medical University, Japan 2Sumiya Orthopaedic Hospital, Wakayama, Japan 3Department of Orthopedic Surgery, Wakayama Medical University, Japan Abstract Background: Meningioma and ependymoma are usually presented as intramedullary and extramedullay tumor of spinal cord, respectively. However, coexistence of meningioma and ependymoma as a single mixed tumor in the single spinal cord and canal is an extremely rare occurrence. To our knowledge, there have been no reports on a mixed tumor with a distinct meningioma in thoracic region and ependymoma occurring at the cauda equina. Here, we report a case of long-term follow-up of coexisting meningioma and intramedullary ependymoma as a collision tumor in the spinal cord. Case Presentation: A 58-year-old woman presented with claudication in the lower limb one month after a fall from a step, characterized by weakness, numbness, and pain. MRI revealed two spinal lesions, one at the T4 level and the other in the cauda equina, at the L2 level, with L1 vertebral fracture. The patient underwent tumor resection via osteoplastic laminotomy from T3 to T5 and L2 to L3 simultaneously. Histopathological examination revealed that the tumor at the T4 level was a WHO grade I meningioma and that the lesion at L2 was a WHO grade II ependymoma. The postoperative course after 8 years was uneventful, with no recurrence, and the patient’s symptoms OPEN ACCESS resolved completely. -

Transcriptome Alterations of Vascular Smooth Muscle Cells in Aortic Wall of Myocardial Infarction Patients
This document is downloaded from DR‑NTU (https://dr.ntu.edu.sg) Nanyang Technological University, Singapore. Transcriptome alterations of vascular smooth muscle cells in aortic wall of myocardial infarction patients Wongsurawat, Thidathip; Woo, Chin Cheng; Giannakakis, Antonis; Lin, Xiao Yun; Cheow, Esther Sok Hwee; Lee, Chuen Neng; Richards, Mark; Sze, Siu Kwan; Nookaew, Intawat; Sorokin, Vitaly; Kuznetsov, Vladimir Andreevich 2018 Wongsurawat, T., Woo, C. C., Giannakakis, A., Lin, X. Y., Cheow, E. S. H., Lee, C. N., et al. (2018). Transcriptome alterations of vascular smooth muscle cells in aortic wall of myocardial infarction patients. Data in Brief, 17, 1112‑1135. https://hdl.handle.net/10356/85590 https://doi.org/10.1016/j.dib.2018.01.108 © 2018 The Authors. Published by Elsevier Inc. This is an open access article under the CC BY license (http://creativecommons.org/licenses/by/4.0/). Downloaded on 09 Oct 2021 06:21:01 SGT Data in Brief 17 (2018) 1112–1135 Contents lists available at ScienceDirect Data in Brief journal homepage: www.elsevier.com/locate/dib Data Article Transcriptome alterations of vascular smooth muscle cells in aortic wall of myocardial infarction patients Thidathip Wongsurawat a,b, Chin Cheng Woo c, Antonis Giannakakis a, Xiao Yun Lin d, Esther Sok Hwee Cheow e, Chuen Neng Lee c,d, Mark Richards f,g, Siu Kwan Sze e, Intawat Nookaew b, Vladimir A. Kuznetsov a,h, Vitaly Sorokin c,d,⁎ a Department of Genome and Gene Expression Data Analysis, Bioinformatics Institute, Agency for Science, Technology and Research (A*STAR), -

Human Induced Pluripotent Stem Cell–Derived Podocytes Mature Into Vascularized Glomeruli Upon Experimental Transplantation
BASIC RESEARCH www.jasn.org Human Induced Pluripotent Stem Cell–Derived Podocytes Mature into Vascularized Glomeruli upon Experimental Transplantation † Sazia Sharmin,* Atsuhiro Taguchi,* Yusuke Kaku,* Yasuhiro Yoshimura,* Tomoko Ohmori,* ‡ † ‡ Tetsushi Sakuma, Masashi Mukoyama, Takashi Yamamoto, Hidetake Kurihara,§ and | Ryuichi Nishinakamura* *Department of Kidney Development, Institute of Molecular Embryology and Genetics, and †Department of Nephrology, Faculty of Life Sciences, Kumamoto University, Kumamoto, Japan; ‡Department of Mathematical and Life Sciences, Graduate School of Science, Hiroshima University, Hiroshima, Japan; §Division of Anatomy, Juntendo University School of Medicine, Tokyo, Japan; and |Japan Science and Technology Agency, CREST, Kumamoto, Japan ABSTRACT Glomerular podocytes express proteins, such as nephrin, that constitute the slit diaphragm, thereby contributing to the filtration process in the kidney. Glomerular development has been analyzed mainly in mice, whereas analysis of human kidney development has been minimal because of limited access to embryonic kidneys. We previously reported the induction of three-dimensional primordial glomeruli from human induced pluripotent stem (iPS) cells. Here, using transcription activator–like effector nuclease-mediated homologous recombination, we generated human iPS cell lines that express green fluorescent protein (GFP) in the NPHS1 locus, which encodes nephrin, and we show that GFP expression facilitated accurate visualization of nephrin-positive podocyte formation in -

Cognitive Characterization of Schizophrenia Risk Variants Involved in Synaptic Transmission: Evidence of CACNA1C 'S Role in Working Memory
Neuropsychopharmacology (2017) 42, 2612–2622 © 2017 American College of Neuropsychopharmacology. All rights reserved 0893-133X/17 www.neuropsychopharmacology.org Cognitive Characterization of Schizophrenia Risk Variants Involved in Synaptic Transmission: Evidence of CACNA1C 's Role in Working Memory 1 1 2 3 4,5 3 Donna Cosgrove , Omar Mothersill , Kimberley Kendall , Bettina Konte , Denise Harold , Ina Giegling , 3 6 6 7 Annette Hartmann , Alex Richards , Kiran Mantripragada , The Wellcome Trust Case Control Consortium , Michael J Owen6, Michael C O’Donovan6, Michael Gill4, Dan Rujescu3, James Walters2, Aiden Corvin4, Derek W Morris1 and Gary Donohoe*,1 1 The Cognitive Genetics & Cognitive Therapy Group, The School of Psychology and Discipline of Biochemistry, The Centre for Neuroimaging & Cognitive Genomics, National University of Ireland Galway, Galway, Ireland; 2Institute of Psychological Medicine and Clinical Neurosciences, Cardiff University, Cardiff, UK; 3Department of Psychiatry, Psychotherapy and Psychosomatics, Martin-Luther-University Halle-Wittenberg, Halle, Germany; 4 Neuropsychiatric Genetics Research Group, Department of Psychiatry, Institute of Molecular Medicine, Trinity College Dublin, Dublin, Ireland; 5 6 School of Biotechnology, Dublin City University, Dublin, Ireland; MRC Centre for Neuropsychiatric Genetics and Genomics, Cardiff University, Cardiff, UK With 4100 common variants associated with schizophrenia risk, establishing their biological significance is a priority. We sought to establish cognitive effects of