An Introduction to Anaesthesia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Patient-Monitoring Systems
17 Patient-Monitoring Systems REED M. GARDNER AND M. MICHAEL SHABOT After reading this chapter,1 you should know the answers to these questions: ● What is patient monitoring, and why is it done? ● What are the primary applications of computerized patient-monitoring systems in the intensive-care unit? ● How do computer-based patient monitors aid health professionals in collecting, analyzing, and displaying data? ● What are the advantages of using microprocessors in bedside monitors? ● What are the important issues for collecting high-quality data either automatically or manually in the intensive-care unit? ● Why is integration of data from many sources in the hospital necessary if a computer is to assist in critical-care-management decisions? 17.1 What Is Patient Monitoring? Continuous measurement of patient parameters such as heart rate and rhythm, respira- tory rate, blood pressure, blood-oxygen saturation, and many other parameters have become a common feature of the care of critically ill patients. When accurate and imme- diate decision-making is crucial for effective patient care, electronic monitors frequently are used to collect and display physiological data. Increasingly, such data are collected using non-invasive sensors from less seriously ill patients in a hospital’s medical-surgical units, labor and delivery suites, nursing homes, or patients’ own homes to detect unex- pected life-threatening conditions or to record routine but required data efficiently. We usually think of a patient monitor as something that watches for—and warns against—serious or life-threatening events in patients, critically ill or otherwise. Patient monitoring can be rigorously defined as “repeated or continuous observations or meas- urements of the patient, his or her physiological function, and the function of life sup- port equipment, for the purpose of guiding management decisions, including when to make therapeutic interventions, and assessment of those interventions” (Hudson, 1985, p. -

Capnography 101 Oxygenation and Ventilation
It’s Time to Start Using it! Capnography 101 Oxygenation and Ventilation What is the difference? Oxygenation and Ventilation Ventilation O Oxygenation (capnography) 2 (oximetry) CO Cellular 2 Metabolism Capnographic Waveform • Capnograph detects only CO2 from ventilation • No CO2 present during inspiration – Baseline is normally zero CD AB E Baseline Capnogram Phase I Dead Space Ventilation • Beginning of exhalation • No CO2 present • Air from trachea, posterior pharynx, mouth and nose – No gas exchange occurs there – Called “dead space” Capnogram Phase I Baseline A B I Baseline Beginning of exhalation Capnogram Phase II Ascending Phase • CO2 from the alveoli begins to reach the upper airway and mix with the dead space air – Causes a rapid rise in the amount of CO2 • CO2 now present and detected in exhaled air Alveoli Capnogram Phase II Ascending Phase C Ascending II Phase Early A B Exhalation CO2 present and increasing in exhaled air Capnogram Phase III Alveolar Plateau • CO2 rich alveolar gas now constitutes the majority of the exhaled air • Uniform concentration of CO2 from alveoli to nose/mouth Capnogram Phase III Alveolar Plateau Alveolar Plateau CD III AB CO2 exhalation wave plateaus Capnogram Phase III End-Tidal • End of exhalation contains the highest concentration of CO2 – The “end-tidal CO2” – The number seen on your monitor • Normal EtCO2 is 35-45mmHg Capnogram Phase III End-Tidal End-tidal C D AB End of the the wave of exhalation Capnogram Phase IV Descending Phase • Inhalation begins • Oxygen fills airway • CO2 level quickly -

General Anaesthesia in Oral Surgery and Outpatient Surgery History
Department of Oral- and Maxillofacial Surgery, Semmelweis University Budapest Head of Department: Dr. Németh Zsolt General anaesthesia in oral surgery and outpatient surgery History 1844 Horace Wells nitrous oxide extraction of one of his own wisdom teeth by a colleague 1846 William Morton (pupil of Wells) ether extraction 1946 introduction of lidocaine General anaesthesia should be strictly limited to those patients and clinical situations in which local anaesthesia (with or without sedation) is not an option. Bourne JG. General anaesthesia in the dental surgery. B Dental J 1962; 113: 54-7. Coleman F. The history of nitrous oxide anaesthesia. Dental Record 1942; 62: 143-9 Naveen Malhotra General Anaesthesia for Dentistry ndian Journal of Anaesthesia 2008;52:Suppl (5):725-737 Types of general anaesthesia Outpatient anaesthesia • Dental chair anaesthesia Relative analgesia for simple extraction • Day care anaesthesia Conscious sedation (Sedoanalgesia) for minor oral surgery In patient anaesthesia Intubation with or without neuromuscular blocking for complicated extractions, oral- and maxillofacial surgical procedures Indications of general anaesthesia • Acute infection (pain) • Children • Mentally challenged patients • Dental phobia • Allergy to local anaesthetics • Extensive dentistry & facio-maxillary surgery Equipments • anaesthesia machine, vaporizers • oxygen, nitrous oxide • breathing circuits (adult and pediatric) • nasal and facial masks • oral and nasal air-ways • different laryngoscopes with all sizes of blades • nasal and -
Drug Administration Routes - Summary
Only Use L6. DrugCourse Administration & Transport 207 by Fluid Motion 243/CENG April 19, 2018 NANO Only Use Course 207 243/CENG Part I: Drug Administration NANO Routes of Drug Administration Only Topical: local effect, substanceUse is applied directly where its action is desired. EnteralCourse: systemic effect, substance is 207given via the gastrointestinal (GI) tract. Parenteral: systemic effect, substance is given by routes other than the gastrointestinal (GI) tract. 243/CENG NANO Topical Drug Delivery Epicutaneous – directly onto the surface of the skin Only allergy testing local anesthesia… Use Eye drops antibiotics for conjunctivitis … Course Inhalational207 asthma medications acute infection in upper airway … 243/CENG Intranasal route decongestant nasal sprays … NANO Enteral Drug Delivery Any form of administration that involves any part of the gastrointestinalOnly tract Use Course 207 Oral: Rectal: Gastric feeding tube: many drugs as tablets, various drugs in many drugs, enteral capsules, drops… suppository or enema nutrition… form… 243/CENG NANO Parenteral Drug Delivery Intravenous: into a vein (many drugs, total parenteral nutrition…) Only Intramuscular: into a muscle (many vaccines, antibiotics…) Use Subcutaneous: under the skin (insulin…) Intraarterial: into an artery (vasodilator drugs in the treatment of vasospasm…) Course Intradermal: into the skin itself (skin testing some allergens, tattoos…) 207 Transdermal: diffusion through the intact skin (transdermal opioid patches in pain management, nicotine patches for treatment -

Methohexital(BAN, Rinn)
1788 General Anaesthetics metabolic pathways include hydroxylation of the 3. Lökken P, et al. Conscious sedation by rectal administration of Methohexital Sodium (BANM, rINNM) midazolam or midazolam plus ketamine as alternatives to gener- cyclohexone ring and conjugation with glucuronic ac- al anesthesia for dental treatment of uncooperative children. Compound 25398; Enallynymalnatrium; Méthohexital Sodique; id. The beta phase half-life is about 2.5 hours. Keta- Scand J Dent Res 1994; 102: 274–80. Methohexitone Sodium; Metohexital sódico; Natrii Methohexi- 4. Louon A, et al. Sedation with nasal ketamine and midazolam for talum. mine is excreted mainly in the urine as metabolites. It cryotherapy in retinopathy of prematurity. Br J Ophthalmol crosses the placenta. 1993; 77: 529–30. Натрий Метогекситал 5. Zsigmond EK, et al. A new route, jet-injection for anesthetic in- C14H17N2NaO3 = 284.3. ◊ References. duction in children–ketamine dose-range finding studies. Int J CAS — 309-36-4; 22151-68-4; 60634-69-7. 1. Clements JA, Nimmo WS. Pharmacokinetics and analgesic ef- Clin Pharmacol Ther 1996; 34: 84–8. ATC — N01AF01; N05CA15. fect of ketamine in man. Br J Anaesth 1981; 53: 27–30. 6. Kronenberg RH. Ketamine as an analgesic: parenteral, oral, rec- tal, subcutaneous, transdermal and intranasal administration. J ATC Vet — QN01AF01; QN05CA15. 2. Grant IS, et al. Pharmacokinetics and analgesic effects of IM and Pain Palliat Care Pharmacother 2002; 16: 27–35. oral ketamine. Br J Anaesth 1981; 53: 805–9. Pharmacopoeias. US includes Methohexital Sodium for In- jection. 3. Grant IS, et al. Ketamine disposition in children and adults. Br J Nonketotic hyperglycinaemia. -

Local Anaesthesia for Major General Surgical Postgrad Med J: First Published As 10.1136/Pgmj.72.844.105 on 1 February 1996
Postgrad Med J' 1996; 72: 105-108 C) The Fellowship of Postgraduate Medicine, 1996 Local anaesthesia for major general surgical Postgrad Med J: first published as 10.1136/pgmj.72.844.105 on 1 February 1996. Downloaded from procedures A review of 1 16 cases over 12 years A Dennison, N Oakley, D Appleton, J Paraskevopoulos, D Kerrigan, J Cole, WEG Thomas Summary ation was collated from medical notes, anaes- Between 1980 and 1992, 116 patients had thetic records and operation notes. Cases in either a simple mastectomy (32) or intra- which local anaesthesia was augmented by abdominal procedures (84) under local regional or intravenous techniques were exc- anaesthesia (0.5-1% lignocaine with luded from the study. Patients were not 1:200 000 adrenaline). A wide variety of included ifthey had neck/head or limb surgery, general surgical procedures were feasible abdominal hernia repair, simple drainage of using only supplementary intravenous intra-abdominal abscess or any minor proce- sedation (54%). Complications were un- dures including peritoneo-venous shunts, common and related to surgical proce- laparoscopic or endoscopic procedures. dure (three incorrect diagnoses, three The 116 patients presented in the study are procedures impossible) rather than the those who had intra-abdominal surgery (84; 53 anaesthetic technique. There were no women, 31 men) or simple mastectomy (32). anaesthetic toxicity or postoperative pro- The median age was 74 years (range 27-92) blems. Local anaesthesia is extremely and all the patients were grade III or worse on safe and facilitates larger surgical proce- the American Society of Anaesthesiologists dures than is generally appreciated. -

Ketamine for Paediatric Sedation/Analgesia in the Emergency Department
275 Emerg Med J: first published as 10.1136/emj.2003.005769 on 22 April 2004. Downloaded from CLINICAL TOPIC REVIEW Emerg Med J: first published as 10.1136/emj.2003.005769 on 22 April 2004. Downloaded from Ketamine for paediatric sedation/analgesia in the emergency department M C Howes ............................................................................................................................... Emerg Med J 2004;21:275–280. doi: 10.1136/emj.2003.005769 This review investigates the use of ketamine for paediatric pain or other noxious stimuli, with relative preservation of respiratory and cardiovascular sedation and analgesia in the emergency department functions despite profound amnesia and analge- ........................................................................... sia,10 30–32 described as ‘‘cataleptic.’’10 This trance- like state of sensory isolation provides a unique combination of amnesia, sedation, and analge- he injured child presents a challenge to sia.7103031 The eyes often remain open, though emergency department (ED) practitioners. nystagmus is commonly seen. Heart rate and The pain and distress can be upsetting for T blood pressure remain stable, and are often staff as well as parents. The child’s distress can stimulated, possibly through sympathomimetic be compounded by the fear of a painful actions.30 31 33 Functional residual capacity and procedure to follow, previous conditioning from tidal volume are preserved, with bronchial unexpected ‘‘jabs’’ when receiving immunisa- smooth muscle relaxation34–37 and maintenance tions, or previous visits to an ED.1 of airway patency and respiration.10 30 31 38 As doctors we strive to relieve pain and However, despite the enthusiasm of many suffering, and swear to do no harm. Forced authors and practitioners, ketamine may not be restraint, still performed in some departments in the ideal agent. -

A Comparative Study of Anaesthetic Agents on High Voltage Activated Calcium
bioRxiv preprint doi: https://doi.org/10.1101/2020.12.17.423182; this version posted December 18, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. A COMPARATIVE STUDY OF ANAESTHETIC AGENTS ON HIGH VOLTAGE ACTIVATED CALCIUM CHANNEL CURRENTS IN IDENTIFIED MOLLUSCAN NEURONS Terrence J. Morris1, Philip M. Hopkins2,3 and William Winlow4,5 1Department Science and Technology - Biology, Douglas College, 700 Ryal Avenue, New Westminster, British Columbia, Canada; 2 Leeds Institute of Medical Research at St James’s, School of Medicine, University of Leeds, Leeds, United Kingdom; 3Malignant Hyperthermia Investigation Unit, Leeds Institute of Molecular Medicine, St. James’s University Hospital, Leeds, LS9 7TF, United Kingdom; 4 Department of Biology, University of Naples Federico II, Via Cintia 26, 80126, Naples, Italy; 5Institute of Ageing and Chronic Diseases, University of Liverpool, Liverpool, United Kingdom. Corresponding author: William Winlow Key Words: General anaesthetic, calcium channels, Lymnaea, light yellow cells SUMMARY 1. Using the two electrode voltage clamp configuration, a high voltage activated whole-cell Ca2+ channel current (IBa) was recorded from a cluster of neurosecretory ‘Light Yellow’ Cells (LYC) in the right parietal ganglion of the pond snail Lymnaea stagnalis. 2. Recordings of IBa from LYCs show a reversible concentration-dependent depression of current amplitude in the presence of the volatile anaesthetics halothane, isoflurane and sevoflurane, or the non-volatile anaesthetic pentobarbitone at clinical concentrations. 3. In the presence of the anaesthetics investigated, IBa measured at the end of the depolarizing test pulse showed proportionally greater depression than that at measured peak amplitude, as well as significant decrease in the rate of activation or increase in inactivation or both. -
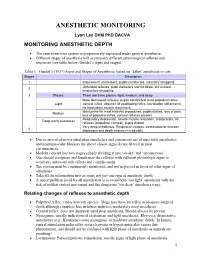

Monitoring Anesthetic Depth
ANESTHETIC MONITORING Lyon Lee DVM PhD DACVA MONITORING ANESTHETIC DEPTH • The central nervous system is progressively depressed under general anesthesia. • Different stages of anesthesia will accompany different physiological reflexes and responses (see table below, Guedel’s signs and stages). Table 1. Guedel’s (1937) Signs and Stages of Anesthesia based on ‘Ether’ anesthesia in cats. Stages Description 1 Inducement, excitement, pupils constricted, voluntary struggling Obtunded reflexes, pupil diameters start to dilate, still excited, 2 involuntary struggling 3 Planes There are three planes- light, medium, and deep More decreased reflexes, pupils constricted, brisk palpebral reflex, Light corneal reflex, absence of swallowing reflex, lacrimation still present, no involuntary muscle movement. Ideal plane for most invasive procedures, pupils dilated, loss of pain, Medium loss of palpebral reflex, corneal reflexes present. Respiratory depression, severe muscle relaxation, bradycardia, no Deep (early overdose) reflexes (palpebral, corneal), pupils dilated Very deep anesthesia. Respiration ceases, cardiovascular function 4 depresses and death ensues immediately. • Due to arrival of newer inhalation anesthetics and concurrent use of injectable anesthetics and neuromuscular blockers the above classic signs do not fit well in most circumstances. • Modern concept has two stages simply dividing it into ‘awake’ and ‘unconscious’. • One should recognize and familiarize the reflexes with different physiologic signs to avoid any untoward side effects and complications • The system must be continuously monitored, and not neglected in favor of other signs of anesthesia. • Take all the information into account, not just one sign of anesthetic depth. • A major problem faced by all anesthetists is to avoid both ‘too light’ anesthesia with the risk of sudden violent movement and the dangerous ‘too deep’ anesthesia stage. -

Jebmh.Com Original Research Article
Jebmh.com Original Research Article A COMPARATIVE STUDY OF SMALL DOSE OF KETAMINE, MIDAZOLAM AND PROPOFOL AS COINDUCTION AGENT TO PROPOFOL Abhimanyu Kalita1, Abu Lais Mustaq Ahmed2 1Senior Resident, Department of Anaesthesiology, Assam Medical College, Dibrugarh. 2Associate Professor, Department of Anaesthesiology, Assam Medical College, Dibrugarh. ABSTRACT BACKGROUND The technique of “coinduction”, i.e. use of a small dose of sedative agent or another anaesthetic agent reduces the dose requirement as well as adverse effects of the main inducing agent. Ketamine, midazolam and propofol have been used as coinduction agents with propofol. MATERIALS AND METHODS This prospective, randomised clinical study compared to three methods of coinduction. One group received ketamine, one group received midazolam and one group received propofol as coinducing agent with propofol. RESULTS The study showed that the group receiving ketamine as coinduction agent required least amount of propofol for induction and was also associated with lesser side effects. CONCLUSION Use of ketamine as coinduction agent leads to maximum reduction of induction dose of propofol and also lesser side effects as compared to propofol and midazolam. KEYWORDS Coinduction, Propofol, Midazolam, Ketamine. HOW TO CITE THIS ARTICLE: Kalita A, Ahmed ALM. A comparative study of small dose of ketamine, midazolam and propofol as coinduction agent to propofol. J. Evid. Based Med. Healthc. 2017; 4(64), 3820-3825. DOI: 10.18410/jebmh/2017/763 BACKGROUND But, the major disadvantage of propofol induction are Propofol is the most frequently used IV anaesthetic agent impaired cardiovascular and respiratory function, which may used today with a desirable anaesthetic profile. It provides put the patients at a higher risk of bradycardia, hypotension faster onset of action, antiemesis, rapid recovery with and apnoea. -

Nerve Blocks for Surgery on the Shoulder, Arm Or Hand
Nerve blocks for surgery on the shoulder, arm or hand Information for patients and families First Edition 2015 www.rcoa.ac.uk/patientinfo Nerve blocks for surgery on the shoulder, arm or hand This leaflet is for anyone who is thinking about having a nerve block for an operation on the shoulder, arm or hand. It will be of particular interest to people who would prefer not to have a general anaesthetic. The leaflet has been written with the help of patients who have had a nerve block for their operation. Throughout this leaflet we have used the above symbol to highlight key facts. Brachial plexus block? The brachial plexus is the group of nerves that lies between your neck and your armpit. It contains all the nerves that supply movement and feeling to your arm – from your shoulder to your fingertips. A brachial plexus block is an injection of local anaesthetic around the brachial plexus. It ‘blocks’ information travelling along these nerves. It is a type of nerve block. Your arm becomes numb and immobile. You can then have your operation without feeling anything. The block can also provide excellent pain relief for between three and 24 hours, depending on what kind of local anaesthetic is used. A brachial plexus block rarely affects the rest of the body so it is particularly advantageous for patients who have medical conditions which put them at a higher risk for a general anaesthetic. A brachial plexus block may be combined with a general anaesthetic or with sedation. This means you have the advantage of the pain relief provided by a brachial plexus block, but you are also unconscious or sedated during the operation. -

Effects of Intraoperative Insufflation with Warmed, Humidified CO2 During Abdominal Surgery: a Review
Annals of Original Article Coloproctology Ann Coloproctol 2018;34(3):125-137 pISSN 2287-9714 eISSN 2287-9722 https://doi.org/10.3393/ac.2017.09.26 www.coloproctol.org Effects of Intraoperative Insufflation With Warmed, Humidified CO2 during Abdominal Surgery: A Review Ju Yong Cheong1,2, Anil Keshava1, Paul Witting2, Christopher John Young1 1Colorectal Surgical Department, Concord Repatriation General Hospital, Sydney Medical School, The University of Sydney, Sydney; 2Discipline of Pathology, Charles Perkins Centre, Sydney Medical School, The University of Sydney, Sydney, Australia Purpose: During a laparotomy, the peritoneum is exposed to the cold, dry ambient air of the operating room (20°C, 0%– 5% relative humidity). The aim of this review is to determine whether the use of humidified and/or warmed CO2 in the intraperitoneal environment during open or laparoscopic operations influences postoperative outcomes. Methods: A review was performed in accordance with PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. The PubMed, OVID MEDLINE, Cochrane Central Register of Controlled Trials and Embase databases were searched for articles published between 1980 and 2016 (October). Comparative studies on humans or nonhuman animals that involved randomized controlled trials (RCTs) or prospective cohort studies were included. Both laparotomy and laparoscopic studies were included. The primary outcomes identified were peritoneal inflammation, core body temperature, and postoperative pain. Results: The literature search identified 37 articles for analysis, including 30 RCTs, 7 prospective cohort studies, 23 human studies, and 14 animal studies. Four studies found that compared with warmed/humidified CO2, cold, dry CO2 resulted in significant peritoneal injury, with greater lymphocytic infiltration, higher proinflammatory cytokine levels and peritoneal adhesion formation.