Inflammation of the Central Nervous System- Encephalitis, Myelitis, and Meningitis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Central Pain in the Face and Head
P1: KWW/KKL P2: KWW/HCN QC: KWW/FLX T1: KWW GRBT050-128 Olesen- 2057G GRBT050-Olesen-v6.cls August 17, 2005 2:10 ••Chapter 128 ◗ Central Pain in the Face and Head J¨orgen Boivie and Kenneth L. Casey CENTRAL PAIN IN THE FACE AND HEAD Anesthesia dolorosa denotes pain in a region with de- creased sensibility after lesions in the CNS or peripheral International Headache Society (IHS) code and diag- nervous system (PNS). The term deafferentation pain is nosis: used for similar conditions, but it is more commonly used in patients with lesions of spinal nerves. 13.18.1 Central causes of facial pain 13.18.1 Anesthesia dolorosa (+ code to specify cause) 13.18.2 Central poststroke pain EPIDEMIOLOGY 13.18.3 Facial pain attributed to multiple sclerosis 13.18.4 Persistent idiopathic facial pain The prevalence of central pain varies depending on the un- 13.18.5 Burning mouth syndrome derlying disorder (Tables 128-1 and 128-2) (7,29). In the ab- 13.19 Other centrally mediated facial pain (+ code to sence of large scale epidemiologic studies, only estimates specify etiology) of central pain prevalence can be quoted. In the only prospective epidemiologic study of central Note that diagnosis with IHS codes 13.18.1, 13.18.4, and pain, 191 patients with central poststroke pain (CPSP) 13.18.5 may have peripheral causes. were followed for 12 months after stroke onset (1). Sixteen World Health Organization (WHO) code and diagnosis: (8.4%) developed central pain, an unexpectedly high inci- G 44.810 or G44.847. -

Caspr2 Antibodies in Patients with Thymomas
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector MALIGNANCIES OF THE THYMUS Caspr2 Antibodies in Patients with Thymomas Angela Vincent, FRCPath,* and Sarosh R. Irani, MA* neuromuscular junction. Neuromyotonia (NMT) is due to Abstract: Myasthenia gravis is the best known autoimmune disease motor nerve hyperexcitability that leads to muscle fascicula- associated with thymomas, but other conditions can be found in tions and cramps. A proportion of patients have antibodies patients with thymic tumors, including some that affect the central that appear to be directed against brain tissue-derived volt- nervous system (CNS). We have become particularly interested in age-gated potassium channels (VGKCs) that control the ax- patients who have acquired neuromyotonia, the rare Morvan disease, onal membrane potential.4,5 VGKC antibody titers are rela- or limbic encephalitis. Neuromyotonia mainly involves the periph- tively low in NMT. eral nerves, Morvan disease affects both the peripheral nervous Morvan disease is a rare condition first described in system and CNS, and limbic encephalitis is specific to the CNS. 1876 but until recently hardly mentioned outside the French Many of these patients have voltage-gated potassium channel auto- literature.6 The patients exhibit NMT plus autonomic distur- antibodies. All three conditions can be associated with thymomas bance (such as excessive sweating, constipation, and cardiac and may respond to surgical removal of the underlying tumor -

Unusual Case of Progressive Multifocal Leukoencephalopathy in a Patient with Sjögren Syndrome
Henry Ford Health System Henry Ford Health System Scholarly Commons Pathology Articles Pathology 1-15-2021 Unusual Case of Progressive Multifocal Leukoencephalopathy in a Patient With Sjögren Syndrome Ifeoma Onwubiko Kanika Taneja Nilesh S. Gupta Abir Mukherjee Follow this and additional works at: https://scholarlycommons.henryford.com/pathology_articles CASE REPORT Unusual Case of Progressive Multifocal Leukoencephalopathy in a Patient With Sjögren Syndrome Ifeoma Ndidi Onwubiko, MD, MPH, Kanika Taneja, MD, Nilesh Gupta, MD, and Abir Mukherjee, MD 03/05/2021 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3i3D0OdRyi7TvSFl4Cf3VC1y0abggQZXdgGj2MwlZLeI= by http://journals.lww.com/amjforensicmedicine from Downloaded 84% neutrophils; glucose, 71 mmol/L; protein, 183 g/dL with neg- Abstract: Progressive multifocal leukoencephalopathy (PML) is a rare Downloaded ative cultures and no malignant cells on cytology). Hepatitis C anti- demyelinating disease caused by reactivation of John Cunningham virus af- body screen was negative. Immunoglobin G antibodies to Sjögren fecting typically subcortical and periventricular white matter of immunocom- syndrome–related antigen A and anti–Sjögren syndrome-related from promised hosts (human immunodeficiency virus infection, hematologic antigen B were positive. Thyroglobulin antibodies and antinuclear http://journals.lww.com/amjforensicmedicine malignancies). Cerebral hemispheric white matter is most commonly affected antibodies were elevated. Autoimmune serological tests for other by lytic -

Neurosyphilis Presenting with Myelitis-Case Series and Literature Review
Neurosyphilis presenting with myelitis-Case series and literature review Yali Wu Capital Medical University Aliated Beijing Ditan Hospital https://orcid.org/0000-0002-9737-6439 Wenqing Wu ( [email protected] ) https://orcid.org/0000-0001-7428-5529 Case report Keywords: Syphilis, Neurosyphilis, Spinal cord, Magnetic resonance imaging Posted Date: April 5th, 2019 DOI: https://doi.org/10.21203/rs.2.1849/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Version of Record: A version of this preprint was published at Journal of Infection and Chemotherapy on February 1st, 2020. See the published version at https://doi.org/10.1016/j.jiac.2019.09.007. Page 1/9 Abstract Background Neurosyphilis is a great imitator because of its various clinical symptoms. Syphilitic myelitis is extremely rare manifestation of neurosyphilis and often misdiagnosed. However, a small amount of literature in the past described its clinical manifestations and imaging features, and there was no relevant data on the prognosis, especially the long-term prognosis. In this paper, 4 syphilis myelitis patients admitted to our hospital between July 2012 and July 2017 were retrospectively reviewed. In the 4 patients, 2 were females, and 2 were males. We present our experiences with syphilitic myelitis, discuss the characteristics, treatment and prognosis. Case presentation The diagnosis criteria were applied: (1) diagnosis of myelitis established by two experienced neurologist based on symptoms and longitudinally extensive transverse myelitis (LETM) at the cervical and thoracic levels mimicked neuromyelitis optic (NMO) on magnetic resonance imaging (MRI) ; (2) Neurosyphilis (NS) was diagnosed by positive treponema pallidum particle assay (TPPA) and toluidine red untreated serum test (TRUST) in the serum and CSF; (3) negative human immunodeciency virus (HIV). -

ICD9 & ICD10 Neuromuscular Codes
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES ICD-9-CM ICD-10-CM Focal Neuropathy Mononeuropathy G56.00 Carpal tunnel syndrome, unspecified Carpal tunnel syndrome 354.00 G56.00 upper limb Other lesions of median nerve, Other median nerve lesion 354.10 G56.10 unspecified upper limb Lesion of ulnar nerve, unspecified Lesion of ulnar nerve 354.20 G56.20 upper limb Lesion of radial nerve, unspecified Lesion of radial nerve 354.30 G56.30 upper limb Lesion of sciatic nerve, unspecified Sciatic nerve lesion (Piriformis syndrome) 355.00 G57.00 lower limb Meralgia paresthetica, unspecified Meralgia paresthetica 355.10 G57.10 lower limb Lesion of lateral popiteal nerve, Peroneal nerve (lesion of lateral popiteal nerve) 355.30 G57.30 unspecified lower limb Tarsal tunnel syndrome, unspecified Tarsal tunnel syndrome 355.50 G57.50 lower limb Plexus Brachial plexus lesion 353.00 Brachial plexus disorders G54.0 Brachial neuralgia (or radiculitis NOS) 723.40 Radiculopathy, cervical region M54.12 Radiculopathy, cervicothoracic region M54.13 Thoracic outlet syndrome (Thoracic root Thoracic root disorders, not elsewhere 353.00 G54.3 lesions, not elsewhere classified) classified Lumbosacral plexus lesion 353.10 Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy 353.50 Neuralgic amyotrophy G54.5 Root Cervical radiculopathy (Intervertebral disc Cervical disc disorder with myelopathy, 722.71 M50.00 disorder with myelopathy, cervical region) unspecified cervical region Lumbosacral root lesions (Degeneration of Other intervertebral disc degeneration, -

Transverse Myelitis Interagency Collaboration
SHNIC Specialized Health Needs Factsheet: Transverse Myelitis Interagency Collaboration What is it? Transverse Myelitis is a neurological disorder caused by inflammation of the spinal cord. A child will experience weakness, pain, sensory and autonomic dysfunction. Auto- nomic, involuntary activities such as breathing, digestion, heartbeat and reflexes can be affected. Symptoms can ap- pear suddenly within hours or progress over a span of sev- eral weeks. Approximately 25% of cases are children. A peak in incidence occurs between ages of 10 and 19 and females are at higher risk than men. During an inflammato- ry response the myelin, or protective fatty coating on nerve cells, is damaged or destroyed. TM can also be the first symptom to diagnose Multiple Sclerosis. What causes it? Researchers believe it is the body’s immune response, not the infection itself, that causes the inflammatory response. This indicates an auto-immune reaction, where the body attacks it’s own tissue rather than the infection, is responsible. Research has made connections to the damage of spinal nerves following a viral or bacterial infection, especially those associated with a rash. According to the National Institute of Neurologic Disorders and Stroke, infectious agents sus- pected of causing TM include Varicella zoster (the virus that causes chickenpox and shingles), Herpes simplex, Cytomegalovirus, Epstein-Barr, Influenza, Echovirus, Human immunodefi- ciency virus (HIV), Hepatitis A, and Rubella. In some cases, bacterial infections like a middle ear infection and bacterial pneumonia have also been linked. What are the symptoms? Symptoms can start slowly and progressively worsen over hours or days. Damage depends on the affected area of the spinal cord. -

CONTENTS EDITORIAL Chronic Fatigue Syndrome
Volume 11 Number 1 2003 CONTENTS EDITORIAL Chronic Fatigue Syndrome Guidelines 1 Kenny De Meirleir Neil McGregor Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols 7 Bruce M. Carruthers Anil Kumar Jain Kenny L. De Meirleir Daniel L. Peterson Nancy G. Klimas A. Martin Lerner Alison C. Bested Pierre Flor-Henry Pradip Joshi A. C. Peter Powles Jeffrey A. Sherkey Marjorie I. van de Sande Recent years have brought growing recognition of the need for clinical criteria for myalgic encephalomyelitis (ME), which is also called chronic fatigue syndrome (CFS). An Expert Subcommittee of Health Canada established the Terms of Refer- ence, and selected an Expert Medical Consensus Panel representing treating physi- cians, teaching faculty and researchers. A Consensus Workshop was held on March 30 to April 1, 2001 to culminate the review process and establish consen- sus for a clinical working case definition, diagnostic protocols and treatment pro- tocols. We present a systematic clinical working case definition that encourages a diagnosis based on characteristic patterns of symptom clusters, which reflect specific areas of pathogenesis. Diagnostic and treatment protocols, and a short overview of research are given to facilitate a comprehensive and integrated ap- proach to this illness. Throughout this paper, “myalgic encephalomyelitis” and “chronic fatigue syndrome” are used interchangeably and this illness is referred to as “ME/CFS.” KEYWORDS. Clinical case definition, myalgic encephalomyelitis, chronic fa- tigue syndrome, ME, CFS, diagnostic protocol, treatment protocol Monitoring a Hypothetical Channelopathy in Chronic Fatigue Syndrome: Preliminary Observations 117 Jo Nijs Christian Demanet Neil R. McGregor Pascale De Becker Michel Verhas Patrick Englebienne Kenny De Meirleir This study was aimed at monitoring of a previously suggested channelopathy in Chronic Fatigue Syndrome, and at searching for possible explanations by means of immune system characteristics. -

Progressive Multifocal Leukoencephalopathy and the Spectrum of JC Virus-Related Disease
REVIEWS Progressive multifocal leukoencephalopathy and the spectrum of JC virus- related disease Irene Cortese 1 ✉ , Daniel S. Reich 2 and Avindra Nath3 Abstract | Progressive multifocal leukoencephalopathy (PML) is a devastating CNS infection caused by JC virus (JCV), a polyomavirus that commonly establishes persistent, asymptomatic infection in the general population. Emerging evidence that PML can be ameliorated with novel immunotherapeutic approaches calls for reassessment of PML pathophysiology and clinical course. PML results from JCV reactivation in the setting of impaired cellular immunity, and no antiviral therapies are available, so survival depends on reversal of the underlying immunosuppression. Antiretroviral therapies greatly reduce the risk of HIV-related PML, but many modern treatments for cancers, organ transplantation and chronic inflammatory disease cause immunosuppression that can be difficult to reverse. These treatments — most notably natalizumab for multiple sclerosis — have led to a surge of iatrogenic PML. The spectrum of presentations of JCV- related disease has evolved over time and may challenge current diagnostic criteria. Immunotherapeutic interventions, such as use of checkpoint inhibitors and adoptive T cell transfer, have shown promise but caution is needed in the management of immune reconstitution inflammatory syndrome, an exuberant immune response that can contribute to morbidity and death. Many people who survive PML are left with neurological sequelae and some with persistent, low-level viral replication in the CNS. As the number of people who survive PML increases, this lack of viral clearance could create challenges in the subsequent management of some underlying diseases. Progressive multifocal leukoencephalopathy (PML) is for multiple sclerosis. Taken together, HIV, lymphopro- a rare, debilitating and often fatal disease of the CNS liferative disease and multiple sclerosis account for the caused by JC virus (JCV). -

Relapsing Polychondritis Presenting with Meningoencephalitis and Dementia: Correlation with Neuroimaging and Clinical Features
30 Relapsing Polychondritis Presenting with Meningoencephalitis and Dementia: Correlation with Neuroimaging and Clinical Features Yung-Pin Hwang1, Richard Kuo2,4, Tien-Ling Chen3, Pei-Hao Chen1,4,5, Shih-Jung Cheng1 Abstract- Purpose: Relapsing polychondritis (RP) is a rare systemic autoimmune disease affecting cartilaginous and non-cartilaginous structures. Neurological involvement is rarer but results in profound disability. Early identification and treatment of underlying RP may promote neurological recovery. Case Report: We illustrated a 53-year-old man diagnosed with dementia. Neuroimaging and cerebrospinal fluid studies disclosed meningoencephalitis. “Prominent ear sign” was evident on diffusion-weight magnetic resonance imaging. After glucocortisone administration, the improvement of clinical manifestations was closely correlated subsequent neuroimaging findings. Conclusion: The importance of better understanding of this disease in terms of the prevention of further tissue damage in patients with RP cannot be overemphasized. Key Words: relapsing polychondritis, auricular chondritis, meningoncephalitis, dementia, prominent ear sign Acta Neurol Taiwan 2015;24:30-33 INTRODUCTION of RP are protean dependent on tissue involvement. Early identification of PR and prompt intervention might be Relapsing polychondritis (RP) is a rare multisystem beneficial for its prognosis. Nervous system involvement disorder affecting cartilaginous tissue including the hyaline can manifest as meningoencephalitis (4), dementia (5), stroke cartilage of joints and the fibrocartilage of extra-articular (6), and parkinsonism (7). Awareness of RP may prevent location, as well as proteoglycan-rich structures such the subsequent disability secondary to irreversible brain or (1) media of the arteritis and eye . Its pathogenesis appears nerve tissue damage. to be an immune-mediated reaction against collagen type We report a case with meningoencephalitis and (2) (3) II , collagens type IX and XI . -
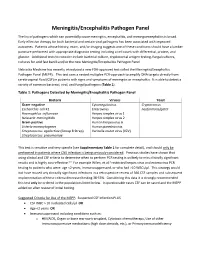
Meningitis/Encephalitis Pathogen Panel
Meningitis/Encephalitis Pathogen Panel The list of pathogens which can potentially cause meningitis, encephalitis, and meningoencephalitis is broad. Early effective therapy for both bacterial and certain viral pathogens has been associated with improved outcomes. Patients whose history, exam, and/or imaging suggests one of these conditions should have a lumber puncture performed with appropriate diagnostic testing including a cell count with differential, protein, and glucose. Additional tests to consider include bacterial culture, cryptococcal antigen testing, fungal cultures, cultures for acid fast bacilli and/or the new Meningitis/Encephalitis Pathogen Panel. Nebraska Medicine has recently introduced a new FDA-approved test called the Meningitis/Encephalitis Pathogen Panel (MEPP). This test uses a nested multiplex PCR-approach to amplify DNA targets directly from cerebrospinal fluid (CSF) in patients with signs and symptoms of meningitis or encephalitis. It is able to detect a variety of common bacterial, viral, and fungal pathogens (Table 1). Table 1: Pathogens Detected by Meningitis/Encephalitis Pathogen Panel Bacteria Viruses Yeast Gram-negative Cytomegalovirus Cryptococcus Escherichia coli K1 Enterovirus neoformans/gattii Haemophilus influenzae Herpes simplex virus 1 Neisseria meningitidis Herpes simplex virus 2 Gram-positive Human herpesvirus 6 Listeria monocytogenes Human parechovirus Streptococcus agalactiae (Group B Strep) Varicella zoster virus (VZV) Streptococcus pneumoniae This test is sensitive and very specific (see Supplementary Table 1 for complete detail), and should only be performed in patients where CNS infection is being seriously considered. Previous studies have shown that using clinical and CSF criteria to determine when to perform PCR testing is unlikely to miss clinically significant results and is highly cost-effective.1-3 For example Wilen, et al.3 restricted herpes virus and enterovirus PCR testing to patients who were: age <2 years, immunosuppressed, or who had >10 WBCs/µl. -

Syringomyelia and Arachnoiditis
106 Journal of Neurology, Neurosurgery, and Psychiatry 1990;53:106-113 Syringomyelia and arachnoiditis L R Caplan, A B Norohna, L L Amico Abstract and weakness in his right hand. Months later, Five patients with chronic arachnoiditis he developed sensory loss and weakness of the and syringomyelia were studied. Three hands, more noticeable in the left than the patients had early life meningitis and right. Atrophy, frequent burns, and hand developed symptoms of syringomyelia tremor were reported by the patient. Four eight, 21, and 23 years after the acute years later, the lower extremities became weak, infection. One patient had a spinal dural initially on the right side. He then experienced thoracic AVM and developed a thoracic weakness in the left leg which soon became syrinx 11 years after spinal subarachnoid more severe than in the right. He complained of haemorrhage and five years after surgery a drawing, burning pain in both arms from the on the AVM. A fifth patient had tuber- hands to the radial forearms and from the hips culous meningitis with transient spinal to the toes. cord dysfunction followed by develop- In 1943 (aged 46), he was first evaluated at ment ofa lumbar syrinx seven years later. the Harvard Neurological Unit at Boston City Arachnoiditis can cause syrinx formation Hospital. There was diminished body hair and by obliterating the spinal vasculature burn scars on his fingers. Mental function and causing ischaemia. Small cystic regions cranial nerves were normal except for a slight of myelomalacia coalesce to form left lower facial droop and slighlt leftward cavities. In other patients, central cord protrusion of the tongue. -

Paraneoplastic Neurological and Muscular Syndromes
Paraneoplastic neurological and muscular syndromes Short compendium Version 4.5, April 2016 By Finn E. Somnier, M.D., D.Sc. (Med.), copyright ® Department of Autoimmunology and Biomarkers, Statens Serum Institut, Copenhagen, Denmark 30/01/2016, Copyright, Finn E. Somnier, MD., D.S. (Med.) Table of contents PARANEOPLASTIC NEUROLOGICAL SYNDROMES .................................................... 4 DEFINITION, SPECIAL FEATURES, IMMUNE MECHANISMS ................................................................ 4 SHORT INTRODUCTION TO THE IMMUNE SYSTEM .................................................. 7 DIAGNOSTIC STRATEGY ..................................................................................................... 12 THERAPEUTIC CONSIDERATIONS .................................................................................. 18 SYNDROMES OF THE CENTRAL NERVOUS SYSTEM ................................................ 22 MORVAN’S FIBRILLARY CHOREA ................................................................................................ 22 PARANEOPLASTIC CEREBELLAR DEGENERATION (PCD) ...................................................... 24 Anti-Hu syndrome .................................................................................................................. 25 Anti-Yo syndrome ................................................................................................................... 26 Anti-CV2 / CRMP5 syndrome ............................................................................................