Submandibular Gland Excision
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Salivary Gland Infections and Salivary Stones (Sialadentis and Sialithiasis)
Salivary Gland Infections and Salivary Stones (Sialadentis and Sialithiasis) What is Sialadenitis and Sialithiasis? Sialdenitis is an infection of the salivary glands that causes painful swelling of the glands that produce saliva, or spit. Bacterial infections, diabetes, tumors or stones in the salivary glands, and tooth problems (poor oral hygiene) may cause a salivary gland infection. The symptoms include pain, swelling, pus in the mouth, neck skin infection. These infections and affect the submandibular gland (below the jaw) or the parotid glands (in front of the ears). The symptoms can be minor and just be a small swelling after meals (symptoms tend to be worse after times of high saliva flow). Rarely, the swelling in the mouth will progress and can cut off your airway and cause you to stop breathing. What Causes Sialadenitis and Sialithiasis When the flow of saliva is blocked by a small stone (salilithiasis) in a salivary gland or when a person is dehydrated, bacteria can build up and cause an infection. A viral infection, such as the mumps, also can cause a salivary gland to get infected and swell. These infections can also be caused by a spread from rotten or decaying teeth. Sometimes there can be a buildup of calcium in the saliva ducts that form into stones. These can easily stop the flow of saliva and cause problems How are these infections and stones treated? Treatment depends on what caused your salivary gland infection. If the infection is caused by bacteria, your doctor may prescribe antibiotics. Home treatment such as drinking fluids, applying warm compresses, and sucking on lemon wedges or sour candy to increase saliva may help to clear the infection quicker. -

Abscesses Apicectomy
BChD, Dip Odont. (Mondchir.) MBChB, MChD (Chir. Max.-Fac.-Med.) Univ. of Pretoria Co Reg: 2012/043819/21 Practice.no: 062 000 012 3323 ABSCESSES WHAT IS A TOOTH ABSCESS? A dental/tooth abscess is a localised acute infection at the base of a tooth, which requires immediate attention from your dentist. They are usually associated with acute pain, swelling and sometimes an unpleasant smell or taste in the mouth. More severe infections cause facial swelling as the bacteria spread to the nearby tissues of the face. This is a very serious condition. Once the swelling begins, it can spread rapidly. The pain is often made worse by drinking hot or cold fluids or biting on hard foods and may spread from the tooth to the ear or jaw on the same side. WHAT CAUSES AN ABSCESS? Damage to the tooth, an untreated cavity, or a gum disease can cause an abscessed tooth. If the cavity isn’t treated, the inside of the tooth can become infected. The bacteria can spread from the tooth to the tissue around and beneath it, creating an abscess. Gum disease causes the gums to pull away from the teeth, leaving pockets. If food builds up in one of these pockets, bacteria can grow, and an abscess may form. An abscess can cause the bone around the tooth to dissolve. WHY CAN'T ANTIBIOTIC TREATMENT ALONE BE USED? Antibiotics will usually help the pain and swelling associated with acute dental infections. However, they are not very good at reaching into abscesses and killing all the bacteria that are present. -

Head and Neck
DEFINITION OF ANATOMIC SITES WITHIN THE HEAD AND NECK adapted from the Summary Staging Guide 1977 published by the SEER Program, and the AJCC Cancer Staging Manual Fifth Edition published by the American Joint Committee on Cancer Staging. Note: Not all sites in the lip, oral cavity, pharynx and salivary glands are listed below. All sites to which a Summary Stage scheme applies are listed at the begining of the scheme. ORAL CAVITY AND ORAL PHARYNX (in ICD-O-3 sequence) The oral cavity extends from the skin-vermilion junction of the lips to the junction of the hard and soft palate above and to the line of circumvallate papillae below. The oral pharynx (oropharynx) is that portion of the continuity of the pharynx extending from the plane of the inferior surface of the soft palate to the plane of the superior surface of the hyoid bone (or floor of the vallecula) and includes the base of tongue, inferior surface of the soft palate and the uvula, the anterior and posterior tonsillar pillars, the glossotonsillar sulci, the pharyngeal tonsils, and the lateral and posterior walls. The oral cavity and oral pharynx are divided into the following specific areas: LIPS (C00._; vermilion surface, mucosal lip, labial mucosa) upper and lower, form the upper and lower anterior wall of the oral cavity. They consist of an exposed surface of modified epider- mis beginning at the junction of the vermilion border with the skin and including only the vermilion surface or that portion of the lip that comes into contact with the opposing lip. -

Basic Histology (23 Questions): Oral Histology (16 Questions
Board Question Breakdown (Anatomic Sciences section) The Anatomic Sciences portion of part I of the Dental Board exams consists of 100 test items. They are broken up into the following distribution: Gross Anatomy (50 questions): Head - 28 questions broken down in this fashion: - Oral cavity - 6 questions - Extraoral structures - 12 questions - Osteology - 6 questions - TMJ and muscles of mastication - 4 questions Neck - 5 questions Upper Limb - 3 questions Thoracic cavity - 5 questions Abdominopelvic cavity - 2 questions Neuroanatomy (CNS, ANS +) - 7 questions Basic Histology (23 questions): Ultrastructure (cell organelles) - 4 questions Basic tissues - 4 questions Bone, cartilage & joints - 3 questions Lymphatic & circulatory systems - 3 questions Endocrine system - 2 questions Respiratory system - 1 question Gastrointestinal system - 3 questions Genitouirinary systems - (reproductive & urinary) 2 questions Integument - 1 question Oral Histology (16 questions): Tooth & supporting structures - 9 questions Soft oral tissues (including dentin) - 5 questions Temporomandibular joint - 2 questions Developmental Biology (11 questions): Osteogenesis (bone formation) - 2 questions Tooth development, eruption & movement - 4 questions General embryology - 2 questions 2 National Board Part 1: Review questions for histology/oral histology (Answers follow at the end) 1. Normally most of the circulating white blood cells are a. basophilic leukocytes b. monocytes c. lymphocytes d. eosinophilic leukocytes e. neutrophilic leukocytes 2. Blood platelets are products of a. osteoclasts b. basophils c. red blood cells d. plasma cells e. megakaryocytes 3. Bacteria are frequently ingested by a. neutrophilic leukocytes b. basophilic leukocytes c. mast cells d. small lymphocytes e. fibrocytes 4. It is believed that worn out red cells are normally destroyed in the spleen by a. neutrophils b. -

SUBMANDIBULAR GLAND REMOVAL Post Operative Instructions
SUBMANDIBULAR GLAND REMOVAL Post Operative Instructions Nurse Line (8:30am to 5pm) 937-496-0261 Emergency After Hours Line 937-496-2600 The Surgery Itself Surgery to remove the submandibular gland involves general anesthesia, typically for about two hours. Patients may be quite sedated for several hours after surgery and may remain sleepy for much of the day. Nausea and vomiting are occasionally seen, and usually resolve by the evening of surgery - even without additional medications. Some patients stay overnight in the hospital; other patients can go home the evening of surgery. Some patients will have a drain in place after surgery; this is removed the following day before you go home from the hospital or in the office 1-2 days after surgery. Your Incision Your incision is closed with absorbable sutures and is covered with a small strip of tape or skin glue. You can shower and wash your hair as usual starting 24 hours after your drain is removed. If you did not have a drain in place after surgery, you may shower 24 hours after surgery. You may wash in a bathtub prior to that time if you are careful not to get your neck wet. Use a dab of Bacitracin ointment on your drain site (on one side of your incision, not covered by the tape or glue) before and after showering. Do not soak or scrub the incision. You might notice bruising around your incision or jaw line and slight swelling above the scar when you are upright. In addition, the scar may become pink and hard. -

Submandibular Gland Transfer for Prevention of Xerostomia After Radiation Therapy Swallowing Outcomes
ORIGINAL ARTICLE Submandibular Gland Transfer for Prevention of Xerostomia After Radiation Therapy Swallowing Outcomes Jana Rieger, PhD; Hadi Seikaly, MD; Naresh Jha, MBBS; Jeffrey Harris, MD; David Williams, MD; Richard Liu, MD; Tim McGaw, DDS; John Wolfaardt, PhD Objective: To assess swallowing outcomes in patients had preservation of 1 submandibular gland (SJP group) with oropharyngeal carcinoma in relation to the Seikaly- and 11 who did not (control group). Jha procedure for submandibular gland transfer (SJP). The SJP has recently been described as beneficial in the Main Outcome Measures: Quantitative and qualita- prevention of xerostomia induced by radiation therapy tive aspects of swallowing were obtained to determine in patients with head and neck cancer. whether patients in the SJP group performed more op- timally than those in the control group. Design: Inception cohort. Results: Baseline and stimulated salivary flow rates were Setting: University-affiliated primary care center. significantly different between groups. Patients in the SJP group were able to move the bolus through the oral cavity Patients: A phase 2 clinical trial was conducted from and into the pharynx faster than those in the control group. February 1, 1999, through February 28, 2002, to evalu- In addition, patients in the SJP group swallowed less often ate SJP in patients with head and neck cancer. During per bolus than patients in the control group. The com- that period, a consecutive sample of 51 patients who un- plete swallowing sequence was twice as long in controls. derwent surgical resection and reconstruction with a ra- dial forearm free flap for oropharyngeal carcinoma were Conclusions: The SJP for submandibular gland trans- referred for functional assessment of swallowing after fer appears to be beneficial in promoting more time- completion of adjuvant radiation therapy. -

A Guide to Salivary Gland Disorders the Salivary Glands May Be Affected by a Wide Range of Neoplastic and Inflammatory
MedicineToday PEER REVIEWED ARTICLE CPD 1 POINT A guide to salivary gland disorders The salivary glands may be affected by a wide range of neoplastic and inflammatory disorders. This article reviews the common salivary gland disorders encountered in general practice. RON BOVA The salivary glands include the parotid glands, examination are often adequate to recognise and MB BS, MS, FRACS submandibular glands and sublingual glands differentiate many of these conditions. A wide (Figure 1). There are also hundreds of minor sali- array of benign and malignant neoplasms may also Dr Bova is an ENT, Head and vary glands located in the mucosa of the hard and affect the salivary glands and a neoplasia should Neck Surgeon, St Vincent’s soft palate, oral cavity, lips, tongue and oro - always be considered when assessing a salivary Hospital, Sydney, NSW. pharynx. The parotid gland lies in the preauricular gland mass. region and extends inferiorly over the angle of the mandible. The parotid duct courses anteriorly Inflammatory disorders from the parotid gland and enters the mouth Acute sialadenitis through the buccal mucosa adjacent to the second Acute inflammation of the salivary glands is usu- upper molar tooth. The submandibular gland lies ally of viral or bacterial origin. Mumps is the most in the submandibular triangle and its duct passes common causative viral illness, typically affecting anteriorly along the floor of the mouth to enter the parotid glands bilaterally. Children are most adjacent to the frenulum of the tongue. The sub- often affected, with peak incidence occurring at lingual glands are small glands that lie just beneath approximately 4 to 6 years of age. -

Major Salivary Gland Neoplasms
Pitfalls in the Staging of Cancer of the Major Salivary Gland Neoplasms Elliott R. Friedman, MDa,*, Amit M. Saindane, MDb KEYWORDS Salivary glands Adenoid cystic carcinoma Benign mixed tumor Carcinoma ex pleomorphic adenoma KEY POINTS The major salivary glands consist of the parotid, submandibular, and sublingual glands. Most neoplasms in other subsites in the head and neck are squamous cell carcinoma, but tumors of the salivary glands may be benign or malignant. Surgical treatment differs if the lesion is benign, and therefore preoperative fine-needle aspiration is important in salivary neoplasms. The role of imaging is to attempt to determine histology, predict likelihood of a lesion being malig- nant, and report an imaging stage. This article reviews the various histologies, imaging features, and staging of major salivary gland neoplasms. ANATOMY AND BOUNDARIES gland is a single contiguous structure, for surgical convenience it has been divided into superficial The major salivary glands consist of the parotid, and deep lobes by the course of the facial nerve, submandibular, and sublingual glands. Submu- which courses lateral to the retromandibular vein. cosal clusters of salivary tissue located in the Most neoplasms arise in the superficial portion of palate, oral cavity, paranasal sinuses, and upper the gland.3 Considerable variation in intraparotid aerodigestive tract are minor salivary glands, and facial nerve anatomy exists, but most commonly are variable in distribution. Primary neoplasms the nerve enters the posteromedial aspect of the arising in the minor salivary glands are staged 1 gland and divides into 2 main trunks before dividing according to the anatomic site of origin. -

Head and Neck Contouring
Practical Medical Physics: Head and Neck Contouring AAPM 2011 Vancouver, British Columbia Jonn Wu, BMSc MD FRCPC Radiation Oncologist, Vancouver Cancer Centre, BCCA Clinical Assistant Professor, UBC August 2nd, 2011 Objectives Review Selection of Normal Organs • Brachial Plexus • Pharyngeal Constrictors • Salivary Glands • Parotid • Submandibular Target Audience: • Physicists • Dosimetrists • Radiation Therapists Outline Why do we have to Contour? Which Organs are Important? How *I* contour? 3 Important Organ Systems • Xerostomia: Salivary Glands • Parotid • Submandibular • Dysphagia: Pharyngeal Constrictors • Brachial Plexus Outline (cont) For Each Organ System • Anatomy • Literature • Examples Why do we have to contour? • Target delineation • Organ avoidance 2D → 3D → IMRT (your fault) 2D Planning 2D Planning 2.5D… 3DCRT IMRT IMRT & Contours • Inverse Planning • Objective Cost Function • Computers are Binary Why take a contouring course? • IMRT and 3D = standard practice • Both techniques require (accurate) contours • Clinical trials require dose constraints • Consistency (precision) • Who: • Intra- vs inter-contourer • Intra- vs inter-institutional • Why: • Good practice • Dose constraints • Dosimetric repositories Why take a contouring course? • No formal training • Few reproducible guidelines • Everyone assumes consistent contouring • NCIC HN6, RTOG 0920, 0615, 0225 • Spinal Cord: • Intra-observer: avg 0.1 cm, max 0.7 cm • Inter-observer: avg 0.2 cm, max 0.9 cm Geets RO 2005 Which organs are important Brain (temporal lobe) Globe, -

Chapter 1 Oral Structures and Tissues Arthur R
Chapter 1 Oral Structures and Tissues Arthur R. Hand1 and Marion E. Frank2 1 Department of Craniofacial Sciences and Cell Biology , School of Dental Medicine, University of Connecticut 2 Department of Oral Health and Diagnostic Sciences , University of Connecticut The oral cavity and its component cells, tissues, and structures the lips and the mucosa lining the inside of the lips, and extends constitute a unique and complex organ system and environment. posteriorly to the palatoglossal folds or arch . Beyond the palato- Of necessity, we study its various parts individually, but the glossal folds are the palatopharyngeal folds and the beginning health and function of the components of the oral cavity depend of the oropharynx , where the digestive and respiratory tracts upon and influence one another. Importantly, the oral cavity come together. The palatine tonsils are located in the tonsillar relies on as well as influences the health and function of the fauces between the palatoglossal and palatopharyngeal folds. entire body. The lymphoid tissue of the palatine tonsils, along with that of the The oral cavity is the gateway to the body, and most of the pharyngeal tonsil ( adenoids ) and the lingual tonsils , guards the substances that enter our bodies do so through the oral cavity. It entrance to the oropharynx. Anteriorly, the respiratory tract is exposed to the physical insults of mastication, hard objects and (nasal cavity) is separated from the oral cavity by the hard palate , various food substances, and extremes of temperature. A variety and posteriorly by the soft palate . The hard palate has an arch-like of chemicals, including those present in foods and drinks and shape that varies in width and height among individuals. -

Submandibular Gland Excision
Submandibular Gland Removal The submandibular gland (also called submaxillary gland) is a salivary gland about the size of a plum that lies immediately below the lower jaw. The most common reason for removing a submandibular gland is chronic infection that occurs if the ducts that drain saliva become blocked, such as with a stone. Other indications for surgery include benign or malignant tumors. The submandibular gland is removed under a general anesthetic. An incision around two inches long is made in the upper part of the neck just below the lower jaw. The gland is mobilized away from the surrounding muscles, vessels, and nerves. Risks of surgery include bleeding from the wound, which is quite unlikely but may require a second surgery. Infection is also uncommon, but you may be placed on antibiotics after surgery. Unexpected scarring can also occur. Very rarely, some leakage of saliva fluid may occur in instances where the gland was partially removed. Bruising of the neck can occur around and below the wound. The removal of one submandibular gland will generally not have a noticeable impact on the amount of saliva that you produce. There are many other salivary glands left in and around the mouth that will still keep it moist. There are three nerves that lie close to the submandibular gland that can be damaged during its removal. Most nerve damage occurs as a result of bruising of the nerves since they are held out of the way and protected during surgery. If nerve damage occurs it is usually temporary. There are three nerves that can be damaged, all with varying results. -
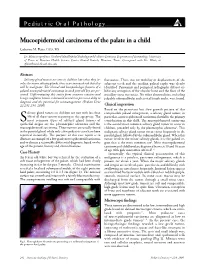
Mucoepidermoid Carcinoma of the Palate in a Child
Pediatric Oral Pathology Mucoepidermoid carcinoma of the palate in a child Catherine M. Flaitz, DDS, MS Dr. Flaitz is a professor, Oral and Maxillofacial Pathology and Pediatric Dentistry, Department of Stomatology, University of Texas at Houston Health Science Center Dental Branch, Houston, Texas. Correspond with Dr. Flaitz at [email protected] Abstract Salivary gland tumors are rare in children but when they in- fluctuance. There was no mobility or displacement of the volve the minor salivary glands, there is an increased risk that they adjacent teeth and the median palatal raphe was clearly will be malignant. The clinical and histopathologic features of a identified. Panoramic and periapical radiographs did not ex- palatal mucoepidermoid carcinoma in an 8 year-old boy are pre- hibit any resorption of the alveolar bone and the floor of the sented. Differentiating this entity from common reactive and maxillary sinus was intact. No other abnormalities, including benign neoplastic lesions is discussed in order to prevent a delay in palpable submandibular and cervical lymph nodes, were found. diagnosis and the potential for mismanagement. (Pediatr Dent 22:292-293, 2000) Clinical impression Based on the persistent but slow growth pattern of this alivary gland tumors in children are rare with less than compressible palatal enlargement, a salivary gland tumor, in 5% of all these tumors occurring in this age group. The particular, a mucoepidermoid carcinoma should be the primary Smost common types of salivary gland tumors of consideration in this child. The mucoepidermoid carcinoma epithelial origin are the pleomorphic adenoma and the is the second most common salivary gland tumor to occur in mucoepidermoid carcinoma.