Section 21 Ophthalmological Preparations Bevacizumab
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Response to Trastuzumab, Erlotinib, and Bevacizumab, Alone and In
2664 Response to trastuzumab, erlotinib, and bevacizumab, alone and in combination, is correlated with the level of human epidermal growth factor receptor-2 expression in human breast cancer cell lines David R. Emlet, Kathryn A. Brown, not increase apoptosis substantially. These studies sug- Deborah L. Kociban, Agnese A. Pollice, gest that the effects of two and three-drug combinations Charles A. Smith, Ben Brian L. Ong, of trastuzumab, erlotinib, and bevacizumab might offer and Stanley E. Shackney potential therapeutic advantages in HER2-overexpressing breast cancers, although these effects are of low Laboratory of Cancer Cell Biology and Genetics, Department of magnitude, and are likely to be transient. [Mol Cancer Human Oncology, Drexel University College of Medicine and the Ther 2007;6(10):2664–74] Allegheny-Singer Research Institute, Allegheny General Hospital, Pittsburgh, Pennsylvania Introduction Human epidermal growth factor receptor-2 (HER2), a Abstract member of the epidermal growth factor receptor (EGFR) Human epidermal growth factor receptor-2 (HER2) and family of tyrosine kinases, is overexpressed in 25% to 30% epidermal growth factor receptor (EGFR) heterodimerize to of human breast cancers (1). It has been implicated in activate mitogenic signaling pathways. We have shown cancer progression (2, 3), and has been identified as a previously, using MCF7 subcloned cell lines with graded prognostic and predictive marker for breast cancer out- levels of HER2 expression, that responsiveness to trastu- come (4). Clinically, chemotherapeutic -

DRUGS REQUIRING PRIOR AUTHORIZATION in the MEDICAL BENEFIT Page 1
Effective Date: 08/01/2021 DRUGS REQUIRING PRIOR AUTHORIZATION IN THE MEDICAL BENEFIT Page 1 Therapeutic Category Drug Class Trade Name Generic Name HCPCS Procedure Code HCPCS Procedure Code Description Anti-infectives Antiretrovirals, HIV CABENUVA cabotegravir-rilpivirine C9077 Injection, cabotegravir and rilpivirine, 2mg/3mg Antithrombotic Agents von Willebrand Factor-Directed Antibody CABLIVI caplacizumab-yhdp C9047 Injection, caplacizumab-yhdp, 1 mg Cardiology Antilipemic EVKEEZA evinacumab-dgnb C9079 Injection, evinacumab-dgnb, 5 mg Cardiology Hemostatic Agent BERINERT c1 esterase J0597 Injection, C1 esterase inhibitor (human), Berinert, 10 units Cardiology Hemostatic Agent CINRYZE c1 esterase J0598 Injection, C1 esterase inhibitor (human), Cinryze, 10 units Cardiology Hemostatic Agent FIRAZYR icatibant J1744 Injection, icatibant, 1 mg Cardiology Hemostatic Agent HAEGARDA c1 esterase J0599 Injection, C1 esterase inhibitor (human), (Haegarda), 10 units Cardiology Hemostatic Agent ICATIBANT (generic) icatibant J1744 Injection, icatibant, 1 mg Cardiology Hemostatic Agent KALBITOR ecallantide J1290 Injection, ecallantide, 1 mg Cardiology Hemostatic Agent RUCONEST c1 esterase J0596 Injection, C1 esterase inhibitor (recombinant), Ruconest, 10 units Injection, lanadelumab-flyo, 1 mg (code may be used for Medicare when drug administered under Cardiology Hemostatic Agent TAKHZYRO lanadelumab-flyo J0593 direct supervision of a physician, not for use when drug is self-administered) Cardiology Pulmonary Arterial Hypertension EPOPROSTENOL (generic) -

Bevacizumab) Injection, for Intravenous Use Persistent, Recurrent, Or Metastatic Cervical Cancer (2.6) Initial U.S
HIGHLIGHTS OF PRESCRIBING INFORMATION First-Line Nonsquamous nonsmall cell lung cancer (2.3) These highlights do not include all the information needed to use • 15 mg/kg every 3 weeks with carboplatin and paclitaxel AVASTIN safely and effectively. See full prescribing information for Recurrent glioblastoma (2.4) AVASTIN. • 10 mg/kg every 2 weeks Metastatic renal cell cancer (2.5) • 10 mg/kg every 2 weeks with interferon alfa AVASTIN (bevacizumab) injection, for intravenous use Persistent, recurrent, or metastatic cervical cancer (2.6) Initial U.S. Approval: 2004 • 15 mg/kg every 3 weeks with paclitaxel and cisplatin, or paclitaxel and topotecan WARNING: GASTROINTESTINAL PERFORATIONS, SURGERY Platinum-resistant recurrent epithelial ovarian, fallopian tube or primary AND WOUND HEALING COMPLICATIONS, and HEMORRHAGE peritoneal cancer (2.7) See full prescribing information for complete boxed warning. • 10 mg/kg every 2 weeks with paclitaxel, pegylated liposomal doxorubicin, Gastrointestinal Perforations: Discontinue for gastrointestinal or topotecan given every week perforation. (5.1) • 15 mg/kg every 3 weeks with topotecan given every 3 weeks Surgery and Wound Healing Complications: Discontinue in Platinum-sensitive recurrent epithelial ovarian, fallopian tube, or primary patients who develop wound healing complications that require peritoneal cancer (2.7) medical intervention. Withhold for at least 28 days prior to • 15 mg/kg every 3 weeks with carboplatin and paclitaxel for 6-8 cycles, elective surgery. Do not administer Avastin for at least 28 days followed by 15 mg/kg every 3 weeks as a single agent after surgery and until the wound is fully healed. (5.2) • 15 mg/kg every 3 weeks with carboplatin and gemcitabine for 6-10 cycles, Hemorrhage: Severe or fatal hemorrhages have occurred. -

Therapeutic Inhibition of VEGF Signaling and Associated Nephrotoxicities
REVIEW www.jasn.org Therapeutic Inhibition of VEGF Signaling and Associated Nephrotoxicities Chelsea C. Estrada,1 Alejandro Maldonado,1 and Sandeep K. Mallipattu1,2 1Division of Nephrology, Department of Medicine, Stony Brook University, Stony Brook, New York; and 2Renal Section, Northport Veterans Affairs Medical Center, Northport, New York ABSTRACT Inhibition of vascular endothelial growth factor A (VEGFA)/vascular endothelial with hypertension and proteinuria. Re- growth factor receptor 2 (VEGFR2) signaling is a common therapeutic strategy in ports describe histologic changes in the oncology, with new drugs continuously in development. In this review, we consider kidney primarily as glomerular endothe- the experimental and clinical evidence behind the diverse nephrotoxicities associ- lial injury with thrombotic microangiop- ated with the inhibition of this pathway. We also review the renal effects of VEGF athy (TMA).8 Nephrotic syndrome has inhibition’s mediation of key downstream signaling pathways, specifically MAPK/ also been observed,9 with the clinical ERK1/2, endothelial nitric oxide synthase, and mammalian target of rapamycin manifestations varying according to (mTOR). Direct VEGFA inhibition via antibody binding or VEGF trap (a soluble decoy mechanism and direct target of VEGF receptor) is associated with renal-specific thrombotic microangiopathy (TMA). Re- inhibition. ports also indicate that tyrosine kinase inhibition of the VEGF receptors is prefer- Current VEGF inhibitors can be clas- entially associated with glomerulopathies such as minimal change disease and FSGS. sifiedbytheirtargetofactioninthe Inhibition of the downstream pathway RAF/MAPK/ERK has largely been associated VEGFA-VEGFR2 pathway: drugs that with tubulointerstitial injury. Inhibition of mTOR is most commonly associated with bind to VEGFA, sequester VEGFA, in- albuminuria and podocyte injury, but has also been linked to renal-specificTMA.In hibit receptor tyrosine kinases (RTKs), all, we review the experimentally validated mechanisms by which VEGFA-VEGFR2 or inhibit downstream pathways. -

Cardiotoxicity Associated with Targeted Cancer Therapies (Review)
MOLECULAR AND CLINICAL ONCOLOGY 4: 675-681, 2016 Cardiotoxicity associated with targeted cancer therapies (Review) ZI CHEN1,2 and DI AI3 1Department of Hematology, Huashan Hospital, Fudan University, Shanghai 200040, P.R. China; 2Department of Hematopathology, University of Texas MD Anderson Cancer Center, Houston, TX 77030; 3Department of Pathology, Baylor Scott and White Memorial Hospital, Texas A&M Health Science Center, Temple, TX 76508, USA Received July 28, 2015; Accepted January 25, 2016 DOI: 10.3892/mco.2016.800 Abstract. Compared with traditional chemotherapy, targeted eliminate rapidly dividing cells, including not only tumor cancer therapy is a novel strategy in which key molecules cells, but also normal tissue cells, such as those in digestive in signaling pathways involved in carcinogenesis and tumor endothelia, hair follicles and bone marrow. This non‑specific spread are inhibited. Targeted cancer therapy has fewer targeting treatment is associated with a broad range of side adverse effects on normal cells and is considered to be the effects, including gastrointestinal (GI) symptoms, alopecia and future of chemotherapy. However, targeted cancer ther- even lethal adverse effects, such as bone marrow suppression. apy-induced cardiovascular toxicities are occasionally critical These negative effects significantly limit the applications issues in patients who receive novel anticancer agents, such of traditional agents and unnecessarily compromise the as trastuzumab, bevacizumab, sunitinib and imatinib. The quality of life of cancer patients. In targeted cancer therapy, aim of this review was to discuss these most commonly used drugs interfere with key signaling molecules and inhibit drugs and associated incidence of cardiotoxicities, including tumorigenesis and metastasis, with fewer associated adverse left ventricular dysfunction, heart failure, hypertension and effects (2). -

Bevacizumab (Avastin) in Combination with Trastuzumab and Docetaxel for Metastatic HER2 Positive Breast Cancer – First Line
Bevacizumab (Avastin) in combination with trastuzumab and docetaxel for metastatic HER2 positive breast cancer – first line August 2010 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive statement on the safety, efficacy or effectiveness of the health technology covered and should not be used for commercial purposes. The National Horizon Scanning Centre Research Programme is part of the National Institute for Health Research August 2010 Bevacizumab (Avastin) in combination with trastuzumab and docetaxel for metastatic HER2 positive breast cancer – first line Target group • Breast cancer: metastatic; HER2 positive – first line; in combination with trastuzumab and docetaxel. Technology description Bevacizumab (Avastin; anti-VEGF monoclonal antibody; R 435; RG435; rhuMAb- VEGF) is a humanised anti-vascular endothelial growth factor (VEGF) monoclonal antibody that inhibits VEGF induced signalling and VEGF driven angiogenesis. This reduces vascularisation of tumours, thereby inhibiting tumour growth. The combination of bevacizumab, trastuzumab (HER2 inhibitor) and docetaxel (mitosis inhibitor), is intended to be used for the treatment of breast cancer with over expression of human epidermal growth factor receptor 2 (HER2). Bevacizumab is administered by IV infusion at 15mg/kg every 3 weeks in combination with trastuzumab (8mg/kg loading dose, thereafter 6mg/kg every 3 weeks) and docetaxel (100mg/m2 every 3 weeks) until disease progression. Bevacizumab is currently licensed for: • Metastatic breast cancer: first line treatment in combination with paclitaxel or docetaxel. • Metastatic colorectal cancer: in combination with fluoropyrimidine based chemotherapy. • Advanced non-small cell lung cancer (NSCLC): first line treatment in combination with platinum based therapy. -

Effectiveness and Costs Associated to Adding Cetuximab Or Bevacizumab
cancers Article Effectiveness and Costs Associated to Adding Cetuximab or Bevacizumab to Chemotherapy as Initial Treatment in Metastatic Colorectal Cancer: Results from the Observational FABIO Project Matteo Franchi 1,2,* , Donatella Garau 3, Ursula Kirchmayer 4, Mirko Di Martino 4 , Marilena Romero 5, Ilenia De Carlo 6, Salvatore Scondotto 7 and Giovanni Corrao 1,2 1 National Centre for Healthcare Research and Pharmacoepidemiology, 20126 Milan, Italy 2 Laboratory of Healthcare Research & Pharmacoepidemiology, Department of Statistics and Quantitative Methods, University of Milano-Bicocca, 20126 Milan, Italy 3 General Directorate for Health, Sardinia Region, 09123 Cagliari, Italy 4 Department of Epidemiology ASL Roma 1, Lazio Regional Health Service, 00154 Rome, Italy 5 Department of Medical, Oral and Biotechnological Sciences—Section of Pharmacology and Toxicology, University of Chieti, 66100 Chieti, Italy 6 Regional Centre of Pharmacovigilance, Regional Health Authority, Marche Region, 60125 Ancona, Italy 7 Department of Health Services and Epidemiological Observatory, Regional Health Authority, Sicily Region, 90145 Palermo, Italy * Correspondence: [email protected]; Tel.: +39-02-6448-5859 Received: 3 March 2020; Accepted: 30 March 2020; Published: 31 March 2020 Abstract: Evidence available on the effectiveness and costs of biological therapies for the initial treatment of metastatic colorectal cancer (mCRC) is scarce and contrasting. We conducted a population-based cohort investigation for assessing overall survival and costs associated with their use in a real-world setting. Healthcare utilization databases were used to select patients newly diagnosed with mCRC between 2010 and 2016. Those initially treated with biological therapy (bevacizumab or cetuximab) added to chemotherapy were propensity-score-matched to those treated with standard chemotherapy alone, and were followed up to June 30th, 2018. -

Primary and Acquired Resistance to Immunotherapy in Lung Cancer: Unveiling the Mechanisms Underlying of Immune Checkpoint Blockade Therapy
cancers Review Primary and Acquired Resistance to Immunotherapy in Lung Cancer: Unveiling the Mechanisms Underlying of Immune Checkpoint Blockade Therapy Laura Boyero 1 , Amparo Sánchez-Gastaldo 2, Miriam Alonso 2, 1 1,2,3, , 1,2, , José Francisco Noguera-Uclés , Sonia Molina-Pinelo * y and Reyes Bernabé-Caro * y 1 Institute of Biomedicine of Seville (IBiS) (HUVR, CSIC, Universidad de Sevilla), 41013 Seville, Spain; [email protected] (L.B.); [email protected] (J.F.N.-U.) 2 Medical Oncology Department, Hospital Universitario Virgen del Rocio, 41013 Seville, Spain; [email protected] (A.S.-G.); [email protected] (M.A.) 3 Centro de Investigación Biomédica en Red de Cáncer (CIBERONC), 28029 Madrid, Spain * Correspondence: [email protected] (S.M.-P.); [email protected] (R.B.-C.) These authors contributed equally to this work. y Received: 16 November 2020; Accepted: 9 December 2020; Published: 11 December 2020 Simple Summary: Immuno-oncology has redefined the treatment of lung cancer, with the ultimate goal being the reactivation of the anti-tumor immune response. This has led to the development of several therapeutic strategies focused in this direction. However, a high percentage of lung cancer patients do not respond to these therapies or their responses are transient. Here, we summarized the impact of immunotherapy on lung cancer patients in the latest clinical trials conducted on this disease. As well as the mechanisms of primary and acquired resistance to immunotherapy in this disease. Abstract: After several decades without maintained responses or long-term survival of patients with lung cancer, novel therapies have emerged as a hopeful milestone in this research field. -

July 1, 2020 RE: Physician Administered Drugs (J Codes)
July 1, 2020 RE: Physician Administered Drugs (J Codes) Included in Prior Authorization Matrix for Molina Healthcare of New York, Inc. Dear Participating Provider: Molina Healthcare of New York, Inc. requires prior authorization for these HCPCS codes for all participating providers. Prior authorization is required before services are rendered for the codes listed. Prior authorization requests should include the most up to date patient information including office notes, consultations, labs, scans, previous treatments tried, and any other patient specific information to support the request. Please fax a completed prior authorization form along with all supporting clinical documentation to fax number: 1-844- 823-5479. Our prior authorization form and most up to date formulary can be found on our website: MolinaHealthcare.com. C9061 INJECTION, TEPROTUMUMAB-TRBW, 10 mg C9063 INJECTION, EPTINEZUMAB-JJMR, 1 mg C9122 MOMETASONE FUROATE SINUS IMPLANT, 10 micrograms (sinuva) J0122 INJECTION, ERAVACYCLINE, 1 mg J0129 Injection, abatacept 10 mg J0178 Injection, aflibercept 1 mg J0179 INJECTION, BROLUCIZUMAB-DBLL, 1MG J0185 Injection, aprepitant 1 mg J0223 INJECTION, GIVOSIRAN, 0.5 mg J0285 INJECTION, AMPHOTERICIN B, 50 mg J0490 Injection, belimumab 10 mg J0517 Injection, benralizumab 1 mg J0567 Injection, cerliponase alfa 1 mg J0584 Injection, burosumab-twza 1 mg J0585 Injection, onabotulinumtoxina, 1 unit J0587 Injection, rimabotulinumtoxinb 100 units J0599 Injection, c-1 esterase inhibitor 10 units J0641 Injection, levoleucovorin, not otherwise -

Pharmaceutical Appendix to the Harmonized Tariff Schedule
Harmonized Tariff Schedule of the United States (2019) Revision 13 Annotated for Statistical Reporting Purposes PHARMACEUTICAL APPENDIX TO THE HARMONIZED TARIFF SCHEDULE Harmonized Tariff Schedule of the United States (2019) Revision 13 Annotated for Statistical Reporting Purposes PHARMACEUTICAL APPENDIX TO THE TARIFF SCHEDULE 2 Table 1. This table enumerates products described by International Non-proprietary Names INN which shall be entered free of duty under general note 13 to the tariff schedule. The Chemical Abstracts Service CAS registry numbers also set forth in this table are included to assist in the identification of the products concerned. For purposes of the tariff schedule, any references to a product enumerated in this table includes such product by whatever name known. -

Amgen and Allergan's MVASI™ (Bevacizumab-Awwb) and KANJINTI™ (Trastuzumab-Anns) Now Available in the United States
Amgen And Allergan's MVASI™ (bevacizumab-awwb) And KANJINTI™ (trastuzumab-anns) Now Available In The United States July 19, 2019 First Biosimilar Avastin® and Herceptin® Products to Launch in the United States THOUSAND OAKS, Calif., July 18, 2019 /PRNewswire/ -- Amgen (NASDAQ:AMGN) and Allergan plc (NYSE:AGN) today announced that MVASI™ (bevacizumab-awwb), a biosimilar to Avastin® (bevacizumab), and KANJINTITM (trastuzumab-anns), a biosimilar to Herceptin® (trastuzumab), are now available in the United States (U.S.). MVASI, the first oncology therapeutic biosimilar approved by the U.S. Food and Drug Administration (FDA), is approved for the treatment of five types of cancer: in combination with chemotherapy for metastatic colorectal cancer (mCRC); in combination with chemotherapy for non-squamous non-small cell lung cancer (NSCLC); recurrent glioblastoma; in combination with interferon-alfa for metastatic renal cell carcinoma; and in combination with chemotherapy for persistent, recurrent, or metastatic cervical cancer. KANJINTI is FDA approved for all approved indications of Herceptin: for the treatment of HER2-overexpressing adjuvant and metastatic breast cancer and HER2-overexpressing metastatic gastric or gastroesophageal junction adenocarcinoma. "The introduction of biosimilars is an important step in increasing options for treating HER2-positive breast cancers, which account for about 25% of all breast cancers," said Paula Schneider, chief executive officer, Susan G. Komen Breast Cancer Foundation. "As patient advocates, we are working to ensure that patients are educated about biosimilars and understand that these FDA-approved treatments are just as effective as the original biologic drugs." The Wholesale Acquisition Cost (WAC or "list price") of both MVASI and KANJINTI will be 15% lower than their reference products. -
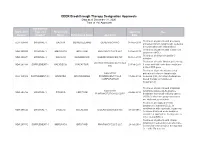
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities