Common Skin Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

This Fact Sheet Provides Information to Patients with Eczema and Their Carers. About Topical Corticosteroids How to Apply Topic
This fact sheet provides information to patients with eczema and their carers. About topical corticosteroids You or your child’s doctor has prescribed a topical corticosteroid for the treatment of eczema. For treating eczema, corticosteroids are usually prepared in a cream or ointment and are applied topically (directly onto the skin). Topical corticosteroids work by reducing inflammation and helping to control an over-reactive response of the immune system at the site of eczema. They also tighten blood vessels, making less blood flow to the surface of the skin. Together, these effects help to manage the symptoms of eczema. There is a range of steroids that can be used to treat eczema, each with different strengths (potencies). On the next page, the potencies of some common steroids are shown, as well as the concentration that they are usually used in cream or ointment preparations. Using a moisturiser along with a steroid cream does not reduce the effect of the steroid. There are many misconceptions about the side effects of topical corticosteroids. However these treatments are very safe and patients are encouraged to follow the treatment regimen as advised by their doctor. How to apply topical corticosteroids How often should I apply? How much should I apply? Apply 1–2 times each day to the affected area Enough cream should be used so that the of skin according to your doctor’s instructions. entire affected area is covered. The cream can then be rubbed or massaged into the Once the steroid cream has been applied, inflamed skin. moisturisers can be used straight away if needed. -

Fungal Infections from Human and Animal Contact
Journal of Patient-Centered Research and Reviews Volume 4 Issue 2 Article 4 4-25-2017 Fungal Infections From Human and Animal Contact Dennis J. Baumgardner Follow this and additional works at: https://aurora.org/jpcrr Part of the Bacterial Infections and Mycoses Commons, Infectious Disease Commons, and the Skin and Connective Tissue Diseases Commons Recommended Citation Baumgardner DJ. Fungal infections from human and animal contact. J Patient Cent Res Rev. 2017;4:78-89. doi: 10.17294/2330-0698.1418 Published quarterly by Midwest-based health system Advocate Aurora Health and indexed in PubMed Central, the Journal of Patient-Centered Research and Reviews (JPCRR) is an open access, peer-reviewed medical journal focused on disseminating scholarly works devoted to improving patient-centered care practices, health outcomes, and the patient experience. REVIEW Fungal Infections From Human and Animal Contact Dennis J. Baumgardner, MD Aurora University of Wisconsin Medical Group, Aurora Health Care, Milwaukee, WI; Department of Family Medicine and Community Health, University of Wisconsin School of Medicine and Public Health, Madison, WI; Center for Urban Population Health, Milwaukee, WI Abstract Fungal infections in humans resulting from human or animal contact are relatively uncommon, but they include a significant proportion of dermatophyte infections. Some of the most commonly encountered diseases of the integument are dermatomycoses. Human or animal contact may be the source of all types of tinea infections, occasional candidal infections, and some other types of superficial or deep fungal infections. This narrative review focuses on the epidemiology, clinical features, diagnosis and treatment of anthropophilic dermatophyte infections primarily found in North America. -

Skin Lesions in Diabetic Patients
Rev Saúde Pública 2005;39(4) 1 www.fsp.usp.br/rsp Skin lesions in diabetic patients N T Foss, D P Polon, M H Takada, M C Foss-Freitas and M C Foss Departamento de Clínica Médica. Faculdade de Medicina de Ribeirão Preto. Universidade de São Paulo. Ribeirão Preto, SP, Brasil Keywords Abstract Skin diseases. Dermatomycoses. Diabetes mellitus. Metabolic control. Objective It is yet unknown the relationship between diabetes and determinants or triggering factors of skin lesions in diabetic patients. The purpose of the present study was to investigate the presence of unreported skin lesions in diabetic patients and their relationship with metabolic control of diabetes. Methods A total of 403 diabetic patients, 31% type 1 and 69% type 2, underwent dermatological examination in an outpatient clinic of a university hospital. The endocrine-metabolic evaluation was carried out by an endocrinologist followed by the dermatological evaluation by a dermatologist. The metabolic control of 136 patients was evaluated using glycated hemoglobin. Results High number of dermophytosis (82.6%) followed by different types of skin lesions such as acne and actinic degeneration (66.7%), pyoderma (5%), cutaneous tumors (3%) and necrobiosis lipoidic (1%) were found. Among the most common skin lesions in diabetic patients, confirmed by histopathology, there were seen necrobiosis lipoidic (2 cases, 0.4%), diabetic dermopathy (5 cases, 1.2%) and foot ulcerations (3 cases, 0.7%). Glycated hemoglobin was 7.2% in both type 1 and 2 patients with adequate metabolic control and 11.9% and 12.7% in type 1 and 2 diabetic patients, respectively, with inadequate metabolic controls. -

Determination of Triamcinolone Acetonide Steroid on Glassy Carbon Electrode by Stripping Voltammetric Methods
Int. J. Electrochem. Sci., 3 (2008) 509-518 International Journal of ELECTROCHEM ICAL SCIENCE www.electrochemsci.org Determination of Triamcinolone Acetonide Steroid on Glassy Carbon Electrode by Stripping Voltammetric Methods C. Vedhi, R. Eswar, H. Gurumallesh Prabu and P. Manisankar* Department of Industrial Chemistry, Alagappa University, Karaikudi –630 003,Tamil Nadu, India *E-mail: [email protected] or [email protected] Received: 9 December 2007 / Accepted: 6 February 2008 / Online published: 20 February 2008 A corticosteroid, triamcinolone acetonide was determined by stripping voltammetric procedure using glassy carbon electrode. Cyclic voltammetric behaviour of steroid was studied in 50% aqueous methanol at acid, neutral and alkaline pH conditions. Influence of pH, sweep rate and steroid concentration were studied. An irreversible and adsorption-controlled well-defined reduction peak was observed in all pH conditions. The reduction peak potential shifted cathodically with change in pH. Controlled potential coulometry revealed two-electron reduction of the α,β-unsaturated carbonyl function present in the steroid. A systematic study of the experimental parameters that affect the differential pulse / square wave stripping voltammetric response was carried out and optimized conditions were arrived at. Under optimum conditions, differential pulse and square wave adsorptive stripping voltammetric procedures were developed for the determination of triamcinolone acetonide steroid at pH 13.0. A calibration plots was derived and the lower limit of determination observed are 0.1 µg/mL from DPSV and 0.01 µg/mL from SWSV. Keywords: Triamcinolone acetonide steroid, Cyclic Voltammetry, Stripping Voltammetry, Glassy carbon electrode. 1. INTRODUCTION Corticosteroids are hormones produced naturally by the adrenal glands, which have many important functions on every organ system. -

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -

Psoriasis, a Systemic Disease Beyond the Skin, As Evidenced by Psoriatic Arthritis and Many Comorbities
1 Psoriasis, a Systemic Disease Beyond the Skin, as Evidenced by Psoriatic Arthritis and Many Comorbities – Clinical Remission with a Leishmania Amastigotes Vaccine, a Serendipity Finding J.A. O’Daly Astralis Ltd, Irvington, NJ USA 1. Introduction Psoriasis is a systemic chronic, relapsing inflammatory skin disorder, with worldwide distribution, affects 1–3% of the world population, prevalence varies according to race, geographic location, and environmental factors (Chandran & Raychaudhuri, 2010; Christophers & Mrowietz, 2003; Farber & Nall, 1974). In Germany, 33,981 from 1,344,071 continuously insured persons in 2005 were diagnosed with psoriasis; thus the one year prevalence was 2.53% in the study group. Up to the age of 80 years the prevalence rate (range: 3.99-4.18%) was increasing with increasing age and highest for the age groups from 50 to 79 years The total rate of psoriasis in children younger than 18 years was 0.71%. The prevalence rates increased in an approximately linear manner from 0.12% at the age of 1 year to 1.2% at the age of 18 years (Schäfer et al., 2011). In France, a case-control study in 6,887 persons, 356 cases were identified (5.16%), who declared having had psoriasis during the previous 12 months (Wolkenstein et al., 2009). The prevalence of psoriasis analyzed across Italy showed that 2.9% of Italians declared suffering from psoriasis (regional range: 0.8-4.5%) in a total of 4109 individuals (Saraceno et al., 2008). The overall rate of comorbidity in subjects with psoriasis aged less than 20 years was twice as high as in subjects without psoriasis. -

The Management of Common Skin Conditions in General Practice
Management of Common Skin Conditions In General Practice including the “red rash made easy” © Arroll, Fishman & Oakley, Department of General Practice and Primary Health Care University of Auckland, Tamaki Campus Reviewed by Hon A/Prof Amanda Oakley - 2019 http://www.dermnetnz.org Management of Common Skin Conditions In General Practice Contents Page Derm Map 3 Classic location: infants & children 4 Classic location: adults 5 Dermatology terminology 6 Common red rashes 7 Other common skin conditions 12 Common viral infections 14 Common bacterial infections 16 Common fungal infections 17 Arthropods 19 Eczema/dermatitis 20 Benign skin lesions 23 Skin cancers 26 Emergency dermatology 28 Clinical diagnosis of melanoma 31 Principles of diagnosis and treatment 32 Principles of treatment of eczema 33 Treatment sequence for psoriasis 34 Topical corticosteroids 35 Combination topical steroid + antimicrobial 36 Safety with topical corticosteroids 36 Emollients 37 Antipruritics 38 For further information, refer to: http://www.dermnetnz.org And http://www.derm-master.com 2 © Arroll, Fishman & Oakley, Department of General Practice and Primary Health Care, University of Auckland, Tamaki Campus. Management of Common Skin Conditions In General Practice DERM MAP Start Is the patient sick ? Yes Rash could be an infection or a drug eruption? No Insect Bites – Crop of grouped papules with a central blister or scab. Is the patient in pain or the rash Yes Infection: cellulitis / erysipelas, impetigo, boil is swelling, oozing or crusting? / folliculitis, herpes simplex / zoster. Urticaria – Smooth skin surface with weals that evolve in minutes to hours. No Is the rash in a classic location? Yes See our classic location chart . -
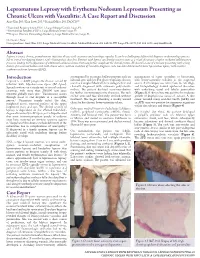
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -
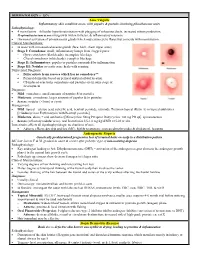
Pediatrics-EOR-Outline.Pdf
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Topical Treatments for Seborrheic Keratosis: a Systematic Review
SYSTEMATIC REVIEW AND META-ANALYSIS Topical Treatments for Seborrheic Keratosis: A Systematic Review Ma. Celina Cephyr C. Gonzalez, Veronica Marie E. Ramos and Cynthia P. Ciriaco-Tan Department of Dermatology, College of Medicine and Philippine General Hospital, University of the Philippines Manila ABSTRACT Background. Seborrheic keratosis is a benign skin tumor removed through electrodessication, cryotherapy, or surgery. Alternative options may be beneficial to patients with contraindications to standard treatment, or those who prefer a non-invasive approach. Objectives. To determine the effectiveness and safety of topical medications on seborrheic keratosis in the clearance of lesions, compared to placebo or standard therapy. Methods. Studies involving seborrheic keratosis treated with any topical medication, compared to cryotherapy, electrodessication or placebo were obtained from MEDLINE, HERDIN, and Cochrane electronic databases from 1990 to June 2018. Results. The search strategy yielded sixty articles. Nine publications (two randomized controlled trials, two non- randomized controlled trials, three cohort studies, two case reports) covering twelve medications (hydrogen peroxide, tacalcitol, calcipotriol, maxacalcitol, ammonium lactate, tazarotene, imiquimod, trichloroacetic acid, urea, nitric-zinc oxide, potassium dobesilate, 5-fluorouracil) were identified. The analysis showed that hydrogen peroxide 40% presented the highest level of evidence and was significantly more effective in the clearance of lesions compared to placebo. Conclusion. Most of the treatments reviewed resulted in good to excellent lesion clearance, with a few well- tolerated minor adverse events. Topical therapy is a viable option; however, the level of evidence is low. Standard invasive therapy remains to be the more acceptable modality. Key Words: seborrheic keratosis, topical, systematic review INTRODUCTION Description of the condition Seborrheic keratoses (SK) are very common benign tumors of the hair-bearing skin, typically seen in the elderly population. -

A Resident's Guide to Pediatric Rheumatology
A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY 4th Revised Edition - 2019 A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY This guide is intended to provide a brief introduction to basic topics in pediatric rheumatology. Each topic is accompanied by at least one up-to-date reference that will allow you to explore the topic in greater depth. In addition, a list of several excellent textbooks and other resources for you to use to expand your knowledge is found in the Appendix. We are interested in your feedback on the guide! If you have comments or questions, please feel free to contact us via email at [email protected]. Supervising Editors: Dr. Ronald M. Laxer, SickKids Hospital, University of Toronto Dr. Tania Cellucci, McMaster Children’s Hospital, McMaster University Dr. Evelyn Rozenblyum, St. Michael’s Hospital, University of Toronto Section Editors: Dr. Michelle Batthish, McMaster Children’s Hospital, McMaster University Dr. Roberta Berard, Children’s Hospital – London Health Sciences Centre, Western University Dr. Liane Heale, McMaster Children’s Hospital, McMaster University Dr. Clare Hutchinson, North York General Hospital, University of Toronto Dr. Mehul Jariwala, Royal University Hospital, University of Saskatchewan Dr. Lillian Lim, Stollery Children’s Hospital, University of Alberta Dr. Nadia Luca, Alberta Children’s Hospital, University of Calgary Dr. Dax Rumsey, Stollery Children’s Hospital, University of Alberta Dr. Gordon Soon, North York General Hospital and SickKids Hospital Northern Clinic in Sudbury, University -

Erythema Nodosum (En)
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 ERYTHEMA NODOSUM (EN) Erythema Nodosum (EN) is a relatively uncommon reaction in the skin consisting of red shiny tender nodular lesions most commonly found on the legs. The erythema refers to the red color that is seen at the surface of the skin. The nodosum refers to the fact that these lesions feel like bumps or nodules underneath the skin surface. Erythema nodosum is a reaction pattern occurring in the subcutaneous tissue and fat. It may be preceded by a low grade fever, fatigue, and joint pains. In about half of the cases, there is an internal condition occurring in the body which contributes to its formation. These include the use of certain medications, certain infections, and a number of other less likely causes. In order to identify cause for the erythema nodosum, it may be necessary to perform blood and laboratory tests. At times, however, the cause cannot be determined and erythema nodosum is considered to be idiopathic in nature. Erythema nodosum often runs an acute course lasting for a brief period from weeks to months. In a small percentage of cases, it can be a more chronic condition. The red nodules are usually confined to the lower legs, but can develop anywhere there is fat under the skin including the thighs, arms, and trunk. Initially, the lesions are more red and inflamed in appearance, but with time become more bruise like.