Psoriasis, a Systemic Disease Beyond the Skin, As Evidenced by Psoriatic Arthritis and Many Comorbities
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Resident's Guide to Pediatric Rheumatology
A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY 4th Revised Edition - 2019 A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY This guide is intended to provide a brief introduction to basic topics in pediatric rheumatology. Each topic is accompanied by at least one up-to-date reference that will allow you to explore the topic in greater depth. In addition, a list of several excellent textbooks and other resources for you to use to expand your knowledge is found in the Appendix. We are interested in your feedback on the guide! If you have comments or questions, please feel free to contact us via email at [email protected]. Supervising Editors: Dr. Ronald M. Laxer, SickKids Hospital, University of Toronto Dr. Tania Cellucci, McMaster Children’s Hospital, McMaster University Dr. Evelyn Rozenblyum, St. Michael’s Hospital, University of Toronto Section Editors: Dr. Michelle Batthish, McMaster Children’s Hospital, McMaster University Dr. Roberta Berard, Children’s Hospital – London Health Sciences Centre, Western University Dr. Liane Heale, McMaster Children’s Hospital, McMaster University Dr. Clare Hutchinson, North York General Hospital, University of Toronto Dr. Mehul Jariwala, Royal University Hospital, University of Saskatchewan Dr. Lillian Lim, Stollery Children’s Hospital, University of Alberta Dr. Nadia Luca, Alberta Children’s Hospital, University of Calgary Dr. Dax Rumsey, Stollery Children’s Hospital, University of Alberta Dr. Gordon Soon, North York General Hospital and SickKids Hospital Northern Clinic in Sudbury, University -

Celiac Disease and Nonceliac Gluten Sensitivitya Review
Clinical Review & Education JAMA | Review Celiac Disease and Nonceliac Gluten Sensitivity A Review Maureen M. Leonard, MD, MMSc; Anna Sapone, MD, PhD; Carlo Catassi, MD, MPH; Alessio Fasano, MD CME Quiz at IMPORTANCE The prevalence of gluten-related disorders is rising, and increasing numbers of jamanetwork.com/learning individuals are empirically trying a gluten-free diet for a variety of signs and symptoms. This review aims to present current evidence regarding screening, diagnosis, and treatment for celiac disease and nonceliac gluten sensitivity. OBSERVATIONS Celiac disease is a gluten-induced immune-mediated enteropathy characterized by a specific genetic genotype (HLA-DQ2 and HLA-DQ8 genes) and autoantibodies (antitissue transglutaminase and antiendomysial). Although the inflammatory process specifically targets the intestinal mucosa, patients may present with gastrointestinal signs or symptoms, extraintestinal signs or symptoms, or both, Author Affiliations: Center for Celiac suggesting that celiac disease is a systemic disease. Nonceliac gluten sensitivity Research and Treatment, Division of is diagnosed in individuals who do not have celiac disease or wheat allergy but who Pediatric Gastroenterology and Nutrition, MassGeneral Hospital for have intestinal symptoms, extraintestinal symptoms, or both, related to ingestion Children, Boston, Massachusetts of gluten-containing grains, with symptomatic improvement on their withdrawal. The (Leonard, Sapone, Catassi, Fasano); clinical variability and the lack of validated biomarkers for nonceliac gluten sensitivity make Celiac Research Program, Harvard establishing the prevalence, reaching a diagnosis, and further study of this condition Medical School, Boston, Massachusetts (Leonard, Sapone, difficult. Nevertheless, it is possible to differentiate specific gluten-related disorders from Catassi, Fasano); Shire, Lexington, other conditions, based on currently available investigations and algorithms. -

Conditions Related to Inflammatory Arthritis
Conditions Related to Inflammatory Arthritis There are many conditions related to inflammatory arthritis. Some exhibit symptoms similar to those of inflammatory arthritis, some are autoimmune disorders that result from inflammatory arthritis, and some occur in conjunction with inflammatory arthritis. Related conditions are listed for information purposes only. • Adhesive capsulitis – also known as “frozen shoulder,” the connective tissue surrounding the joint becomes stiff and inflamed causing extreme pain and greatly restricting movement. • Adult onset Still’s disease – a form of arthritis characterized by high spiking fevers and a salmon- colored rash. Still’s disease is more common in children. • Caplan’s syndrome – an inflammation and scarring of the lungs in people with rheumatoid arthritis who have exposure to coal dust, as in a mine. • Celiac disease – an autoimmune disorder of the small intestine that causes malabsorption of nutrients and can eventually cause osteopenia or osteoporosis. • Dermatomyositis – a connective tissue disease characterized by inflammation of the muscles and the skin. The condition is believed to be caused either by viral infection or an autoimmune reaction. • Diabetic finger sclerosis – a complication of diabetes, causing a hardening of the skin and connective tissue in the fingers, thus causing stiffness. • Duchenne muscular dystrophy – one of the most prevalent types of muscular dystrophy, characterized by rapid muscle degeneration. • Dupuytren’s contracture – an abnormal thickening of tissues in the palm and fingers that can cause the fingers to curl. • Eosinophilic fasciitis (Shulman’s syndrome) – a condition in which the muscle tissue underneath the skin becomes swollen and thick. People with eosinophilic fasciitis have a buildup of eosinophils—a type of white blood cell—in the affected tissue. -

Comorbidities in Psoriasis: the Recognition of Psoriasis As a Systemic Disease and Current Management
Review Derleme 71 DOI: 10.4274/turkderm.09476 Turkderm-Turk Arch Dermatol Venereology 2017;51:71-7 Comorbidities in psoriasis: The recognition of psoriasis as a systemic disease and current management Psoriazisde komorbiditeler: Psoriazisin sistemik hastalık olarak kabul edilmesi ve güncel yaklaşım Göknur Kalkan Ankara Yıldırım Beyazıt University Faculty of Medicine, Department of Dermatology, Ankara, Turkey Abstract Psoriasis, with a worldwide prevalence of 2-3%, is now assumed as a systemic chronic inflammatory disease accompanied by comorbidities while it was accepted as a disease limited only to the skin in the past. There are several classifications of the comorbidities which are more common in patients with moderate to severe psoriasis. Simply, comorbidities can be classified as classic, emerging, related to lifestyle, related to treatment. They can also be categorized as medical comorbidities, psychiatric/psychologic comorbidities, and behaviors contributing to medical and psychiatric comorbidities. In this review, providing early diagnosis and treatment of comorbidities, learning screening recommendations for early detection and long-term disease control and improvement in life quality by integrated, multidisciplinary approach were targeted. Keywords: Psoriasis, comorbidity, systemic disease Öz Tüm dünyada %2-3 oranında görülme sıklığına sahip psoriazis, geçmişte sadece deriye sınırlı kabul edilirken, günümüzde birçok komorbiditenin eşlik ettiği kronik sistemik enflamatuvar bir hastalık olarak ele alınmaktadır. Orta-şiddetli düzeyde -

UC Davis Dermatology Online Journal
UC Davis Dermatology Online Journal Title Proposed classification for koebner, wolf isotopic, renbok, koebner nonreaction, isotopic nonreaction & other related phenomen. Permalink https://escholarship.org/uc/item/96s656b4 Journal Dermatology Online Journal, 20(11) Authors Kannangara, Ajith P Yosipovitch, Gil Fleischer Jr., Alan B Publication Date 2014 DOI 10.5070/D32011024682 License https://creativecommons.org/licenses/by-nc-nd/4.0/ 4.0 eScholarship.org Powered by the California Digital Library University of California Volume 20 Number 11 November 2014 Commentary Proposed classification for koebner, wolf isotopic, renbok, koebner nonreaction, isotopic nonreaction & other related phenomen. Ajith P. Kannangara MD1, Gil Yosipovitch MD PhD2, Alan B. Fleischer Jr MD3 Dermatology Online Journal 20 (11): 12 1Base Hospital Balapitiya, Ministry of Health, Sri Lanka 2Department of Dermatology, Temple University School of Medicine, Philadelphia, USA 3Department of Dermatology, Wake Forest University School of Medicine; Winston-Salem, North Carolina, USA Correspondence: Ajith P. Kannangara, M.D Base Hospital Balapitiya, Ministry of Health, Sri Lanka. E-mail: [email protected] Abstract Students of skin diseases have long noted a variety of disease responses and non-responses to trauma and the presence of structural abnormalities. This article will review the series of these responses including: Koebner phenomenon, Wolf isotopic response, Renbök response, Koebner nonreaction, isotopic nonreaction, and other related skin reactions. Because most of these reported phenomena have similar morphological features the diagnosis is often made on the basis of differences in the clinical presentation. Note that some of the cutaneous reactions of similar phenomena have been described using varied nomenclature, further adding to the confusion. -

Koebner Phenomenon in Rheumatoid Arthritis
ndrom Sy es tic & e G n e e n G e f T o Yamamoto and Ueki, J Genet Syndr Gene Ther 2013, 4:8 Journal of Genetic Syndromes h l e a r n a r p DOI: 10.4172/2157-7412.1000173 u y o J & Gene Therapy ISSN: 2157-7412 Review Article Open Access Koebner Phenomenon in Rheumatoid Arthritis Yamamoto T1* and Ueki H2 1Department of Dermatology, Fukushima Medical University, Japan 2Department of Dermatology, Kawasaki Medical School, Japan Abstract Koebner phenomenon indicates the newly appearance of isomorphic lesions at the sites of mechanically stimulated or injured skin. This phenomenon can be seen in various inflammatory, auto-immune, viral, fibrotic, and even tumoral disorders. Also, rheumatic diseases such as lupus erythematosus, dermatomyositis, and rheumatoid arthritis (RA) often present with cutaneous manifestations with isomorphic response of Koebner. RA presents with various skin conditions as extra-articular manifestations. Rheumatoid nodule is the representative specific skin lesion which frequently occurs on the hand, elbow, sole, sacrum, occipital area, and so on. These sites are susceptible to both outer and inner mechanical stress. Rheumatoid nodules involve not only skin but internal tissues such as spine, lung, heart valves, and gastrointestinal tract, which are also susceptible to mechanical stress. This isomorphic response may be induced at deeper levels than skin, and thus considered to be “deep” or “internal” Koebner phenomenon. Other than rheumatoid nodules, several specific skin conditions are associated with RA, such as palisaded neutrophilic granulomatous dermatitis and rheumatoid neutrophilic dermatitis, which can be seen on the fingers, elbows, knees and sole. -

Oral and Maxillo-Facial Manifestations of Systemic Diseases: an Overview
medicina Review Oral and Maxillo-Facial Manifestations of Systemic Diseases: An Overview Saverio Capodiferro *,† , Luisa Limongelli *,† and Gianfranco Favia Department of Interdisciplinary Medicine, University of Bari Aldo Moro, Piazza G. Cesare, 11, 70124 Bari, Italy; [email protected] * Correspondence: [email protected] (S.C.); [email protected] (L.L.) † These authors contributed equally to the paper. Abstract: Many systemic (infective, genetic, autoimmune, neoplastic) diseases may involve the oral cavity and, more generally, the soft and hard tissues of the head and neck as primary or secondary localization. Primary onset in the oral cavity of both pediatric and adult diseases usually represents a true challenge for clinicians; their precocious detection is often difficult and requires a wide knowledge but surely results in the early diagnosis and therapy onset with an overall better prognosis and clinical outcomes. In the current paper, as for the topic of the current Special Issue, the authors present an overview on the most frequent clinical manifestations at the oral and maxillo-facial district of systemic disease. Keywords: oral cavity; head and neck; systemic disease; oral signs of systemic diseases; early diagnosis; differential diagnosis Citation: Capodiferro, S.; Limongelli, 1. Introduction L.; Favia, G. Oral and Maxillo-Facial Oral and maxillo-facial manifestations of systemic diseases represent an extensive and Manifestations of Systemic Diseases: fascinating study, which is mainly based on the knowledge that many signs and symptoms An Overview. Medicina 2021, 57, 271. as numerous systemic disorders may first present as or may be identified by head and https://doi.org/10.3390/ neck tissue changes. -

Martin Steinhoff Dirk Roosterman, Tobias Goerge, Stefan W
Dirk Roosterman, Tobias Goerge, Stefan W. Schneider, Nigel W. Bunnett and Martin Steinhoff Physiol Rev 86:1309-1379, 2006. doi:10.1152/physrev.00026.2005 You might find this additional information useful... This article cites 963 articles, 265 of which you can access free at: http://physrev.physiology.org/cgi/content/full/86/4/1309#BIBL Medline items on this article's topics can be found at http://highwire.stanford.edu/lists/artbytopic.dtl on the following topics: Biochemistry .. Transient Receptor Potential Channel Biochemistry .. Endopeptidases Biochemistry .. Proteolytic Enzymes Oncology .. Inflammation Medicine .. Neurogenic Inflammation Physiology .. Nerves Updated information and services including high-resolution figures, can be found at: http://physrev.physiology.org/cgi/content/full/86/4/1309 Downloaded from Additional material and information about Physiological Reviews can be found at: http://www.the-aps.org/publications/prv This information is current as of February 8, 2008 . physrev.physiology.org on February 8, 2008 Physiological Reviews provides state of the art coverage of timely issues in the physiological and biomedical sciences. It is published quarterly in January, April, July, and October by the American Physiological Society, 9650 Rockville Pike, Bethesda MD 20814-3991. Copyright © 2005 by the American Physiological Society. ISSN: 0031-9333, ESSN: 1522-1210. Visit our website at http://www.the-aps.org/. Physiol Rev 86: 1309–1379, 2006; doi:10.1152/physrev.00026.2005. Neuronal Control of Skin Function: The Skin as a Neuroimmunoendocrine Organ DIRK ROOSTERMAN, TOBIAS GOERGE, STEFAN W. SCHNEIDER, NIGEL W. BUNNETT, AND MARTIN STEINHOFF Department of Dermatology, IZKF Mu¨nster, and Boltzmann Institute for Cell and Immunobiology of the Skin, University of Mu¨nster, Mu¨nster, Germany; and Departments of Surgery and Physiology, University of California, San Francisco, California I. -

Cutaneous Manifestations of Systemic Disease
Cutaneous Manifestations of Systemic Disease Dr. Lloyd J. Cleaver D.O. FAOCD FAAD Northeast Regional Medical Center A.T.Still University/KCOM Assistant Vice President/Professor ACOI Board Review Disclosure I have no financial relationships to disclose I will not discuss off label use and/or investigational use in my presentation I do not have direct knowledge of AOBIM questions I have been granted approvial by the AOA to do this board review Dermatology on the AOBIM ”1-4%” of exam is Dermatology Table of Test Specifications is unavailable Review Syllabus for Internal Medicine Large amount of information Cutaneous Multisystem Cutaneous Connective Tissue Conditions Connective Tissue Diease Discoid Lupus Erythematosus Subacute Cutaneous LE Systemic Lupus Erythematosus Scleroderma CREST Syndrome Dermatomyositis Lupus Erythematosus Spectrum from cutaneous to severe systemic involvement Discoid LE (DLE) / Chronic Cutaneous Subacute Cutaneous LE (SCLE) Systemic LE (SLE) Cutaneous findings common in all forms Related to autoimmunity Discoid LE (Chronic Cutaneous LE) Primarily cutaneous Scaly, erythematous, atrophic plaques with sharp margins, telangiectasias and follicular plugging Possible elevated ESR, anemia or leukopenia Progression to SLE only 1-2% Heals with scarring, atrophy and dyspigmentation 5% ANA positive Discoid LE (Chronic Cutaneous LE) Scaly, atrophic plaques with defined margins Discoid LE (Chronic Cutaneous LE) Scaly, erythematous plaques with scarring, atrophy, dyspigmentation DISCOID LUPUS Subacute Cutaneous -

SKIN VERSUS PEMPHIGUS FOLIACEUS and the AUTOIMMUNE GANG Lara Luke, BS, RVT, Dermatology, Purdue Veterinary Teaching Hospital
VETERINARY NURSING EDUCATION SKIN VERSUS PEMPHIGUS FOLIACEUS AND THE AUTOIMMUNE GANG Lara Luke, BS, RVT, Dermatology, Purdue Veterinary Teaching Hospital This program was reviewed and approved by the AAVSB Learning Objective: After reading this article, the participant will be able to dis- RACE program for 1 hour of continuing education in jurisdictions which recognize AAVSB RACE approval. cuss and compare autoimmune diseases that have dermatological afects, includ- Please contact the AAVSB RACE program if you have any ing Pemphigus Foliaceus (PF), Pemphigus Erythematosus (PE), Discoid Lupus comments/concerns regarding this program’s validity or relevancy to the veterinary profession. Erythematosus (DLE), Systemic Lupus Erythematosus (SLE). In addition, the reader will become familiar with diagnostic and treatment techniques. FUNCTION OF THE SKIN Te skin is the largest organ of the body. Along with sensory function, it provides a barrier between the inside and outside world. Te epidermis is composed of the following fve layers: stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum. Te stratum lucidum is found only on the nasal planum and footpads. When the cells of the epidermis are disrupted by systemic disease, the barrier is also disrupted. Clinical signs of skin disease will bring the patient into the veterinarian’s ofce for diagnosis. 32 THE NAVTA JOURNAL | NAVTA.NET VETERINARY NURSING EDUCATION THE PEMPHIGUS COMPLEX article.3 Histologically it shares characteris- Pemphigus Foliaceus tics of both PF and DLE.1 This classifcation PF is an immune mediated pustular disor- is still considered controversial and PE may der included in a group of diseases known just be a localized variant of PF.1 as the pemphigus complex. -
Reverse Koebner Phenomenon in Vasculitis
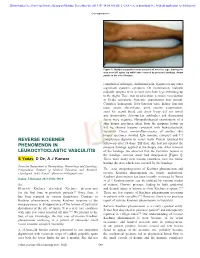
[Downloaded free from http://www.e-ijd.org on Monday, December 05, 2011, IP: 14.99.170.50] || Click here to download free Android application for this journal Correspondence Management of urticaria. Allergy 2006;61:321-31. 2. Hurst M, Spencer CM. Ebastine: An update of its use in allergic disorders. Drugs 2000;59:981-1006. 3. Sastre J. Ebastine in allergic rhinitis and chronic idiopathic urticaria. Allergy 2008;63:1-20. 4. Godse KV. Updosing of antihistamines to improve control of chronic urticaria. Indian J Dermatol Venereol Leprol 2010;76:61-2. 5. Frossard N, Benabdesselam O, Purohit A, Mounedji N, Pauli G. Activity of ebastine (10 and 20 mg) and cetirizine at 24 hours of a steady state treatment in the skin of healthy volunteers. Fundam Clin Pharmacol 2000;14:409-13. 6. Magerl M, Schmolke J, Metz M, Zuberbier T, Siebenhaar F, Maurer M. Prevention of signs and symptoms of dermographic urticaria by single-dose ebastine 20 mg. Clin Exp Dermatol Figure 1: Multiple purpuric lesions present all over the legs, barring the 2009l;34: E137-40. area over left upper leg which was covered by pressure bandage. Arrow points to the site of biopsy 7. Gillen MS, Miller B, Chaikin P, Morganroth J. Effects of supratherapeutic doses of ebastine and terfenadine on the QT interval. Br J Clin Pharmacol 2001;52:201-4. complain of arthralgia, abdominal pain, dyspnea or any other significant systemic symptom. On examination, multiple Access this article online palpable purpura were present over both legs extending up Quick Response Code: to the thighs. -

Skin Manifestations of Systemic Disease
THEME WEIRD SKIN STUFF Adriene Lee BSc(Med), MBBS(Hons), FACD, is visiting dermatologist, St Vincent's Hospital and Monash Medical Centre, and Lecturer, Department of General Practice, Monash University, Victoria. [email protected] Skin manifestations of systemic disease Dermatologic complaints are a common reason for Background presentation to a general practitioner. In such cases, one needs Dermatologic complaints are a common reason for presentation to determine if the complaint may be a manifestation of a more to a general practitioner. In some cases, one needs to determine serious underlying systemic disease. Disorders of the every if the complaint may be a manifestation of a more serious underlying systemic disease. organ system may cause skin symptoms and signs, some of which are due to treatment of these conditions. It is beyond the Objective scope of this review to cover all potential skin manifestations of This article aims to highlight common dermatologic systemic disease. This article highlights the more common, presentations where further assessment is needed to exclude classic and important manifestations in three different groups: an underlying systemic disease, to discuss classic cutaneous features of specific systemic diseases, and to outline rare • ‘When to look further’ – where dermatologic presentations cutaneous paraneoplastic syndromes. require further assessment to exclude underlying systemic disease, and guide appropriate management Discussion • ‘What to look for’ – where certain systemic diseases have Skin manifestations of systemic disease are wide, varied, classic cutaneous findings specific and nonspecific. Generalised pruritus and cutaneous • ‘What not to miss’ – where specific cutaneous signs might be vasculitis are more common cutaneous presentations where an underlying systemic disease may be present and will the initial presentation of an underlying malignancy.