MYELOPATHY ASSOCIATED with SYSTEMIC LUPUS ERYTHEMATOSUS (Erythema Nodosum)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -
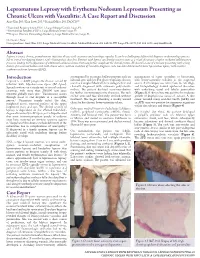
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -

Erythema Nodosum (En)
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 ERYTHEMA NODOSUM (EN) Erythema Nodosum (EN) is a relatively uncommon reaction in the skin consisting of red shiny tender nodular lesions most commonly found on the legs. The erythema refers to the red color that is seen at the surface of the skin. The nodosum refers to the fact that these lesions feel like bumps or nodules underneath the skin surface. Erythema nodosum is a reaction pattern occurring in the subcutaneous tissue and fat. It may be preceded by a low grade fever, fatigue, and joint pains. In about half of the cases, there is an internal condition occurring in the body which contributes to its formation. These include the use of certain medications, certain infections, and a number of other less likely causes. In order to identify cause for the erythema nodosum, it may be necessary to perform blood and laboratory tests. At times, however, the cause cannot be determined and erythema nodosum is considered to be idiopathic in nature. Erythema nodosum often runs an acute course lasting for a brief period from weeks to months. In a small percentage of cases, it can be a more chronic condition. The red nodules are usually confined to the lower legs, but can develop anywhere there is fat under the skin including the thighs, arms, and trunk. Initially, the lesions are more red and inflamed in appearance, but with time become more bruise like. -

Drug Eruptions
DRUG ERUPTIONS http://www.aocd.org A drug eruption is an adverse skin reaction to a drug. Many medications can cause reactions, especially antimicrobial agents, sulfa drugs, NSAIDs, chemotherapy agents, anticonvulsants, and psychotropic drugs. Drug eruptions can imitate a variety of other skin conditions and therefore should be considered in any patient taking medications or that has changed medications. The onset of drug eruptions is usually within 2 weeks of beginning a new drug or within days if it is due to re-exposure to a certain drug. Itching is the most common symptom. Drug eruptions occur in approximately 2-5% of hospitalized patients and in greater than 1% of the outpatient population. Adverse reactions to drugs are more prevalent in women, in the elderly, and in immunocompromised patients. Drug eruptions may be immunologically or non-immunologically mediated. There are 4 types of immunologically mediated reactions, with Type IV being the most common. Type I is immunoglobulin-E dependent and can result in anaphylaxis, angioedema, and urticaria. Type II is cytotoxic and can result in purpura. Type III reactions are immune complex reactions which can result in vasculitis and type IV is a delayed-type reaction which results in contact dermatitis and photoallergic reactions. This is important as different medications are associated with different types of reactions. For example, insulin is related with type I reactions whereas penicillin, cephalosporins, and sulfonamides cause type II reactions. Quinines and salicylates can cause type III reactions and topical medications such as neomycin can cause type IV reactions. The most common drugs that may potentially cause drug eruptions include amoxicillin, trimethoprim sulfamethoxazole, ampicillin, penicillin, cephalosporins, quinidine and gentamicin sulfate. -

Lichen Planus, Erythema Nodosum, and Erythema Multiforme in a Patient with Chronic Hepatitis C Donato Calista, MD, Cesena, Italy Giorgio Landi, MD, Cesena, Italy
Lichen Planus, Erythema Nodosum, and Erythema Multiforme in a Patient With Chronic Hepatitis C Donato Calista, MD, Cesena, Italy Giorgio Landi, MD, Cesena, Italy After identification of the hepatitis C virus (HCV) in the patient experienced weakness and malaise, fol- 1989, evidence was established supporting its role lowed by the onset of 2 distinct dermatoses: bilateral, in the pathogenesis of a number of cutaneous dis- dermal, painful, tender plaques on both shins and eases. This evidence ranges from mere epidemio- confluent bright red papules on his trunk (Figure 3) logic associations, such as lichen planus, to and arms. The patient denied any drug use or the molecular biological investigations that have onset of infections during the previous 2 months. identified the virus in the pathologic tissues of Laboratory investigations showed a rise in cutaneous vasculitis, vasculitis with mixed cryo- serum levels of aspartate aminotransferase (AST) globulinemia, and porphyria cutanea tarda. We (910 U/L) and alanine aminotransferase (ALT) describe a 52-year-old man who was diagnosed (1130 U/L). Serologic markers for hepatitis B, cyto- with chronic hepatitis C, preceding the appear- megalovirus, and Epstein-Barr virus were negative. A ance of lichen planus, erythema nodosum, and qualitative recombinant immunoblot assay on serum erythema multiforme that coincided with the reacti- showed the presence of HCV messenger RNA. Skin vation of viral replication. biopsy specimens obtained from the different skin lesions confirmed the clinical diagnosis of erythema utaneous disorders, such as vasculitis and es- nodosum of the legs and erythema multiforme of the pecially mixed cryoglobulin-associated vasculi- trunk (Figure 4). -

Morbo Serpentino
CLINICAL CARE CONUNDRUM Morbo Serpentino The approach to clinical conundrums by an expert clinician is revealed through the presentation of an actual patient’s case in an approach typical of a morning report. Similarly to patient care, sequential pieces of information are provided to the clinician, who is unfamiliar with the case. The focus is on the thought processes of both the clinical team caring for the patient and the discussant. This icon represents the patient’s case. Each paragraph that follows represents the discussant’s thoughts. Helene Møller Nielsen, MD1*, Shakil Shakar, MD1, Ulla Weinreich MD1, Mary Hansen MD2, Rune Fisker, MD3, Thomas E. Baudendistel, MD4, Paul Aronowitz MD5 1Department of Pulmonary Medicine, Aalborg University Hospital, Aalborg, Denmark; 2Department of Pathology, Aalborg University Hospital, Aal- borg, Denmark; 3Department of Nuclear Medicine, Aalborg University Hospital, Aalborg, Denmark; 4Department of Medicine, Kaiser Permanente, Oakland, California; 5Department of Medicine, University of California, Davis, California. A 58-year-old Danish man presented to an urgent respectively, and to assess visual fields. An afferent pupillary care center due to several months of gradually wors- defect would suggest optic nerve pathology. ening fatigue, weight loss, abdominal pain, and changes in Disorders that could unify the constitutional, abdominal, vision. His abdominal pain was diffuse, constant, and and visual symptoms include systemic inflammatory diseas- moderate in severity. There was no association with meals, es, such as sarcoidosis (which has an increased incidence and he reported no nausea, vomiting, or change in bowel among Northern Europeans), tuberculosis, or cancer. While movements. He also said his vision in both eyes was blur- diabetes mellitus could explain his visual problems, weight ry, but denied diplopia and said the blurring did not im- loss, and fatigue, the absence of polyuria, polydipsia, or po- prove when either eye was closed. -

Erythema Nodosum: an Evaluation of 100 Cases A
Erythema nodosum: an evaluation of 100 cases A. Mert1, H. Kumbasar1, R. Ozaras1, S. Erten2, L. Tasli3, F. Tabak1, R. Ozturk1 1Infectious Diseases and Clinical Microbiology, Cerrahpasa Medical Faculty, Istanbul University; 2Internal Medicine Clinic, Gebze Hospital, Istanbul; 3Dermatology, Cerrahpasa Medical Faculty, Istanbul University, Istanbul. Abstract Objective In this study, we investigated the clinical features, etiology, and also predictive factors of secondary erythema nodosum (EN) in patients with EN. Method A total of 100 patients (mean age: 37 years) diagnosed with EN between 1993 and 2004 in our clinic were included in the study prospectively. A skin biopsy was performed in 46 of the patients. Patients were considered to have secondary EN when an underlying condition was found, and to have primary EN when no such condition was found. For the diagnosis of the underlying diseases, the pertinent diagnostic criteria and/or diagnostic methods were used. Categorical andand continuouscontinuous variablesvariables wwereere comparedcompared byby usingusing chi-squarechi-square andand Mann-WhitneyMann-Whitney U teststests rrespectively.espectively. Multiple regression analysis was applied to the signifi cantly different variables. Results. The majority of the patients were female (female/male: 6/1) and nearly half (47%) of the cases had a determined etiology. The leading etiology was poststreptococcal (11%), followed in decreasing order by primary tuberculosis (10%), sarcoidosis (10%), Behçet’s syndromesyndrome (BS)(BS) (6%),(6%), drugsdrugs (5%),(5%), inflinfl ammatoryammatory bowelbowel diseasesdiseases (IBD)(IBD) (3%),(3%), andand pregnancy (2%). Fifteen (15%) patients complained of cough; the diagnosis was primary tuberculosis in eight cases and sarcoidosis in seven. Four patients with arthritis were diagnosed as having BS (in 3) and Crohn’s diseasedisease (in(in 1).1). -

Current Clinical Issue of Skin Lesions in Patients with Inflammatory Bowel Disease
Clinical Journal of Gastroenterology (2019) 12:501–510 https://doi.org/10.1007/s12328-019-00958-y CLINICAL REVIEW Current clinical issue of skin lesions in patients with inflammatory bowel disease Tomoya Iida1 · Tokimasa Hida2 · Minoru Matsuura3 · Hisashi Uhara2 · Hiroshi Nakase1 Received: 11 January 2019 / Accepted: 28 February 2019 / Published online: 5 March 2019 © Japanese Society of Gastroenterology 2019 Abstract Inflammatory bowel disease (IBD) is associated with a number of extraintestinal complications, including skin lesions. Most reports have shown that skin lesions are found in 10–15% of IBD cases, although this depends on the definition of skin lesions. The representative skin lesions in patients with IBD are erythema nodosum, pyoderma gangrenosum, Sweet’s syndrome, and so on. These lesions are often associated with IBD progression, and intestinal lesions in particular require appropriate treat- ment. Recently, another clinical issue regarding skin lesions in patients with IBD, a so-called paradoxical reaction, during the treatment with anti-tumor necrosis factor (TNF)-α agents has emerged. These reactions are termed paradoxical reactions because the skin lesions sometimes resemble psoriasis, although the anti-TNF-α agents have been historically used to treat psoriasis. Paradoxical reactions are reportedly found in approximately 5–10% of patients using anti-TNF-α agents and are no longer rare. Now that the use of biologics is at its culmination, reports regarding paradoxical reactions are predicted to increase in number; thus, -

Stroger Cook County Hospital, March 2009
Chicago Dermatological Society______________________________________ Craig A. Elmets, MD Dr. Sidney Barsky Lecture John H. Stroger Jr. Hospital of Cook County Dr Elmets’ lecture is funded by the Chicago Dermatological Society ______________________________________________________________________________ 1 Chicago Dermatological Society______________________________________ ______________________________________________________________________________ 2 Chicago Dermatological Society______________________________________ TABLE OF CONTENTS Case Number Page 1. Harlequin ichthyosis 6 2. Erythema nodosum leprosum 8 3. Congenital cutaneous candidiasis 10 4. Prostatic adenocarcinoma with metastasis to the skin 12 5. Unknown # 1 14 6. Benign cutaneous polyarteritis nodosa 15 7. Disseminated discoid lupus erythematosus 19 8. Post-transfusion urticarial vascultis secondary to serum sickness 21 9. Borderline lepromatous leprosy 23 10. Unknown # 2 25 11. Unknown # 3 (video to be presented) 26 12. Exogenous ochronosis 27 13. Kaposi sarcoma 29 14. Primary systemic (AL type) amyloidosis 31 15. Atypical generalized herpes zoster without primary dermatomal involvement 34 16. Secondary syphilis with HIV co-infection 37 17. Epidermolytic hyperkeratosis 39 18. Chronic actinic dermatitis 41 19. Lymphocytic Sweet syndrome with associated acute myelogenous leukemia 43 20. Cutaneous cryptococcus infection 46 ______________________________________________________________________________ 3 Chicago Dermatological Society______________________________________ ______________________________________________________________________________ -

Blanching Rashes
BLANCHING RASHES Facilitators Guide Author Aoife Fox (Edits by the DFTB Team) [email protected] Author Aoife Fox Duration 1-2h Facilitator level Senior trainee/ANP and above Learner level Junior trainee/Staff nurse and Senior trainee/ANP Equipment required None OUTLINE ● Pre-reading for learners ● Basics ● Case 1: Chicken Pox (15 min) ● Case 2: Roseola (15 min) ● Case 3: Scarlet fever (20 min) ● Case 4: Kawasaki disease (including advanced discussion) (25 min) ● Game ● Quiz ● 5 take home learning points PRE-READING FOR LEARNERS BMJ Best Practice - Evaluation of rash in children PEDS Cases - Viral Rashes in Children RCEM Learning - Common Childhood Exanthems American Academy of Dermatology - Viral exanthems 2 Infectious Non-infectious Blanching Blanching Staphylococcus scalded skin syndrome Sunburn Impetigo Eczema Bullous impetigo Urticaria Eczema hepeticum Atopic dermatitis Measles Acne vulgaris Glandular fever/infectious mononucleosis Ichthyosis vulgaris keratosis pilaris Hand foot and mouth disease Salmon patch Erythema infectiosum/Fifth disease Melasma Chickenpox (varicella zoster) Napkin rash Scabies Seborrhoea Tinea corporis Epidermolysis bullosa Tinea capitis Kawasaki disease Molluscum contagiosum Steven-Johnson syndrome Scarlet fever Steven-Johnson syndrome/toxic epi- Lyme disease dermal necrolysis Congenital syphilis Erythema multiforme Congenital rubella Erythema nodosum Herpes simplex Roseola (sixth disease) Non-blanching Epstein-Barr virus Port-wine stain Pityriasis rosea Henoch-Schoenlein purpura Idiopathic thrombocytopenia Acute leukaemia Haemolytic uremic syndrome Trauma Non-blanching Mechanical (e.g. coughing, vomiting – in Meningococcal rash distribution of superior vena cava) 3 BASE Key learning points Image: used with gratitude from Wikipedia.org Definitions/rash description: ● Macule: a flat area of colour change <1 cm in size (e.g., viral exanthem [such as measles and rubella], morbilliform drug eruption). -

Febrile Illness with Skin Rashes Jin Han Kang Department of Pediatrics, College of Medicine, the Catholic University of Korea, Seoul, Korea
Review Article Infection & http://dx.doi.org/10.3947/ic.2015.47.3.155 Infect Chemother 2015;47(3):155-166 Chemotherapy ISSN 2093-2340 (Print) · ISSN 2092-6448 (Online) Febrile Illness with Skin Rashes Jin Han Kang Department of Pediatrics, College of Medicine, The Catholic University of Korea, Seoul, Korea Skin rashes that appear during febrile illnesses are in fact caused by various infectious diseases. Since infectious exanthema- tous diseases range from mild infections that disappear naturally to severe infectious diseases, focus on and basic knowledge of these diseases is very important. But, these include non-infectious diseases, so that comprehensive knowledge of these oth- er diseases is required. Usually, early diagnostic testing for a febrile illness with a rash is inefficient. For clinical diagnosis of diseases accompanied by skin rash and fever, a complete history must be taken, including recent travel, contact with animals, medications, and exposure to forests and other natural environments. In addition, time of onset of symptoms and the character- istics of the rash itself (morphology, location, distribution) could be helpful in the clinical diagnosis. It is also critical to under- stand the patient’s history of specific underlying diseases. However, diagnostic basic tests could be helpful in diagnosis if they are repeated and the clinical course is monitored. Generally, skin rashes are nonspecific and self-limited. Therefore, it could be clinically meaningful as a characteristic diagnostic finding in a very small subset of specific diseases. Key Words: Febrile illness; Skin rash; Infectious disease; Non-infectious disease Introduction non-infectious diseases, so that comprehensive knowledge of these other diseases is required for clinical diagnosis of a fe- When patients with febrile illnesses also develop a rash, they brile illness with a rash. -

Erythema Nodosum As a Reactive Vasculitis, Induced by Letrozole the Rapyin a Patient with Hormone - Sensitive Breast Cancer
Case Report American Journal of Arthritis Published: 13 Feb, 2019 Erythema Nodosum as a Reactive Vasculitis, Induced by Letrozole the Rapyin a Patient with Hormone - Sensitive Breast Cancer Lyubomir Marinchev* and Milena Kirilova Department of Rheumatology, University Hospital Sofiamed, Bulgaria Abstract Introduction: Erythema nodosum is an acute, nodular vasculitis that is usually limited to the extensor aspects of the lower legs. Presumably, it is a hypersensitivity reaction and may occur in association with several systemic diseases or drug therapies. Letrozole, an aromatase inhibitor, is a commonly used drug to treat hormone-sensitive breast cancer. There have been a few cases of aromatase inhibitor induced vasculitis. Presentation of Case: We report the case of a 73-years old woman with relapsing erythema nodosuma few weeks after start of treatment with Letrozole, because of hormone-sensitive breast cancer. The patient was presented with painful erythematous nodules located on the lower limbs and reactive synovitisof theankles. We excluded systemic autoimmune disease, sarcoidosis or tuberculosis; evaluated ANA-antibodies/negative, urine analysis/negative/chest X-ray/normal, TB- spot/negative. Discussion: We accepted that erythema nodosum is associated with the letrozole therapy. It was stopped and we started systemic corticosteroids. After 2 months there were no more erythema nodosum manifestations and we tapered the steroid dose. Conclusion: There are few cases of necrotizing or leucocytoclasticvasculitis induced by aromatase inhibitors. Letrozoleis often used drug for treatment of hormone-sensitive breast cancer, so with this case we would like to report this side effect of Letrozole as rare cause for erythema nodosum. OPEN ACCESS Introduction *Correspondence: Erythema Nodosum (EN) is an acute, nodular, erythematous eruption that usually is limited to Lyubomir Marinchev, Department of the extensor aspects of the lower legs.