Dermatologic Manifestations of Systemic Diseases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pyoderma Gangrenosum and Cobalamin
Teoh et al. BMC Rheumatology (2021) 5:7 https://doi.org/10.1186/s41927-021-00177-4 BMC Rheumatology CASE REPORT Open Access Pyoderma gangrenosum and cobalamin deficiency in systemic lupus erythematosus: a rare but non fortuitous association Sing Chiek Teoh1, Chun Yang Sim2* , Seow Lin Chuah3, Victoria Kok1 and Cheng Lay Teh3 Abstract Background: Pyoderma gangrenosum (PG) is an uncommon, idiopathic, ulcerative neutrophilic dermatosis. In many cases, PG is associated with a wide variety of different disorders but SLE in association with PG is relatively uncommon. In this article we present the case of a middle aged patient with PG as the initial clinical presentation of SLE. We also provide a brief review of cobalamin deficiency which occurred in our patient and evidence-based management options. Case presentation: A 35 years old man presented with a 5 month history of debilitating painful lower limb and scrotal ulcers. This was associated with polyarthralgia and morning stiffness involving both hands. He also complained of swallowing difficulties. He had unintentional weight loss of 10 kg and fatigue. Physical examination revealed alopecia, multiple cervical lymphadenopathies, bilateral parotid gland enlargement and atrophic glossitis. There was Raynaud’s phenomenon noted over both hands and generalised hyper-pigmented fragile skin. Laboratory results disclosed anaemia, leukopenia, hyponatraemia and hypocortisolism. Detailed anaemic workup revealed low serum ferritin and cobalamin level. The autoimmune screen showed positive ANA, anti SmD1, anti SS- A/Ro 52, anti SSA/Ro 60, anti U1-snRNP with low complement levels. Upper gastrointestinal endoscopy with biopsies confirmed atrophic gastritis and duodenitis. Intrinsic factor antibodies and anti-tissue transglutaminase IgA were all negative. -

Evicore Pediatric PVD Imaging Guidelines
CLINICAL GUIDELINES Pediatric Peripheral Vascular Disease (PVD) Imaging Guidelines Version 1.0 Effective January 1, 2021 eviCore healthcare Clinical Decision Support Tool Diagnostic Strategies: This tool addresses common symptoms and symptom complexes. Imaging requests for individuals with atypical symptoms or clinical presentations that are not specifically addressed will require physician review. Consultation with the referring physician, specialist and/or individual’s Primary Care Physician (PCP) may provide additional insight. CPT® (Current Procedural Terminology) is a registered trademark of the American Medical Association (AMA). CPT® five digit codes, nomenclature and other data are copyright 2020 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative values or related listings are included in the CPT® book. AMA does not directly or indirectly practice medicine or dispense medical services. AMA assumes no liability for the data contained herein or not contained herein. © 2020 eviCore healthcare. All rights reserved. Pediatric PVD Imaging Guidelines V1.0 Pediatric Peripheral Vascular Disease (PVD) Imaging Guidelines Procedure Codes Associated with PVD Imaging 3 PEDPVD-1: General Guidelines 5 PEDPVD-2: Vascular Anomalies 10 PEDPVD-3: Vasculitis 15 PEDPVD-4: Disorders of the Aorta and Visceral Arteries 19 PEDPVD-5: Infantile Hemangiomas 25 ______________________________________________________________________________________________________ ©2020 eviCore healthcare. All Rights Reserved. Page 2 of -

PNWD Talk 2016
Best Cases OHSU Kelly Griffith-Bauer, MD Case 1 •Inpatient consult: Possible vasculitis •HPI: 51 y/o gentleman with h/o COPD, recent pneumonia with 3 month history of ulcers on the R foot, unintentional 30lb weight loss •Epistaxis and tongue ulcer Physical Exam Physical Exam Histology •Neutrophilic Vasculitis involving small to medium sized vessels, as seen on step level sections through the entire tissue segment. Case 1 •Elevated ESR, +c-ANCA, cavitary lung mass Diagnosis: Wegener’s Granulomatosis • AKA granulomatosis with polyangiitis (GPA) • Granulomatous inflammation usually involving the upper and lower respiratory tract and focal necrotizing glomerulitis. • Small and medium-sized (“mixed”) vasculitis • Predominant ANCA type/antigen – C/PR3 90%, P/MPO 10% • Findings include palpable purpura, friable gums, Palisaded neutrophilic granulomatous dermatitis (PNGD) (umbilicated papules on extensors, face), subcutaneous nodules, PG-like ulcers, digital necrosis Case 2: • Presented to the OHSU dermatology clinic with an ~6 month history of painful “bumps” involving bilateral palms. • HPI: 47 y/o Native American female with a hx of Primary Biliary Cirrhosis (undergoing liver transplant work up), DM2, HTN. Physical Exam Differential for lesions of the palms/soles: • Calcinosis cutis • Corns and/or callous • Verruca Vulgaris (common and plantar warts) • Xanthoma Striatum Palmare/Plane Xanthomas • Arsenic keratoses • Gouty tophi • Acrokeratosis paraneoplastic of Bazex • Acquired keratodermas (ex, Aquatic syringeal palmar keratoderma) Histology •Nodular and interstitial granulomatous dermatitis with foam cells, consonant with xanthoma. Histology 40x CD68 Diagnosis: Xanthoma Striatum Palmare • Xanthoma striatum palmare = plane xanthomas involving the palmar creases. • Causes of xanthoma striatum palmare include: • Familial dysbetalipoproteinemia (type III). • Primary biliary cirrhosis and other cholestatic liver diseases ( Incr lipoprotein X). -

Sarcoidosis and Pyoderma Gangrenosum, an Unusual
Open Journal of Clinical & Medical Volume 4 (2018) Issue 19 Case Reports ISSN 2379-1039 Sarcoidosis and pyoderma gangrenosum, an unusual combination Naval Mendiratta*; Muzafar Bindroo Ahmed; Shruti Bajad; Rajiva Gupta *Naval Mendiratta Department of Rheumatology and Clinical Immunology, Medanta Hospital Gurgaon, Haryana, India Email: [email protected] Abstract We present a case of unusual combination of Sarcoidosis with refractory Pyoderma Gangrenosum. Pyoderma Gangrenosum has been a reported with other autoimmune disorders like Rheumatoid Arthritis and Ulcerative colitis but it has hardly ever been reported with another rare disease like Sarcoidosis. Here we present a case of 39 year old female, who was diagnosed and treated for Sarcoidosis but later presented to our OPD with worsening skin lesions which were biopsied and diagnosed as Pyoderma Gangrenosum. Not only were they unusual, but they were even refractory to standard medical therapy. Keywords pyoderma; sarcoidosis; refractory pyoderma; cyclophosphamide Abbreviations ESR : Erythrocyte sedimentation rat; CRP: C- Reactive protein; CT: Computerized tomography; EUS: Endoscopic ultrasound; FNAC: Fine needle aspiration cytology; AFB: Acid fast bacilli; OPD: Out patient department; ACE : Angiotensin converting enzyme Case Report 39 year old female, was referred to our OPD for further management once the diagnosis of Sarcoidosis was conirmed. Symptoms started in December 2014, when she had complaints of fever along with cough. Further evaluation was done and a chest CT revealed multiple mediastinal lymph nodes. Patient was started on empiricalanti tubercular drugs (4 drug regimen ) ,which was given for 6 months. She felt better during the treatment course but after a period of 2 months, she started having again low grade fever with myalgia's and arthalgias. -

Skin Test Christina P
SKINTEST Skin Test Christina P. Linton 1. A middle-aged, diabetic woman presents with 6. What is the estimated 5-year survival rate for well-demarcated, yellow-brown, atrophic, telangiectatic melanoma that has spread beyond the original area plaques with a raised, violaceous border on her shins. of involvement to the nearby lymph nodes (but What is the most likely diagnosis? not to distant nodes or organs)? a. Lipodermatosclerosis a. 25% b. Pyoderma gangrenosum b. 41% c. Necrobiosis lipoidica c. 63% d. Erythema nodosum d. 87% 2. Which of the following types of fruit is most likely 7. What is another name for leprosy? to cause phytophotodermatitis? a. von Recklinghausen’s disease a. Pineapple b. MuchaYHabermann disease b. Grapefruit c. Schamberg’s disease c. Kiwi d. Hansen’s disease d. Peach 8. Which of the following is not an expected 3. Hypothyroidism can cause several changes to the skin extracutaneous finding in patients with and skin appendages including all of the following, HenochYScho¨ nlein purpura? except: a. Abdominal pain a. Hyperpigmentation b. Hematuria b. Easy bruising c. Shortness of breath c. Thin, brittle nails d. Arthralgias d. Dry, coarse skin 9. When the term ‘‘papillomatous’’ is used to describe 4. In a patient with neurofibromatosis, which sign refers a skin lesion, it means that the lesion is to the presence of bilateral axillary freckling? a. characterized by multiple fine surface projections. a. Auspitz sign b. erupting like a mushroom or fungus. b. Crowe sign c. characterized by fine fissures and cracks in the skin. c. Russell sign d. sieve like and contains many perforations. -

Skin Lesions in Diabetic Patients
Rev Saúde Pública 2005;39(4) 1 www.fsp.usp.br/rsp Skin lesions in diabetic patients N T Foss, D P Polon, M H Takada, M C Foss-Freitas and M C Foss Departamento de Clínica Médica. Faculdade de Medicina de Ribeirão Preto. Universidade de São Paulo. Ribeirão Preto, SP, Brasil Keywords Abstract Skin diseases. Dermatomycoses. Diabetes mellitus. Metabolic control. Objective It is yet unknown the relationship between diabetes and determinants or triggering factors of skin lesions in diabetic patients. The purpose of the present study was to investigate the presence of unreported skin lesions in diabetic patients and their relationship with metabolic control of diabetes. Methods A total of 403 diabetic patients, 31% type 1 and 69% type 2, underwent dermatological examination in an outpatient clinic of a university hospital. The endocrine-metabolic evaluation was carried out by an endocrinologist followed by the dermatological evaluation by a dermatologist. The metabolic control of 136 patients was evaluated using glycated hemoglobin. Results High number of dermophytosis (82.6%) followed by different types of skin lesions such as acne and actinic degeneration (66.7%), pyoderma (5%), cutaneous tumors (3%) and necrobiosis lipoidic (1%) were found. Among the most common skin lesions in diabetic patients, confirmed by histopathology, there were seen necrobiosis lipoidic (2 cases, 0.4%), diabetic dermopathy (5 cases, 1.2%) and foot ulcerations (3 cases, 0.7%). Glycated hemoglobin was 7.2% in both type 1 and 2 patients with adequate metabolic control and 11.9% and 12.7% in type 1 and 2 diabetic patients, respectively, with inadequate metabolic controls. -

The Prevalence of Cutaneous Manifestations in Young Patients with Type 1 Diabetes
Clinical Care/Education/Nutrition/Psychosocial Research ORIGINAL ARTICLE The Prevalence of Cutaneous Manifestations in Young Patients With Type 1 Diabetes 1 2 MILOSˇ D. PAVLOVIC´, MD, PHD SLAANA TODOROVIC´, MD tions, such as neuropathic foot ulcers; 2 4 TATJANA MILENKOVIC´, MD ZORANA ÐAKOVIC´, MD and 4) skin reactions to diabetes treat- 1 1 MIROSLAV DINIC´, MD RADOSˇ D. ZECEVIˇ , MD, PHD ment (1). 1 5 MILAN MISOVIˇ C´, MD RADOJE DODER, MD, PHD 3 To understand the development of DRAGANA DAKOVIC´, DS skin lesions and their relationship to dia- betes complications, a useful approach would be a long-term follow-up of type 1 OBJECTIVE — The aim of the study was to assess the prevalence of cutaneous disorders and diabetic patients and/or surveys of cuta- their relation to disease duration, metabolic control, and microvascular complications in chil- neous disorders in younger type 1 dia- dren and adolescents with type 1 diabetes. betic subjects. Available data suggest that skin dryness and scleroderma-like RESEARCH DESIGN AND METHODS — The presence and frequency of skin mani- festations were examined and compared in 212 unselected type 1 diabetic patients (aged 2–22 changes of the hand represent the most years, diabetes duration 1–15 years) and 196 healthy sex- and age-matched control subjects. common cutaneous manifestations of Logistic regression was used to analyze the relation of cutaneous disorders with diabetes dura- type 1 diabetes seen in up to 49% of the tion, glycemic control, and microvascular complications. patients (3). They are interrelated and also related to diabetes duration. Timing RESULTS — One hundred forty-two (68%) type 1 diabetic patients had at least one cutaneous of appearance of various cutaneous le- disorder vs. -

Splenectomy for HIV-Related Immune Thrombocytopenia Comparison with Results of Splenectomy for Non-HIV Immune Thrombocytopenic Purpura
ORIGINAL ARTICLE Splenectomy for HIV-Related Immune Thrombocytopenia Comparison With Results of Splenectomy for Non-HIV Immune Thrombocytopenic Purpura Reginald V. N. Lord, FRACS; Maxwell J. Coleman, FRACS; Samuel T. Milliken, FRACP Objective: To determine the effectiveness and safety of tomy, with an elevation of the platelet count to greater splenectomy for patients with human immunodefi- than 1003109/L. After a median follow-up of 26.5 months, ciency virus (HIV)–related immune thrombocytopenia, all but 1 patient had a sustained complete remission with using the results of splenectomy for patients with non- no need for medical therapy for thrombocytopenia. Sple- HIV immune thrombocytopenic purpura as a control nectomy was more effective in the HIV-related throm- group for comparison. bocytopenia group than in the non-HIV immune throm- bocytopenic purpura group, with significantly higher Design: Retrospective study. platelet counts at 1 week and 1 month after splenec- tomy in the HIV group (t test, P=.02 and P=.009, respec- Setting: Tertiary care university hospital. tively). There were significantly fewer patients needing medical therapy for thrombocytopenia after splenec- Patients: Fourteen patients who underwent splenec- tomy in the HIV group (x2 test, P=.02). There were no tomy for symptomatic, medically refractory HIV- remarkable short- or long-term complications in the pa- related immune thrombocytopenia at this hospital from tients with HIV infection, including no overwhelming 1988 to 1997. During the same period, 20 patients had postsplenectomy infections. Three patients have died, and splenectomy for treatment of non-HIV immune throm- 2 patients have developed AIDS since operation. bocytopenic purpura. -

Pyoderma Gangrenosum with Positive Antinuclear Antibody, in the Absence of Systemic Association
Case Report http://dx.doi.org/10.3126/njdvl.v16i1.19418 Pyoderma Gangrenosum with Positive Antinuclear Antibody, in the Absence of Systemic Association Shrestha S1, Aryal A2 1Lecturer, 2Second Year Resident, Department of Dermatology, Dhulikhel Hospital, Kathmandu University-Teaching Hospital, Dhulikhel, Kavre, Nepal. Abstract Pyoderma gangrenosum is an uncommon neutrophilic dermatosis, seen on legs, and infrequently on hands and other anatomical sites. It is associated with systemic diseases in 50-70% of the cases. Antinuclear antibody (ANA) seropositivity has been reported in pyoderma gangrenosum associated with connective tissue disorders. However, there are very few case reports of pyoderma gangrenosum in patients of systemic lupus erythematosus, while we did not find any reports of ANA seropositivity in isolated pyoderma gangrenosum. Hence, we report this unique case of pyoderma gangrenosum with classical clinicohistopathology, positive ANA but no systemic association. As anticipated, our patient responded promptly to steroids. Key words: Antibodies; connective tissue diseases; lupus erythematosus; vasculitis, leukocytoclastic Introduction systemic comorbidi es were elicited from history. She was a nonsmoker. yoderma gangrenosum (PG) is a rare necro zing, Pulcera ve neutrophilic dermatosis.1 It is usually On examina on, pa ent was afebrile with normal associated with various systemic illnesses, but vital signs (BP 100/60 mm of mercury, Pulse 84/m, rarely described in associa on with systemic lupus RR 18/min). Cutaneous examina on revealed fi ve erythematosus (SLE) or an nuclear an body (ANA) annular lesions on sun-exposed sites of hands and seroposi vity. We report this case of PG on sunexposed feet (Figure 1). Among them, only one lesion on right sites, with posi ve ANA and no internal disease. -

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -

Psoriasis, a Systemic Disease Beyond the Skin, As Evidenced by Psoriatic Arthritis and Many Comorbities
1 Psoriasis, a Systemic Disease Beyond the Skin, as Evidenced by Psoriatic Arthritis and Many Comorbities – Clinical Remission with a Leishmania Amastigotes Vaccine, a Serendipity Finding J.A. O’Daly Astralis Ltd, Irvington, NJ USA 1. Introduction Psoriasis is a systemic chronic, relapsing inflammatory skin disorder, with worldwide distribution, affects 1–3% of the world population, prevalence varies according to race, geographic location, and environmental factors (Chandran & Raychaudhuri, 2010; Christophers & Mrowietz, 2003; Farber & Nall, 1974). In Germany, 33,981 from 1,344,071 continuously insured persons in 2005 were diagnosed with psoriasis; thus the one year prevalence was 2.53% in the study group. Up to the age of 80 years the prevalence rate (range: 3.99-4.18%) was increasing with increasing age and highest for the age groups from 50 to 79 years The total rate of psoriasis in children younger than 18 years was 0.71%. The prevalence rates increased in an approximately linear manner from 0.12% at the age of 1 year to 1.2% at the age of 18 years (Schäfer et al., 2011). In France, a case-control study in 6,887 persons, 356 cases were identified (5.16%), who declared having had psoriasis during the previous 12 months (Wolkenstein et al., 2009). The prevalence of psoriasis analyzed across Italy showed that 2.9% of Italians declared suffering from psoriasis (regional range: 0.8-4.5%) in a total of 4109 individuals (Saraceno et al., 2008). The overall rate of comorbidity in subjects with psoriasis aged less than 20 years was twice as high as in subjects without psoriasis. -
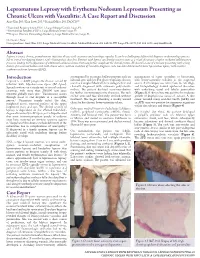
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa.