Scientific Paper Session 4
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Redalyc.Variations in Branching Pattern of the Axillary Artery: a Study
Jornal Vascular Brasileiro ISSN: 1677-5449 [email protected] Sociedade Brasileira de Angiologia e de Cirurgia Vascular Brasil Astik, Rajesh; Dave, Urvi Variations in branching pattern of the axillary artery: a study in 40 human cadavers Jornal Vascular Brasileiro, vol. 11, núm. 1, marzo, 2012, pp. 12-17 Sociedade Brasileira de Angiologia e de Cirurgia Vascular São Paulo, Brasil Available in: http://www.redalyc.org/articulo.oa?id=245023701001 How to cite Complete issue Scientific Information System More information about this article Network of Scientific Journals from Latin America, the Caribbean, Spain and Portugal Journal's homepage in redalyc.org Non-profit academic project, developed under the open access initiative ORIGINAL ARTICLE Variations in branching pattern of the axillary artery: a study in 40 human cadavers Variações na ramificação do padrão da artéria axilar: um estudo em 40 cadáveres humanos Rajesh Astik1, Urvi Dave2 Abstract Background: Variations in the branching pattern of the axillary artery are a rule rather than an exception. The knowledge of these variations is of anatomical, radiological, and surgical interest to explain unexpected clinical signs and symptoms. Objective: The large percentage of variations in branching pattern of axillary artery is making it worthwhile to take any anomaly into consideration. The type and frequency of these vascular variations should be well understood and documented, as increasing performance of coronary artery bypass surgery and other cardiovascular surgical procedures. The objective of this study is to observe variations in axillary artery branches in human cadavers. Methods: We dissected 80 limbs of 40 human adult embalmed cadavers of Asian origin and we have studied the branching patterns of the axillary artery. -

Risk of Encountering Dorsal Scapular and Long Thoracic Nerves During Ultrasound-Guided Interscalene Brachial Plexus Block with Nerve Stimulator
Korean J Pain 2016 July; Vol. 29, No. 3: 179-184 pISSN 2005-9159 eISSN 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.179 | Original Article | Risk of Encountering Dorsal Scapular and Long Thoracic Nerves during Ultrasound-guided Interscalene Brachial Plexus Block with Nerve Stimulator Department of Anesthesiology and Pain Medicine, Wonkwang University College of Medicine, Wonkwang Institute of Science, Iksan, *Department of Anesthesiology and Pain Medicine, Presbyterian Medical Center, University of Seonam College of Medicine, Jeonju, Korea Yeon Dong Kim, Jae Yong Yu*, Junho Shim*, Hyun Joo Heo*, and Hyungtae Kim* Background: Recently, ultrasound has been commonly used. Ultrasound-guided interscalene brachial plexus block (IBPB) by posterior approach is more commonly used because anterior approach has been reported to have the risk of phrenic nerve injury. However, posterior approach also has the risk of causing nerve injury because there are risks of encountering dorsal scapular nerve (DSN) and long thoracic nerve (LTN). Therefore, the aim of this study was to evaluate the risk of encountering DSN and LTN during ultrasound-guided IBPB by posterior approach. Methods: A total of 70 patients who were scheduled for shoulder surgery were enrolled in this study. After deciding insertion site with ultrasound, awake ultrasound-guided IBPB with nerve stimulator by posterior approach was performed. Incidence of muscle twitches (rhomboids, levator scapulae, and serratus anterior muscles) and current intensity immediately before muscle twitches disappeared were recorded. Results: Of the total 70 cases, DSN was encountered in 44 cases (62.8%) and LTN was encountered in 15 cases (21.4%). Both nerves were encountered in 10 cases (14.3%). -
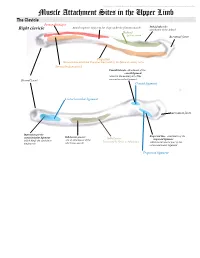
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major -

Examination of the Shoulder Bruce S
Examination of the Shoulder Bruce S. Wolock, MD Towson Orthopaedic Associates 3 Joints, 1 Articulation 1. Sternoclavicular 2. Acromioclavicular 3. Glenohumeral 4. Scapulothoracic AC Separation Bony Landmarks 1. Suprasternal notch 2. Sternoclavicular joint 3. Coracoid 4. Acromioclavicular joint 5. Acromion 6. Greater tuberosity of the humerus 7. Bicipital groove 8. Scapular spine 9. Scapular borders-vertebral and lateral Sternoclavicular Dislocation Soft Tissues 1. Rotator Cuff 2. Subacromial bursa 3. Axilla 4. Muscles: a. Sternocleidomastoid b. Pectoralis major c. Biceps d. Deltoid Congenital Absence of Pectoralis Major Pectoralis Major Rupture Soft Tissues (con’t) e. Trapezius f. Rhomboid major and minor g. Latissimus dorsi h. Serratus anterior Range of Motion: Active and Passive 1. Abduction - 90 degrees 2. Adduction - 45 degrees 3. Extension - 45 degrees 4. Flexion - 180 degrees 5. Internal rotation – 90 degrees 6. External rotation – 45 degrees Muscle Testing 1. Flexion a. Primary - Anterior deltoid (axillary nerve, C5) - Coracobrachialis (musculocutaneous nerve, C5/6 b. Secondary - Pectoralis major - Biceps Biceps Rupture- Longhead Muscle Testing 2. Extension a. Primary - Latissimus dorsi (thoracodorsal nerve, C6/8) - Teres major (lower subscapular nerve, C5/6) - Posterior deltoid (axillary nerve, C5/6) b. Secondary - Teres minor - Triceps Abduction Primary a. Middle deltoid (axillary nerve, C5/6) b. Supraspinatus (suprascapular nerve, C5/6) Secondary a. Anterior and posterior deltoid b. Serratus anterior Deltoid Ruputure Axillary Nerve Palsy Adduction Primary a. Pectoralis major (medial and lateral pectoral nerves, C5-T1 b. Latissimus dorsi (thoracodorsal nerve, C6/8) Secondary a. Teres major b. Anterior deltoid External Rotation Primary a. Infraspinatus (suprascapular nerve, C5/6) b. Teres minor (axillary nerve, C5) Secondary a. -

Dorsal Scapular Nerve Neuropathy: a Narrative Review of the Literature Brad Muir, Bsc.(Hons), DC, FRCCSS(C)1
ISSN 0008-3194 (p)/ISSN 1715-6181 (e)/2017/128–144/$2.00/©JCCA 2017 Dorsal scapular nerve neuropathy: a narrative review of the literature Brad Muir, BSc.(Hons), DC, FRCCSS(C)1 Objective: The purpose of this paper is to elucidate Objectif : Ce document a pour objectif d’élucider this little known cause of upper back pain through a cette cause peu connue de douleur dans le haut du narrative review of the literature and to discuss the dos par un examen narratif de la littérature, ainsi que possible role of the dorsal scapular nerve (DSN) in de discuter du rôle possible du nerf scapulaire dorsal the etiopathology of other similar diagnoses in this (NSD) dans l’étiopathologie d’autres diagnostics area including cervicogenic dorsalgia (CD), notalgia semblables dans ce domaine, y compris la dorsalgie paresthetica (NP), SICK scapula and a posterolateral cervicogénique (DC), la notalgie paresthésique (NP), arm pain pattern. l’omoplate SICK et un schéma de douleur postéro- Background: Dorsal scapular nerve (DSN) latérale au bras. neuropathy has been a rarely thought of differential Contexte : La neuropathie du nerf scapulaire dorsal diagnosis for mid scapular, upper to mid back and (NSD) constitue un diagnostic différentiel rare pour la costovertebral pain. These are common conditions douleur mi-scapulaire, costo-vertébrale et au bas/haut presenting to chiropractic, physiotherapy, massage du dos. Il s’agit de troubles communs qui surgissent therapy and medical offices. dans les cabinets de chiropratique, de physiothérapie, de Methods: The methods used to gather articles for this massothérapie et de médecin. paper included: searching electronic databases; and Méthodologie : Les méthodes utilisées pour hand searching relevant references from journal articles rassembler les articles de ce document comprenaient la and textbook chapters. -

Variations in the Branching Pattern of the Radial Nerve Branches to Triceps Brachii
Review Article Clinician’s corner Images in Medicine Experimental Research Case Report Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2019/39912.12533 Original Article Postgraduate Education Variations in the Branching Pattern Case Series of the Radial Nerve Branches to Anatomy Section Triceps Brachii Muscle Short Communication MYTHRAEYEE PRASAD1, BINA ISAAC2 ABSTRACT Results: The branching patterns seen were types A 1 (3.6%), Introduction: The axillary nerve arises from the posterior cord B1 (1st pattern) 1 (3.6%), B2 (2nd pattern) 1 (3.6%), and C3 of the brachial plexus and supplies the deltoid and teres minor 22 (78.6%). Two new patterns observed were: type B2 muscles. Axillary nerve injuries lead to abduction and external (6th pattern) 1 (3.6%) and type D (2nd pattern) 2 (7.1%). The long rotation weakness. In such cases, branches to the heads of head had single innervation in 89.3% cases and the lateral and triceps brachii muscle have been transferred to the axillary nerve medial heads had dual innervation in 10.7% and 7.1% cases to establish reinnervation of the deltoid muscle. In addition, the respectively. triceps nerve branches can be nerve recipients to reinstitute Conclusion: The knowledge of the different branching patterns elbow extension. that are present will help surgeons to identify the most suitable Aim: To study the different branching patterns of the radial radial nerve branch to triceps brachii that can be used for nerve nerve branches to triceps brachii muscle. transfer to restore the motor function of the deltoid muscle or to reanimate the triceps brachii muscle. -

Pectoral Region and Axilla Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Pectoral Region and Axilla Doctors Notes Notes/Extra explanation Editing File Objectives By the end of the lecture the students should be able to : Identify and describe the muscles of the pectoral region. I. Pectoralis major. II. Pectoralis minor. III. Subclavius. IV. Serratus anterior. Describe and demonstrate the boundaries and contents of the axilla. Describe the formation of the brachial plexus and its branches. The movements of the upper limb Note: differentiate between the different regions Flexion & extension of Flexion & extension of Flexion & extension of wrist = hand elbow = forearm shoulder = arm = humerus I. Pectoralis Major Origin 2 heads Clavicular head: From Medial ½ of the front of the clavicle. Sternocostal head: From; Sternum. Upper 6 costal cartilages. Aponeurosis of the external oblique muscle. Insertion Lateral lip of bicipital groove (humerus)* Costal cartilage (hyaline Nerve Supply Medial & lateral pectoral nerves. cartilage that connects the ribs to the sternum) Action Adduction and medial rotation of the arm. Recall what we took in foundation: Only the clavicular head helps in flexion of arm Muscles are attached to bones / (shoulder). ligaments / cartilage by 1) tendons * 3 muscles are attached at the bicipital groove: 2) aponeurosis Latissimus dorsi, pectoral major, teres major 3) raphe Extra Extra picture for understanding II. Pectoralis Minor Origin From 3rd ,4th, & 5th ribs close to their costal cartilages. Insertion Coracoid process (scapula)* 3 Nerve Supply Medial pectoral nerve. 4 Action 1. Depression of the shoulder. 5 2. Draw the ribs upward and outwards during deep inspiration. *Don’t confuse the coracoid process on the scapula with the coronoid process on the ulna Extra III. -

A Comprehensive Review of Anatomy and Regional Anesthesia Techniques of Clavicle Surgeries
vv ISSN: 2641-3116 DOI: https://dx.doi.org/10.17352/ojor CLINICAL GROUP Received: 31 March, 2021 Research Article Accepted: 07 April, 2021 Published: 10 April, 2021 *Corresponding author: Dr. Kartik Sonawane, Uncovering secrets of the Junior Consultant, Department of Anesthesiol- ogy, Ganga Medical Centre & Hospitals, Pvt. Ltd. Coimbatore, Tamil Nadu, India, E-mail: beauty bone: A comprehensive Keywords: Clavicle fractures; Floating shoulder sur- gery; Clavicle surgery; Clavicle anesthesia; Procedure review of anatomy and specific anesthesia; Clavicular block regional anesthesia techniques https://www.peertechzpublications.com of clavicle surgeries Kartik Sonawane1*, Hrudini Dixit2, J.Balavenkatasubramanian3 and Palanichamy Gurumoorthi4 1Junior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 2Fellow in Regional Anesthesia, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 3Senior Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India 4Consultant, Department of Anesthesiology, Ganga Medical Centre & Hospitals, Pvt. Ltd., Coimbatore, Tamil Nadu, India Abstract The clavicle is the most frequently fractured bone in humans. General anesthesia with or without Regional Anesthesia (RA) is most frequently used for clavicle surgeries due to its complex innervation. Many RA techniques, alone or in combination, have been used for clavicle surgeries. These include interscalene block, cervical plexus (superficial and deep) blocks, SCUT (supraclavicular nerve + selective upper trunk) block, and pectoral nerve blocks (PEC I and PEC II). The clavipectoral fascial plane block is also a safe and simple option and replaces most other RA techniques due to its lack of side effects like phrenic nerve palsy or motor block of the upper limb. -

Axillary Nerve Injury Associated with Sports
Neurosurg Focus 31 (5):E10, 2011 Axillary nerve injury associated with sports SANGKOOK LEE, M.D.,1 KRIANGSAK SAETIA, M.D.,2 SUPARNA SAHA, M.D.,1 DAVID G. KLINE, M.D.,3 AND DANIEL H. KIM, M.D.1 1Department of Neurosurgery, Baylor College of Medicine, Houston, Texas; 2Division of Neurosurgery, Department of Surgery, Ramathibodi Hospital, Mahidol University, Bangkok, Thailand; and 3Department of Neurosurgery, Louisiana State University Health Sciences Center, New Orleans, Louisiana Object. The aim of this retrospective study was to present and investigate axillary nerve injuries associated with sports. Methods. This study retrospectively reviewed 26 axillary nerve injuries associated with sports between the years 1985 and 2010. Preoperative status of the axillary nerve was evaluated by using the Louisiana State University Health Science Center (LSUHSC) grading system published by the senior authors. Intraoperative nerve action potential recordings were performed to check nerve conduction and assess the possibility of resection. Neurolysis, suture, and nerve grafts were used for the surgical repair of the injured nerves. In 9 patients with partial loss of function and 3 with complete loss, neurolysis based on nerve action potential recordings was the primary treatment. Two patients with complete loss of function were treated with resection and suturing and 12 with resection and nerve grafting. The minimum follow-up period was 16 months (mean 20 months). Results. The injuries were associated with the following sports: skiing (12 cases), football (5), rugby (2), base- ball (2), ice hockey (2), soccer (1), weightlifting (1), and wrestling (1). Functional recovery was excellent. Neurolysis was performed in 9 cases, resulting in an average functional recovery of LSUHSC Grade 4.2. -

Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies
Electrodiagnosis of Brachial Plexopathies and Proximal Upper Extremity Neuropathies Zachary Simmons, MD* KEYWORDS Brachial plexus Brachial plexopathy Axillary nerve Musculocutaneous nerve Suprascapular nerve Nerve conduction studies Electromyography KEY POINTS The brachial plexus provides all motor and sensory innervation of the upper extremity. The plexus is usually derived from the C5 through T1 anterior primary rami, which divide in various ways to form the upper, middle, and lower trunks; the lateral, posterior, and medial cords; and multiple terminal branches. Traction is the most common cause of brachial plexopathy, although compression, lacer- ations, ischemia, neoplasms, radiation, thoracic outlet syndrome, and neuralgic amyotro- phy may all produce brachial plexus lesions. Upper extremity mononeuropathies affecting the musculocutaneous, axillary, and supra- scapular motor nerves and the medial and lateral antebrachial cutaneous sensory nerves often occur in the context of more widespread brachial plexus damage, often from trauma or neuralgic amyotrophy but may occur in isolation. Extensive electrodiagnostic testing often is needed to properly localize lesions of the brachial plexus, frequently requiring testing of sensory nerves, which are not commonly used in the assessment of other types of lesions. INTRODUCTION Few anatomic structures are as daunting to medical students, residents, and prac- ticing physicians as the brachial plexus. Yet, detailed understanding of brachial plexus anatomy is central to electrodiagnosis because of the plexus’ role in supplying all motor and sensory innervation of the upper extremity and shoulder girdle. There also are several proximal upper extremity nerves, derived from the brachial plexus, Conflicts of Interest: None. Neuromuscular Program and ALS Center, Penn State Hershey Medical Center, Penn State College of Medicine, PA, USA * Department of Neurology, Penn State Hershey Medical Center, EC 037 30 Hope Drive, PO Box 859, Hershey, PA 17033. -

Radial Medial Head Triceps Branch Transfer to Axillary Nerve by Axillary Approach Acesso Ao Nervo Axilar Por Via Axilar Anterior
THIEME 134 Review Article | Artigo de Revisão Radial Medial Head Triceps Branch Transfer to Axillary Nerve by Axillary Approach Acesso ao nervo axilar por via axilar anterior José Marcos Pondé 1 Lazaro Santos 2 João Pedro Magalhaes 2 Ana Flavia D ’Álmeida 2 1 Department of Neurosciences and Mental Health, Universidade Address for correspondence José Marcos Pondé, MD, PhD, Av. Paulo Federal da Bahia (UFBA), Salvador, Bahia, Brazil VI, 111, Pituba, Salvador, BA, Brazil 41810-000 2 Bahian School of Medicine and Public Health, Salvador, Bahia, Brazil (e-mail: [email protected]). Arq Bras Neurocir 2015;34:134 –138. - Abstract Objective To describe axillary approach for axillary nerve transfer with radial nerve branch in brachial plexus lesions. Methods Six patients aged 24 to 54 (mean 30) years with traumatic superior trunk brachial plexus injury underwent axillary approach between October 2011 and April 2012. On physical examination prior to surgery, they could not perform shoulder abduction, external rotation, or elbow flexion. Surgical approach was made through axillary pathway without any muscular section. The transfer was done with the radial branch to the medial head of triceps. In addition to transfer to axillary nerve, each Keywords patient had spinal accessory nerve transferred to suprascapular nerve and ulnar nerve ► axillary nerve fascicle transferred to musculocutaneous nerve. ► brachial plexus Conclusion Theaxillary approach allowseasyaccesstoaxillarynerveand, therefore, is ► transfer a feasible pathway to transferences involving this nerve. Resumo Objetivo Apresentar via axilar por transferência de nervo axilar com ramo de nervo radial em lesões do plexus braquial. Métodos Seis pacientes com idade entre 24 e 54 anos (média de 30) com lesão braquial traumática do plexus no tronco superior submetidos a via axilar entre outubro de 2011 e abril de 2012. -

Original Article
[Downloaded free from http://www.internationalshoulderjournal.org on Tuesday, January 27, 2009] Original Article A contribution to the calculation of a safe deltoid split Gulihar Abhinav, Balasubramanian Sivaraman, Nixon Matthew, Taylor Grahame J.S. ABSTRACT Leicester Medical School and GlenÞ eld Hospital, Leicester, UK. Purpose: Traditional teaching suggests that a safe deltoid split should extend no more than 5 cm from the lateral edge of the acromion. However, there are reports of nerves lying within this Correspondence: Mr Abhinav Gulihar distance. Our aim was to redeÞ ne the safe maximum split and also to study the inß uence of arm Department of Orthopedics, length and position. GlenÞ eld Hospital, Materials and Methods: Thirty cadaveric shoulders were dissected using the deltoid-splitting Leicester LE3 9QP UK. E-mail: [email protected] approach and the acromion-axillary nerve distance was measured in the neutral position, in abduction, and in adduction. This was correlated to upper arm length. Deltoid splits were measured at the end of 13 deltoid-splitting shoulder operations. Results: The mean acromion-axillary nerve distance was 6.0 cm (SD 0.6; range 4.5–6.5). Abduction brought the nerve closer by 1.5 cm. There was a strong correlation with upper arm length (r = 0.82) but the presence of high individual variability did not allow calculation of a safe deltoid split. The mean deltoid split in 13 open shoulder operations was 3.4 cm. Conclusions: Taking the mean acromion-axillary nerve distance minus three standard deviations as the safe deltoid split would protect 99.7% of nerves.