Having a Ureteroscopy and Stone Removal
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Testosterone Replacement Therapy Is Associated with an Increased Risk of Urolithiasis
World Journal of Urology (2019) 37:2737–2746 https://doi.org/10.1007/s00345-019-02726-6 ORIGINAL ARTICLE Testosterone replacement therapy is associated with an increased risk of urolithiasis Tyler R. McClintock1 · Marie‑Therese I. Valovska2 · Nicollette K. Kwon3 · Alexander P. Cole1,3 · Wei Jiang3 · Martin N. Kathrins1 · Naeem Bhojani4 · George E. Haleblian1 · Tracey Koehlmoos5 · Adil H. Haider3,6 · Shehzad Basaria7 · Quoc‑Dien Trinh1,3 Received: 16 November 2018 / Accepted: 7 March 2019 / Published online: 23 March 2019 © Springer-Verlag GmbH Germany, part of Springer Nature 2019 Abstract Purpose To determine whether TRT in men with hypogonadism is associated with an increased risk of urolithiasis. Methods We conducted a population-based matched cohort study utilizing data sourced from the Military Health System Data Repository (a large military-based database that includes benefciaries of the TRICARE program). This included men aged 40–64 years with no prior history of urolithiasis who received continuous TRT for a diagnosis of hypogonadism between 2006 and 2014. Eligible individuals were matched using both demographics and comorbidities to TRICARE enrollees who did not receive TRT. The primary outcome was 2-year absolute risk of a stone-related event, comparing men on TRT to non-TRT controls. Results There were 26,586 pairs in our cohort. Four hundred and eighty-two stone-related events were observed at 2 years in the non-TRT group versus 659 in the TRT group. Log-rank comparisons showed this to be a statistically signifcant dif- ference in events between the two groups (p < 0.0001). This diference was observed for topical (p < 0.0001) and injection (p = 0.004) therapy-type subgroups, though not for pellet (p = 0.27). -

Jebmh.Com Original Research Article
Jebmh.com Original Research Article URETERIC STRICTURES AN ANALYTICAL STUDY OF AETIOLOGY, PATHOLOGY AND MANAGEMENT Saju P. R1, Rema Priyadarsini2, Vaibhav Vikas3, Praveen Gopi4, Rustum Singh Kaurav5 1Additional Professor, Department of Urology, Trivandrum Medical College, Trivandrum. 2Additional Professor, Department of Pathology, Alappuzha Medical College, Kerala. 3Senior Resident, Department of Urology, Trivandrum Medical College, Trivandrum. 4Senior Resident, Department of Urology, Trivandrum Medical College, Trivandrum. 5Senior Resident, Department of Urology, Trivandrum Medical College, Trivandrum. ABSTRACT BACKGROUND Ureteric strictures are common diseases of India due to tuberculosis, instrumentation, congenital and other reasons. In this study we found that tuberculosis (27%) and instrumentation (27%) were the leading causes of ureteric stricture. MATERIALS AND METHODS This is a prospective study conducted in the Department of Urology, Government Medical College, Thiruvananthapuram. Cases diagnosed as ureteric strictures by IVP and CT scan were taken up for this study. Their clinical features, investigations, treatment and surgical options were studied. RESULTS The total number of cases studied were 11 (5 males and 6 females). We found that three patients had tuberculous strictures and two patients had lower ureteric strictures with obstructive megaureter like presentation. Three cases had upper ureteric strictures with unknown aetiology. Three cases had iatrogenic ureteric strictures secondary to instrumentation. CONCLUSION We concluded from our study that Tuberculosis is a common cause of ureteric stricture. Prior history of instrumentation is the second most common cause of ureteric stricture. Lower ureteric stricture with obstructive megaureter like presentation was also not uncommon and an equally significant group of ureteric strictures had unknown aetiology. KEYWORDS Ureteric Stricture, Tuberculosis, Iatrogenic Stricture, Obstructive Megaureter, Instrumentation. -

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Ureter an Innocent Bystander: Lower Ureteral Stricture Following
Arch Nephrol Urol 2019; 2 (2): 029-032 DOI: 10.26502/anu.2644-2833007 Case Report Ureter an Innocent Bystander: Lower Ureteral Stricture Following Angioembolisation of Uterine Artery Tushar Aditya Narain1, Manjeet Kumar2*, Shrawan Singh1, Gopal Sharma1, Shantanu Tyagi1 1Department of Urology, Postgraduate Institute of Medical Education and Research, Chandigarh, India 2Indira Gandhi Medical College and Hospital (IGMC), Shimla, Himachal Pradesh, India *Corresponding Author: Dr. Manjeet Kumar, Department of Urology, Indira Gandhi Medical College and Hospital (IGMC), Shimla, Himachal Pradesh, India, E-mail: [email protected] Received: 24 May 2019; Accepted: 31 May 2019; Published: 10 June 2019 Abstract Lower ureteric strictures are a common cause for unilateral hydroureteronephrosis, commonly resulting from previous surgeries, weather endoscopic, laproscopic or open. Devascularisation of the ureter resulting in fibrosis forms the underlying pathophysiology of stricture formation. We report a case of ureteral stricture resulting from angioembolization done for a bleeding arteriovenous malformation (AVM) of the uterus. Keywords: Angioembolisation; Stricture; Ureter 1. Introduction The main cause for ureteral stricture are surgical trauma, impacted ureteral stones, extrinsic compression from a tumor and congenital narrowing. Ureteral stricture is the most frequent complication observed in pelvic surgery. Ureteral strictures are typically due to ischemia, resulting in fibrosis. Wolf and colleagues defined a stricture as ischemic, when it follows open surgery or radiation therapy, whereas a stricture is considered nonischemic if it is caused by spontaneous stone passage or a congenital abnormality [1]. We report a case of ureteral stricture which developed after angioembolisation of bilateral uterine artery done for a bleeding arterio-venous malformation of the uterine cavity. -

Onlay Repair Technique for the Management of Ureteral Strictures: a Comprehensive Review
Hindawi BioMed Research International Volume 2020, Article ID 6178286, 11 pages https://doi.org/10.1155/2020/6178286 Review Article Onlay Repair Technique for the Management of Ureteral Strictures: A Comprehensive Review Shengwei Xiong ,1,2,3 Jie Wang,1,2,3 Weijie Zhu,1,2,3 Kunlin Yang,1,2,3 Guangpu Ding,1,2,3 Xuesong Li ,1,2,3 and Daniel D. Eun 4 1Department of Urology, Peking University First Hospital, No. 8 Xishiku St, Xicheng District, Beijing 100034, China 2Institute of Urology, Peking University, No. 8 Xishiku St, Xicheng District, Beijing 100034, China 3National Urological Cancer Center, No. 8 Xishiku St, Xicheng District, Beijing 100034, China 4Department of Urology, Temple University School of Medicine, 255S 17th Street, 7th Floor Medical Tower, Philadelphia, PA 19103, USA Correspondence should be addressed to Xuesong Li; [email protected] and Daniel D. Eun; [email protected] Received 5 March 2020; Revised 29 June 2020; Accepted 6 July 2020; Published 28 July 2020 Academic Editor: Achim Langenbucher Copyright © 2020 Shengwei Xiong et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Ureteroplasty using onlay grafts or flaps emerged as an innovative procedure for the management of proximal and midureteral strictures. Autologous grafts or flaps used commonly in ureteroplasty include the oral mucosae, bladder mucosae, ileal mucosae, and appendiceal mucosae. Oral mucosa grafts, especially buccal mucosa grafts (BMGs), have gained wide acceptance as a graft choice for ureteroplasty. -

Biodegradable Stent with Mtor Inhibitor-Eluting Reduces Progression of Ureteral Stricture
International Journal of Molecular Sciences Article Biodegradable Stent with mTOR Inhibitor-Eluting Reduces Progression of Ureteral Stricture Dong-Ru Ho 1,2,3 , Shih-Horng Su 4, Pey-Jium Chang 2, Wei-Yu Lin 1, Yun-Ching Huang 1, Jian-Hui Lin 1, Kuo-Tsai Huang 1, Wai-Nga Chan 1 and Chih-Shou Chen 1,* 1 Division of Urology, Department of Surgery, Chang Gung Memorial Hospital, Chiayi 613016, Taiwan; [email protected] (D.-R.H.); [email protected] (W.-Y.L.); [email protected] (Y.-C.H.); [email protected] (J.-H.L.); [email protected] (K.-T.H.); [email protected] (W.-N.C.) 2 Department of Medicine, College of Medicine, Chang Gung University, Taoyuan 333323, Taiwan; [email protected] 3 Department of Nursing, Chang Gung University of Science and Technology, Chiayi 613016, Taiwan 4 DuNing Incorperated, Tustin, CA 92780, USA; [email protected] * Correspondence: [email protected]; Tel.: +886-975-353-211 Abstract: In this study, we investigated the effect of mTOR inhibitor (mTORi) drug-eluting biodegrad- able stent (DE stent), a putative restenosis-inhibiting device for coronary artery, on thermal-injury- related ureteral stricture in rabbits. In vitro evaluation confirmed the dose-dependent effect of mTORi, i.e., rapamycin, on fibrotic markers in ureteral component cell lines. Upper ureteral fibro- sis was induced by ureteral thermal injury in open surgery, which was followed by insertion of biodegradable stents, with or without rapamycin drug-eluting. Immunohistochemistry and Western blotting were performed 4 weeks after the operation to determine gross anatomy changes, collagen deposition, expression of epithelial–mesenchymal transition markers, including Smad, α-SMA, and Citation: Ho, D.-R.; Su, S.-H.; Chang, SNAI 1. -

Complications of Ureteroscopic Approaches, Including Incisions
18 Complications of Ureteroscopic Approaches, Including Incisions Farjaad M. Siddiq, MD and Raymond J. Leveillee, MD CONTENTS INTRODUCTION PREPARATION FOR URETEROSCOPY URETERAL ACCESS DILATION OF THE URETERAL ORIFICE: IS IT NECESSARY? COMPLICATIONS OF URETEROSCOPY URETERAL STENTS: ARE THEY NECESSARY? POSTOPERATIVE IMAGING COMPLICATIONS OF URETEROSCOPIC MANAGEMENT OF UPPER TRACT TCC COMPLICATIONS OF URETEROSCOPIC INCISIONS CONCLUSION REFERENCES SUMMARY Ureteroscopy has progressed from cystoscopic examination of a dilated ureter in a child in 1929 and the initial use of rigid ureteroscopes in the 1980s, to its current state of small caliber semirigid and flexible instruments. In this chapter the authors review complications of ureteroscopy including those associated with incisional techniques where one would anticipate a higher incidence of complications. They review the his- tory and development of modern ureteroscopes, focusing on engineering advances. Clinical points made include proper patient selection and preparation; proper use of dilators, wires, and ureteral access sheaths; and the incidence, identification, and man- agement of complications associated with ureterorenoscopy (both intraopertively and postoperatively). Key Words: Ureteroscopy; calculi; urinary stones; stricture or ureter; urothelial carcinoma; surgical complications. From: Advanced Endourology: The Complete Clinical Guide Edited by: S. Y. Nakada and M. S. Pearle © Humana Press Inc., Totowa, NJ 299 300 Siddiq and Leveillee INTRODUCTION Ureteroscopy has progressed from cystoscopic examination of a dilated ureter in a child with posterior urethral valves by Young and McKay (1) in 1929 and the initial use of a rigid ureteroscope by Perez-Castro Ellendt and Martinez-Pineiro (2,3) in the early 1980s, to its current state of small caliber semirigid and flexible instruments. -

Clinical Study of Unilateral Or Bilateral Noncalculus Hydronephrosis and Or Hydroureter
International Journal of Recent Trends in Science And Technology, ISSN 2277-2812 E-ISSN 2249-8109, Volume 10, Issue 3, 2014 pp 438-446 Clinical Study of Unilateral or Bilateral Noncalculus Hydronephrosis and or Hydroureter 1 2 3* Kasabe P. , R. D. Jaykar , Rahul Wagh {1Assistant Professor,2 Associate Professor, 3 Resident} Department of General Surgery, Dr. V. M. Govt. Medical College, Solapur, Maharashtra, INDIA. *Corresponding Address: [email protected] Research Article Abstract: Background: Hydronephrosis is the dilation of the renal to the interruption of flow of urine, it is often due to an pelvis or calyces. Although patients usually presents with some obstructive process. Hydronephrosis is a very common signs and symptoms it can be clinically silent and is diagnosed as condition and it causes significant pain due to obstruction. an incidental finding during evaluation of an unrelated cause. Although calculus is the commonest cause of hydronephosis and Hydronephrosis can result from anatomic or functional hydroureter there are multiple noncalculus aetiology for the same process obstructing the flow of urine which can occur depending on the age and sex of the patient. This study is aimed anywhere from kidneys to the urethral meatus. Symptoms towards meticulous implementation of the accurate diagnostic tools depend on cause, location and duration of the obstruction. for early evaluation of noncalculus hydronephrosis and or Although patients usually presents with some signs and hydroureter and to assess the effectiveness of the early treatment symptoms it can be clinically silent and is diagnosed as towards the renal function sparing. Methods: In this prospective clinical study of 50 patients of hydronephrosis and or hydroureter an incidental finding during evaluation of an unrelated of all age groups and both the genders admitted in the department cause. -

Cystoscopy Insertion / Removal of Ureteric Stent
Tennyson Centre Darwin Private Hospital Suite 19 Suite 5 520 South Road Rocklands Drive Kurralta Park SA 5037 Tiwi NT 0810 P 08 8292 2399 P 08 8920 6212 F 08 8292 2388 F 08 8920 6213 [email protected] [email protected] www.urologicalsolutions.com.au www.urologicalsolutions.com.au CYSTOSCOPY INSERTION / REMOVAL OF URETERIC STENT Providing Specialist Care in South Australia & Northern Territory Associates: Dr Kym Horsell Dr Kim Pese Dr Michael Chong Dr Jason Lee Dr Alex Jay Dr Henry Duncan What is a Ureteric Stent? A ureteric stent is a specially designed hollow tube, made of a flexible plastic material that is placed in the ureter. The length of the stents used in adult patients varies between 22-30cm. 22-30cm long It is designed to stay in the urinary system by having both ends coiled; the top end coils in the kidney and the lower end coils inside the bladder to prevent its displacement. Stents are flexible enough to withstand various body movements. Stents are temporarily placed in the kidney to prevent or relieve obstruction. They allow urine to pass down the ureter, can help to relieve pain (e.g. from a stone/stone fragments), drain infection or help with kidney function if the kidney is obstructed. Having a stent in place will allow the ureter to heal. In the majority of patients, stents are required for only a short duration. This may be just a few days. However, a stent can stay in for up to three months without the need to replace it. -

EAU Guidelines on Urinary Incontinence 2016
EAU Guidelines on Urinary Incontinence in Adults F.C . Burkhard (Chair), M.G. Lucas, L.C. Berghmans, J.L.H.R. Bosch, F. Cruz, G.E. Lemack, A.K. Nambiar, C.G. Nilsson, R. Pickard, A. Tubaro Guidelines Associates: D. Bedretdinova, F. Farag, B.B. Rozenberg © European Association of Urology 2016 TABLE OF CONTENTS PAGE 1. INTRODUCTION 6 1.1 Aim and objectives 6 1.2 Panel composition 6 1.3 Available publications 6 1.4 Publication history 6 2. METHODS 7 2.1 Introduction 7 2.2 Review 7 2.3 Terminology 7 3. DIAGNOSTIC EVALUATION 8 3.1 History and physical examination 8 3.2 Patient questionnaires 8 3.2.1 Questions 8 3.2.2 Evidence 8 3.3 Voiding diaries 9 3.3.1 Questions 10 3.3.2 Evidence 10 3.4 Urinalysis and urinary tract infection 10 3.4.1 Questions 10 3.4.2 Evidence 10 3.5 Post-voiding residual volume 11 3.5.1 Question 11 3.5.2 Evidence 11 3.6 Urodynamics 11 3.6.1 Question 11 3.6.2 Evidence 11 3.6.2.1 Variability 11 3.6.2.2 Diagnostic accuracy 12 3.6.2.3 Does urodynamics influence the outcome of conservative therapy 12 3.6.2.4 Does urodynamics influence the outcome of surgery for urinary incontinence? 12 3.6.2.5 Does urodynamics help to predict complications of surgery for UI? 12 3.6.2.6 Does urodynamics influence the outcome of treatment for post- prostatectomy urinary incontinence in men? 13 3.6.3 Research priority 13 3.7 Pad testing 13 3.7.1 Question 13 3.7.2 Evidence 13 3.7.3 Research priority 14 3.8 Imaging 14 3.8.1 Questions 14 3.8.2 Evidence 14 3.8.3 Research priority 15 4. -
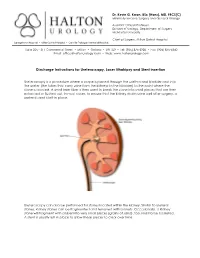
Discharge Instructions for Ureteroscopy, Laser Lithotripsy and Stent Insertion
Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Chief of Surgery, Milton District Hospital Georgetown Hospital • Milton District Hospital • Oakville Trafalgar Memorial Hospital Suite 205 - 311 Commercial Street • Milton • Ontario • L9T 3Z9 • Tel: (905) 875-3920 • Fax: (905) 875-4340 Email: [email protected] • Web: www.haltonurology.com Discharge Instructions for Ureteroscopy, Laser lithotripsy and Stent insertion Ureteroscopy is a procedure where a scope is passed through the urethra and bladder and into the ureter (the tubes that carry urine from the kidneys to the bladder) to the point where the stone is located. A small laser fiber is then used to break the stone into small pieces that are then extracted or flushed out. In most cases, to ensure that the kidney drains urine well after surgery, a ureteral stent is left in place. Ureteroscopy can also be performed for stones located within the kidney. Similar to ureteral stones, kidney stones can be fragmented and removed with baskets. Occasionally, a kidney stone will fragment with a laser into very small pieces (grains of sand), too small to be basketed. A stent is usually left in place to allow these pieces to clear over time. Ureteral Stenting: Almost always after ureteroscopy, a ureteral stent will be placed. This is a thin, hollow, plastic tube that is used temporarily to keep the ureter open and facilitates drainage of urine down to the bladder until it heals. It also allows the urine to drain and any small stone fragments to pass freely. -

EAU Guidelines on Urinary Incontinence in Adults
EAU Guidelines on Urinary Incontinence in Adults F.C . Burkhard (Chair), J.L.H.R. Bosch, F. Cruz, G.E. Lemack, A.K. Nambiar, N. Thiruchelvam, A. Tubaro Guidelines Associates: D. Ambühl, D.A. Bedretdinova, F. Farag, R. Lombardo, M.P. Schneider © European Association of Urology 2018 TABLE OF CONTENTS PAGE 1. INTRODUCTION 8 1.1 Aim and objectives 8 1.1.1 The elderly 8 1.2 Panel composition 8 1.3 Available publications 8 1.4 Publication history 9 1.4.1 Summary of changes. 9 2. METHODS 11 2.1 Introduction 11 2.2 Review 11 2.3 Future goals 11 3. DIAGNOSTIC EVALUATION 11 3.1 History and physical examination 11 3.2 Patient questionnaires 12 3.2.1 Questions 12 3.2.2 Evidence 12 3.2.3 Summary of evidence and recommendations for patient questionnaires 13 3.3 Voiding diaries 14 3.3.1 Question 14 3.3.2 Evidence 14 3.3.3 Summary of evidence and recommendations for voiding diaries 14 3.4 Urinalysis and urinary tract infection 14 3.4.1 Question 14 3.4.2 Evidence 14 3.4.3 Summary of evidence and recommendations for urinalysis 15 3.5 Post-void residual volume 15 3.5.1 Question 15 3.5.2 Evidence 15 3.5.3 Summary of evidence and recommendations for post-void residual 15 3.6 Urodynamics 15 3.6.1 Question 16 3.6.2 Evidence 16 3.6.2.1 Variability 16 3.6.2.2 Diagnostic accuracy 16 3.6.2.3 Question 16 3.6.2.4 Evidence 16 3.6.2.5 Question 16 3.6.2.6 Evidence 16 3.6.2.7 Question 17 3.6.2.8 Evidence 17 3.6.2.9 Question 17 3.6.2.10 Evidence 17 3.6.3 Summary of evidence and recommendations for urodynamics 17 3.6.4 Research priority 18 3.7 Pad testing 18 3.7.1 Questions 18 3.7.2 Evidence 18 3.7.3 Summary of evidence and recommendations for pad testing 18 3.7.4 Research priority 18 3.8 Imaging 18 3.8.1 Questions 19 3.8.2 Evidence 19 3.8.3 Summary of evidence and recommendations for imaging 19 3.8.4 Research priority 19 2 URINARY INCONTINENCE IN ADULTS - LIMITED UPDATE MARCH 2018 4.