Oncologic Emergencies: Pathophysiology, Presentation, Diagnosis, and Treatment
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pathologic Rupture of the Spleen in a Patient with Acute Myelogenous Leukemia and Leukostasis
rev bras hematol hemoter. 2014;36(4):290–292 Revista Brasileira de Hematologia e Hemoterapia Brazilian Journal of Hematology and Hemotherapy www.rbhh.org Case report Pathologic rupture of the spleen in a patient with acute myelogenous leukemia and leukostasis Gil Cunha De Santis ∗, Luciana Correa Oliveira, Aline Fernanda Ramos, Nataly Dantas Fortes da Silva, Roberto Passetto Falcão Universidade de São Paulo (USP), Ribeirão Preto, SP, Brazil article info abstract Article history: Rupture of the spleen can be classified as spontaneous, traumatic, or pathologic. Patho- Received 14 October 2013 logic rupture has been reported in infectious diseases such as infectious mononucleosis, Accepted 14 January 2014 and hematologic malignancies such as acute and chronic leukemias. Splenomegaly is con- Available online 28 May 2014 sidered the most relevant factor that predisposes to splenic rupture. A 66-year-old man with acute myeloid leukemia evolved from an unclassified myeloproliferative neoplasm, Keywords: complaining of fatigue and mild upper left abdominal pain. He was pale and presented Splenomegaly fever and tachypnea. Laboratory analyses showed hemoglobin 8.3 g/dL, white blood cell 9 9 Leukemia count 278 × 10 /L, platelet count 367 × 10 /L, activated partial thromboplastin time (aPTT) Myeloid ratio 2.10, and international normalized ratio (INR) 1.60. A blood smear showed 62% of Acute myeloblasts. The immunophenotype of the blasts was positive for CD117, HLA-DR, CD13, Leukostasis CD56, CD64, CD11c and CD14. Lactate dehydrogenase was 2384 U/L and creatinine 2.4 mg/dL (normal range: 0.7–1.6 mg/dL). Two sessions of leukapheresis were performed. At the end of the second session, the patient presented hemodynamic instability that culminated in cir- culatory shock and death. -

Hematology, Oncology, and Palliative Care Jessica L
Pediatric Acute Care Review Course Hematology, Oncology, and Palliative Care Jessica L. Spruit, DNP, CPNP-AC Assistant Clinical Professor, College of Nursing Wayne State University, Detroit, MI Pediatric Bone Marrow Transplant Nurse Practitioner Children’s Hospital of Michigan, Detroit, MI C.S. Mott Children’s Hospital, Ann Arbor, MI ©2020 Disclosures No relevant financial disclosures ©2020 Learning Objectives Objectives: 1. Describe assessment, evaluation, key diagnostic studies, and management of acute hematology and oncology disorders 2. Identify common presentations of oncologic emergencies and management 3. Introduce palliative care concepts and ethical considerations ©2020 Hematologic Disorders ©2020 Anemia • Reduction in hemoglobin concentration < 2 standard deviations below the mean for age, gender and race • Causes (in acute settings): • Excessive red cell destruction • Excessive blood loss • Deficient red blood cell production • Ineffective hematopoiesis ©2020 Anemia • Clinical Presentation: • Weakness, pallor, confusion, tachycardia, palpitations, flow murmur, diminished pulses, possible jaundice • Diagnostic Evaluation: • Decreased Hgb, Hct • RBC indices and morphology • Increased retic and low MCV = hemoglobinopathy • Increased retic and normal MCV = membrane/enzyme/immune disorder, microangiopathic anemia, DIC, infection‐induced hemolysis, or chronic blood loss • Low MCV (low to sl elevated reticulocyte) = iron deficiency anemia, lead toxicity, Thalassemia trait, Sideroblastic anemia, anemia of chronic disease • High MCV -
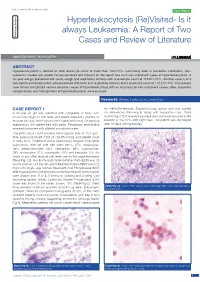
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Novel Emergency Medicine Curriculum Utilizing Self- Directed Learning and the Flipped Classroom Method: Hematologic/Oncologic Emergencies Small Group
CURRICULUM Novel Emergency Medicine Curriculum Utilizing Self- Directed Learning and the Flipped Classroom Method: Hematologic/Oncologic Emergencies Small Group Module Michael G Barrie, MD*, Chad L Mayer, MD*, Colin Kaide, MD*, Emily Kauffman, DO*, Jennifer Mitzman, MD*, Matthew Malone, MD*, Daniel Bachmann, MD*, Ashish Panchal, MD*, Howard Werman, MD*, Benjamin Ostro, MD* and Andrew King, MD* *The Ohio State University Wexner Medical Center, Department of Emergency Medicine, Columbus, OH Correspondence should be addressed to Andrew King, MD, FACEP at [email protected], Twitter: @akingermd Submitted: August 6, 2018; Accepted: November 21, 2018; Electronically Published: January 15, 2019; https://doi.org/10.21980/J8VW56 Copyright: © 2019 Barrie, et al. This is an open access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY 4.0) License. See: http://creativecommons.org/licenses/by/4.0/ ABSTRACT: Audience: This curriculum, created and implemented at The Ohio State University Wexner Medical Center, was designed to educate our emergency medicine (EM) residents, intern to senior resident level, as well as medical students and attending physicians. Introduction: Disorders of the hematologic system represent a wide spectrum of disease, including bleeding disorders, coagulopathies, blood cell disorders, and oncology related disorders. Hematologic related problems often complicate other disease processes, including malignancy. The number of patients diagnosed with malignancy is increasing due to many factors, including, but not limited to, an aging population and the increased ability for early detection.1 Patients with oncologic conditions can present in a variety of ways with a variety of complications,2 and understanding the steps in diagnosis and management are important components of any emergency physician’s training. -

Hemodialysis Leukopenia. Pulmonary Vascular Leukostasis Resulting from Complement Activation by Dialyzer Cellophane Membranes
Hemodialysis leukopenia. Pulmonary vascular leukostasis resulting from complement activation by dialyzer cellophane membranes. P R Craddock, … , K L Brighan, H S Jacob J Clin Invest. 1977;59(5):879-888. https://doi.org/10.1172/JCI108710. Research Article Acute leukopenia occurs in all patients during the first hour of hemodialysis with cellophanemembrane equipment. This transient cytopenia specifically involves granulocytes and monocytes, cells which share plasma membrane reactivity towards activated complement components. The present studies document that complement is activated during exposure of plasma to dialyzer cellophane, and that upon reinfusion of this plasma into the venous circulation, granulocyte and monocyte entrapment in the pulmonary vasculature is induced. During early dialysis, conversion of both C3 and factor B can be demonstrated in plasma as it leaves the dialyzer. Moreover, simple incubation of human plasma with dialyzer cellophane causes conversion of C3 and factor B, accompanied by depletion of total hemolytic complement and C3 but sparing of hemolytic C1. Reinfusion of autologous, cellophane-incubated plasma into rabbits produces selective granulocytopenia and monocytopenia identical to that seen in dialyzed patients. Lungs from such animals reveal striking pulmonary vessel engorgement with granulocytes. The activated complement component(s) responsible for leukostasis has an approximate molecular weight of 7,000-20,000 daltons. Since it is generated in C2-deficient plasma and is associated with factor B conversion, it is suggested that activation of complement by dialysis is predominantly through the altermative pathway. Find the latest version: https://jci.me/108710/pdf Hemodialysis Leukopenia PULMONARY VASCULAR LEUKOSTASIS RESULTING FROM COMPLEMENT ACTIVATION BY DIALYZER CELLOPHANE MEMBRANES PHILIP R. -

Statistical Analysis Plan
Cover Page for Statistical Analysis Plan Sponsor name: Novo Nordisk A/S NCT number NCT03061214 Sponsor trial ID: NN9535-4114 Official title of study: SUSTAINTM CHINA - Efficacy and safety of semaglutide once-weekly versus sitagliptin once-daily as add-on to metformin in subjects with type 2 diabetes Document date: 22 August 2019 Semaglutide s.c (Ozempic®) Date: 22 August 2019 Novo Nordisk Trial ID: NN9535-4114 Version: 1.0 CONFIDENTIAL Clinical Trial Report Status: Final Appendix 16.1.9 16.1.9 Documentation of statistical methods List of contents Statistical analysis plan...................................................................................................................... /LQN Statistical documentation................................................................................................................... /LQN Redacted VWDWLVWLFDODQDO\VLVSODQ Includes redaction of personal identifiable information only. Statistical Analysis Plan Date: 28 May 2019 Novo Nordisk Trial ID: NN9535-4114 Version: 1.0 CONFIDENTIAL UTN:U1111-1149-0432 Status: Final EudraCT No.:NA Page: 1 of 30 Statistical Analysis Plan Trial ID: NN9535-4114 Efficacy and safety of semaglutide once-weekly versus sitagliptin once-daily as add-on to metformin in subjects with type 2 diabetes Author Biostatistics Semaglutide s.c. This confidential document is the property of Novo Nordisk. No unpublished information contained herein may be disclosed without prior written approval from Novo Nordisk. Access to this document must be restricted to relevant parties.This -

If You Will Be Having a Brain Tumor Surgery Soon, There Are a Few Things to Consider Which Can Keep Your Options Open
Version 7 If you will be having a brain tumor surgery soon, there are a few things to consider which can keep your options open. See Chapter 4 for new treatment options! Updated November 1, 2012 Copyright 2012 Musella Foundation For Brain Tumor Research & Information, Inc. 888-295-4740 Al Musella, DPM, Maryann Augusta & The Members of the Grey Ribbon Crusade 1100 Peninsula Blvd. Hewlett, New York 11557 Virtualtrials.com1 Dr. Henry Friedman and Dr. Linda Liau reviewed and approved the contents of this guide. Dr. Friedman Henry S. Friedman, MD, is the Deputy Director of The Preston Robert Tisch Brain Tumor Center at Duke. An internationally recognized neuro-oncologist, Dr. Friedman has a long-standing career in the treatment of children and adults with brain and spinal cord tumors. He has written hundreds of research articles and his work has been showcased on several segments of the CBS program 60 Minutes. Dr. Friedman strongly believes that there is hope for patients who are being treated for brain cancer. Dr. Linda Liau Linda Liau, MD, Ph.D. is the Director of the UCLA Comprehensive Brain Tumor Program at the Ronald Reagan UCLA Medical Center. She is a neurosurgeon with a clinical expertise in intra-operative functional brain mapping and imaging for resection of brain tumors. Dr. Liau’s research is focused on the molecular biology of brain tumors, gene therapy, immunotherapy, and brain cancer vaccines. Her work has been published in journals, textbooks, and highlighted on several television shows. The Brain Tumor Guide for the Newly Diagnosed is sponsored in part by a generous grant from the Richard M. -

Therapeutic Leukapheresis in Patients with Leukostasis Secondary to Acute Myelogenous Leukemia
Journal of Clinical Apheresis 26:181–185 (2011) Therapeutic Leukapheresis in Patients with Leukostasis Secondary to Acute Myelogenous Leukemia Gil Cunha De Santis,1 Luciana Correa Oliveira de Oliveira,1,2*y Lucas Gabriel Maltoni Romano,3 Benedito de Pina Almeida Prado Jr.,1 Belinda Pinto Simoes,1,2 Eduardo Magalhaes Rego,1,2 Dimas Tadeu Covas,1,2 and Roberto Passetto Falcao1,2 1Center for Cell Based Therapy, Medical School of Ribeirao Preto, University of Sao Paulo, Brazil 2Department of Internal Medicine, Hematology Division, Medical School of Ribeirao Preto, University of Sao Paulo, Brazil 3Medical School of Ribeirao Preto, University of Sao Paulo, Brazil Leukostasis is a relatively uncommon but potentially catastrophic complication of acute myelogenous leukemia (AML). Prompt leukoreduction is considered imperative to reduce the high mortality rate in this condition. Leu- kapheresis, usually associated with chemotherapy, is an established approach to diminish blast cell counts. We report a single center experience in managing leukostasis with leukapheresis. Fifteen patients with leukostasis of 187 patients with AML (8.02%) followed at our institution were treated with leukapheresis associated with chem- otherapy. The procedures were scheduled to be performed on a daily basis until clinical improvement was achieved and WBC counts were significantly reduced. Overall and early mortalities, defined as that occurred in the first 7 days from diagnosis, were reported. A high proportion of our patients with leukostasis (46.66%) had a monocytic subtype AML (M4/M5, according to French-American-British classification). The median overall sur- vival was 10 days, despite a significant WBC reduction after the first apheresis procedure (from 200.7 3 109/L to 150.3 3 109/L). -

MEDICAL GRAND ROUNDS Parkland Memorial Hospital June 1, 1978
- MEDICAL GRAND ROUNDS Parkland Memorial Hospital June 1, 1978 OBSTACLES TO THE CONTROL OF ACUTE LEUKEMIA R. Graham Smith, M.D. I. INTRODUCTION Acute leukemia is a group of neoplastic disorders of hematopoiesis in which abnormal clones of immature leukocytes progressively accumulate, leading to death from bone marrow or other vital organ failu~ if treatment is unsuccessful. The overall yearly incidence is about 3.5 cases/10 inhabitants (1); i.e., about 80 cases are annually observed in the Dallas-Fort Worth area. This number will increase as Metroplex hospitals accept patients from an increasingly larger referral area. This review will summarize recent information pertinent to etiology, classification, · diagnosis, and therapy of acute leukemia, with emphasis on the lymphocytic and granulocytic types -- the former the most common malignancy of children, and the latter increasing in frequency with age through at least the 8th decade. A major focus will be an analysis of the variability of prognosis. II. ETIOLOGY Although several unequivocal risk factors have been identified and are tabulated below, in the vast majority of cases of human acute leukemia no predisposing factors can be identified. At least 4 factors can provoke similar diseases in animals; epidemiologic observations suggest that the same factors may contribute to human leukemia. A. Chemical Factors 1. Animal models. 7 ,12- dimethy lbenz(a)anthracene (DMBA) causes leuke mias in mice and rats (2). The widely used L1210 murine leukemia originated in a DBA strain female mouse following skin paintings with m ethy lchola.nthrene (3 ). 2. Human acute leukemia a. Benzene (i) Heavy exposure causes aplastic anemia followed in a small proportion of cases (perhaps 20%) by acute leukemia (4). -

Hematology & Oncology Emergencies
HEMATOLOGIC & ONCOLOGIC EMERGENCIES MEG KELLEY MS, FNP- BC, OCN COURSE OBJECTIVES At the conclusion of this presentation, participants should be able to: 1. Define hematological and oncologic (heme-onc) emergencies 2. Recognize lab and clinical presentations of heme- onc emergencies 3. Review initial work up including basic labs and imaging for patients with concern of heme-onc emergencies •Leukopenia/Leukocytosis •Febrile neutropenia CBC •Hyperleukocytosis/Leukostasis Abnormalities •Thrombocytopenia •DIC, TTP/aHUS Metabolic •Tumor lysis syndrome Abnormalities •Hypercalcemia Compressive/ •SVC syndrome Obstructive •Spinal cord compression Syndromes HEMATOPOIETIC STEM CELL DIFFERENTIATION LEUKOPENIA/NEUTROPENIA Definition: Low white blood cells • Neutropenia is ANC < 1500 (1.0x109) • Severe neutropenia is ANC <500 (0.5x109) Implications: Increased risk of infection • Particularly risk of fungal or bacterial infections if prolonged neutropenia Differentials: • Inherited and acquired conditions • Micronutrient deficiencies • Autoimmune disorders, splenomegaly • Drug-induced neutropenia • Neutropenia with infectious diseases • Acute or chronic bacterial infections, viral or parasitic infections, i.e. HIV, hepatitis, sepsis LEUKOPENIA/NEUTROPENIA WORK UP Acute vs chronic? Recent travel Peripheral smear Obtain baseline labs if Diet CBC with differential possible ETOH use Liver function test GI/malabsorption Labs: Consider issues micronutrients, ANA, Chemical exposures rheumatoid factor Recent infections Screening for infectious diseases Chronicity: -

Blood and Immune Disorders
Blood and immune disorders Mgr. Veronika Borbélyová, PhD. [email protected] www.imbm.sk Blood • 4-6 L • Hematopoetic system • Formed blood elements, not cells!!! • Erythrocytes: transport of O2 and CO2 • Leukocytes: specific and nonspecific immune defenses • Thrombocytes (platelets) – hemostasis • pH 7.35-7.45 Plasma vs. Serum • Blood clot – Blood cells + fibrin Li Heparin K EDTA – yellow liquid = serum. 3 • Anticoagulants: heparin, citrate, EDTA (after centrifugation): – Erythrocytes – Leukocytes – Platelets – Plasma Plasma Albumin plasma osmotic pressure and the maintenance of blood volume serves as a carrier for certain substances Globulins • alpha globulins (transport of bilirubin and steroids) • beta globulins (transport iron and copper) • gamma globulins (constitute the antibodies of the immune system) Fibrinogen conversion to fibrin in the clotting process • Hematocrit (Hct): • ratio of blood cell volume to total blood volume (99% erythrocytes) muži 44±5%; ženy 39±4% Functions of the blood • Transport of various substances: – gases: O2, CO2 – nutrients – metabolic products – vitamins – hormones • Termoregulation - transport of heat (heating, cooling) • Immune response - defense against foreign materials and microorganisms • Hemostasis (prevention of water and nutrients lost) Formation of blood cells • The hematopoietic tissue: – adults: bone marrow – fetus: spleen and liver • pluripotent stem cells • → hematopoietic growth factors → – Myeloid precursor cells – Erythroid precursor cells – Lymphoid precursor cells • Lymphocytes - require further maturation (thymus, bone marrow) • later formed in the spleen and the lymph nodes (lymphopoiesis) • all other precursor cells proliferate and mature up to their final stage in the bone marrow (myelopoiesis) Erythropoietin Thrombopoietin Regulation of hematopoiesis • hormone-like growth factors = cytokines • production: • bone marrow stromal cells • liver and kidney Hematopoietic growth factors (colony-stimulating factors: CSF) 1. -

Tumor Treatment Fields Therapy When It Is Determined to Be Medically Necessary Because the Medical Criteria Shown Below Are Met
Corporate Medical Policy Tumor-Treatment Fields Therapy File Name: tumor_treatment_fields_therapy Origination: 9/2013 Last CAP Review: 8/2021 Next CAP Review: 8/2022 Last Review: 8/2021 Description of Procedure or Service Tumor-treatment fields therapy is a noninvasive technology that uses alternating electrical fields. It is used to treat glioblastoma multiforme and has been proposed for use in other tumor types. Glioblastoma, also known as glioblastoma multiforme (GBM), is the most common form of malignant primary brain tumor in adults, comprising approximately 38% of all brain and central nervous system tumors. The peak incidence for GBM occurs between the ages of 45 and 70 years, with a median age at diagnosis of 64 years. GBMs are grade IV astrocytomas, a rapidly progressing and deadly type of glial cell tumor, which is often resistant to standard chemotherapy. According to the National Comprehensive Cancer Network (NCCN), GBM is the "deadliest brain tumor with only a third of patients surviving for one year and less than 5% living beyond 5 years." Treatment of Newly Diagnosed Glioblastoma Multiforme The primary treatment for newly diagnosed GBM is to resect the tumor to confirm a diagnosis while debulking the tumor to relieve symptoms of increased intracranial pressure or compression. If total resection is not feasible, subtotal resection and open biopsy are options. During surgery, some patients may undergo implantation of the tumor cavity with a carmustine (BCNU) - impregnated wafer. Due to the poor efficacy of local treatment, postsurgical treatment with adjuvant radiotherapy, chemotherapy (typically temozolomide), or a combination of these 2 therapies is recommended. After adjuvant therapy, some patients may undergo maintenance therapy with temozolomide.