Lab Manual Appendicular Skele
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Minimally Invasive Surgical Treatment Using 'Iliac Pillar' Screw for Isolated
European Journal of Trauma and Emergency Surgery (2019) 45:213–219 https://doi.org/10.1007/s00068-018-1046-0 ORIGINAL ARTICLE Minimally invasive surgical treatment using ‘iliac pillar’ screw for isolated iliac wing fractures in geriatric patients: a new challenge Weon‑Yoo Kim1,2 · Se‑Won Lee1,3 · Ki‑Won Kim1,3 · Soon‑Yong Kwon1,4 · Yeon‑Ho Choi5 Received: 1 May 2018 / Accepted: 29 October 2018 / Published online: 1 November 2018 © Springer-Verlag GmbH Germany, part of Springer Nature 2018 Abstract Purpose There have been no prior case series of isolated iliac wing fracture (IIWF) due to low-energy trauma in geriatric patients in the literature. The aim of this study was to describe the characteristics of IIWF in geriatric patients, and to pre- sent a case series of IIWF in geriatric patients who underwent our minimally invasive screw fixation technique named ‘iliac pillar screw fixation’. Materials and methods We retrospectively reviewed six geriatric patients over 65 years old who had isolated iliac wing fracture treated with minimally invasive screw fixation technique between January 2006 and April 2016. Results Six geriatric patients received iliac pillar screw fixation for acute IIWFs. The incidence of IIWFs was approximately 3.5% of geriatric patients with any pelvic bone fractures. The main fracture line exists in common; it extends from a point between the anterosuperior iliac spine and the anteroinferior iliac spine to a point located at the dorsal 1/3 of the iliac crest whether fracture was comminuted or not. Regarding the Koval walking ability, patients who underwent iliac pillar screw fixation technique tended to regain their pre-injury walking including one patient in a previously bedridden state. -

Body Mechanics As the Rotator Cuff Gether in a Cuff-Shape Across the Greater and Lesser Tubercles the on Head of the Humerus
EXPerT CONTENT Body Mechanics by Joseph E. Muscolino | Artwork Giovanni Rimasti | Photography Yanik Chauvin Rotator Cuff Injury www.amtamassage.org/mtj WORKING WITH CLieNTS AFFecTED BY THIS COmmON CONDITION ROTATOR CUFF GROUP as the rotator cuff group because their distal tendons blend and attach to- The four rotator cuff muscles are gether in a cuff-shape across the greater and lesser tubercles on the head of the supraspinatus, infraspinatus, the humerus. Although all four rotator cuff muscles have specific concen- teres minor, and subscapularis (Fig- tric mover actions at the glenohumeral (GH) joint, their primary functional ure 1). These muscles are described importance is to contract isometrically for GH joint stabilization. Because 17 Before practicing any new modality or technique, check with your state’s or province’s massage therapy regulatory authority to ensure that it is within the defined scope of practice for massage therapy. the rotator cuff group has both mover and stabilization roles, it is extremely functionally active and therefore often physically stressed and injured. In fact, after neck and low back conditions, the shoulder is the most com- Supraspinatus monly injured joint of the human body. ROTATOR CUFF PATHOLOGY The three most common types of rotator cuff pathology are tendinitis, tendinosus, and tearing. Excessive physi- cal stress placed on the rotator cuff tendon can cause ir- ritation and inflammation of the tendon, in other words, tendinitis. If the physical stress is chronic, the inflam- matory process often subsides and degeneration of the fascial tendinous tissue occurs; this is referred to as tendinosus. The degeneration of tendinosus results in weakness of the tendon’s structure, and with continued Teres minor physical stress, whether it is overuse microtrauma or a macrotrauma, a rotator cuff tendon tear might occur. -

Pelvic Anatomyanatomy
PelvicPelvic AnatomyAnatomy RobertRobert E.E. Gutman,Gutman, MDMD ObjectivesObjectives UnderstandUnderstand pelvicpelvic anatomyanatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony structures Connective tissue (fascia, ligaments) Pelvic floor and abdominal musculature DescribeDescribe functionalfunctional anatomyanatomy andand relevantrelevant pathophysiologypathophysiology Pelvic support Urinary continence Fecal continence AbdominalAbdominal WallWall RectusRectus FasciaFascia LayersLayers WhatWhat areare thethe layerslayers ofof thethe rectusrectus fasciafascia AboveAbove thethe arcuatearcuate line?line? BelowBelow thethe arcuatearcuate line?line? MedianMedial umbilicalumbilical fold Lateralligaments umbilical & folds folds BonyBony AnatomyAnatomy andand LigamentsLigaments BonyBony PelvisPelvis TheThe bonybony pelvispelvis isis comprisedcomprised ofof 22 innominateinnominate bones,bones, thethe sacrum,sacrum, andand thethe coccyx.coccyx. WhatWhat 33 piecespieces fusefuse toto makemake thethe InnominateInnominate bone?bone? PubisPubis IschiumIschium IliumIlium ClinicalClinical PelvimetryPelvimetry WhichWhich measurementsmeasurements thatthat cancan bebe mademade onon exam?exam? InletInlet DiagonalDiagonal ConjugateConjugate MidplaneMidplane InterspinousInterspinous diameterdiameter OutletOutlet TransverseTransverse diameterdiameter ((intertuberousintertuberous)) andand APAP diameterdiameter ((symphysissymphysis toto coccyx)coccyx) -

Gluteal Region-II
Gluteal Region-II Dr Garima Sehgal Associate Professor King George’s Medical University UP, Lucknow Structures in the Gluteal region • Bones & joints • Ligaments Thickest muscle • Muscles • Vessels • Nerves Thickest nerve • Bursae Learning Objectives By the end of this teaching session Gluteal region –II all the MBBS 1st year students must be able to: • Enumerate the nerves of gluteal region • Write a short note on nerves of gluteal region • Describe the location & relations of sciatic nerve in gluteal region • Enumerate the arteries of gluteal region • Write a short note on arteries of gluteal region • Enumerate the arteries taking part in trochanteric and cruciate anastomosis • Write a short note on trochanteric and cruciate anastomosis • Enumerate the structures passing through greater sciatic foramen • Enumerate the structures passing through lesser sciatic foramen • Enumerate the bursae in relation to gluteus maximus • Enumerate the structures deep to gluteus maximus • Discuss applied anatomy Nerves of Gluteal region (all nerves in gluteal region are branches of sacral plexus) Superior gluteal nerve (L4,L5, S1) Inferior gluteal nerve (L5, S1, S2) FROM DORSAL DIVISIONS Perforating cutaneous nerve (S2,S3) Nerve to quadratus femoris (L4,L5, S1) Nerve to obturator internus (L5, S1, S2) FROM VENTRAL DIVISIONS Pudendal nerve (S2,S3,S4) Sciatic nerve (L4,L5,S1,S2,S3) Posterior cutaneous nerve of thigh FROM BOTH DORSAL &VENTRAL (S1,S2) & (S2,S3) DIVISIONS 1. Superior Gluteal nerve (L4,L5,S1- dorsal division) 1 • Enters through the greater 3 sciatic foramen • Above piriformis 2 • Runs forwards between gluteus medius & gluteus minimus • SUPPLIES: 1. Gluteus medius 2. Gluteus minimus 3. Tensor fasciae latae 2. -

Correlation Analysis of Greater Sciatic Notch Dimensions and His Index in Gender Prediction Based on Hip Bone
International Journal of Multidisciplinary and Current Educational Research (IJMCER) ISSN: 2581-7027 ||Volume|| 3 ||Issue|| 3 ||Pages 175-183 ||2021|| Correlation analysis of greater sciatic notch dimensions and his index in gender prediction based on hip bone 1,Aida Sarač – Hadžihalilović, 2,Emir Beganović, 3,Zurifa Ajanović, 4,Ilvana Hasanbegović, 5,Lejla Dervišević, 6,Senad Šljuka 1,3,4,5Department of Anatomy, Faculty of Medicine, University of Sarajevo, Bosnia and Herzegovina 2 Fachklinik fur Amputationsmedizin. Osterhofen, Bayern, Germany 6 Department of Biology, Faculty of Science, University of Sarajevo, Bosnia and Herzegovina ABSTRACT BACKGROUND/AIM: The greater sciatic notch is important because the gender of the hip bone can be determined on the basis of its appearance and dimensions. Important parameters that are taken into consideration when measuring greater sciatic notch dimensions are: the width and depth of the greater sciatic notch, the width of the upper part of greater sciatic notch. It is important to monitor the ratio of the width and depth of the notch, when assessing the appearance alone. The aim of the study was to determine correlations between the upper part of the greater sciatic notch with the values of it’s width, as well as between depth and width of the upper part of the great sciatic notch. MATERIALS AND METHODS: The study was conducted prospectively on 98 hip bone, of which 56 were single and 42 were within the pelvis. The gender and age of the bones were unknown. All bones belonged to adults in the Bosnian population. The research is based on the osteometric measurements of the width and depth of the greater sciatic notch and width of the upper part of greater sciatic notch, that was used for index calculations of the upper part of the greater sciatic notch. -

Should Joint Presentation File
6/5/2017 The Shoulder Joint Bones of the shoulder joint • Scapula – Glenoid Fossa Infraspinatus fossa – Supraspinatus fossa Subscapular fossa – Spine Coracoid process – Acromion process • Clavicle • Humerus – Greater tubercle Lesser tubercle – Intertubercular goove Deltoid tuberosity – Head of Humerus Shoulder Joint • Bones: – humerus – scapula Shoulder Girdle – clavicle • Articulation – glenohumeral joint • Glenoid fossa of the scapula (less curved) • head of the humerus • enarthrodial (ball and socket) 1 6/5/2017 Shoulder Joint • Connective tissue – glenoid labrum: cartilaginous ring, surrounds glenoid fossa • increases contact area between head of humerus and glenoid fossa. • increases joint stability – Glenohumeral ligaments: reinforce the glenohumeral joint capsule • superior, middle, inferior (anterior side of joint) – coracohumeral ligament (superior) • Muscles play a crucial role in maintaining glenohumeral joint stability. Movements of the Shoulder Joint • Arm abduction, adduction about the shoulder • Arm flexion, extension • Arm hyperflexion, hyperextension • Arm horizontal adduction (flexion) • Arm horizontal abduction (extension) • Arm external and internal rotation – medial and lateral rotation • Arm circumduction – flexion, abduction, extension, hyperextension, adduction Scapulohumeral rhythm • Shoulder Joint • Shoulder Girdle – abduction – upward rotation – adduction – downward rotation – flexion – elevation/upward rot. – extension – Depression/downward rot. – internal rotation – Abduction (protraction) – external rotation -
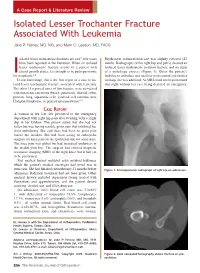
Isolated Lesser Trochanter Fracture Associated with Leukemia
A Case Report & Literature Review Isolated Lesser Trochanter Fracture Associated With Leukemia Jake P. Heiney, MD, MS, and Mark C. Leeson, MD, FACS solated lesser trochanteric fractures are rare1; few cases Erythrocyte sedimentation rate was slightly elevated (23 have been reported in the literature. When an isolated mm/h). Radiographs of the right hip and pelvis showed an lesser trochanteric fracture occurs in a patient with isolated lesser trochanteric avulsion fracture and no signs closed growth plates, it is thought to be pathognomonic of a pathologic process (Figure 1). Given the patient’s Ifor neoplasm.2-4 inability to ambulate and need for pain control and further To our knowledge, this is the first report of a case of iso- workup, she was admitted. As MRI could not be performed lated lesser trochanteric fracture associated with leukemia. that night without her case being declared an emergency, The other 18 reported cases of this fracture were associated with metastatic carcinoma (breast, pancreatic, thyroid, colon, prostate, lung, squamous cell), synovial cell sarcoma, non- Hodgkin lymphoma, or primary plasmacytoma.2-8 CASE REPORT A woman in her late 40s presented to the emergency department with right hip pain after twisting with a slight slip in her kitchen. The patient stated that she had not fallen but was having terrible groin pain that inhibited her from ambulating. She said there had been no groin pain before the incident. She had been seeing an orthopedic surgeon for knee pain on the ipsilateral side for some time. The knee pain was global but had increased tenderness in the medial joint line. -

Applied Anatomy of the Hip RICARDO A
Applied Anatomy of the Hip RICARDO A. FERNANDEZ, MHS, PT, OCS, CSCS • Northwestern University The hip joint is more than just a ball-and- bones fuse in adults to form the easily recog- socket joint. It supports the weight of the nized “hip” bone. The pelvis, meaning bowl head, arms, and trunk, and it is the primary in Latin, is composed of three structures: the joint that distributes the forces between the innominates, the sacrum, and the coccyx pelvis and lower extremities.1 This joint is (Figure 1). formed from the articu- The ilium has a large flare, or iliac crest, Key PointsPoints lation of the proximal superiorly, with the easily palpable anterior femur with the innomi- superior iliac spine (ASIS) anterior with the The hip joint is structurally composed of nate at the acetabulum. anterior inferior iliac spine (AIIS) just inferior strong ligamentous and capsular compo- The joint is considered to it. Posteriorly, the crest of the ilium ends nents. important because it to form the posterior superior iliac spine can affect the spine and (PSIS). With respect to surface anatomy, Postural alignment of the bones and joints pelvis proximally and the PSIS is often marked as a dimple in the of the hip plays a role in determining the femur and patella skin. Clinicians attempting to identify pelvic functional gait patterns and forces associ- distally. The biomechan- or hip subluxations, leg-length discrepancies, ated with various supporting structures. ics of this joint are often or postural faults during examinations use There is a relationship between the hip misunderstood, and the these landmarks. -

H20/1, H20/2, H20/3, H20/4 (1000285 1000286 1000287 1000288) Latin
…going one step further H20/1 (1000285) H20/2 (1000286) H20/3 (1000287) H20/4 (1000288) H20/1, H20/2, H20/3, H20/4 (1000285_1000286_1000287_1000288) Latin H20/1, H20/2, H20/3, H20/4 H20/2, H20/3, H20/4 H20/4 1 Promontorium 38 Lig. longitudinale anterius 78 A. iliaca externa 2 Processus articularis 39 Membrana obturatoria 79 V. iliaca externa superior 40 Lig. sacrospinale 80 A. iliaca interna 3 Vertebra lumbalis V 41 Lig. sacrotuberale 81 V. iliaca interna 4 Processus costalis 42 Lig. inguinale 82 A. iliaca communis dextra 5 Discus intervertebralis 43 Ligg. sacroiliaca anteriora 83 V. cava inferior 6 Crista iliaca 44 Lig. iliolumbale 84 Pars abdominalis aortae 7 Ala ossis ilii 45 Ligg. sacroiliaca interossea 85 A. iliaca communis sinistra 8 Spina iliaca anterior 46 Lig. sacroiliacum posterius 86 N. ischiadicus superior 47 Lig. supraspinale 87 A. femoralis 9 Spina iliaca anterior 88 Plexus sacralis inferior 89 N. dorsalis clitoridis 10 Acetabulum H20/3, H20/4 90 N. pudendus 11 Foramen obturatum 48 Rectum 91 M. piriformis 12 Ramus ossis ischii 49 Ovarium 92 Nn. rectales inferiores 13 Ramus superior ossis pubis 50 Tuba uterina 93 Nn. perineales 14 Ramus inferior ossis pubis 51 Uterus 94 Nn. labiales posteriores 15 Tuberculum pubicum 52 Lig. ovarii proprium 95 V. femoralis 16 Crista pubica 53 Vesica urinaria 96 V. iliaca communis sinistra 17 Symphysis pubica 54 Membrana perinei 97 A. glutealis superior 18 Corpus ossis pubis 55 M. obturatorius internus 98 A. glutealis inferior 19 Tuber ischiadicum 56 M. transversus perinei 99 A. pudenda interna 20 Spina ischiadica profundus 100 ® A. -

Lab #23 Anal Triangle
THE BONY PELVIS AND ANAL TRIANGLE (Grant's Dissector [16th Ed.] pp. 141-145) TODAY’S GOALS: 1. Identify relevant bony features/landmarks on skeletal materials or pelvic models. 2. Identify the sacrotuberous and sacrospinous ligaments. 3. Describe the organization and divisions of the perineum into two triangles: anal triangle and urogenital triangle 4. Dissect the ischiorectal (ischioanal) fossa and define its boundaries. 5. Identify the inferior rectal nerve and artery, the pudendal (Alcock’s) canal and the external anal sphincter. DISSECTION NOTES: The perineum is the diamond-shaped area between the upper thighs and below the inferior pelvic aperture and pelvic diaphragm. It is divided anatomically into 2 triangles: the anal triangle and the urogenital (UG) triangle (Dissector p. 142, Fig. 5.2). The anal triangle is bounded by the tip of the coccyx, sacrotuberous ligaments, and a line connecting the right and left ischial tuberosities. It contains the anal canal, which pierced the levator ani muscle portion of the pelvic diaphragm. The urogenital triangle is bounded by the ischiopubic rami to the inferior surface of the pubic symphysis and a line connecting the right and left ischial tuberosities. This triangular space contains the urogenital (UG) diaphragm that transmits the urethra (in male) and urethra and vagina (in female). A. Anal Triangle Turn the cadaver into the prone position. Make skin incisions as on page 144, Fig. 5.4 of the Dissector. Reflect skin and superficial fascia of the gluteal region in one flap to expose the large gluteus maximus muscle. This muscle has proximal attachments to the posteromedial surface of the ilium, posterior surfaces of the sacrum and coccyx, and the sacrotuberous ligament. -

Approach to the Anterior Pelvis (Enneking Type III Resection) Bruno Fuchs, MD Phd & Franklin H.Sim, MD Indication 1
Approach to the Anterior Pelvis (Enneking Type III Resection) Bruno Fuchs, MD PhD & Franklin H.Sim, MD Indication 1. Tumors of the pubis 2. part of internal and external hemipelvectomy 3. pelvic fractures Technique 1. Positioning: Type III resections involve the excision of a portion of the symphysis or the whole pubis from the pubic symphysis to the lateral margin of the obturator foramen. The best position for these patients is the lithotomy or supine position. The patient is widely prepared and draped in the lithotomy position with the affected leg free to allow manipulation during the procedure. This allows the hip to be flexed, adducted, and externally rotated to facilitate exposure. 2. Landmarks: One should palpate the ASIS, the symphysis with the pubic tubercles, and the ischial tuberosity. 3. Incision: The incision may be Pfannenstiel like with vertical limbs set laterally along the horizontal incision depending on whether the pubic bones on both sides are resected or not. Alternatively, if only one side is resected, a curved incision following the root of the thigh may be used. This incision begins below the inguinal ligament along the medial border of the femoral triangle and extends across the medial thigh a centimeter distal to the inguinal crease and perineum, to curve distally below the ischium several centimeters (Fig.1). 4. Full thickness flaps are raised so that the anterior inferior pubic ramus is shown in its entire length, from the pubic tubercle to the ischial spine. Laterally, the adductor muscles are visualized, cranially the pectineus muscle and the pubic tubercle with the insertion of the inguinal ligament (Fig.2). -

Percutaneous Reduction Techniques
AAOS 2016 Specialty Day Orthopaedic Trauma Associacion (OTA) Percutaneous Reduction Techniques Christian Krettek Trauma Department, Hannover Medical School, Germany [email protected] www.mhh-unfallchirurgie.de Short segment tibial fractures can be stabilized using different implants like plates, screws, external fixators and nails. This syllabus deals mainly with reduction techniques in the context of the use of intramedullary nails. 1.1 PREOPERATIVE PLANNING AND MANAGEMENT 1.1.1 Primary shortening and secondary overdistraction eases definitive nailing In the acute setting primary shortening of a shaft fracture is a helpful strategy to de- crease soft tissue tension and intra-compartmental pressure. However, reduction gets more difficult and more time consuming, the longer the fracture is kept in a shortened position. The concept of primary shortening (acute phase) and secondary (after 3 or 4 days) overdistraction eases definitive nailing. Using a electro-mechanical load cell, our group has compared the reduction forces in patients undergoing femoral nailing after Damage Control in shortend vs overdistracted fracture configuration. In the overdistrac- tion group, the reduction forces were lower (200 N +/-43.1 N vs. 336 N +/- 51.9 N, p = 0.007) and the reduction time was shorter (5.8 min +/-4.0 min vs. 28.3 min +/-21.8 min, p = 0.056). It was concluded, that DCO with the fracture shortened leads to higher restrai- ning forces & prolonged reduction time. Overdistraction should be performed as soon as possible under careful soft-tissue monitoring [1a, 2a]. Primary shortening and secondary overdistraction eases definitive nailing Example of a femoral shaft fracture stabilized in shortening first with an external fixator.