Iliac Crest Herniation Secondary to Autogenous Bone Grafting Found on Osteopathic Examination Christine J
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Minimally Invasive Surgical Treatment Using 'Iliac Pillar' Screw for Isolated
European Journal of Trauma and Emergency Surgery (2019) 45:213–219 https://doi.org/10.1007/s00068-018-1046-0 ORIGINAL ARTICLE Minimally invasive surgical treatment using ‘iliac pillar’ screw for isolated iliac wing fractures in geriatric patients: a new challenge Weon‑Yoo Kim1,2 · Se‑Won Lee1,3 · Ki‑Won Kim1,3 · Soon‑Yong Kwon1,4 · Yeon‑Ho Choi5 Received: 1 May 2018 / Accepted: 29 October 2018 / Published online: 1 November 2018 © Springer-Verlag GmbH Germany, part of Springer Nature 2018 Abstract Purpose There have been no prior case series of isolated iliac wing fracture (IIWF) due to low-energy trauma in geriatric patients in the literature. The aim of this study was to describe the characteristics of IIWF in geriatric patients, and to pre- sent a case series of IIWF in geriatric patients who underwent our minimally invasive screw fixation technique named ‘iliac pillar screw fixation’. Materials and methods We retrospectively reviewed six geriatric patients over 65 years old who had isolated iliac wing fracture treated with minimally invasive screw fixation technique between January 2006 and April 2016. Results Six geriatric patients received iliac pillar screw fixation for acute IIWFs. The incidence of IIWFs was approximately 3.5% of geriatric patients with any pelvic bone fractures. The main fracture line exists in common; it extends from a point between the anterosuperior iliac spine and the anteroinferior iliac spine to a point located at the dorsal 1/3 of the iliac crest whether fracture was comminuted or not. Regarding the Koval walking ability, patients who underwent iliac pillar screw fixation technique tended to regain their pre-injury walking including one patient in a previously bedridden state. -

Lab #23 Anal Triangle
THE BONY PELVIS AND ANAL TRIANGLE (Grant's Dissector [16th Ed.] pp. 141-145) TODAY’S GOALS: 1. Identify relevant bony features/landmarks on skeletal materials or pelvic models. 2. Identify the sacrotuberous and sacrospinous ligaments. 3. Describe the organization and divisions of the perineum into two triangles: anal triangle and urogenital triangle 4. Dissect the ischiorectal (ischioanal) fossa and define its boundaries. 5. Identify the inferior rectal nerve and artery, the pudendal (Alcock’s) canal and the external anal sphincter. DISSECTION NOTES: The perineum is the diamond-shaped area between the upper thighs and below the inferior pelvic aperture and pelvic diaphragm. It is divided anatomically into 2 triangles: the anal triangle and the urogenital (UG) triangle (Dissector p. 142, Fig. 5.2). The anal triangle is bounded by the tip of the coccyx, sacrotuberous ligaments, and a line connecting the right and left ischial tuberosities. It contains the anal canal, which pierced the levator ani muscle portion of the pelvic diaphragm. The urogenital triangle is bounded by the ischiopubic rami to the inferior surface of the pubic symphysis and a line connecting the right and left ischial tuberosities. This triangular space contains the urogenital (UG) diaphragm that transmits the urethra (in male) and urethra and vagina (in female). A. Anal Triangle Turn the cadaver into the prone position. Make skin incisions as on page 144, Fig. 5.4 of the Dissector. Reflect skin and superficial fascia of the gluteal region in one flap to expose the large gluteus maximus muscle. This muscle has proximal attachments to the posteromedial surface of the ilium, posterior surfaces of the sacrum and coccyx, and the sacrotuberous ligament. -

Surgical Approaches to Fractures of the Acetabulum and Pelvis Joel M
Surgical Approaches to Fractures of the Acetabulum and Pelvis Joel M. Matta, M.D. Sponsored by Mizuho OSI APPROACHES TO THE The table will also stably position the ACETABULUM limb in a number of different positions. No one surgical approach is applicable for all acetabulum fractures. KOCHER-LANGENBECK After examination of the plain films as well as the CT scan the surgeon should APPROACH be knowledgeable of the precise anatomy of the fracture he or she is The Kocher-Langenbeck approach is dealing with. A surgical approach will primarily an approach to the posterior be selected with the expectation that column of the Acetabulum. There is the entire reduction and fixation can excellent exposure of the be performed through the surgical retroacetabular surface from the approach. A precise knowledge of the ischial tuberosity to the inferior portion capabilities of each surgical approach of the iliac wing. The quadrilateral is also necessary. In order to maximize surface is accessible by palpation the capabilities of each surgical through the greater or lesser sciatic approach it is advantageous to operate notch. A less effective though often the patient on the PROfx® Pelvic very useful approach to the anterior Reconstruction Orthopedic Fracture column is available by manipulation Table which can apply traction in a through the greater sciatic notch or by distal and/or lateral direction during intra-articular manipulation through the operation. the Acetabulum (Figure 1). Figure 2. Fractures operated through the Kocher-Langenbeck approach. Figure 3. Positioning of the patient on the PROfx® surgical table for operations through the Kocher-Lagenbeck approach. -

An Isolated Iliac Wing Stress Fracture in a Marathon Runner
A Case Report & Literature Review An Isolated Iliac Wing Stress Fracture in a Marathon Runner Louis F. Amorosa, MD, Alana C. Serota, MD, Nathaniel Berman, MD, Dean G. Lorich, MD, and David L. Helfet, MD To our knowledge, there has been only 1 reported case in Abstract the English language literature of an isolated stress fracture of Iliac stress fractures are uncommon and are usually the iliac wing not extending into the sacroiliac joint. In 2003, insufficiency fractures related to osteoporosis. Only Atlihan and colleagues7 reported on a 35-year-old woman who 2 previous case reports of iliac stress fractures in had experienced 2 and a half months of activity-related lateral- runners that extended into the sacroiliac joint, and 1 sided hip pain that became acutely more severe while running previous case of an isolated iliac wing stress fracture a marathon. Magnetic resonance imaging (MRI) showed a not involving the sacroiliac joint were found in the horizontal fracture of the ilium 4 cm cephalad to the hip joint English language literature. with surrounding soft-tissue and muscle edema. The patient We report on a second case of an isolated stress was treated with rest and restricted activity, and the fracture fracture of the iliac wing in a female marathon runner healed. and the associated diagnosis of the female athlete triad. We report a second case of an isolated iliac wing stress Iliac stress fractures can be an occult cause of hip fracture, also in a woman marathon runner, which was as- pain in athletes and should be included in the differ- sociated with the female athlete triad. -

Iliac Crest Bone Graft: a 23-Years Hystory of Infection at Donor Site in Vertebral Arthrodesis and a Review of Current Bone Substitutes
Eur opean Rev iew for Med ical and Pharmacol ogical Sci ences 2016; 20: 4670-4676 Iliac crest bone graft: a 23-years hystory of infection at donor site in vertebral arthrodesis and a review of current bone substitutes L. BABBI, G. BARBANTI-BRODANO, A. GASBARRINI, S. BORIANI Department of Oncological and Degenerative Spine Surgery, Istituto Ortopedico Rizzoli, Bologna, Italy Abstract. – OBJECTIVE : This is an exemplary ognized drawbacks on iliac crest bone graft, in - case report underlining a relevant morbidity which cluding increased operative time, increased blood could be associated to the use of autologous iliac loss, increased donor site morbidity, and a limita - creCsAt bSoEn Re EgPraOfRt (TI:CBG) for spine fusion. tion to the amount that can be realistically har - Starting from 1990, a 25-years- vested for multilevel fusion 1. Successful fusion old woman underwent two subsequent surgical has been demonstrated following iliac crest bone treatments for non-Hodgkin lymphoma vertebral grafting in various applications in lumbar spine localizations. In the second surgery, arthrodesis 2,3 was obtained with autograft through right poste - surgery . However, the morbidity rates associat - rior iliac crest osteotomy. During the chemother - ed with the use of ICBG remain high, with some apy treatment following the surgery, the patient studies reporting up to a 50% rate of persistent suffered from infection at posterior iliac crest donor site pain, paresthesias, hematoma and in - scar, the site ofS ptraepvhioyulosc ogcrcaufts, caauuresueds by methi - fection 4. Other authors 5-8 describe a complication cillin-resistant . She was subjected to surgical debridement and specific rate ranging from 2.4% to 5.8% for major com - antibiotic treatment with local healing and phlo - plications and from 9% to 37.9% for minor com - gosis index reduction. -

Osteotomy of the Anterior Superior Iliac Spine for Pelvic and Acetabular Fracture Surgery
OSTEOTOMY OF THE ANTERIOR SUPERIOR ILIAC SPINE FOR PELVIC AND ACETABULAR FRACTURE SURGERY. H. CLAUDE SAGI PURPOSE: To improve the exposure offered through the lateral window along the iliac crest (window #1) when performing open reduction internal fixation of acetabular and pelvic fractures. BENEFITS: 1) Improved anterior exposure of the sacro-iliac joint 2) Improved exposure of the internal iliac fossa, psoas gutter, pubic root and anterior wall for acetabular fractures, without opening the middle window (#2). 3) Improved access to the posterior column and quadrilateral surface from the lateral window for reduction clamp placement. 4) Improved access to the retro-supra-acetabular bone for reduction clamp placement. 5) Decreased risk of injury to the Lateral Femoral Cutaneous Nerve (LFCN). TECHNIQUE: 1) Leave the distal 2 cm of External Oblique attached to ASIS 2) Develop interval between Tensor Fascia Lata and Sartorius 3) Expose the LFCN 4) Elevate a small portion of TFL off the outer table to expose inter-spinous notch 5) Leave Sartorius attached to ASIS –resulting in a digastric osteotomy 6) Oscillating saw with irrigation or curved osteotome to perform the osteotomy from approximately 2cm proximal to ASIS into the inter-spinous notch 7) LFCN stays with Sartorius as it is retracted medially with ASIS and iliopsoas to expose the psoas gutter, pubic root and anterior wall (release rectus from AIIS) 8) Repair the osteotomy with a single 3.5mm lag-screw into the iliac tubercle. ( I don’t pre-drill it) 9) You will love it. BIBLIOGRAPHY: 1) Reinert CM1, Bosse MJ, Poka A, Schacherer T, Brumback RJ, Burgess AR. -

Myofascial Pain Syndrome of Low Back And
MyofascialMyofascial PainPain SyndromeSyndrome ofof LowLow BackBack andand HipHip MusclesMuscles z QuadratusQuadratus lumborumlumborum z IliopsoasIliopsoas z RectusRectus abdominisabdominis z GluteusGluteus maximusmaximus z GluteusGluteus mediusmedius z GluteusGluteus minimusminimus z PiriformisPiriformis QuadratusQuadratus LumborumLumborum QuadratusQuadratus LumborumLumborum z TheThe mostmost frequentfrequent causecause ofof lowlow backback painpain OriginOrigin InferiorInferior borderborder ofof 12th12th ribrib InsertionInsertion ApicesApices ofof transversetransverse processesprocesses ofof L1L1--4,4, iliolumbariliolumbar ligamentligament andand posteriorposterior thirdthird ofof iliaciliac crestcrest ActionAction FixesFixes 12th12th ribrib duringduring respirationrespiration andand laterallateral flexesflexes trunktrunk SuperficialSuperficial TriggerTrigger PointPoint TriggerTrigger pointpoint verticalvertical layerlayer ofof musclemuscle ReferRefer painpain greatgreat trochantertrochanter ofof femurfemur ÆÆ extendextend alongalong iliaciliac crestcrest ÆÆ lowerlower abdomenabdomen DeepDeep TriggerTrigger PointPoint TriggerTrigger pointpoint diagonaldiagonal layerlayer ofof muscle,muscle, midlinemidline ReferRefer painpain sacralsacral areaarea ÆÆ lowerlower buttockbuttock areaarea ÆÆ glutealgluteal areaarea SpraySpray andand StretchStretch SpraySpray andand StretchStretch IliopsoasIliopsoas IliopsoasIliopsoas IliopsoasIliopsoas Psoas major Psoas minor Iliacus Origin Transverse Bodies of T12 Iliac fossa within processes of L1-5, and -
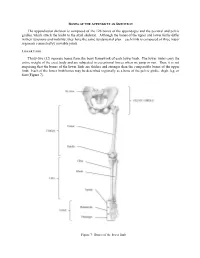
Bones of the Appendicular Skeleton
BONES OF THE APPENDICULAR SKELETON The appendicular skeleton is composed of the 126 bones of the appendages and the pectoral and pelvic girdles, which attach the limbs to the axial skeleton. Although the bones of the upper and lower limbs differ in their functions and mobility, they have the same fundamental plan – each limb is composed of three major segments connected by movable joints. LOWER LIMB Thirty-two (32) separate bones form the bony framework of each lower limb. The lower limbs carry the entire weight of the erect body and are subjected to exceptional forces when we jump or run. Thus, it is not surprising that the bones of the lower limb are thicker and stronger than the comparable bones of the upper limb. Each of the lower limb bones may be described regionally as a bone of the pelvic girdle, thigh, leg, or foot (Figure 7). Figure 7: Bones of the lower limb Pelvic (Hip) Girdle (Marieb / Hoehn – Chapter 7; Pgs. 234 – 238) The pelvic girdle is formed by the paired os coxae (coxal bones). Together with the sacrum and coccyx of the axial skeleton, this group of bones forms the bony pelvis. The ability to bear weight is more important in the pelvic girdle than the pectoral girdle. Thus, the os coxae are heavy and massive with a firm attachment to the axial skeleton. Each os coxa is a result of the fusion of three bones: the ilium, ischium, and pubis. These three bones fuse at the deep hemispherical socket, the acetabulum, which receives the femur. Figure 8: Right os coxa, lateral and medial views A. -

Biomechanical Analysis of Iliac Crest Loading Following Cortico-Cancellous
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by University of Regensburg Publication Server Schmitz et al. Journal of Orthopaedic Surgery and Research (2018) 13:108 https://doi.org/10.1186/s13018-018-0822-1 RESEARCHARTICLE Open Access Biomechanical analysis of iliac crest loading following cortico-cancellous bone harvesting Paul Schmitz1* , Christoph Cornelius Neumann2, Carsten Neumann1, Michael Nerlich1 and Sebastian Dendorfer2 Abstract Background: Iliac crest bone harvesting is a frequently performed surgical procedure widely used to treat bone defects. The objective of this study is to assess the biomechanical quantities related to risk for pelvic fracture after harvesting an autologous bone graft at the anterior iliac crest. Methods: Finite element models with a simulated harvest site (sized 15 × 20 mm, 15 × 35 mm, 30 × 20 mm and 30 × 35 mm) in the iliac wing are created. The relevant loading case is when the ipsilateral leg is lifted off the ground. Musculoskeletal analysis is utilized to compute the muscle and joint forces involved in this motion. These forces are used as boundary conditions for the finite element analyses. Bone tissue stress is analyzed. Results: Critical stress peaks are located between the anterior superior iliac spine (ASIS) and the anterior edge of the harvest site. Irrespective of the graft size, the iliac wing does not show any significant stress peaks with the harvest site being 20 to 25 mm posterior to the ASIS. The harvest area itself inhibits the distribution of the forces applied on the ASIS to extend to the posterior iliac wing. -
Is There an Optimal Placement for the Supra-Acetabular Pin?
Orthopedic Technologies & Techniques Anterior Pelvic External Fixation: Is There an Optimal Placement for the Supra-Acetabular Pin? Leo A. Calafi, MD, and ML Chip Routt, MD the anterior inferior iliac spine (AIIS) and contained within Abstract the pelvic brim bone.7,8 Anterior pelvic external fixation using supra- Although the technique for supra-acetabular external acetabular bone pins is frequently used for fixation has been previously described,9-15 important details manipulation and reduction of unstable pelvic regarding optimal pin placement are lacking. The optimal su- ring injuries prior to definitive fixation. The pra-acetabular pins should provide maximal frame stability, supra-acetabular bone pin must be strategi- patient comfort, hip mobility, and avoid obstructing poten- cally placed in order to provide optimal frame tial internal fixation osseous pathways. This is an important stability, patient comfort, and hip mobility, consideration, since external fixation is often a temporary without obstructing subsequent osseous fixa- resuscitative measure prior to subsequent definitive fixation tion pathways. We describe a technique for al- of anterior and posterior pelvic ring injuries. ternative placement of supra-acetabular bone We describe a simplistic and alternative fluoroscopically pins. The intraoperative imaging is detailed. guided technique for supra-acetabular bone pins insertion The bone pin starting point is located more that does not obstruct other local pelvic osseous fixation cranially at the anterior inferior iliac spineAJO than pathways. previously described and the pin is directed to accommodate better hip motion. Surgical Technique The patient is placed supine on a radiolucent operating table. The entire abdomen and bilateral flanks are prepared with iodine solution and isopropyl alcohol, and then draped. -
Standardized Patient Exercise 3 IPM 1 2000
Introduction to the Practice of Medicine 1 ABDOMEN EXAM DETAILS FROM ABDOMEN VIDEO Preliminaries to the abdominal exam: S Patient should be supine for the abdomen exam. S Pull out the ledge for the patient’s legs. S Make sure the patient is appropriately draped. Let the patient lift up his/her gown to expose the abdomen. Drape the sheet across the pelvis. S Patient’s arms should be at his/her sides, NOT above his/her head. S Examiner should be on patient’s right side. This is the classic position for the abdomen exam. S Make sure the exam room door is closed. S Exam should be done on skin and not over the gown or an article of clothing. S Always inform the patient of what you are going to do before you do it. WASH HANDS 1. Identify and locate the costal margin The costal margin is made of the cartilaginous border of ribs: 7 – 10 anteriorly. 2. Identify and locate the xiphoid process The xiphoid process is a midline finger-like projection from the most inferior part of the body of the sternum. 3. Identify and locate the midline which is overlying the linea alba Linea alba runs from the xiphoid process inferiorly to the symphysis pubis. 4. Identify and locate the rectus abdominis muscle Student may ask patient to raise their head and shoulders from the supine position. These muscles run about 7-10 cm lateral to and parallel to the linea alba. The lateral border of the rectus abdominis muscle is known as the linea semilunaris. -

Handy Tips for Finding Key Bony Landmarks
Spinal Seating Professional Development Project Assessment Form RD4.1: Initial Interview Handy tips for finding key bony landmarks Pelvis: Greater trochanter Photo used with permission from Smith & Nephew Find these on yourself or practice these with a colleague. Anterior superior iliac spine (ASIS) Put your hand on the hips locate the Iliac Crest / hip bone palpate frontward ASIS is a sharp notch:, above the femur/ thigh bone when seated. Posterior superior iliac spine (PSIS) The “dimples’ between the buttocks and waist Put your hand on the hips Locate the Iliac Crest / hip bone and palpate backward PSIS is less pronounced but has no muscle over it Ischial tuberosity (IT) The IT is located only about 5cm from midline, slip you hand right under your buttock and towards the midline Sit on your hand with palm up to feel the IT against your fingers tips. When you assess others, wear a slippery glove / plastic bag to reduce friction as you slide you hand under the buttock. If you squad down to level your shoulder with the cushion, you will gain more leverage to get your hand under. If the client is sitting with posterior pelvic tilt (slouching), the ITs will be moved forward, away from backrest. If the client is sitting with anterior pelvic tilt (arching the back), the ITs will be pointing backwards toward the backrest. Greater trochanter (GT) Using the ball of your palm, rub along the lateral aspect of the thigh, back and forth between mid-thigh and pelvis to find a bony notch. Produced by NSW State Spinal Cord Injury Service, Spinal Seating Professional Development Program Developed by Turnbull, Charisse in 2008.