Ischio-Pubic Osteochondritis (Van Neck- Odelberg Disease): a Case Report
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Advances in the Pathogenesis and Possible Treatments for Multiple Hereditary Exostoses from the 2016 International MHE Conference
Connective Tissue Research ISSN: 0300-8207 (Print) 1607-8438 (Online) Journal homepage: https://www.tandfonline.com/loi/icts20 Advances in the pathogenesis and possible treatments for multiple hereditary exostoses from the 2016 international MHE conference Anne Q. Phan, Maurizio Pacifici & Jeffrey D. Esko To cite this article: Anne Q. Phan, Maurizio Pacifici & Jeffrey D. Esko (2018) Advances in the pathogenesis and possible treatments for multiple hereditary exostoses from the 2016 international MHE conference, Connective Tissue Research, 59:1, 85-98, DOI: 10.1080/03008207.2017.1394295 To link to this article: https://doi.org/10.1080/03008207.2017.1394295 Published online: 03 Nov 2017. Submit your article to this journal Article views: 323 View related articles View Crossmark data Citing articles: 1 View citing articles Full Terms & Conditions of access and use can be found at https://www.tandfonline.com/action/journalInformation?journalCode=icts20 CONNECTIVE TISSUE RESEARCH 2018, VOL. 59, NO. 1, 85–98 https://doi.org/10.1080/03008207.2017.1394295 PROCEEDINGS Advances in the pathogenesis and possible treatments for multiple hereditary exostoses from the 2016 international MHE conference Anne Q. Phana, Maurizio Pacificib, and Jeffrey D. Eskoa aDepartment of Cellular and Molecular Medicine, Glycobiology Research and Training Center, University of California, San Diego, La Jolla, CA, USA; bTranslational Research Program in Pediatric Orthopaedics, Division of Orthopaedic Surgery, The Children’s Hospital of Philadelphia, Philadelphia, PA, USA ABSTRACT KEYWORDS Multiple hereditary exostoses (MHE) is an autosomal dominant disorder that affects about 1 in 50,000 Multiple hereditary children worldwide. MHE, also known as hereditary multiple exostoses (HME) or multiple osteochon- exostoses; multiple dromas (MO), is characterized by cartilage-capped outgrowths called osteochondromas that develop osteochondromas; EXT1; adjacent to the growth plates of skeletal elements in young patients. -

Post-Traumatic Osteolysis of the Clavicle: a Case Report C
Arch Emerg Med: first published as 10.1136/emj.3.2.129 on 1 June 1986. Downloaded from Archives of Emergency Medicine, 1986, 3, 129-132 Post-traumatic osteolysis of the clavicle: a case report C. J. GRIFFITHS AND E. GLUCKSMAN Department ofAccident and Emergency Medicine, King's College Hospital, Denmark Hill, London, England SUMMARY A case of post-traumatic osteolysis of the clavicle occurring in a 25-year-old male is described. The condition should be suspected in anyone giving a history of persistent shoulder pain following trauma or intensive sporting activities. Characteristic resorp- tion of the distal tip of the clavicle is found on X-ray. The condition usually responds by copyright. within 2 years to conservative treatment. Previous reports ofthe condition are reviewed, and the possible pathogenesis and differential diagnosis discussed. INTRODUCTION Post-traumatic osteolysis of the clavicle is an uncommon condition characterized by http://emj.bmj.com/ persistent shoulder pain associated with decalcification of the distal tip of the clavicle following trauma to the acromio-clavicular joint (Madsen, 1963; Smart, 1972; Quinn & Glass, 1983). Patients usually give a history of previous trauma to the shoulder, but the condition may follow active sports such as weight training (Cahill, 1982) or the use of pneumatic tools (Ehricht, 1959). The condition usually resolves within 2 years in the absence of further trauma. This article describes a case of post-traumatic osteolysis of on September 28, 2021 by guest. Protected the clavicle, and discusses the diagnosis and possible pathogenesis of the condition. CASE REPORT A 25-year-old medical student (C.G.) was involved in a bicycle accident and received a direct blow to his right shoulder. -

Joints Classification of Joints
Joints Classification of Joints . Functional classification (Focuses on amount of movement) . Synarthroses (immovable joints) . Amphiarthroses (slightly movable joints) . Diarthroses (freely movable joints) . Structural classification (Based on the material binding them and presence or absence of a joint cavity) . Fibrous mostly synarthroses . Cartilagenous mostly amphiarthroses . Synovial diarthroses Table of Joint Types Functional across Synarthroses Amphiarthroses Diarthroses (immovable joints) (some movement) (freely movable) Structural down Bony Fusion Synostosis (frontal=metopic suture; epiphyseal lines) Fibrous Suture (skull only) Syndesmoses Syndesmoses -fibrous tissue is -ligaments only -ligament longer continuous with between bones; here, (example: radioulnar periosteum short so some but not interosseous a lot of movement membrane) (example: tib-fib Gomphoses (teeth) ligament) -ligament is periodontal ligament Cartilagenous Synchondroses Sympheses (bone united by -hyaline cartilage -fibrocartilage cartilage only) (examples: (examples: between manubrium-C1, discs, pubic epiphyseal plates) symphesis Synovial Are all diarthrotic Fibrous joints . Bones connected by fibrous tissue: dense regular connective tissue . No joint cavity . Slightly immovable or not at all . Types . Sutures . Syndesmoses . Gomphoses Sutures . Only between bones of skull . Fibrous tissue continuous with periosteum . Ossify and fuse in middle age: now technically called “synostoses”= bony junctions Syndesmoses . In Greek: “ligament” . Bones connected by ligaments only . Amount of movement depends on length of the fibers: longer than in sutures Gomphoses . Is a “peg-in-socket” . Only example is tooth with its socket . Ligament is a short periodontal ligament Cartilagenous joints . Articulating bones united by cartilage . Lack a joint cavity . Not highly movable . Two types . Synchondroses (singular: synchondrosis) . Sympheses (singular: symphesis) Synchondroses . Literally: “junction of cartilage” . Hyaline cartilage unites the bones . Immovable (synarthroses) . -

Management of the 'Young' Patient with Hip Disease
ARTHROPLASTY OF THE LOWER EXTREMITIES Management of the ‘Young’ Patient with Hip Disease SCOTT A. RITTERMAN, MD; LEE E. RUBIN, MD ABSTRACT abnormalities lead to impingement within the joint, altered Although hip arthritis typically affects older patients, biomechanics and ultimately cartilage loss.2 Secondary there is a rapidly growing population of “young” patients osteoarthritis can be due to an identifiable cause such as experiencing debilitating symptoms from hip disease. trauma to the femoral head, post-infection arthritis, slipped Most commonly, osteoarthritis and avascular necrosis af- capital femoral epiphysis, or hip dysplasia. fect this population, but a variety of other primary struc- As we age, the water content of cartilage increases with tural and metabolic causes can also occur. The expecta- a concomitant decrease in protein content, both leading to tions of these younger patients are often distinct from degeneration. The progressive loss of the cartilage matrix geriatric patients, and the challenges in optimizing their leads to recurrent bouts of inflammation as bone contacts care are unique in this demanding population. Selection bone, and reactive bone called osteophyte forms around the of the implant, bearing surface, and surgical technique joint. In the subchondral bone, hardening and cyst formation can all impact the success and longevity of total hip re- occurs. Repeated bouts of inflammation also extend into the placement. A consideration for respecting the native peri-articular soft tissues leading to deformity and contrac- bone stock is an important consideration that can poten- tures of the capsule, supporting ligaments, and tendons. Put tially reduce some of the future challenges of revision ar- together, these changes lead to pain, stiffness, and gait dis- throplasty in this young population. -

Pathological Fracture of the Tibia As a First Sign Of
ANTICANCER RESEARCH 41 : 3083-3089 (2021) doi:10.21873/anticanres.15092 Pathological Fracture of the Tibia as a First Sign of Hyperparathyroidism – A Case Report and Systematic Review of the Current Literature ALEXANDER KEILER 1, DIETMAR DAMMERER 1, MICHAEL LIEBENSTEINER 1, KATJA SCHMITZ 2, PETER KAISER 1 and ALEXANDER WURM 1 1Department of Orthopaedics and Traumatology, Medical University of Innsbruck, Innsbruck, Austria; 2Institute for Pathology, INNPATH GmbH, Innsbruck, Austria Abstract. Background/Aim: Pathological fractures are rare, of the distal clavicles, a “salt and pepper” appearance of the suspicious and in some cases mentioned as the first sign of a skull, bone cysts, and brown tumors of the bones (3). malignant tumor. We present an uncommon case with a Primary hyperparathyroidism (PHPT), also known as “brown pathological fracture of the tibia diaphysis as the first sign of tumor”, also involves unifocal or multifocal bone lesions, which severe hyperparathyroidism. Case Report: We report the case represent a terminal stage of hyperparathyroidism-dependent of a female patient who was referred to the emergency bone pathology (4). This focal lesion is not a real neoplasm. In department with a history of progressively worsening pain in localized regions where bone loss is particularly rapid, the lower left leg and an inability to fully bear weight. No hemorrhage, reparative granulation tissue, and active, vascular, history of trauma or any other injury was reported. An x-ray proliferating fibrous tissue may replace the healthy marrow revealed an extensive osteolytic lesion in the tibial shaft with contents, resulting in a brown tumor. cortical bone destruction. Conclusion: Our case, together with Histologically, the tumor shows bland spindle cell very few cases described in the current literature, emphasizes proliferation with multinucleated osteoclastic giant cells and that in the presence of hypercalcemia and lytic lesions primary signs of bone resorption. -

Yagenich L.V., Kirillova I.I., Siritsa Ye.A. Latin and Main Principals Of
Yagenich L.V., Kirillova I.I., Siritsa Ye.A. Latin and main principals of anatomical, pharmaceutical and clinical terminology (Student's book) Simferopol, 2017 Contents No. Topics Page 1. UNIT I. Latin language history. Phonetics. Alphabet. Vowels and consonants classification. Diphthongs. Digraphs. Letter combinations. 4-13 Syllable shortness and longitude. Stress rules. 2. UNIT II. Grammatical noun categories, declension characteristics, noun 14-25 dictionary forms, determination of the noun stems, nominative and genitive cases and their significance in terms formation. I-st noun declension. 3. UNIT III. Adjectives and its grammatical categories. Classes of adjectives. Adjective entries in dictionaries. Adjectives of the I-st group. Gender 26-36 endings, stem-determining. 4. UNIT IV. Adjectives of the 2-nd group. Morphological characteristics of two- and multi-word anatomical terms. Syntax of two- and multi-word 37-49 anatomical terms. Nouns of the 2nd declension 5. UNIT V. General characteristic of the nouns of the 3rd declension. Parisyllabic and imparisyllabic nouns. Types of stems of the nouns of the 50-58 3rd declension and their peculiarities. 3rd declension nouns in combination with agreed and non-agreed attributes 6. UNIT VI. Peculiarities of 3rd declension nouns of masculine, feminine and neuter genders. Muscle names referring to their functions. Exceptions to the 59-71 gender rule of 3rd declension nouns for all three genders 7. UNIT VII. 1st, 2nd and 3rd declension nouns in combination with II class adjectives. Present Participle and its declension. Anatomical terms 72-81 consisting of nouns and participles 8. UNIT VIII. Nouns of the 4th and 5th declensions and their combination with 82-89 adjectives 9. -

1. Synarthrosis - Immovable
jAnatomy Lecture Notes Chapter 9 I. classification A. by function - 1. synarthrosis - immovable 2. amphiarthrosis - slightly movable 3. diarthrosis - freely movable B. by structure - material attaching bones together 1. fibrous -.dense c.t., no joint cavity a. suture - very thin, short fibers synostosis - ossification of fibrous c.t. in a suture joint b. syndesmosis - ligament (the longer the fibers the more movement is possible) c. gomphosis - periodontal ligament holds teeth in alveoli 2. cartilaginous - cartilage, no joint cavity a. synchondrosis - hyaline cartilage b. symphysis - fibrocartilage 3. synovial - joint capsule and ligaments II. structure of a synovial joint A. bone and articular cartilage (hyaline) • articular cartilage cushions bone ends by absorbing compression stress Strong/Fall 2008 page 1 jAnatomy Lecture Notes Chapter 9 B. articular capsule 1. fibrous capsule - dense irregular c.t.; holds bones together 2. synovial membrane - areolar c.t. with some simple squamous e.; makes synovial fluid C. joint cavity and synovial fluid 1. synovial fluid consists of: • fluid that is filtered from capillaries in the synovial membrane • glycoprotein molecules that are made by fibroblasts in the synovial membrane 2. fluid lubricates surface of bones inside joint capsule D. ligaments - made of dense fibrous c.t.; strengthen joint • capsular • extracapsular • intracapsular E. articular disc / meniscus - made of fibrocartilage; improves fit between articulating bones F. bursae - membrane sac enclosing synovial fluid found around some joints; cushion ligaments, muscles, tendons, skin, bones G. tendon sheath - elongated bursa that wraps around a tendon Strong/Fall 2008 page 2 jAnatomy Lecture Notes Chapter 9 III. movements at joints flexion extension abduction adduction circumduction rotation inversion eversion protraction retraction supination pronation elevation depression opposition dorsiflexion plantar flexion gliding Strong/Fall 2008 page 3 jAnatomy Lecture Notes Chapter 9 IV. -

3-Joints.Pdf
“In order to succeed, we must first believe that we can”. - Nikos Kazantzakis. objectives: - Define the term “Joint”. - Describe the classification of the 3 types of joints & give an example of each. - Describe the characteristics of synovial joints. - Describe the classification of synovial joints & give an example of each. - List factors maintaining stability of joints. - Recite “Hilton’s law” for nerve supply of joints. Joints: What is a joint? Classification of joints: It is the site where two or more bones meet According to the tissues that lie between the bones, Joints are classified into: together. What we mean by "two or more" in the Fibrous Cartilaginous Synovial definition is that at some articulations, - The articulating - The Two bone are - The bones are joined two or more bones might be joined together like the knee joint, where the surfaces are joined joined by cartilage by a fibrous capsule. femur, tibia and patella articulate by fibrous tissue together by a synovial joint. - The articular surfaces are covered by a thin layer of hyaline cartilage 1-Fibrous Joints: - The articulating surfaces are joined by : fibrous tissue - Movement: No or very mild movement - Examples: -inferior tibiofibular -Skull Sutures- joints (syndesmosis)- -Gomphosis- Temporary (ossify later) - Minimal movement dental alveolar joints. - Permanent joints. Between the teeth and there socket. 2-Cartilaginous Joints: - The two bones are joined by : Cartilage. The main difference between the primary and the secondary cartilaginous joints is that the primary is joined by a plate of hyaline cartilage, meanwhile the secondary is joined by a - TYPES: small amount of fibrous tissue forming a plate of fibrocartilage. -

1019 2 Feb 11 Weisbrode FINAL.Pages
The Armed Forces Institute of Pathology Department of Veterinary Pathology Wednesday Slide Conference 2010-2011 Conference 19 2 February 2011 Conference Moderator: Steven E. Weisbrode, DVM, PhD, Diplomate ACVP CASE I: 2173 (AFIP 2790938). Signalment: 3.5-month-old, male intact, Chow-Rottweiler cross, canine (Canis familiaris). History: This 3.5-month-old male Chow-Rottweiler mixed breed dog was presented to a veterinary clinic with severe neck pain. No cervical vertebral lesions were seen radiographically. The dog responded to symptomatic treatment. A week later the dog again presented with neck pain and sternal recumbency. The nose was swollen, and the submandibular and popliteal lymph nodes were moderately enlarged. The body temperature was normal. A complete blood count (CBC) revealed a marked lymphocytosis (23,800 lymphocytes/uI). Over a 3-4 hour period there was a noticeable increase in the size of all peripheral lymph nodes. Treatment included systemic antibiotics and corticosteroids. The dog became ataxic and developed partial paralysis. The neurologic signs waxed and waned over a period of 7 days, and the lymphadenopathy persisted. The peripheral blood lymphocyte count 5 days after the first CBC was done revealed a lymphocyte count of 6,000 lymphocytes/uI. The clinical signs became progressively worse, and the dog was euthanized two weeks after the initial presentation. Laboratory Results: Immunohistochemical (IHC) staining of bone marrow and lymph node sections revealed that tumor cells were negative for CD3 and CD79α. Gross Pathology: Marked generalized lymph node enlargement was found. Cut surfaces of the nodes bulged out and had a white homogeneous appearance. The spleen was enlarged and meaty. -

Diagnosis and Treatment of Osteochondral Defects of the Ankle
SAOJ Winter 2009.qxd:Orthopaedics Vol3 No4 5/10/09 2:40 PM Page 44 Page 44 / SA ORTHOPAEDIC JOURNAL Winter 2009 CLINICAL ARTICLE C LINICAL A RTICLE Diagnosis and treatment of osteochondral defects of the ankle ML Reilingh, MD CJA van Bergen, MD CN van Dijk, MD, PhD Department of Orthopaedic Surgery, Academic Medical Centre, University of Amsterdam, Amsterdam, The Netherlands Corresponding address: Academic Medical Centre University of Amsterdam Department of Orthopaedic Surgery Prof Dr C Niek van Dijk PO Box 22660 1100 DD Amsterdam, The Netherlands Tel: + 31 20 566-2938 Fax: +31 20 566-9117 Email: [email protected], [email protected] Abstract An osteochondral defect of the talus is a lesion involving talar articular cartilage and subchondral bone. It is fre- quently caused by a traumatic event. The lesions may either heal, stabilise or progress to subchondral bone cysts. The subchondral cysts may develop due to the forcing of cartilaginous or synovial fluid with every step. Malalignment of the hindfoot plays an important role in the development of further degeneration. Plain radio- graphs may disclose the lesion. Modern imaging technology has enhanced the ability to fully evaluate and accu- rately determine the size and extent of the lesion, which are fundamental for proper treatment. Asymptomatic or low-symptomatic lesions are treated nonoperatively. For surgical treatment the following types of surgery are in clinical use: debridement and bone marrow stimulation, retrograde drilling, internal fixation, cancellous bone grafting, osteochondral autograft transfer, autologous chondrocyte implantation, and allograft transplantation. Although these are often successful, malalignment may persist with these treatment options. -
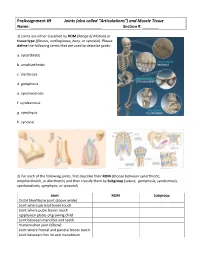
Preassignment #9 Joints (Also Called “Articulations”) and Muscle Tissue Name: Section #: __
PreAssignment #9 Joints (also called “Articulations”) and Muscle Tissue Name: _______________________________ Section #: _______ 1) Joints are either classified by ROM (Range of Motion) or tissue type (fibrous, cartilaginous, bony, or synovial). Please define the following terms that are used to describe joints: a. synarthrotic b. amphiarthrotic c. diarthrotic d. gomphosis e. synchondrosis f. syndesmosis g. symphysis h. synovial 2) For each of the following joints, first describe their ROM (choose between synarthrotic, amphiarthrotic, or diarthrotic) and then classify them by Subgroup (suture, gomphosis, syndesmosis, synchondrosis, symphysis, or synovial). Joint ROM Subgroup Distal tibiofibular joint (above ankle) Joint where parietal bones touch Joint where pubic bones touch Epiphyseal plates of growing child Joint between mandible and teeth Humeroulnar joint (elbow) Joint where frontal and parietal bones touch Joint between first rib and manubrium 3) Please label the parts of the generic synovial joint below. Use the terms: synovial membrane, ligament, periosteum, articular cartilage, synovial fluid, fibrous capsule, and joint capsule. Now, to see if you really understand joints, can you add labels for the diaphyseal cavity and epiphyseal line? 4) Synovial joints (or diarthroses) are usually classified as plane, hinge, saddle, ball-and-socket, or pivot joints. Note: I don’t list condyloid as a subgroup since it is really just a modified form of the hinges! For each of the following joints, please identify the classification to which they belong: a. humeroradial b. scapulohumeral c. interphalangeal d. atloaxis e. carpometacarpal #1 f. intercarpals g. proximal radioulnar h. sacroiliac 5) Movements at a joint are referred to as actions. For each of the following statements, tell me the proper action that is being used: a. -

Pathophysiology of Chronic Bacterial Osteomyelitis. Why Do Antibiotics Fail
Postgrad Med J 2000;76:479–483 479 Pathophysiology of chronic bacterial osteomyelitis. Postgrad Med J: first published as 10.1136/pmj.76.898.479 on 1 August 2000. Downloaded from Why do antibiotics fail so often? J Ciampolini, K G Harding Abstract sinuses overlying a focus of chronic osteomyeli- In this review the pathophysiology of tis. Mackowiack in 1978 demonstrated the low chronic bacterial osteomyelitis is summa- positive predictive value of sinus tract swabs; in rised, focusing on how bacteria succeed so a retrospective analysis of 40 patients, only often in overcoming both host defence 44% of the soft tissue swabs contained the mechanisms and antibiotic agents. Bacte- same pathogen as that obtained from a bone ria adhere to bone matrix and orthopae- sample at the time of operation. However, iso- dic implants via receptors to fibronectin lation of Staphylococcus aureus from the sinus and to other structural proteins. They tract swab had a higher positive predictive subsequently elude host defences and value than for other bacteria (78%). The same antibiotics by “hiding” intracellularly, by study found 60% of chronic osteomyelitis to be developing a slimy coat, or by acquiring a due to S aureus, followed by enterobacteriaceae very slow metabolic rate. The presence of (23%), pseudomonas (9%) and streptococcus an orthopaedic implant also causes a local (9%).3 Similar results with regards to the inac- polymorphonuclear cell defect, with de- curacy of wound swabs were obtained in creased ability to kill phagocytosed bacte- prospective studies on diabetic foot infection4 ria. Osteolysis is determined locally by the and on post-traumatic chronic osteomyelitis.5 interaction of bacterial surface compo- The latter study also demonstrated the poor nents with immune system cells and positive predictive value of Craig needle biopsy subsequent cytokine production.