Age–Related Macular Degeneration
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vision Rehabi I Itation for Patients with Age Related Macular Degeneration
Vision rehabi I itation for GARY S. RUBIN patients with age related macular degeneration Epidemiology of low vision The over-representation of macular degeneration patients in the low-vision clinic is The epidemiology of vision impairment is dealt reflected in the chief complaints of those with in detail elsewhere.1 However, there is one referred for rehabilitation. A study of 1000 particularly salient factor that bears emphasis. consecutive patients seen at the Wilmer Low The prevalence of vision impairment increases Vision clinic indicated that 64% listed 'reading' dramatically with advancing age. Statistics as their chief complaint, while other activities compiled in the UK by the Royal National were identified by fewer than 8% of patients. Institute for the Blind2 indicate that there were Undoubtedly the bias towards reading approximately 1.1 million blind or partially problems results partly from the nature of the sighted persons in 1996, of whom 82% were 65 low-vision services offered. Those served by a years of age or older. Thus it is not surprising to community-based programme that includes learn that the major causes of vision impairment home visits might be more likely to report are age-related eye diseases. Fig. 1 illustrates the problems with activities of daily living, while a distribution of causes of vision impairment blind rehabilitation centre would be more likely 5 from three recent studies?- Approximately to address mobility issues. Nevertheless, most equal percentages are attributed to macular macular degeneration patients are referred to degeneration and cataract, with smaller hospital or optometry clinic services, and as percentages for glaucoma, diabetic retinopathy their overwhelming concern is with reading, and optic neuropathies. -

Symptoms of Age Related Macular Degeneration
WHAT IS MACULAR DEGENERATION? wavy or crooked, visual distortions, doorway and the choroid are interrupted causing waste or street signs seem bowed, or objects may deposits to form. Lacking proper nutrients, the light- Age related macular degeneration (AMD) is appear smaller or farther away than they sensitive cells of the macula become damaged. a disease that may either suddenly or gradually should, decrease in or loss of central vision, and The damaged cells can no longer send normal destroy the macula’s ability to maintain sharp, a central blurry spot. signals from the macula through the optic nerve to central vision. Interestingly, one’s peripheral or DRY: Progression with dry AMD is typically slower your brain, and consequently your vision becomes side vision remains unaffected. AMD is the leading de-gradation of central vision: need for increasingly blurred cause of “legal blindness” in the United States for bright illumination for reading or near work, diffi culty In either form of AMD, your vision may remain fi ne persons over 65 years of age. AMD is present in adapting to low levels of illumination, worsening blur in one eye up to several years even while the other approximately 10 percent of the population over of printed words, decreased intensity or brightness of eye’s vision has degraded. Most patients don’t the age of 52 and in up to 33 percent of individuals colors, diffi culty recognizing faces, gradual increase realize that one eye’s vision has been severely older than 75. The macula allows alone gives us the in the haziness of overall vision, and a profound drop reduced because your brain compensates the bad ability to have: sharp vision, clear vision, color vision, in your central vision acuity. -

Macular Degeneration
DRIVEWELL Driving When You Have Macular Degeneration You have been a safe driver for years. For you, driving means freedom and control. As you get older, changes in your physical and mental health can affect how safely you drive. Macular degeneration (also known as age-related macular degeneration) damages the macula, a spot near the center of the retina (light-sensitive inner lining of the eyeball). It is a common eye problem among older drivers that makes it hard to drive safely. Age-related macular degeneration is the leading cause of new cases of blindness in people 65 and older. If you have macular degeneration, you may not notice any signs in the early stages. You may not know you have this condition until you lose your peripheral vision (what you see out of the corner of your eyes). In time it will affect your central vision, causing a dark or empty area in the center of your vision. How Can Macular Degeneration Affect the Way I Drive? • Your central vision may be dull and blurry. This can lead to loss of sharp vision. • You may not see the road, street signs, lane markers, and even people and bicyclists in the road. • You may need more bright light to see up close. • Colors may look less vivid or bright. • You may have trouble when you go from bright light to low light. • You may not be able to recognize people’s faces. What Should I Do if I Have Any of These Signs? As soon as you notice any of these warning signs: • Tell your family or someone close to you, especially if you have a family history of macular degeneration or have changes in your central vision. -

Detached and Torn Retina Retinal Detachments Occur in 1 out of 10,000 Americans Each Year
Detached and Torn Retina Retinal Detachments Occur in 1 Out of 10,000 Americans Each Year A retinal detachment is not as common as other eye conditions such as glaucoma or macular degeneration, however… it is just as serious and it is a vision threatening condition which should be treated as an emergency. Dr. Randy Katz, Florida Eye’s Diabetic Retinopathy, Retinal Detachment & Macular Degeneration Specialist says that the sooner a retinal tear or detachment is treated the better the chances of saving the vision in the eye. What Is a Retinal Detachment? The retina is the light-sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position. When this occurs, if not promptly treated, retinal detachment can cause permanent vision loss. In some cases there may be small areas of the retina that are torn. These areas, called retinal tears or retinal breaks, can lead to a retinal detachment. Vitreous gel, the clear material that fills the eyeball, is attached to the retina in the back of the eye. As we get older, the vitreous may change shape, pulling away from the retina. If the vitreous pulls a piece of the retina with it, it causes a retinal tear. Once a retinal tear occurs, vitreous fluid may seep through and lift the retina off the back wall of the eye, causing the retina to detach or pull away. 2 Are You At Risk for a Torn or Detached Retina? A retinal detachment can occur at any age, but it is more common in people over age 40. -

The Eye Is a Natural Optical Tool
KEY CONCEPT The eye is a natural optical tool. BEFORE, you learned NOW, you will learn •Mirrors and lenses focus light • How the eye depends on to form images natural lenses •Mirrors and lenses can alter • How artificial lenses can be images in useful ways used to correct vision problems VOCABULARY EXPLORE Focusing Vision cornea p. 607 How does the eye focus an image? pupil p. 607 retina p. 607 PROCEDURE 1 Position yourself so you can see an object about 6 meters (20 feet) away. 2 Close one eye, hold up your index finger, and bring it as close to your open eye as you can while keeping the finger clearly in focus. 3 Keeping your finger in place, look just to the side at the more distant object and focus your eye on it. 4 Without looking away from the more distant object, observe your finger. WHAT DO YOU THINK? • How does the nearby object look when you are focusing on something distant? • What might be happening in your eye to cause this change in the nearby object? The eye gathers and focuses light. The eyes of human beings and many other animals are natural optical tools that process visible light. Eyes transmit light, refract light, and respond to different wavelengths of light. Eyes contain natural lenses that focus images of objects. Eyes convert the energy of light waves into signals that can be sent to the brain. The brain interprets these signals as shape, brightness, and color. Altogether, these processes make vision possible. In this section, you will learn how the eye works. -
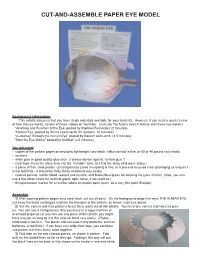
Cut-And-Assemble Paper Eye Model
CUT-AND-ASSEMBLE PAPER EYE MODEL Background information: This activity assumes that you have study materials available for your students. However, if you need a quick review of how the eye works, try one of these videos on YouTube. (Just use YouTube’s search feature with these key words.) “Anatomy and Function of the Eye: posted by Raphael Fernandez (2 minutes) “Human Eye” posted by Smart Learning for All (cartoon, 10 minutes) “A Journey Through the Human Eye” posted by Bausch and Lomb (2.5 minutes) “How the Eye Works” posted by AniMed (2.5 minutes) You will need: • copies of the pattern pages printed onto lightweight card stock (vellum bristol is fine, or 65 or 90 pound card stock) • scissors • white glue or good quality glue stick (I always advise against “school glue.”) • clear tape (I use the shiny kind, not the “invisible” kind, as I find the shiny kind more sticky.) • a piece of thin, clear plastic (a transparency [used in copiers] is fine, or a piece of recycled clear packaging as long as it is not too thick-- it should be fairly flimsy and bend very easily) • colored pencils: red for blood vessels and muscle, and brown/blue/green for coloring iris (your choice) (Also, you can use a few other colors for lacrimal gland, optic nerve, if you want to.) • thin permanent marker for a number labels on plastic parts (such as a very thin point Sharpie) Assembly: 1) After copying pattern pages onto card stock, cut out all parts. On the background page that says THE HUMAN EYE, cut away the black rectangles and trim the triangles at the bottom, as shown in picture above. -

Scleral Lenses and Eye Health
Scleral Lenses and Eye Health Anatomy and Function of the Human Eye How Scleral Lenses Interact with the Ocular Surface Just as the skin protects the human body, the ocular surface protects the human Scleral lenses are large-diameter lenses designed to vault the cornea and rest on the conjunctival tissue sitting on eye. The ocular surface is made up of the cornea, the conjunctiva, the tear film, top of the sclera. The space between the back surface of the lens and the cornea acts as a fluid reservoir. Scleral and the glands that produce tears, oils, and mucus in the tear film. lenses can range in size from 13mm to 19mm, although larger diameter lenses may be designed for patients with more severe eye conditions. Due to their size, scleral lenses consist SCLERA: The sclera is the white outer wall of the eye. It is SCLERAL LENS made of collagen fibers that are arranged for strength rather of at least two zones: than transmission of light. OPTIC ZONE The optic zone vaults over the cornea CORNEA: The cornea is the front center portion of the outer Cross section of FLUID RESERVOIR wall of the eye. It is made of collagen fibers that are arranged in the eye shows The haptic zone rests on the conjunctiva such a way so that the cornea is clear. The cornea bends light the cornea, overlying the sclera as it enters the eye so that the light is focused on the retina. conjunctiva, and sclera as CORNEA The cornea has a protective surface layer called the epithelium. -

Anatomy and Physiology of the Afferent Visual System
Handbook of Clinical Neurology, Vol. 102 (3rd series) Neuro-ophthalmology C. Kennard and R.J. Leigh, Editors # 2011 Elsevier B.V. All rights reserved Chapter 1 Anatomy and physiology of the afferent visual system SASHANK PRASAD 1* AND STEVEN L. GALETTA 2 1Division of Neuro-ophthalmology, Department of Neurology, Brigham and Womens Hospital, Harvard Medical School, Boston, MA, USA 2Neuro-ophthalmology Division, Department of Neurology, Hospital of the University of Pennsylvania, Philadelphia, PA, USA INTRODUCTION light without distortion (Maurice, 1970). The tear–air interface and cornea contribute more to the focusing Visual processing poses an enormous computational of light than the lens does; unlike the lens, however, the challenge for the brain, which has evolved highly focusing power of the cornea is fixed. The ciliary mus- organized and efficient neural systems to meet these cles dynamically adjust the shape of the lens in order demands. In primates, approximately 55% of the cortex to focus light optimally from varying distances upon is specialized for visual processing (compared to 3% for the retina (accommodation). The total amount of light auditory processing and 11% for somatosensory pro- reaching the retina is controlled by regulation of the cessing) (Felleman and Van Essen, 1991). Over the past pupil aperture. Ultimately, the visual image becomes several decades there has been an explosion in scientific projected upside-down and backwards on to the retina understanding of these complex pathways and net- (Fishman, 1973). works. Detailed knowledge of the anatomy of the visual The majority of the blood supply to structures of the system, in combination with skilled examination, allows eye arrives via the ophthalmic artery, which is the first precise localization of neuropathological processes. -

Refractive Error Is a Disease of the Eye, and We Should Treat It
Refractive error is a disease of the eye, and we should treat it. believe that refractive error is a disease of the eye— no different from glaucoma, dry eye disease, and other issues for which we readily offer treatment. In the world of modern cataract and refractive surgery, we have the capability to correct visual Iacuity that is compromised due to astigmatism and other types refractive error, so why shouldn't we treat astigmatism during cataract surgery? A large percentage of our cataract patients, about 75%, have at least 0.50 D of astigmatism. Even this small amount of astigmatism can and often does create issues visually for patients. The higher the My Philosophy of level of astigmatism, the more it can affect vision. My philosophy is, why not try to help these people? Correcting their astigmatism will help them to achieve better visual acuity, and this is even more crucial in patients who elect a multifocal, extended depth of focus, or other premium IOL. It is important to educate patients about their astigmatism and to relay to them what we can do ASTIGMATISM to correct it. The level of care and attention to detail affects everything, from our surgical outcomes, to the practice’s reputation, to future referral patterns. THRESHOLDS AND BEST PRACTICES My threshold for astigmatism treatment is about 0.75 D. Above that, the patient can lose contrast and can have functional visual acuity issues if the astig- MANAGEMENT matism is not addressed. I believe that correction of low astigmatism, especially, is low-hanging fruit, as it provides surgeons with an additional opportunity to improve their practices. -

Corneal Erosion?
What Is the Cornea? The cornea is the clear front window of the eye. It covers the iris (colored portion of the eye) and the round pupil, much like a watch crystal covers the face of a watch. The cornea is composed of five layers. The outermost surface layer is called the epithelium. Normal Eye Anatomy What Is a Corneal Abrasion? A corneal abrasion is an injury (a scratch, scrape or cut) to the corneal epithelium. Abrasions are commonly caused by fingernail scratches, paper cuts, makeup brushes, scrapes from tree or bush limbs, and rubbing of the eye. Some eye conditions, such as dry eye, increase the chance of an abrasion. You may experience the following symptoms with corneal abrasion: • Feeling of having something in your eye • Pain and soreness of the eye • Redness of the eye • Sensitivity to light • Tearing • Blurred vision To detect an abrasion on the cornea, your ophthalmologist (Eye M.D.) will use a special dye called fluorescein (pronounced FLOR-uh-seen) to illuminate the injury. How Is a Corneal Abrasion Treated? Treatment may include the following: • Patching the injured eye to prevent eyelid blinking from irritating the injury. • Applying lubricating eyedrops or ointment to the eye to form a soothing layer between the eyelid and the abrasion. • Using antibiotics to prevent infection. • Dilating (widening) the pupil to relieve pain. • Wearing a special contact lens to help healing. Minor abrasions usually heal within a day or two; larger abrasions usually take about a week. It is important not to rub the eye while it is healing. -

A Bright Vision for the Future
RetinaReview A newsletter from the Wilmer Eye Institute at Johns Hopkins SUMMER 2013 A Bright Vision for the Future here’s little doubt that improve patient outcomes in the Wilmer faculty. Our eight other diseases and disorders in years ahead. Fernando Arevalo assistant and associate retina pro- ophthalmology, specifi- serves as chief of the retina service fessors—unquestionably some of Tcally those that involve the for Wilmer’s collaboration with the the brightest stars in ophthalmol- retina, are some of the most vex- King Khaled Eye Specialist Hospital ogy—are bringing fresh insights and ing conditions in medicine today. in Riyadh, Saudi Arabia. From energy to today’s major challenges Retinal detachment, retinitis pig- 2006 to 2012, Neil Bressler led in retina research and patient care. mentosa, and retinal vein occlusion the National Institutes of Health- Read on to learn about how these are among retina conditions that sponsored Diabetic Retinopathy junior faculty members are working rob the vision of countless children Clinical Research Network, likely to harness telemedicine in the treat- and adults throughout the world. the largest collaborative clinical ment of retina diseases, attacking The good news? Thanks to ongo- research program in retina in the vision loss from retinal detachment ing advances by Wilmer’s retina world, and now serves as Past Chair. surgery or poor circulation to the specialists, dramatic strides are being retina, developing new imaging made. The most common causes of WILMER RETINA DIVISION and robotic approaches to retinal blindness, if left untreated, are reti- BY THE NUMBERS disease, and taking their renowned nal diseases, including age-related treatments and research to those macular degeneration and diabetic 7 Number of endowed throughout the region. -

Low Vision Devices for Age-Related Macular Degeneration: a Systematic Review
LOW VISION DEVICES FOR MACULAR DEGENERATION 1 Low Vision Devices for Age-Related Macular Degeneration: A Systematic Review Anne Macnamara, BPsy(Hons),1 Celia S. Chen, PhD,2 Andrew Davies, BASc,3 Charlotte Sloan,1 & Tobias Loetscher, PhD,1 1 Cognitive Ageing & Impairment Neurosciences Laboratory, UniSA Justice & Society, University of South Australia, Adelaide, SA, Australia 2 College of Medicine and Public Health, Flinders Medical Centre, Flinders University, Adelaide, SA, Australia 3 Royal Society for the Blind, Adelaide, SA, Australia Corresponding author. Anne Macnamara Email: [email protected] Postal address: Campus Central – Magill, University of South Australia, St Bernards Road, Magill SA 5072 LOW VISION DEVICES FOR MACULAR DEGENERATION 2 Abstract Significance: Age-related macular degeneration (AMD) is a degenerative condition impacting central vision. Evaluating the effectiveness of low vision devices provides empirical evidence on how devices can overcome deficits caused by AMD and facilitates discussion on future improvements to vision enhancement technology. Methods: A systematic review of the literature was conducted on the use of low vision devices in AMD populations. Relevant peer-reviewed research articles from six databases were screened. Results: The findings of thirty-five studies revealed a significant impact of low vision devices leading to improvements in visual acuity, reading performance, facial recognition, and more. While the studies were generally found to have a moderate risk of bias, a GRADE assessment of the evidence suggests that the general certainty of the evidence was low-moderate. Conclusions: A positive effect of low vision devices was found for visual acuity, reading performance, facial recognition, and more.