Tug Endotracheal Tube to Assess Tube Location; a Randomized Clinical Trial William P
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

HEENT EXAMINIATION ______HEENT Exam Exam Overview
HEENT EXAMINIATION ____________________________________________________________ HEENT Exam Exam Overview I. Head A. Visual inspection B. Palpation of scalp II. Eyes A. Visual Acuity B. Visual Fields C. Extraocular Movements/Near Response D. Inspection of sclera & conjunctiva E. Pupils F. Ophthalmoscopy III. Ears A. External Inspection B. Otoscopy C. Hearing Acuity D. Weber/Rinne IV. Nose A. External Inspection B. Speculum/otoscope C. Sinus areas V. Throat/Mouth A. Mouth Examination B. Pharynx Examination C. Bimanual Palpation VI. Neck A. Lymph nodes B. Thyroid gland 29 HEENT EXAMINIATION ____________________________________________________________ HEENT Terms Acuity – (ehk-yu-eh-tee) sharpness, clearness, and distinctness of perception or vision. Accommodation - adjustment, especially of the eye for seeing objects at various distances. Miosis – (mi-o-siss) constriction of the pupil of the eye, resulting from a normal response to an increase in light or caused by certain drugs or pathological conditions. Conjunctiva – (kon-junk-ti-veh) the mucous membrane lining the inner surfaces of the eyelids and anterior part of the sclera. Sclera – (sklehr-eh) the tough fibrous tunic forming the outer envelope of the eye and covering all of the eyeball except the cornea. Cornea – (kor-nee-eh) clear, bowl-shaped structure at the front of the eye. It is located in front of the colored part of the eye (iris). The cornea lets light into the eye and partially focuses it. Glaucoma – (glaw-ko-ma) any of a group of eye diseases characterized by abnormally high intraocular fluid pressure, damaged optic disk, hardening of the eyeball, and partial to complete loss of vision. Conductive hearing loss - a hearing impairment of the outer or middle ear, which is due to abnormalities or damage within the conductive pathways leading to the inner ear. -

Advanced Interpretation of Adult Vital Signs in Trauma William D
Advanced Interpretation of Adult Vital Signs in Trauma William D. Hampton, DO Emergency Physician 26 March 2015 Learning Objectives 1. Better understand vital signs for what they can tell you (and what they can’t) in the assessment of a trauma patient. 2. Appreciate best practices in obtaining accurate vital signs in trauma patients. 3. Learn what teaching about vital signs is evidence-based and what is not. 4. Explain the importance of vital signs to more accurately triage, diagnose, and confidently disposition our trauma patients. 5. Apply the monitoring (and manipulation of) vital signs to better resuscitate trauma patients. Disclosure Statement • Faculty/Presenters/Authors/Content Reviewers/Planners disclose no conflict of interest relative to this educational activity. Successful Completion • To successfully complete this course, participants must attend the entire event and complete/submit the evaluation at the end of the session. • Society of Trauma Nurses is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center's Commission on Accreditation. Vital Signs Vital Signs Philosophy: “View vital signs as compensatory to the illness/complaint as opposed to primary.” Crowe, Donald MD. “Vital Sign Rant.” EMRAP: Emergency Medicine Reviews and Perspectives. February, 2010. Vital Signs Truth over Accuracy: • Document the true status of the patient: sick or not? • Complete vital signs on every patient, every time, regardless of the chief complaint. • If vital signs seem misleading or inaccurate, repeat them! • Beware sending a patient home with abnormal vitals (especially tachycardia)! •Treat vital signs the same as any other diagnostics— review them carefully prior to disposition. The Mother’s Vital Sign: Temperature Case #1 - 76-y/o homeless ♂ CC: 76-y/o homeless ♂ brought to the ED by police for eval. -

Blood Pressure Year 1 Year 2 Core Clinical/Year 3+
Blood Pressure Year 1 Year 2 Core Clinical/Year 3+ Do Do • Patient at rest for 5 minutes • Measure postural BP and pulse in patients with a • Arm at heart level history suggestive of volume depletion or • Correct size cuff- bladder encircles 80% of arm syncope • Center of cuff aligns with brachial artery -Measure BP and pulse in supine position • Cuff wrapped snugly on bare arm with lower -Slowly have patient rise and stand (lie them down edge 2-3 cm above antecubital fossa promptly if symptoms of lightheadedness occur) • Palpate radial artery, inflate cuff to 70 mmHg, -Measure BP and pulse after 1 minute of standing then increase in 10 mmHg increments to 30 mmHg above point where radial pulse disappears. Know Deflate slowly until pulse returns; this is the • Normally when a person stands fluid shifts to approximate systolic pressure. lower extremities causing a compensatory rise in • Auscultate the Korotkoff sounds pulse by up to 10 bpm with BP dropping slightly -place bell lightly in antecubital fossa • Positive postural vital signs are defined as -inflate BP to 20-30mmHg above SBP as determined symptoms of lightheadedness and/or a drop in by palpation SBP of 20 mmHg with standing -deflate cuff at rate 2mmHg/second while auscultating • Know variations in BP cuff sizes -first faint tapping (Phase I Korotkoff) = SBP; • A lack of rise in pulse in a patient with an Disappearance of sound (Phase V Korotkoff)=DBP orthostatic drop in pressure is a clue that the Know cause is neurologic or related or related to -Korotkoff sounds are lower pitch, better heard by bell medications (eg. -

Patient Assessment: 3 Techniques of Physical Examination: 2
Patient Assessment: 3 Techniques of Physical Examination: 2 W4444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444444 UNIT TERMINAL OBJECTIVE 3-2 At the completion of this unit, the EMT-Critical Care Technician student will be able to explain the significance of physical exam findings commonly found in emergency situations. COGNITIVE OBJECTIVES At the completion of this unit, the EMT-Critical Care Technician student will be able to: 3-2.1 Define the terms inspection, palpation, percussion, auscultation. (C-1) 3-2.2 Describe the techniques of inspection, palpation, percussion, and auscultation. (C-1) 3-2-3 Review the procedure for taking and significance of vital signs (pulse, respiration, and blood pressure.) (C-2) 3-2.4 Describe the evaluation of mental status. (C-1) 3-2.5 Evaluate the importance of a general survey. (C-3) 3-2.6 Describe the examination of skin and nails. (C-1) 3-2.7 Differentiate normal and abnormal findings of the assessment of the skin. (C-3) 3-2.8 Distinguish the importance of abnormal findings of the assessment of the skin. (C-3) 3-2.9 Describe the normal and abnormal assessment findings of the head (including the scalp, skull, face and skin). (C-1) 3-2.10 Describe the examination of the head (including the scalp, skull, face, and skin). (C-1) 3-2.11 Describe the examination of the eyes. (C-1) 3-2.12 Distinguish between normal and abnormal assessment findings of the eyes. (C-3) 3-2.13 Describe the examination of the ears. (C-1) 3-2.14 Differentiate normal and abnormal assessment findings of the ears. -

Examination of the Knee
Examination of the Knee The Examination For every joint of the lower extremity always begin with the patient in standing IN STANDING INSPECTION 1. Cutaneous Structures: Look for Erythema, scarring, bruising, and swelling in the following areas: a. Peripatellar grooves b. Suprapatellar bursa c. Prepatellar bursa d. Infrapatellar tendon e. Anserine bursa f. Popliteal fossa 2. Muscle & Soft Tissue: a. Quadriceps atrophy b. Hamstring atrophy c. Calf atrophy 3. Bones & Alignment: a. Patella position (Alta, Baha, Winking, Frog eyed), b. Varus or Valgus alignment c. Flexion contracture or Genu recurvatum RANGE OF MOTION - ACTIVE Standing is the best opportunity to assess active range of motion of the knee. 1. Ask the patient to squat into a deep knee bend. Both knees should bend symmetrically. 2. Ask the patient to then stand and extend the knee fully – lock the knee. The knee should straighten to 0 degrees of extension. Some people have increased extension referred to as genu recurvatum. GAIT 1. Look for a short stance phase on the affected limb and an awkward gait if a concomitant leg length discrepancy 2. Look for turning on block 3. Screening 1. Walk on the toes 2. Walk on the heels 3. Squat down – Active Range of Motion testing SPECIAL TESTS 1. Leg Length Discrepancy a. Look at patients back for evidence of a functional scoliosis b. Place your hands on the patients Iliac crests looking for inequality which may mean a leg length discrepancy IN SITTING NEUROLOGIC EXAMINATION 1. Test the reflexes a. L4 – Quadriceps reflex VASCULAR EXAMINATION 1. Feel for the posterior tibial artery SUPINE POSITION INSPECTION 1. -

Abdominal Palpation/Auscultation of Fetal Heart Rate
Shared Maternity Care Program Guidelines Abdominal Palpation/Auscultation of Fetal Heart Rate Introduction Abdominal palpation and auscultation of the fetal heart rate is recommended as part of routine examination in pregnancy to assist in assessing fetal wellbeing. Requirements Sonicaid to identify the fetal heart rate. Aqueous gel Tape measure Recommendations for Abdominal Palpation Palpation is not performed during a contraction Only perform a GENTLE abdominal palpation for any woman with: History of ante partum hemorrhage Premature labour Severe (acute) abdominal pain Documentation of fundal height is advised from 24/40 A clinical estimate followed by a symphyso-fundal height using a tape measure should also be used A consistent approach to measurement increases accuracy Palpate the fundus first to identify the upper limit . Measure from the top of the fundus to the top of the pubic symphysis . The tape measure should stay in contact with the skin. It is not recommended to repeat the measurement. If the fundal height is more than 2cm below or above expected height, an obstetric opinion advised. Refer Antenatal Clinic 9784 2626 or if unavailable contact the obstetric registrar via switchboard 9784 7777 Fundal height measurement is of little value in a twin pregnancy. Recommendations for Intermittent Auscultation of fetal Heart Rate Is recommended from 20 weeks gestation It is important to identify maternal pulse before locating the fetal heart. Using intermittent auscultation the normal heart rate range is >110bpm and < 160bpm If fetal heart rate or fetal movements are not present after 24 weeks gestation immediately, contact the Women’s Health Unit on 9784 7959 SMCP GPLU 2018 Shared Maternity Care Program Guidelines Abdominal Palpation/Auscultation of Fetal Heart Rate Leopold’s manoeuvres:[1] a) Fundal palpation- to locate the upper pole of the fetus and note if cephalic or breech b) Lateral palpation- to locate the fetal back, anterior shoulder and limbs c) Pawlick’s grip- to assess the presentation and station. -

Physical Examination and Chronic Lower-Extremity Ischemia a Critical Review
ORIGINAL INVESTIGATION Physical Examination and Chronic Lower-Extremity Ischemia A Critical Review Steven R. McGee, MD; Edward J. Boyko, MD, MPH Objective: To determine the clinical utility of physical cians diagnose the presence of peripheral arterial dis- examination in patients with suspected chronic ische- ease: abnormal pedal pulses, a unilaterally cool extrem- mia of the lower extremities. ity, a prolonged venous filling time, and a femoral bruit. Other physical signs help determine the extent and dis- Data Sources: MEDLINE search (January 1966 to tribution of vascular disease, including an abnormal fem- January 1997), personal files, and bibliographies of oral pulse, lower-extremity bruits, warm knees, and the textbooks on physical diagnosis, surgery, and vascular Buerger test. The capillary refill test and the findings of surgery. foot discoloration, atrophic skin, and hairless extremi- ties are unhelpful in diagnostic decisions. Mathematical Study Selection: Both authors independently graded formulas, derived from 2 studies using multivariate analy- the studies as level 1, 2, or 3, according to predeter- sis, allow clinicians to estimate the probability of periph- mined criteria. Criteria deemed essential for analysis of eral arterial disease in their patients. sensitivity, specificity, and likelihood ratios were (1) clear definition of study population, (2) clear definition of Conclusion: Certain aspects of the physical examination physical examination maneuver, and (3) use of an ac- help clinicians make accurate judgments about -

History & Physical Format
History & Physical Format SUBJECTIVE (History) Identification name, address, tel.#, DOB, informant, referring provider CC (chief complaint) list of symptoms & duration. reason for seeking care HPI (history of present illness) - PQRST Provocative/palliative - precipitating/relieving Quality/quantity - character Region - location/radiation Severity - constant/intermittent Timing - onset/frequency/duration PMH (past medical /surgical history) general health, weight loss, hepatitis, rheumatic fever, mono, flu, arthritis, Ca, gout, asthma/COPD, pneumonia, thyroid dx, blood dyscrasias, ASCVD, HTN, UTIs, DM, seizures, operations, injuries, PUD/GERD, hospitalizations, psych hx Allergies Meds (Rx & OTC) SH (social history) birthplace, residence, education, occupation, marital status, ETOH, smoking, drugs, etc., sexual activity - MEN, WOMEN or BOTH CAGE Review Ever Feel Need to CUT DOWN Ever Felt ANNOYED by criticism of drinking Ever Had GUILTY Feelings Ever Taken Morning EYE OPENER FH (family history) age & cause of death of relatives' family diseases (CAD, CA, DM, psych) SUBJECTIVE (Review of Systems) skin, hair, nails - lesions, rashes, pruritis, changes in moles; change in distribution; lymph nodes - enlargement, pain bones , joints muscles - fractures, pain, stiffness, weakness, atrophy blood - anemia, bruising head - H/A, trauma, vertigo, syncope, seizures, memory eyes- visual loss, diplopia, trauma, inflammation glasses ears - deafness, tinnitis, discharge, pain nose - discharge, obstruction, epistaxis mouth - sores, gingival bleeding, teeth, -

OPQRST-AAA One Tool That Some Clinicians Find Helpful Is Using the Mnemonic OPQRST-AAA to Elicit the Details of a Pain Complaint
#1 Take a history related to diarrhea Diarrhea is subjective and can be defined as an increase in the volume, frequency or fluidity of stool relative to normal conditions. First introduce yourself to the patient and start: Personal and Social History: name, age, gender, occupation – Use as your own (Single, living with parents. No tobacco use). Present complaint: “ What brought you here”? 1-When these complaints started? It started early in the morning. 2-How many times do you go to the toilet today? 6 times. 3-How many times did you use to go to the toilet before this problem? Once daily. 4-Can you describe your stool: a. Is it watery, or bulky? Yes, watery. b.What color? Light yellow. c. Is there any blood or mucous in stool? No. d.Does it have foul smell? A little bit. 5-Do you have any additional symptoms - any nausea or vomiting? I vomited twice. 6-Do you have fever? No 7- Is there any pain on passing stools? No, but I have abdominal discomfort. 8-Can you describe what do you mean by abdominal discomfort? Is it located in certain part of the abdomen? When it comes I urgently go to the toilet. It is all around, I can’t specify any location. 9-Recent dietary history, consumption of meats (cooked, uncooked) eggs, seafood, or unusual foods? I ate fast food last night in the restaurant. 10-Anyone around you have the same symptoms? No 11-Does anything make it better or worse? I did not recognize anything specific. -
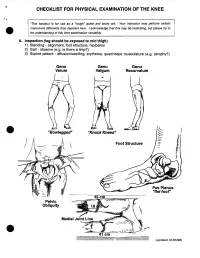
Checklist for Physical Examination of the Knee
• CHECKLIST FOR PHYSICAL EXAMINATION OF THE KNEE *This handout is for use as a "rough" guide and study aid. Your instructor may perform certain maneuvers differently than depicted here. I acknowledge that this may be frustrating, but please try to be understanding of this inter-examination variability. • A. Inspection (leg should be exposed to mid thigh) 1) Standing - alignment, foot structure, hip/pelvis 2) Gait - observe (e.g. is there a limp?) 3) Supine patient - effusion/swelling, erythema, quadriceps musculature (e.g. atrophy?) Genu Genu Genu Varum Valgum Recurvatum I .. "Bowlegged" "Knock Kneed" I • l ) Foot Structure \ J rI. Pes Planus "flat foot" Pelvic - / Obliquity ~.. • (updated 01/05/98) ... B. Palpation • w 1) Student should indicate that these were checked a) Warmth b) Crepitus (What is it? What might it represent?) • c) Effusion Test for effusion .. Fluid wave • Test for effusion .. Ballotable patella \ • 2 2) Tenderness (landmarks) - Medial/lateral joint lines, MCl, lClJ patellar facets, quadriceps insertion, patellar tendon, tibial tubercle, iliotibial band, pes anserine 0 0 (Patient is supine with the knee flexed to a comforable postion "" 20 - 90 ) • Anatomy of the knee jOint (right) (anteromedial aspect) ·....--Ijj;,HHI"'~-ME!CJ. Epicondyle of Femur TIbial Tu hAI~"'Ij£_ Medial Joint Line Area of Pes Anserine Insertion • • 3 Points of orientation for palpation of the knee • (Always start with the t distal pole of patella.) then ... • • 4 The patellar tendon is p'alpated toward 12" at the tibial tubercle • The Tibial Tubercle (Insertion of Patellar Tendon) • MEDIAL VIEW Tibial Tubercle ';',I" y,'". ~ "Pes Anser~I ne n Insertion of the sartorius, gracilis, • and semitendinosus tendons. -

SOAP Notes Format in EMR
SOAP Notes Format in EMR SOAP stands for Subjective, Objective, Assessment, and Plan Standard Elements of SOAPnote Date: 08/01/02 Time: Provider: Vital Signs: Height, Weight, Temp, B/P, Pulse S: This ___ yr old fe/male presents for ____ History of Present Illness symptoms: Review Of Symptoms/Systems: (For problem-focused visit, document only pertinent information) Past Medical History: (For problem-focused visit, document only pertinent information) Current Medications: Medication allergies: Social History: (For problem-focused visit, document only pertinent information) Family History: ((For problem-focused visit, document only pertinent information) Genogram: 3 generations with health problems, causes of deaths, etc. or History of major health or genetic disorders in family, including early death, spontaneous abortions or stillbirths. Social History: Past Medical History History of Present Illness: Cultural Background: Hospitalizations: Location: Education Level: Surgical History: Quality Economic Condition: T&A: Severity: Housing: Appendectomy: Duration: Number in household: Hysterectomy: Timing (Onset): Marital Status: Hernia: Timing (Frequency): Lives with: Coronary Artery Bypass: Context: Children: Other: Relieved by: Chronic Medical Problems: Occupation: Hypertension Worsened by: Occupational Health Diabetes Associated signs and symptoms: Hazards: Coronary Heart Disease Nutrition: Cerebrovascular Disease Exercise: Asthma or other COPD Tobacco use: Arthritis Review Of Symptoms (Systems): Constitutional: Caffeine: Gout Sexual activity: -

Role of Physical Exam, General Observation, Skin Screening & Vital
Role of Physical Exam, General Observation, Skin Screening & Vital Signs Charlie Goldberg, MD POM – September 18, 2019 Professor of Medicine, UCSD SOM [email protected] Reading, Prep & Other Tools • Bate’s Guide To The Physical Examination and History Taking, 12th ed - Lynn Bickley • Practical Guide To Clinical Medicine, Charlie Goldberg and Jan Thompson – Created explicitly for USCD SOM http://meded.ucsd.edu/clinicalmed/ & Links to other on-line resources http://meded.ucsd.edu/clinicalmed/links.htm • Catalog of Clinical Images https://meded.ucsd.edu/clinicalimg/ • Digital DDx http://digitalddx.com/ Check Lists • Each session has a check list • Posted on POM1 Web Site – example below • Also via PocketPex App (free): • iPhones, android phones Pocket PEx Purpose Of The Physical Exam • Screening for occult disease, assure good health, develop relationship w/patient • Identify cause of symptoms, guide use of adjuvant testing • Follow known disease, assist in adjusting treatment • Part of mystique & magic of medicine – power of touch & observation • ***Exam inextricably linked to the History*** Review Of Systems (ROS) & Connection to Clinical Care • List of questions, arranged by organ system (e.g. cardiac, pulmonary, neurologic, etc.) designed to uncover dysfunction and disease • Screening tool asked of every patient • Asked only of patients who fall into particular risk categories • Asked to better define the likely causes of a presenting symptom Practical Approach To ROS • Gain facility, so can apply right questions @ right time