Prevention of Infection in Children and Adolescents with Primary Immunodeficiency Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Recurrent Infection, Pulmonary Disease, and Autoimmunity As Manifestations of Immune Deficiency Property of Presenter Not for Re
Recurrent Infection, Pulmonary Disease, and Autoimmunity as Manifestations of Immune Deficiency Presenter of Erwin W. ReproductionGelfand, M.D. Professor, Departmentfor of Pediatrics PropertyNational Jewish Health Professor ofNot Immunology and Pediatrics University of Colorado School of Medicine Presenter of Reproduction for Property Not • Investigator: Boehringer Ingelheim Disclosures Learning Objectives • To understand the interplay between immunodeficiency and allergic and pulmonary disorders. Presenter • To recognize the increasingof numbers of monoallelic immune systemReproduction mutations that have allergic and pulmonaryfor manifestations. • To incorporateProperty genetic testing in the clinical Not evaluation of patients with seemingly common diseases. Presenter of Reproduction for Property Not Hypogammaglobulinemia (Immunodeficiency) Autoimmunity HypersensitivityAllergy Host Defense Specific Non-Specific Presenter of • Adaptive immunity • Innate immunity Reproduction • Barriers for Property Not The Innate and Adaptive Immune Response Specific antigen receptors Presenter of Reproduction for Property Pattern Not recognition receptors Dranoff G. Nature Reviews Cancer 2004;4:11-22. Presenter of Reproduction for Property Not Primary Immunodeficiency Diseases Infection Malignancy Autoimmunity Atopy Primary Immunodeficiency Diseases Infection Autoimmunity Malignancy Presenter of Deficient/defective Deficient/defective effector cells Reproductionregulatory cells for Property Not Primary Immunodeficiency Diseases Infection Autoimmunity -

Cells, Tissues and Organs of the Immune System
Immune Cells and Organs Bonnie Hylander, Ph.D. Aug 29, 2014 Dept of Immunology [email protected] Immune system Purpose/function? • First line of defense= epithelial integrity= skin, mucosal surfaces • Defense against pathogens – Inside cells= kill the infected cell (Viruses) – Systemic= kill- Bacteria, Fungi, Parasites • Two phases of response – Handle the acute infection, keep it from spreading – Prevent future infections We didn’t know…. • What triggers innate immunity- • What mediates communication between innate and adaptive immunity- Bruce A. Beutler Jules A. Hoffmann Ralph M. Steinman Jules A. Hoffmann Bruce A. Beutler Ralph M. Steinman 1996 (fruit flies) 1998 (mice) 1973 Discovered receptor proteins that can Discovered dendritic recognize bacteria and other microorganisms cells “the conductors of as they enter the body, and activate the first the immune system”. line of defense in the immune system, known DC’s activate T-cells as innate immunity. The Immune System “Although the lymphoid system consists of various separate tissues and organs, it functions as a single entity. This is mainly because its principal cellular constituents, lymphocytes, are intrinsically mobile and continuously recirculate in large number between the blood and the lymph by way of the secondary lymphoid tissues… where antigens and antigen-presenting cells are selectively localized.” -Masayuki, Nat Rev Immuno. May 2004 Not all who wander are lost….. Tolkien Lord of the Rings …..some are searching Overview of the Immune System Immune System • Cells – Innate response- several cell types – Adaptive (specific) response- lymphocytes • Organs – Primary where lymphocytes develop/mature – Secondary where mature lymphocytes and antigen presenting cells interact to initiate a specific immune response • Circulatory system- blood • Lymphatic system- lymph Cells= Leukocytes= white blood cells Plasma- with anticoagulant Granulocytes Serum- after coagulation 1. -
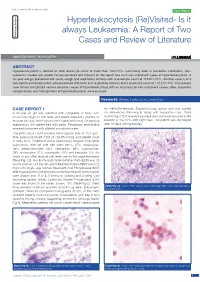
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

DOCK8 Regulates Fitness and Function of Regulatory T Cells Through Modulation of IL-2 Signaling
DOCK8 regulates fitness and function of regulatory T cells through modulation of IL-2 signaling Akhilesh K. Singh, … , Troy R. Torgerson, Mohamed Oukka JCI Insight. 2017;2(19):e94275. https://doi.org/10.1172/jci.insight.94275. Research Article Immunology Foxp3+ Tregs possess potent immunosuppressive activity, which is critical for maintaining immune homeostasis and self- tolerance. Defects in Treg development or function result in inadvertent immune activation and autoimmunity. Despite recent advances in Treg biology, we still do not completely understand the molecular and cellular mechanisms governing the development and suppressive function of these cells. Here, we have demonstrated an essential role of the dedicator of cytokinesis 8 (DOCK8), guanine nucleotide exchange factors required for cytoskeleton rearrangement, cell migration, and immune cell survival in controlling Treg fitness and their function. Treg-specific DOCK8 deletion led to spontaneous multiorgan inflammation in mice due to uncontrolled T cell activation and production of proinflammatory cytokines. In addition, we show that DOCK8-deficient Tregs are defective in competitive fitness and in vivo suppressive function. Furthermore, DOCK8 controls IL-2 signaling, crucial for maintenance and competitive fitness of Tregs, via a STAT5- dependent manner. Our study provides potentially novel insights into the essential function of DOCK8 in Tregs and immune regulation, and it explains the autoimmune manifestations associated with DOCK8 deficiency. Find the latest version: https://jci.me/94275/pdf RESEARCH ARTICLE DOCK8 regulates fitness and function of regulatory T cells through modulation of IL-2 signaling Akhilesh K. Singh,1 Ahmet Eken,1 David Hagin,1 Khushbu Komal,1 Gauri Bhise,1 Azima Shaji,1 Tanvi Arkatkar,1 Shaun W. -

Practice Parameter for the Diagnosis and Management of Primary Immunodeficiency
Practice parameter Practice parameter for the diagnosis and management of primary immunodeficiency Francisco A. Bonilla, MD, PhD, David A. Khan, MD, Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD, David I. Bernstein, MD, Joann Blessing-Moore, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Chief Editor: Francisco A. Bonilla, MD, PhD Co-Editor: David A. Khan, MD Members of the Joint Task Force on Practice Parameters: David I. Bernstein, MD, Joann Blessing-Moore, MD, David Khan, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Primary Immunodeficiency Workgroup: Chairman: Francisco A. Bonilla, MD, PhD Members: Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD GlaxoSmithKline, Merck, and Aerocrine; has received payment for lectures from Genentech/ These parameters were developed by the Joint Task Force on Practice Parameters, representing Novartis, GlaxoSmithKline, and Merck; and has received research support from Genentech/ the American Academy of Allergy, Asthma & Immunology; the American College of Novartis and Merck. -

The Extended Clinical Phenotype of 64 Patients with Dedicator of Cytokinesis 8 Deficiency
The extended clinical phenotype of 64 patients with dedicator of cytokinesis 8 deficiency Karin R. Engelhardt, PhD,a,b,c Michael E. Gertz, PhD,d Sevgi Keles, MD,e,f,g* Alejandro A. Schaffer,€ PhD,d* Elena C. Sigmund, BSc,b Cristina Glocker, PhD,b Shiva Saghafi, MSc,h Zahra Pourpak, MD, PhD,h Ruben Ceja, MSc,e,g Atfa Sassi, PhD,i Laura E. Graham, BSc, MBChB,a Michel J. Massaad, PhD,g Fethi Mellouli, MD,j Imen Ben-Mustapha, MD,i Monia Khemiri, MD,k Sara Sebnem Kilic, MD,l Amos Etzioni, MD,m Alexandra F. Freeman, MD,n Jens Thiel, MD,b Ilka Schulze, MD,b Waleed Al-Herz, MD,o Ayse Metin, MD, PhD,p Ozden€ Sanal, MD,q Ilhan Tezcan, MD,q Mehdi Yeganeh, MD,r Tim Niehues, MD,s Gregor Dueckers, MD,s Sebastian Weinspach, MD,t Turkan Patiroglu, MD,u Ekrem Unal, MD,v Majed Dasouki, MD,w Mustafa Yilmaz, MD,x Ferah Genel, MD,y Caner Aytekin, MD,z Necil Kutukculer, MD,aa Ayper Somer, MD,bb Mehmet Kilic, MD,cc Ismail Reisli, MD,f Yildiz Camcioglu, MD,dd Andrew R. Gennery, MD,c Andrew J. Cant, MD,c Alison Jones, MD,ee Bobby H. Gaspar, MD,ee Peter D. Arkwright, MD, DPhil,ff Maria C. Pietrogrande, MD,gg Zeina Baz, MD,hh Salem Al-Tamemi, MD,ii Vassilios Lougaris, MD,jj Gerard Lefranc, PhD,kk Andre Megarbane, MD, PhD,ll Jeannette Boutros, MD,mm Nermeen Galal, MD,mm Mohamed Bejaoui, MD,j Mohamed-Ridha Barbouche, MD, PhD,i Raif S. Geha, MD,g Talal A. -

Original Article Anemia, Leukocytosis and Eosinophilia in a Resource-Poor
Original Article Anemia, leukocytosis and eosinophilia in a resource-poor population with helmintho-ectoparasitic coinfection Daniel Pilger1, Jörg Heukelbach2, Alexander Diederichs1, Beate Schlosser1, Cinthya Pereira Leite Costa Araújo3, Anne Keysersa1, Oliver Liesenfeld1, Hermann Feldmeier1 1Charité - Universitätsmedizin Berlin, Campus Benjamin Franklin, Institute of Microbiology and Hygiene, D-12203 Berlin, Germany 2Department of Community Health, School of Medicine, Federal University of Ceará, Fortaleza, CE 60430-140, Brazil 3Department of Hematology, Estate University of Health Science of Alagoas, Alagoas, CEP 57010-300, Brazil Abstract Introduction: Eosinophilia and anemia are very common hematological alterations in the tropics but population-based studies scrutinizing their value for diagnosing parasitic infections are rare. Methodology: A cross-sectional study was conducted in a rural district in northeast Brazil where parasitic infections are common. Stool and blood samples were collected and individuals were clinically examined for the presence of ectoparasites. Results: In total, 874 individuals were examined. Infection with intestinal helminths occurred in 70% (95% CI 67 – 75), infestation with ectoparasites in 45% (95% CI 42 - 49) and co-infection with both helminths and ectoparasites was found in 33% (95% CI 29% - 36%) of all inhabitants. Eosinophil counts ranged from 40/µl to 13.800/µl (median: 900/µl). Haemoglobin levels ranged from 4.8 g/dl to 16.8 g/dl (median: 12.5 g/dl), and anemia was present in 24% of the participants. Leukocytosis was found in 13%, eosinophilia in 74%, and hypereosinophilia in 44% of the participants. Eosinophilia was more pronounced in individuals co-infected with intestinal helminths and ectoparasites (p < 0.001) and correctly predicted parasitic infection in 87% (95% CI 84%-90.7%) of all cases. -

Hyper Ige Syndromes and DOCK8 Forms of HIES Table 20:1
Immune Deficiency Foundation Patient & Family Handbook For Primary Immunodeficiency Diseases Chapter 20 Immune Deficiency Foundation Patient & Family Handbook For Primary Immunodeficiency Diseases 6th Edition The development of this publication was supported by Shire, now Takeda. 110 West Road, Suite 300 Towson, MD 21204 800.296.4433 www.primaryimmune.org [email protected] Chapter 20 Hyper IgE Syndromes (HIES): STAT3 Loss of Function, DOCK8 Deficiency and Others Alexandra Freeman, MD, National Institutes of Health, Bethesda, Maryland, USA Jennifer Heimall, MD, Children’s Hospital of Philadelphia, Philadelphia, Pennsylvania, USA Hyper IgE Syndromes (HIES) are rare forms of primary immunodeficiency diseases (PI) characterized by recurrent eczema, skin abscesses, lung infections, eosinophilia (high numbers of eosinophils in the blood), and high serum levels of immunoglobulin E (IgE). Although initially described as two forms, with autosomal dominant (AD) and autosomal recessive (AR) inheritance, we now recognize that these are two distinct diseases caused by different genetic causes, with the two most common being from harmful mutations in STAT3 causing loss of function (STAT3-LOF) and DOCK8. These diseases share overlapping clinical and laboratory features; however, they also exhibit distinct clinical symptoms, disease courses, and outcomes. In addition, several other genetic variants have since been described to present with similar symptoms. History Clinical Presentation STAT3-LOF was described first as Job Syndrome STAT3 Deficiency in 1966 in two girls with many episodes of STAT3 Deficiency, is associated with heterozygous pneumonia, eczema-like rashes, and recurrent skin loss of function mutations in the transcription factor boils. These boils were remarkable for their lack STAT3. This is the more common form of HIES in of surrounding warmth, redness or tenderness, the U.S. -

Leukocytosis & Lymphocytosis
Leukocytosis Leukocytosis >11 (Repeated) Blood Smear AND History & EMERGENT REFERRAL Refer to Blasts on Smear Physical Exam Lymphocytes >4 Page Hematologist On-Call Lymphocytosis Algorithm Include nodes and spleen Myeloid Cells Basophils Monocytes Neutrophils Eosinophils CONCERNING FEATURES CONCERNING FEATURES CONCERNING FEATURES » Count >2 or increasing, or persistent » Count >50 » Count >2 or increasing or persistent » Not explained by infection » Promyelocytes and myelocytes » Dysplasia YES » Dysplasia » Dysplasia YES » Anemia » Immature forms » Basophilia » New organ damage » Anemia/thrombo-cytopenia » Splenomegaly » NOT explained by infection, allergies » Splenomegaly » NOT associated with acute infection or collagen vascular disease NO NO NO Consider Consider » Cancer Reactive Causes » drugs NO » Collagen VD YES e.g. Infection / inflammation, NO NO » Infections YES » Chronic infection autoimmune, drugs esp. steroids » Allergies » Marrow recovery » Collagen Vascular Disease Refer to Hematology Treat and Observe for recovery Refer to Hematology Treat and Observe for recovery © Blood Disorder Day Pathways are subject to clinical judgement and actual practice patterns may not always follow the proposed steps in this pathway. Lymphocytosis Lymphocytosis >4 (Repeated) Concerning Features “Reactive” Lymphocytes Asymptomatic » Lymphocytes >30 Patient symptoms of infection or acute illness » Hgb <100 » Night sweats/ weight loss » Splenomegaly Flow Cytometry AND Flow Cytometry IF PERSISTENT Work-up for secondary causes »Immunization »Viral -

1. Introduction to Immunology Professor Charles Bangham ([email protected])
MCD Immunology Alexandra Burke-Smith 1. Introduction to Immunology Professor Charles Bangham ([email protected]) 1. Explain the importance of immunology for human health. The immune system What happens when it goes wrong? persistent or fatal infections allergy autoimmune disease transplant rejection What is it for? To identify and eliminate harmful “non-self” microorganisms and harmful substances such as toxins, by distinguishing ‘self’ from ‘non-self’ proteins or by identifying ‘danger’ signals (e.g. from inflammation) The immune system has to strike a balance between clearing the pathogen and causing accidental damage to the host (immunopathology). Basic Principles The innate immune system works rapidly (within minutes) and has broad specificity The adaptive immune system takes longer (days) and has exisite specificity Generation Times and Evolution Bacteria- minutes Viruses- hours Host- years The pathogen replicates and hence evolves millions of times faster than the host, therefore the host relies on a flexible and rapid immune response Out most polymorphic (variable) genes, such as HLA and KIR, are those that control the immune system, and these have been selected for by infectious diseases 2. Outline the basic principles of immune responses and the timescales in which they occur. IFN: Interferon (innate immunity) NK: Natural Killer cells (innate immunity) CTL: Cytotoxic T lymphocytes (acquired immunity) 1 MCD Immunology Alexandra Burke-Smith Innate Immunity Acquired immunity Depends of pre-formed cells and molecules Depends on clonal selection, i.e. growth of T/B cells, release of antibodies selected for antigen specifity Fast (starts in mins/hrs) Slow (starts in days) Limited specifity- pathogen associated, i.e. -

Exotics Oncology: Special Focus on Updates on Therapies for Rabbits & Ferrets
Exotics Oncology: Special Focus on Updates on Therapies for Rabbits & Ferrets La’Toya Latney, DVM Exotic Companion Animal Medicine Service Penn Vet THYMOMAS IN RABBITS Rabbits possess a persistent thymus, which does not involute with age. The thymus is comprised of thymic epithelium, reticuloendothelial tissue, and lymphoid tissue. Primary thymic neoplasms recognized in rabbits include (1) benign neoplasm of thymic epithelial cells, (2) thymic carcinoma, a rare malignant neoplasm of the epithelial cells and (3) thymic lymphoma, which is a malignant neoplasm of the lymphoid tissue of the thymus. Clinically, thymomas are diagnosed as lymphoid-rich, epithelial-rich, or mixed lymphoepithelial. The incidence in pet rabbits is largely unknown, however in one retrospective study, thymomas comprised 7% of all neoplasms in 55 colony rabbits in rabbits 2-4 years of age in 1949. More recently, in a retrospective evaluation of 1,100 female rabbits more than 2 years of age submitted for necropsy over a 17-year period, 4 cases of the 234 rabbits that had neoplasia were thymomas (Andres 2012). Literary resources are mainly comprised of clinical case reports (Guzman, Kunzel, Pilny, Bennett, Kovalik, Wagner, Quesenberry, Florizoone, Vernau). Based on current literature, there is no specific sex predisposition, but the common age range is 3-10 years of age, with the median age of 6 years (Kunzel, Andres). Certain breeds have been consistently prominent in clinical case reports, including Netherland dwarves and Lionhead rabbits (Kunzel, Andres). Clinical signs commonly include severe dyspnea and nasal flaring, third eyelid protrusion, orthopneic body position, and bilateral exophthalmos due to caval compression resulting in the pooling of blood in retrobulbar venous plexus. -

Bleeding Disorders in Congenital Syndromes Susmita N
Bleeding Disorders in Congenital Syndromes Susmita N. Sarangi, MD, Suchitra S. Acharya, MD Pediatricians provide a medical home for children with congenital abstract syndromes who often need complex multidisciplinary care. There are some syndromes associated with thrombocytopenia, inherited platelet disorders, factor deficiencies, connective tissue disorders, and vascular abnormalities, which pose a real risk of bleeding in affected children associated with trauma or surgeries. The risk of bleeding is not often an obvious feature of the syndrome and not well documented in the literature. This makes it especially hard for pediatricians who may care for a handful of children with these rare congenital syndromes in their lifetime. This review provides an overview of the etiology of bleeding in the different congenital syndromes along with a concise review of the hematologic and nonhematologic clinical manifestations. It also highlights the need and timing of diagnostic evaluation to uncover the bleeding risk in these syndromes emphasizing a primary care approach. Bleeding Disorders and Thrombosis Program, Cohen Children with congenital syndromes these patients as part of surveillance Children’s Medical Center of New York, New Hyde Park, with multiple anomalies need a or before scheduled procedures New York multidisciplinary approach to and recommends guidelines for Drs Sarangi and Acharya contributed to the their care, along with continued appropriate and timely referral to the conceptualization, content, and composition of the surveillance for rare manifestations hematologist. manuscript and approved the fi nal manuscript as such as a bleeding diathesis, which submitted. may not be evident at diagnosis. This Achieving hemostasis is a complex DOI: 10.1542/peds.2015-4360 accompanying bleeding diathesis process starting with endothelial Accepted for publication Aug 15, 2016 due to thrombocytopenia or other injury that results in platelet plug Address correspondence to Suchitra S.