Salisbury Helathcare Nhs Trust
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Focal Spot, Spring 2006
Washington University School of Medicine Digital Commons@Becker Focal Spot Archives Focal Spot Spring 2006 Focal Spot, Spring 2006 Follow this and additional works at: http://digitalcommons.wustl.edu/focal_spot_archives Recommended Citation Focal Spot, Spring 2006, April 2006. Bernard Becker Medical Library Archives. Washington University School of Medicine. This Book is brought to you for free and open access by the Focal Spot at Digital Commons@Becker. It has been accepted for inclusion in Focal Spot Archives by an authorized administrator of Digital Commons@Becker. For more information, please contact [email protected]. SPRING 2006 VOLUME 37, NUMBER 1 *eiN* i*^ MALLINCKRC RADIOLO AJIVERSITY *\ irtual Colonoscopy: a Lifesaving Technology ^.IIMi.|j|IUII'jd-H..l.i.|i|.llJ.lii|.|.M.; 3 2201 20C n « ■ m "■ ■ r. -1 -1 NTENTS FOCAL SPOT SPRING 2006 VOLUME 37, NUMBER 1 MIR: 75 YEARS OF RADIOLOGY EXPERIENCE In the early 1900s, radiology was considered by most medical practitioners as nothing more than photography. In this 75th year of Mallinckrodt Institute's existence, the first of a three-part series of articles will chronicle the rapid advancement of radiol- ogy at Washington University and the emergence of MIR as a world leader in the field of radiology. THE METABOLISM OF THE DIABETIC HEART More diabetic patients die from cardiovascular disease than from any other cause. Researchers in the Institute's Cardiovascular Imaging Laboratory are finding that the heart's metabolism may be one of the primary mechanisms by which diseases such as diabetes have a detrimental effect on heart function. VIRTUAL C0L0N0SC0PY: A LIFESAVING TECHNOLOGY More than 55,000 Americans die each year from cancers of the colon and rectum. -

Research Article Magnetic Resonance Sialography Findings of Submandibular Ducts Imaging
Hindawi Publishing Corporation BioMed Research International Volume 2013, Article ID 417052, 6 pages http://dx.doi.org/10.1155/2013/417052 Research Article Magnetic Resonance Sialography Findings of Submandibular Ducts Imaging Nezahat Karaca ErdoLan,1 Canan Altay,2 Nesibe Özenler,3 TuLba Bozkurt,1 Engin Uluç,1 Berna Dirim Mete,1 and Esmail Özdemir4 1 Department of Radiology, Izmir Ataturk¨ Research and Training Hospital, Basın Sitesi, Karabaglar,˘ 35360 Izmir, Turkey 2 Department of Radiology, Medical School, Dokuz Eylul University, Inciralti, 35340 Izmir, Turkey 3 Department of Radiology, Balıkesir Ataturk¨ State Hospital, Yıldız Mahallesi Soma Caddesi No. 1, 10100 Balıkesir, Turkey 4 Universal Ege Health Hospital, 35220 Izmir, Turkey Correspondence should be addressed to Canan Altay; [email protected] Received 2 April 2013; Revised 29 May 2013; Accepted 12 June 2013 Academic Editor: Yoshito Tsushima Copyright © 2013 Nezahat Karaca Erdogan˘ et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Purpose. We aimed to assess the problem solving capability of magnetic resonance sialography (MR sialography), a noninvasive method for imaging submandibular gland ducts and determining duct-related pathologies, by comparing diseased and healthy cases. Materials and Methods. We conducted radiological assessment on a total of 60 submandibular glands (mean age 44.7) in 20 cases and 10 volunteers. MR sialography examinations were conducted with single-shot fast spin-echo sequence by using a surface coil placed on the submandibular gland. Each gland was evaluated in terms of the length, width and stricture of the main duct, as well as the difference between the intraparenchymal duct width, and the main duct width. -

Rectal Water Contrast Transvaginal Ultrasound Versus Double-Contrast Barium Enema in the Diagnosis of Bowel Endometriosis
Open Access Research BMJ Open: first published as 10.1136/bmjopen-2017-017216 on 7 September 2017. Downloaded from Rectal water contrast transvaginal ultrasound versus double-contrast barium enema in the diagnosis of bowel endometriosis Jipeng Jiang, Ying Liu, Kun Wang, Xixiang Wu, Ying Tang To cite: Jiang J, Liu Y, Wang K, ABSTRACT Strengths and limitations of this study et al. Rectal water contrast Objectives The aim of study was to compare the transvaginal ultrasound versus accuracy between rectal water contrast transvaginal ► This is the first comparison of the accuracy between double-contrast barium enema ultrasound (RWC-TVS) and double-contrast barium enema in the diagnosis of bowel rectal water contrast transvaginal ultrasound (RWC- (DCBE) in evaluating the bowel endometriosis presence as endometriosis. BMJ Open TVS) and double-contrast barium enema (DCBE) in well as its extent. 2017;7:e017216. doi:10.1136/ the diagnosis of bowel endometriosis. Design and setting 198 patients at reproductive age with bmjopen-2017-017216 ► This study demonstrated RWC-TVS as a very reliable suspicious bowel endometriosis were included. Physicians technique to determine the bowel endometriosis ► Prepublication history for in two groups specialised at endometriosis performed presence and extent and it has similar accuracy to this paper is available online. RWC-TVS as well as DCBE before laparoscopy and both To view these files please visit that of DCBE. groups were blinded to other groups’ results. Findings the journal online (http:// dx. doi. ► We demonstrate that DCBE is related to more from RWC-TVS or DCBE were compared with histological org/ 10. 1136/ bmjopen- 2017- tolerance than RWC-TVS. -
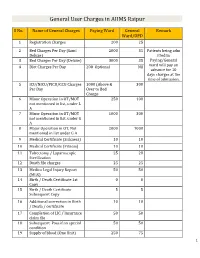
General User Charges in AIIMS Raipur
General User Charges in AIIMS Raipur S No. Name of General Charges Paying Ward General Remark Ward/OPD 1 Registration Charges 200 25 2 Bed Charges Per Day (Sami 2000 35 Patients being adm Deluxe) itted in 3 Bed Charges Per Day (Deluxe) 3000 35 Paying/General 4 Diet Charges Per Day 200 Optional Nil ward will pay an advance for 10 days charges at the time of admission. 5 ICU/NICU/PICU/CCU Charges 1000 (Above & 300 Per Day Over to Bed Charge 6 Minor Operation in OT/MOT 250 100 not mentioned in list, under L A 7 Minor Operation in OT/MOT 1000 300 not mentioned in list, under G A 8 Major Operation in OT, Not 2000 1000 mentioned in list under G A 9 Medical Certificate (Sickness) 10 10 10 Medical Certificate (Fitness) 10 10 11 Tubectomy / Laparoscopic 25 20 Sterilization 12 Death file charges 25 25 13 Medico Legal Injury Report 50 50 (MLR) 14 Birth / Death Certificate 1st 0 0 Copy 15 Birth / Death Certificate 5 5 Subsequent Copy 16 Additional correction in Birth 10 10 / Death / certificate 17 Completion of LIC / Insurance 50 50 claim file 18 Subsequent Pass if on special 50 50 condition 19 Supply of blood (One Unit) 250 75 1 20 Medical Board Certificate 500 500 On Special Case User Charges for Investigations in AIIMS Raipur S No. Name of Investigations Paying General Remark Ward Ward/OPD Anaesthsia 1 ABG 75 50 2 ABG ALONGWITH 150 100 ELECTROLYTES(NA+,K+)(Na,K) 3 ONLY ELECTROLYTES(Na+,K+,Cl,Ca+) 75 50 4 ONLY CALCIUM 50 25 5 GLUCOSE 25 20 6 LACTATE 25 20 7 UREA. -

ACR Manual on Contrast Media
ACR Manual On Contrast Media 2021 ACR Committee on Drugs and Contrast Media Preface 2 ACR Manual on Contrast Media 2021 ACR Committee on Drugs and Contrast Media © Copyright 2021 American College of Radiology ISBN: 978-1-55903-012-0 TABLE OF CONTENTS Topic Page 1. Preface 1 2. Version History 2 3. Introduction 4 4. Patient Selection and Preparation Strategies Before Contrast 5 Medium Administration 5. Fasting Prior to Intravascular Contrast Media Administration 14 6. Safe Injection of Contrast Media 15 7. Extravasation of Contrast Media 18 8. Allergic-Like And Physiologic Reactions to Intravascular 22 Iodinated Contrast Media 9. Contrast Media Warming 29 10. Contrast-Associated Acute Kidney Injury and Contrast 33 Induced Acute Kidney Injury in Adults 11. Metformin 45 12. Contrast Media in Children 48 13. Gastrointestinal (GI) Contrast Media in Adults: Indications and 57 Guidelines 14. ACR–ASNR Position Statement On the Use of Gadolinium 78 Contrast Agents 15. Adverse Reactions To Gadolinium-Based Contrast Media 79 16. Nephrogenic Systemic Fibrosis (NSF) 83 17. Ultrasound Contrast Media 92 18. Treatment of Contrast Reactions 95 19. Administration of Contrast Media to Pregnant or Potentially 97 Pregnant Patients 20. Administration of Contrast Media to Women Who are Breast- 101 Feeding Table 1 – Categories Of Acute Reactions 103 Table 2 – Treatment Of Acute Reactions To Contrast Media In 105 Children Table 3 – Management Of Acute Reactions To Contrast Media In 114 Adults Table 4 – Equipment For Contrast Reaction Kits In Radiology 122 Appendix A – Contrast Media Specifications 124 PREFACE This edition of the ACR Manual on Contrast Media replaces all earlier editions. -

Procedure Codes for Physician: Radiology
NEW YORK STATE MEDICAID PROGRAM PHYSICIAN - PROCEDURE CODES SECTION 4 - RADIOLOGY Physician – Procedure Codes, Section 4 - Radiology Table of Contents GENERAL INSTRUCTIONS ............................................................................................................ 4 GENERAL RULES AND INFORMATION ......................................................................................... 6 MMIS RADIOLOGY MODIFIERS .................................................................................................... 8 DIAGNOSTIC RADIOLOGY (DIAGNOSTIC IMAGING)................................................................. 9 HEAD AND NECK.................................................................................................................... 9 CHEST .................................................................................................................................. 10 SPINE AND PELVIS .............................................................................................................. 11 UPPER EXTREMITIES .......................................................................................................... 12 LOWER EXTREMITIES ......................................................................................................... 13 ABDOMEN ............................................................................................................................ 14 GASTROINTESTINAL TRACT ............................................................................................... 15 URINARY -

Virtual Colonoscopy
Virtual Colonoscopy National Digestive Diseases Information Clearinghouse Virtual colonoscopy (VC) uses x rays and • You will be asked to hold your breath computers to produce two- and three- during the scan to avoid distortion on dimensional images of the colon (large the images. intestine) from the lowest part, the rectum, • The scanning procedure is then National all the way to the lower end of the small Institute of repeated with you lying on your Diabetes and intestine and display them on a screen. Digestive stomach. and Kidney The procedure is used to diagnose colon Diseases and bowel disease, including polyps, diver- After the examination, the information ticulosis, and cancer. VC can be performed from the scanner must be processed to NATIONAL INSTITUTES with computed tomography (CT), some- create the computer picture or image of OF HEALTH times called a CAT scan, or with magnetic your colon. A radiologist evaluates the resonance imaging (MRI). results to identify any abnormalities. You may resume normal activity after the VC Procedure procedure, although your doctor may While preparations for VC vary, you will usually be asked to take laxatives or other oral agents at home the day before the pro- cedure to clear stool from your colon. You Conventional Colonoscopy may also be asked to use a suppository to In a conventional colonoscopy, the cleanse your rectum of any remaining fecal doctor inserts a colonoscope—a long, matter. flexible, lighted tube—into the patient’s VC takes place in the radiology department rectum and slowly guides it up through of a hospital or medical center. -

Virtual Colonography
Virtual Colonography Radiologists at the VCU Medical Center were among the first in Virginia to develop, test and adopt for routine use a more patient-friendly way to screen for colon polyps and colon cancer. The noninvasive treatment procedure known medically as - Virtual Colonography (VC) or CT Colonography (CTC) - uses computed tomography (CT) scanning to determine whether or not colon polyps are present. Because Virtual Colonography does not require the use of a colonoscope as in a conventional colonoscopy procedure, it is sometimes referred to as a “Virtual Colonoscopy”. What makes Virtual Colonography an ideal option for screening? Because the procedure is noninvasive, safe, quick (lasting only a few minutes), and does not require sedation, Virtual Colonography is an excellent screening technology, and often preferred by patients over the conventional or standard colonoscopy. There are no risks of complications such as bowel perforation or complications from sedation associated with standard colonoscopy. Patients may return to their usual activities as soon as the test is over. Virtual Colonography also allows for evaluation of the entire colon, something a standard colonoscopy may not be able to do in all cases because normal twists and turns in the large intestines make navigating the colonoscope difficult. Virtual Colonography is accurate in identifying significant polyps and offers an alternative screening option for those who are simply not willing to undergo conventional colonoscopy, which is invasive, can be uncomfortable, and requires sedation. How accurate is Virtual Colonography compared to conventional colonoscopy? Early studies show that Virtual Colonography is comparable to conventional colonoscopy in terms of identifying polyps six millimeters or greater in size. -

Digestive Endoscopy in Five Decades
■ COLLEGE LECTURES Digestive endoscopy in five decades Peter B Cotton ABSTRACT – The world of gastroenterology scopy. So-called semi-flexible gastroscopes were changed forever when flexible endoscopes cumbersome and used infrequently by only a few became available in the 1960s. Diagnostic and enthusiasts. therapeutic techniques proliferated and entered the mainstream of medicine, not without some Diagnostic endoscopy controversy. Success resulted in a huge service demand, with the need to train more endo- The first truly flexible gastroscope was developed in 1 This paper is scopists and to organise large endoscopy units the USA, following pioneering work on fibre-optic 2 based on the Lilly and teams of staff. The British health service light transmission in the UK by Harold Hopkins. Lecture given at struggled with insufficient numbers of consul- However, commercial production of endoscopes was the Royal College tants, other staff and resources, and British rapidly dominated by Japanese companies, building of Physicians on endoscopy fell behind that of most other devel- on their earlier expertise with intragastric cameras. 12 April 2005 by oped countries. This situation is now being My involvement began in 1968, whilst doing bench Peter B Cotton addressed aggressively, with many local and research with Dr Brian Creamer at St Thomas’ MD FRCP FRCS, national initiatives aimed at improving access and Hospital, London. An expert in coeliac disease (and Medical Director, choice, and at promoting and documenting jejunal biopsy), he opined that gastroscopy might Digestive Disease quality. Many more consultants are needed and become useful and legitimate only if it became pos- Center, Medical some should be relieved of their internal medi- sible to take target biopsy specimens – since no one University of South Carolina, cine commitment to focus on their specialist seriously believed what endoscopists said that they Charleston, USA skills. -

Ography C Virtual Colonoscopy for Screening
466 Gut 2004;53:466 Gut: first published as on 11 February 2004. Downloaded from Please visit the Gut website (www.gutjnl.com) for links possible to generate three dimensional ultrasound cholangiograms. to these articles – many to full text. The authors prospectively evaluated the ability of this technique, compared with direct cholangiography (endoscopic retrograde cholangiopancreatography (ERCP)/percutaneous transhepatic cho- langiogram (PTC)) and MRCP, to detect and characterise biliary ....................................................................... obstruction in 40 patients. Experienced operators, who were blinded to the results of the other tests, evaluated images for Pseudo-pseudomembranous collagenous technical adequacy, presence and level of obstruction, and c suspected cause of any stricture. Compared with two dimensional colitis ultrasound, three dimensional analysis improved the assessment of m Yuan S, Reyes V, Bronner MP. Pseudomembranous collagenous colitis. Am J biliary anatomy in seven of 40 patients. Three dimensional Surg Pathol 2003;27:1375–9. ultrasound however visualised the peripapillary region less well Microscopic colitis has been divided into three types (Warren BF, et (80%) than MRCP (95%) and direct cholangiography (100%) but al. Histopathology 2002;40:374–6), all characterised by watery was superior at demonstrating the gall bladder and biliary tree diarrhoea and minimal mucosal changes at colonoscopy, asso- proximal to a stricture. All techniques were highly sensitive for ciated with an increase in lamina propria lymphocytes and minimal detection of biliary obstruction (100%) and each diagnosed the crypt architectural distortion. Of the three types, lymphocytic colitis likely cause in 90–95% of cases. Three dimensional ultrasound also has an increase in intraepithelial lymphocytes, collagenous detected the correct level of obstruction in 92% of cases compared colitis has a subepithelial collagen band, and microscopic colitis not with 95% for MRCP and 90% for ERCP/PTC. -

Posters and Exhibits
Posters and Exhibits List of Presiding Officers Ronald S. Arellano, MD Pamela T. Johnson, MDH Nabile M. Safdar, MD Tami J. Bang, MD Jamlik-Omari Johnson, MDH Mariano Scaglione, MD Ferco H. Berger, MD Douglas S. Katz, MD Alan E. Schlesinger, MD George S. Bisset III, MD Arvin Kheterpal, MD Aarti Sekhar, MD Matthew D. Bucknor, MD Gregory Kicska, MD, PhD Gaurang V. Shah, MD Brett W. Carter, MDH Edward Y. Kim, MD Anna Shapiro, MD Abhishek Chaturvedi, MD John Kim, MD Akash Sharma, MD Asim F. Choudhri, MD Phillip J. Koo, MDH Andrew Sher, MD Donna J. Cross, PhD Benjamin Larimer, PhD Atul B. Shinagare, MDH Cinthia Cruz, MD Karen S. Lee, MD Girish S. Shroff, MD Patricia M. de Groot, MD Seon-Kyu Lee, MD, PhD Dorothy A. Sippo, MD Zachary S. Delproposto, MD Bob Liu, PhD Clint W. Sliker, MD Jun Deng, PhD Zheng Feng Lu, PhD William C. Small, MD, PhD Vinay A. Duddalwar, MD, FRCR Martha B. Mainiero, MD Tina D. Tailor, MDH Gabriel C. Fine, MD Naganathan B. Mani, MD Ukihide Tateishi, MD, PhD Phoebe E. Freer, MD Gordon McLennan, MDH Temel Tirkes, MD David M. Gauntt, PhD Amy R. Mehollin-Ray, MD Srini Tridandapani, MD, PhDH Joseph R. Grajo, MD Martha G. Menchaca, MD, PhD Yolanda D. Tseng, MD John C. Grecula, MDH Suyash Mohan, MDH Dharshan R. Vummidi, MD, FRCR Martin L. Gunn, MBChBH Savvas Nicolaou, MDH Carolyn L. Wang, MD Richard S. Ha, MD Paul Nikolaidis, MD Antonio C. Westphalen, MDH Koichi Hayano, MD Ogonna K. Nwawka, MDH Sarah B. White, MD,MSH Pedram Heidari, MD Robert Orth, MD,PhD Geoffrey E. -

Virtual Colonoscopy Exam Preparation Stanford Radiology Scheduling Center for 7Days Before the Test: Phone: 650-723-6855 DO NOT Take Iron Pills (Ferrous Sulfate)
Scheduling An Appointment Virtual Colonoscopy Exam Preparation Stanford Radiology Scheduling Center For 7days before the test: Phone: 650-723-6855 DO NOT take iron pills (Ferrous Sulfate). DO NOT EAT foods with seeds such as poppy, tomatoes, watermelon, or cucumbers. Avoid celery, grapes, Fax: 650-723-6036 green peas, beans, seaweed, popcorn and nuts. For maps and directions, go to: Day before the test: www.imaging.stanfordhospital.com Starting at midnight, drink clear liquids only: Clear liquids includes water, tea with no milk, black coffee, Virtual 7-UP, ginger ale, apple juice, white grape juice, white cranberry juice (no juice that is red or purple), clear soup broth, gelatin (no red, blue, green or purple), popsicles (no red or purple). Redwood City Colonoscopy Stanford Medicine Outpatient Center You may wish to place the kit in the refrigerator to make the contents more pleasant to drink. Or, you may 450 Broadway Pavilion B, drink them at room temperature. Redwood City, CA 94063 Do not eat any solid food while on this diet. Do not drink alcohol. No dairy products. Stanford Medicine Imaging Step One - 11:00 am Take two Bisacodyl® (Dulcolax) tablets (5 mg each) with 1 glass of clear liquids. Hours: Monday-Friday, 7:00AM to 5:00 PM Services: MRI, CT, Diagnostic X-Ray, US, Bone Step Two - 2:00 pm Drink one bottle (296 mL) of magnesium citrate. Follow this with 6 cups of clear liquids over Density the next 90 minutes. Step Three - 5:00 pm Directions: From South (San Jose)-Take US-101 Mix package of barium sulfate (EZ CAT) with 450 mL of water.