Fibular (Peroneal) Neuropathy Electrodiagnostic Features and Clinical Correlates
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Tibialis Posterior Tendon Transfer Corrects the Foot Drop Component
456 COPYRIGHT Ó 2014 BY THE JOURNAL OF BONE AND JOINT SURGERY,INCORPORATED Tibialis Posterior Tendon Transfer Corrects the Foot DropComponentofCavovarusFootDeformity in Charcot-Marie-Tooth Disease T. Dreher, MD, S.I. Wolf, PhD, D. Heitzmann, MSc, C. Fremd, M.C. Klotz, MD, and W. Wenz, MD Investigation performed at the Division for Paediatric Orthopaedics and Foot Surgery, Department for Orthopaedic and Trauma Surgery, Heidelberg University Clinics, Heidelberg, Germany Background: The foot drop component of cavovarus foot deformity in patients with Charcot-Marie-Tooth disease is commonly treated by tendon transfer to provide substitute foot dorsiflexion or by tenodesis to prevent the foot from dropping. Our goals were to use three-dimensional foot analysis to evaluate the outcome of tibialis posterior tendon transfer to the dorsum of the foot and to investigate whether the transfer works as an active substitution or as a tenodesis. Methods: We prospectively studied fourteen patients with Charcot-Marie-Tooth disease and cavovarus foot deformity in whom twenty-three feet were treated with tibialis posterior tendon transfer to correct the foot drop component as part of a foot deformity correction procedure. Five patients underwent unilateral treatment and nine underwent bilateral treatment; only one foot was analyzed in each of the latter patients. Standardized clinical examinations and three-dimensional gait analysis with a special foot model (Heidelberg Foot Measurement Method) were performed before and at a mean of 28.8 months after surgery. Results: The three-dimensional gait analysis revealed significant increases in tibiotalar and foot-tibia dorsiflexion during the swing phase after surgery. These increases were accompanied by a significant reduction in maximum plantar flexion at the stance-swing transition but without a reduction in active range of motion. -

Peroneus Longus Tendon Regeneration After Anterior Cruciate Ligament Reconstruction with Magnetic Resonance Imaging Evaluation
Scientific Foundation SPIROSKI, Skopje, Republic of Macedonia Open Access Macedonian Journal of Medical Sciences. 2020 Nov 14; 8(A):916-920. https://doi.org/10.3889/oamjms.2020.5487 eISSN: 1857-9655 Category: A - Basic Sciences Section: Sports Medicine Peroneus Longus Tendon Regeneration after Anterior Cruciate Ligament Reconstruction with Magnetic Resonance Imaging Evaluation Sholahuddin Rhatomy1,2*, Bambang Kisworo3, Bunarwan Prihargono4, Faiz Alam Rashid1, Nolli Kressoni5 1Department of Orthopaedics and Traumatology, Dr. Soeradji Tirtonegoro General Hospital, Klaten, Indonesia; 2Department of Orthopaedics and Traumatology, Faculty of Medicine, Public Health and Nursing, Universitas Gadjah Mada, Yogyakarta, Indonesia; 3Department of Orthopaedics and Traumatology, Panti Rapih Hospital, Yogyakarta, Indonesia; 4Department of Orthopaedics and Traumatology, Karanganyar General Hospital, Karanganyar, Indonesia; 5Department of Radiology, Indriati Hospital, Sukoharjo, Indonesia Abstract Edited by: Slavica Hristomanova-Mitkovska BACKGROUND: Peroneus longus graft can be recommended as a superior graft over hamstring in anterior cruciate Citation: Rhatomy S, Kisworo B, Prihargono B, Rashid FA, Kressoni N. Peroneus Longus Tendon ligament (ACL) reconstruction. There are many studies concerning hamstring tendon regeneration, but there are few Regeneration after Anterior Cruciate Ligament studies on the regeneration of the peroneus longus tendon after ACL reconstruction. Reconstruction with Magnetic Resonance Imaging Evaluation. Open Access Maced J -

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -

Peroneal Nerve Injury Associated with Sports-Related Knee Injury
Neurosurg Focus 31 (5):E11, 2011 Peroneal nerve injury associated with sports-related knee injury DOSANG CHO, M.D., PH.D.,1 KRIANGSAK SAETIA, M.D.,2 SANGKOOK LEE, M.D.,4 DAVID G. KLINE, M.D.,3 AND DANIEL H. KIM, M.D.4 1Department of Neurosurgery, School of Medicine, Ewha Womans University, Seoul, Korea; 2Division of Neurosurgery, Department of Surgery, Ramathibodi Hospital, Mahidol University, Bangkok, Thailand; 3Department of Neurosurgery, Louisiana State University Health Sciences Center, New Orleans, Louisiana; and 4Department of Neurosurgery, Baylor College of Medicine, Houston, Texas Object. This study analyzes 84 cases of peroneal nerve injuries associated with sports-related knee injuries and their surgical outcome and management. Methods. The authors retrospectively reviewed the cases of peroneal nerve injury associated with sports between the years 1970 and 2010. Each patient was evaluated for injury mechanism, preoperative neurological status, electro- physiological studies, lesion type, and operative technique (neurolysis and graft repair). Preoperative status of injury was evaluated by using a grading system published by the senior authors. All lesions in continuity had intraoperative nerve action potential recordings. Results. Eighty-four (approximately 18%) of 448 cases of peroneal nerve injury were found to be sports related, which included skiing (42 cases), football (23 cases), soccer (8 cases), basketball (6 cases), ice hockey (2 cases), track (2 cases) and volleyball (1 case). Of these 84 cases, 48 were identified as not having fracture/dislocation and 36 cases were identified with fracture/dislocation for surgical interventions. Good functional outcomes from graft repair of graft length < 6 cm (70%) and neurolysis (85%) in low-intensity peroneal nerve injuries associated with sports were obtained. -

Cutaneous Innervation of the Lower Limb Cutaneous Nerves on the Front of the Thigh
Cutaneous Innervation of the Lower Limb https://www.earthslab.com/anatomy/cutaneous-innervation-of-the-lower-limb/ Cutaneous nerves on the front of the thigh • The ilio-inguinal nerve (L1) • The femoral branch of genitofemoral nerve (L1, L2) • The lateral cutaneous nerve of thigh (L2, L3) • The intermediate cutaneous nerve of thigh (L2, L3) • The medial cutaneous nerve of thigh (L2, L3) • The saphenous nerve (L3,4) https://www.slideshare.net/DrMohammadMahmoud/2-front-of-the-thigh-ii https://slideplayer.com/slide/9424949/ Cutaneous nerves of the gluteal region • Subcostal (T12) and ilio- hypogastric (L1) nerves • Posterior primary rami of L1,2,3 and S1,2,3 • Lateral cutaneous nerve of thigh (L2,3) • Posterior cutaneous nerve of thigh (S1,2,3) and perforating cutaneous nerve (S2,3) Cutaneous nerves on the front of leg and dorsum of foot • The infrapatellar branch of the saphenous nerve • The saphenous nerve • The lateral cutaneous nerve of the calf • The superficial peroneal nerve • The sural nerve • The deep peroneal nerve • The digital branches of the medial and lateral plantar nerves Cutaneous nerves on the back of leg • Saphenous nerve (L3, L4) • Posterior division of the medial cutaneous nerve of the thigh (L2, L3) • Posterior cutaneous nerve of the thigh (S1, S2, S3) • Sural nerve (L5, S1, S2) • Lateral cutaneous nerve of the calf (L4, L5, S1) • Peroneal or sural communicating nerve (L5, S1, S2) • Medial calcanean branches (S1, S2) Cutaneous nerves of the sole • Medial calcaneal branches of tibial nerve • Branches from medial plantar nerve • Branches from lateral plantar nerve SEGMENTAL INNERVATION Dermatomes • The area of skin supplied by one spinal segment is called a dermatome. -

Chronic Tibialis Anterior Tendon Tear Treated with an Achilles Tendon Allograft Technique
n tips & techniques Section Editor: Steven F. Harwin, MD Chronic Tibialis Anterior Tendon Tear Treated With an Achilles Tendon Allograft Technique Ezequiel Palmanovich, MD; Yaron S. Brin, MD; Lior Laver, MD; Dror Ben David, MD; Sabri Massrawe, MD; Meir Nyska, MD; Iftach Hetsroni, MD tus,16,17 rheumatoid arthritis,17 erative tibialis anterior tendon Abstract: Tibialis anterior tendon tear is an uncommon in- psoriasis,18 and deposition of was diagnosed clinically and jury. Nontraumatic or degenerative tears are usually seen gout tophi19,20 also have been confirmed by ultrasound. in the avascular zone of the tendon. Treatment can be con- reported to be associated with After 3 months of phys- servative or surgical. Conservative treatment is adequate tendon ruptures. In older pa- iotherapy treatment without for low-demand older patients. For active patients, surgical tients and in partial tears, non- improvement, surgical treat- treatment can be challenging for the surgeon because after operative treatment has been ment was recommended. The debridement of degenerative tissue, a gap may be formed described.8,21 patient’s American Orthopae- that can make side-to-side suture impossible. The authors Surgical techniques de- dic Foot and Ankle Society present allograft Achilles tendon insertion for reconstruc- scribed in the literature in- (AOFAS)22 score was 23 and tion of chronic degenerative tears. Using Achilles tendon al- clude direct side-to-side his Foot and Ankle Disabil- lograft has the advantage of bone-to-bone fixation, allowing repair and interposition of ity Index (FADI)23 score was rapid incorporation and earlier full weight bearing. autogenous tendon graft for 34.6 preoperatively. -

A Cadaver Research
Journal of Arthroscopy and Joint Surgery 6 (2019) 114e116 Contents lists available at ScienceDirect Journal of Arthroscopy and Joint Surgery journal homepage: www.elsevier.com/locate/jajs Tensile strength comparison between hamstring tendon, patellar tendon, quadriceps tendon and peroneus longus tendon: A cadaver research * Krisna Y. Phatama a, , Mohamad Hidayat a, Edi Mustamsir a, Ananto Satya Pradana a, Brian Dhananjaya b, Surya Iman Muhammad b a Orthopaedic and Traumatology Department, Lower Extremity and Adult Reconstruction Division, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No.2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia b Orthopaedic and Traumatology Department, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No. 2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia article info abstract Article history: Knee ligament injury is a frequent occurrence. Ligament reconstruction using tendon graft is the best Received 6 December 2018 therapy recommendation in the case of severe knee ligament injury. Tendon graft that is oftenly used are Accepted 15 February 2019 hamstring tendon, patellar tendon (BPTB), quadriceps tendon and peroneus longus tendon have been Available online 19 February 2019 proposed as tendon graft donor. Biomechanically, tensile strength from tendon graft is the main factor that greatly contributes to the success of ligament reconstruction procedure. Numerous researches have Keywords: been done to calculate tensile strengths of hamstring and patellar tendon, but there has not been a Ligament reconstruction research done yet on the comparison of the tensile strengths of peroneus longus tendon, hamstring, Tendon graft Tensile strength patellar tendon and quadriceps tendon. This research will strive to record the tensile strengths of per- oneus longus tendon, hamstring, patellar tendon and quadriceps tendon as well as their comparison. -

GBS/CIDP Foundation International
Guillain-Barré Syndrome GBS: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International 2012 Edition GBS/CIDP Foundation International The Holly Building 104 1/2 Forrest Avenue Narberth, PA 19072 Phone: 610.667.0131 Toll Free: 866.224.3301 Fax: 610.667.7036 [email protected] www.gbs-cidp.org Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals Contents Page Acknowledgements . i Introduction . 1 Initial Patient Evaluation . 4 Natural History of GBS: Implications for Patient Care . 6 Respiratory Complications . 8 Dysautonomia and Cardiovascular Complications . 12 Bladder, Bowel Dysfunction . 14 Metabolism: Nutrition, Hydration, Electrolytes . 14 Pain . 17 ICU Delirium . 18 Skin . 18 Musculo-Skeletal Issues, Occupational and Physical Therapy . 19 Infection . 22 Disorder Specific Treatments . 22 Appendix A. Checklist of Patient Issues to Monitor . 24 B. Diagnostic Criteria for GBS . 25 C. Prognosis . 26 References . 27 This pamphlet is provided as a service of the GBS/CIDP Foundation International Serving the medical community and patients with Guillain-Barré syndrome and related acute and chronic paralyzing disorders of the peripheral nerves. Acknowledgements Guillain-Barré syndrome (GBS) is a rare disorder. Some health professionals may not be familiar with treating it. A beautiful video by Tanya Ooraikul chronicled the superb care provided to her husband Kit during his recovery from GBS. His care at Gray Nuns Community Hospital in Edmonton, Alberta, Canada included 86 days in the intensive care unit. The video handsomely demonstrates the high quality of care that can be provided for this rare and complicated disorder in a community hospital. -

Femoral and Sciatic Nerve Blocks for Total Knee Replacement in an Obese Patient with a Previous History of Failed Endotracheal Intubation −A Case Report−
Anesth Pain Med 2011; 6: 270~274 ■Case Report■ Femoral and sciatic nerve blocks for total knee replacement in an obese patient with a previous history of failed endotracheal intubation −A case report− Department of Anesthesiology and Pain Medicine, School of Medicine, Catholic University of Daegu, Daegu, Korea Jong Hae Kim, Woon Seok Roh, Jin Yong Jung, Seok Young Song, Jung Eun Kim, and Baek Jin Kim Peripheral nerve block has frequently been used as an alternative are situations in which spinal or epidural anesthesia cannot be to epidural analgesia for postoperative pain control in patients conducted, such as coagulation disturbances, sepsis, local undergoing total knee replacement. However, there are few reports infection, immune deficiency, severe spinal deformity, severe demonstrating that the combination of femoral and sciatic nerve blocks (FSNBs) can provide adequate analgesia and muscle decompensated hypovolemia and shock. Moreover, factors relaxation during total knee replacement. We experienced a case associated with technically difficult neuraxial blocks influence of successful FSNBs for a total knee replacement in a 66 year-old the anesthesiologist’s decision to perform the procedure [1]. In female patient who had a previous cancelled surgery due to a failed tracheal intubation followed by a difficult mask ventilation for 50 these cases, peripheral nerve block can provide a good solution minutes, 3 days before these blocks. FSNBs were performed with for operations on a lower extremity. The combination of 50 ml of 1.5% mepivacaine because she had conditions precluding femoral and sciatic nerve blocks (FSNBs) has frequently been neuraxial blocks including a long distance from the skin to the used for postoperative pain control after total knee replacement epidural space related to a high body mass index and nonpalpable lumbar spinous processes. -

LECTURE (SACRAL PLEXUS, SCIATIC NERVE and FEMORAL NERVE) Done By: Manar Al-Eid Reviewed By: Abdullah Alanazi
CNS-432 LECTURE (SACRAL PLEXUS, SCIATIC NERVE AND FEMORAL NERVE) Done by: Manar Al-Eid Reviewed by: Abdullah Alanazi If there is any mistake please feel free to contact us: [email protected] Both - Black Male Notes - BLUE Female Notes - GREEN Explanation and additional notes - ORANGE Very Important note - Red CNS-432 Objectives: By the end of the lecture, students should be able to: . Describe the formation of sacral plexus (site & root value). List the main branches of sacral plexus. Describe the course of the femoral & the sciatic nerves . List the motor and sensory distribution of femoral & sciatic nerves. Describe the effects of lesion of the femoral & the sciatic nerves (motor & sensory). CNS-432 The Mind Maps Lumber Plexus 1 Branches Iliohypogastric - obturator ilioinguinal Femoral Cutaneous branches Muscular branches to abdomen and lower limb 2 Sacral Plexus Branches Pudendal nerve. Pelvic Splanchnic Sciatic nerve (largest nerves nerve), divides into: Tibial and divides Fibular and divides into : into: Medial and lateral Deep peroneal Superficial planter nerves . peroneal CNS-432 Remember !! gastrocnemius Planter flexion – knee flexion. soleus Planter flexion Iliacus –sartorius- pectineus – Hip flexion psoas major Quadriceps femoris Knee extension Hamstring muscles Knee flexion and hip extension gracilis Hip flexion and aids in knee flexion *popliteal fossa structures (superficial to deep): 1-tibial nerve 2-popliteal vein 3-popliteal artery. *foot drop : planter flexed position Common peroneal nerve injury leads to Equinovarus Tibial nerve injury leads to Calcaneovalgus CNS-432 Lumbar Plexus Formation Ventral (anterior) rami of the upper 4 lumbar spinal nerves (L1,2,3 and L4). Site Within the substance of the psoas major muscle. -

A Study on Peroneus Longus Autograft for Anterior Cruciate Ligament Reconstruction
International Journal of Research in Medical Sciences Kumar VK et al. Int J Res Med Sci. 2020 Jan;8(1):183-188 www.msjonline.org pISSN 2320-6071 | eISSN 2320-6012 DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20195904 Original Research Article A study on peroneus longus autograft for anterior cruciate ligament reconstruction Kumar V. K.*, Narayanan S. K., Vishal R. B. Department of Orthopedics, Sree Gokulam Medical College and Research Foundation, Venjaramoodu, Trivandrum, Kerala, India Received: 20 October 2019 Revised: 20 November 2019 Accepted: 02 December 2019 *Correspondence: Dr. Kumar V. K., E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: To compare the clinical outcome and donor site morbidity of ACL reconstruction with Peroneus longus tendon autografts in patients with isolated ACL injury. Methods: This was a prospective study that included patients who underwent ACL reconstruction using Peroneus longus tendon autograft. Results were assessed via physical examination. Donor site morbidity of the foot and ankle after tendon harvesting was assessed using Medical Research Council (MRC) grading of ankle and foot movements. Post-operative knee function was evaluated by the International Knee Documentation Committee (IKDC) scoring. Results: In this study sample of 25 patients, the ankle functions at the donor site are grossly preserved in almost all the patients, which was elucidated by grading the power of foot eversion. -
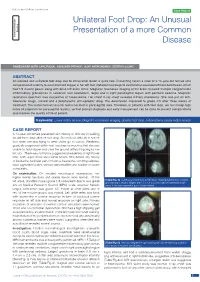
Unilateral Foot Drop: an Unusual Presentation of a More Common
DOI: 10.7860/JCDR/2017/26249.10738 Case Report Unilateral Foot Drop: An Unusual Section Presentation of a more Common Internal Medicine Disease RAMESHWAR NATH CHAURASIA1, ABHISHEK PathaK2, VIJAY nath MISHRA3, DEEPIKA JOSHI4 ABSTRACT An isolated and unilateral foot drop due to intracranial lesion is quite rare. Presenting herein a case of a 14-year-old female who complained of inability to wear and hold slipper in her left foot. Detailed neurological examination revealed left foot dorsiflexion which had 1/5 muscle power along with brisk left ankle reflex. Magnetic resonance imaging of the brain revealed multiple conglomerate inflammatory granulomas in cerebrum and cerebellum, larger one in right parasagittal region with perifocal oedema. Magnetic resonance spectrum was suggestive of tuberculoma. Her chest X-ray chest revealed milliary shadowing. She was put on anti- tubercular drugs, steroid and a prophylactic anti-epileptic drug. The dorsiflexion improved to grade 4/5 after three weeks of treatment. The motor homunculus for foot is located in parasagittal area. Therefore, in patients with foot drop, we must keep high index of suspicion for parasagittal lesions, so that prompt diagnosis and early management can be done to prevent complications and improve the quality of life of patient. Keywords: Lower motor neuron, Magnetic resonance imaging, Spastic foot drop, Tuberculoma, Upper motor neuron CASE REPORT A 14-year-old female presented with history of difficulty in walking for last three days after left foot drop. She noticed difficulty in her left foot when she was trying to wear shoes go to school. Weakness gradually progressed within next two days so much so that she was unable to hold slipper and clear the ground without tripping by her left foot.