Differential Guide for Sports and Exercise Medicine
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Prevention of Traumatic Corneal Ulcer in South East Asia
FROM OUR SOUTH ASIA EDITION Prevention of traumatic corneal ulcer in South East Asia S C AE Srinivasan/ (c)M Country Principal Investigator and Lead Principal Investigator with village health workers in Bhutan Dr. M. Srinivasan ciasis, and leprosy, are declining, and (VVHW) of the Government were utilized Director Emeritus, Aravind Eye Care, soon the majority of corneal blindness will to identify ocular injury and treat corneal Madurai, Tamil Nadu India. be due to microbial keratitis. Most abrasion corneal ulcers occur among agricultural Myanmar: Village Health Workers (VHW) workers in developing countries following of the health department Introduction corneal abrasion. India: paid village volunteers were utilized Corneal ulceration is a leading cause of Several non-randomized prevention visual impairment globally, with a dispro- studies conducted before 2000 Inclusion criteria 2 portionate burden in developing (Bhaktapur Eye Study) and during 2002 • Resident of study area countries. It was estimated that 6 million to 2004 in India, Myanmar, and Bhutan • Corneal abrasion after ocular injury, corneal ulcers occur annually in the ten by World Health Organization(WHO), have confirmed by clinical examination with countries of South East Asia Region suggested that antibiotic ointment fluorescein stain and a blue torch encompassing a total population of 1.6 applied promptly after a corneal abrasion • Reported within 48 hours of the injury billion.1 While antimicrobial treatment is could lower the incidence of ulcers, • Subject aged >5 years of age generally effective in treating infection, relative to neighbouring or historic “successful” treatment is often controls.3-4 Prevention of traumatic Exclusion criteria associated with a poor visual outcome. -

Fractures Fractura Pathologica
Fractures Fractura pathologica Myeloma Fractura traumatica Fractura aperta/clausa Fractura simplex/multiplex Fractura comminutiva Fractura transversa/obliqua Fractura spiralis/longitudinalis Fractura compressiva/impressiva Fractura incuneata Infractio = f. partialis = f. incompleta Fractura cum dislocatione ad axim ad latus ad longitudinem cum contractione ad longitudinem cum distractione AO ClassificationAuthentic reports of fractures : 2 S 4220 Fractura colli chirurgici humeri l. dx. comminutiva AO 11-C3 Fracture Healing: 1: REPOSITIO = REDUCTIO fragmentorum CLOSED (short /long term) Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum PLASTER CAST INTERNAL FIXATION Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum INTERNAL FIXATION Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum Name the type of fracture A B C D E F Choose a bone and break it. Try to write as much detailed diagnosis as possible. Authentic reports :1 collement = severe damage of soft tissues Authentic reports :2 Fr. aperta TSCHERNE I - open fracture with small skin injury without its contusion - negligible bacterial contamination Profesor Dr. Harald Tscherne (1933), Traumatology Clinic, Hannover: Classification of fractures published in 1982, T. divides fracture into open and closed. The most important for him is the degree of the soft tissues damage. Authentic reports :3 1 A 45-year-old woman presented with a 3-month history of generalized body pains nonresponsive to analgesic agents. Along with low back pain, she had progressive difficulty in getting up from sitting and supine positions and in walking. There was no history of trauma or any medication intake. She is an orthodox believer who wears a black veil outdoors and is completely covered, with little exposure to the sun. An anteroposterior radio- graph of the pelvis showed an undisplaced transverse fracture of the shaft of both femurs. -

Biomechanical Comparison of Fixation Stability Using a Lisfranc Plate
Foot and Ankle Surgery 25 (2019) 71–78 Contents lists available at ScienceDirect Foot and Ankle Surgery journa l homepage: www.elsevier.com/locate/fas Biomechanical comparison of fixation stability using a Lisfranc plate $ versus transarticular screws a,b a,c, d d Nathan C. Ho , Sophia N. Sangiorgio *, Spenser Cassinelli , Stephen Shymon , d a,b a,c d John Fleming , Virat Agrawal , Edward Ebramzadeh , Thomas G. Harris a The J. Vernon Luck, Sr., M.D. Orthopaedic Research Center, Orthopaedic Institute for Children, in Alliance with UCLA, 403 W. Adams Blvd., Los Angeles, CA 90007, United States b University of Southern California Department of Biomedical Engineering, Los Angeles, CA, United States c University of California, Los Angeles Department of Orthopaedic Surgery, Los Angeles, CA, United States d Los Angeles County Harbor—UCLA Medical Center, Los Angeles, CA, United States A R T I C L E I N F O A B S T R A C T Article history: Background: To obtain adequate fixation in treating Lisfranc soft tissue injuries, the joint is commonly Received 3 March 2017 stabilized using multiple transarticular screws; however iatrogenic injury is a concern. Alternatively, two Received in revised form 28 July 2017 parallel, longitudinally placed plates, can be used to stabilize the 1st and 2nd tarsometatarsal joints; Accepted 8 August 2017 however this may not provide adequate stability along the Lisfranc ligament. Several biomechanical studies have comparedearliermethodsoffixation using platestothestandardtransarticularscrew fixationmethod, Keywords: highlighting the potential issue of transverse stability using plates. A novel dorsal plate is introduced, Lisfranc injury intended to provide transverse and longitudinal stability, without injury to the articular cartilage. -
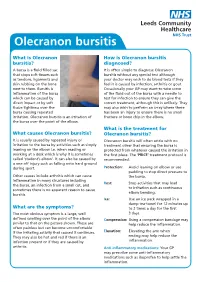
Olecranon Bursitis
Olecranon bursitis What is Olecranon How is Olecranon bursitis bursitis? diagnosed? A bursa is a fluid filled sac It is often simple to diagnose Olecranon that stops soft tissues such bursitis without any special test although as tendons, ligaments and your doctor may wish to do blood tests if they skin rubbing on the bone feel it is caused by infection, arthritis or gout. next to them. Bursitis is Occasionally your GP may want to take some inflammation of the bursa of the fluid out of the bursa with a needle to which can be caused by test for infection to ensure they can give the direct impact or by soft correct treatment, although this is unlikely. They tissue tightness over the may also wish to perform an x-ray where there bursa causing repeated has been an injury to ensure there is no small irritation. Olecranon bursitis is an irritation of fracture or bone chip in the elbow. the bursa over the point of the elbow. What is the treatment for What causes Olecranon bursitis? Olecranon bursitis? It is usually caused by repeated injury or Olecranon bursitis will often settle with no irritation to the bursa by activities such as simply treatment other that ensuring the bursa is leaning on the elbow i.e. when reading or protected from whatever caused the irritation in working at a desk which is why it is sometimes the first place. The ‘PRICE’ treatment protocol is called ‘student’s elbow’. It can also be caused by recommended: a one off injury such as falling onto hard ground during sport. -

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

OES Site Color Scheme 1
Nuisance Problems You will Grow to Love Thomas V Gocke, MS, ATC, PA-C, DFAAPA President & Founder Orthopaedic Educational Services, Inc. Boone, NC [email protected] www.orthoedu.com Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Faculty Disclosures • Orthopaedic Educational Services, Inc. Financial Intellectual Property No off label product discussions American Academy of Physician Assistants Financial PA Course Director, PA’s Guide to the MSK Galaxy Urgent Care Association of America Financial Intellectual Property Faculty, MSK Workshops Ferring Pharmaceuticals Consultant Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. 2 LEARNING GOALS At the end of this sessions you will be able to: • Recognize nuisance conditions in the Upper Extremity • Recognize nuisance conditions in the Lower Extremity • Recognize common Pediatric Musculoskeletal nuisance problems • Recognize Radiographic changes associates with common MSK nuisance problems • Initiate treatment plans for a variety of MSK nuisance conditions Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Inflammatory Response Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Inflammatory Response* When does the Inflammatory response occur: • occurs when injury/infection triggers a non-specific immune response • causes proliferation of leukocytes and increase in blood flow secondary to trauma • increased blood flow brings polymorph-nuclear leukocytes (which facilitate removal of the injured cells/tissues), macrophages, and plasma proteins to injured tissues *Knight KL, Pain and Pain relief during Cryotherapy: Cryotherapy: Theory, Technique and Physiology, 1st edition, Chattanooga Corporation, Chattanooga, TN 1985, p 127-137 Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. -

ICD-10 Diagnoses on Router
L ARTHRITIS R L HAND R L ANKLE R L FRACTURES R OSTEOARTHRITIS: PRIMARY, 2°, POST TRAUMA, POST _____ CONTUSION ACHILLES TEN DYSFUNCTION/TENDINITIS/RUPTURE FLXR TEN CLAVICLE: STERNAL END, SHAFT, ACROMIAL END CRYSTALLINE ARTHRITIS: GOUT: IDIOPATHIC, LEAD, CRUSH INJURY AMPUTATION TRAUMATIC LEVEL SCAPULA: ACROMION, BODY, CORACOID, GLENOID DRUG, RENAL, OTHER DUPUYTREN’S CONTUSION PROXIMAL HUMERUS: SURGICAL NECK 2 PART 3 PART 4 PART CRYSTALLINE ARTHRITIS: PSEUDOGOUT: HYDROXY LACERATION: DESCRIBE STRUCTURE CRUSH INJURY PROXIMAL HUMERUS: GREATER TUBEROSITY, LESSER TUBEROSITY DEP DIS, CHONDROCALCINOSIS LIGAMENT DISORDERS EFFUSION HUMERAL SHAFT INFLAMMATORY: RA: SEROPOSITIVE, SERONEGATIVE, JUVENILE OSTEOARTHRITIS PRIMARY/SECONDARY TYPE _____ LOOSE BODY HUMERUS DISTAL: SUPRACONDYLAR INTERCONDYLAR REACTIVE: SECONDARY TO: INFECTION ELSEWHERE, EXTENSION OR NONE INTESTINAL BYPASS, POST DYSENTERIC, POST IMMUNIZATION PAIN OCD TALUS HUMERUS DISTAL: TRANSCONDYLAR NEUROPATHIC CHARCOT SPRAIN HAND: JOINT? OSTEOARTHRITIS PRIMARY/SECONDARY TYPE _____ HUMERUS DISTAL: EPICONDYLE LATERAL OR MEDIAL AVULSION INFECT: PYOGENIC: STAPH, STREP, PNEUMO, OTHER BACT TENDON RUPTURES: EXTENSOR OR FLEXOR PAIN HUMERUS DISTAL: CONDYLE MEDIAL OR LATERAL INFECTIOUS: NONPYOGENIC: LYME, GONOCOCCAL, TB TENOSYNOVITIS SPRAIN, ANKLE, CALCANEOFIBULAR ELBOW: RADIUS: HEAD NECK OSTEONECROSIS: IDIOPATHIC, DRUG INDUCED, SPRAIN, ANKLE, DELTOID POST TRAUMATIC, OTHER CAUSE SPRAIN, ANKLE, TIB-FIB LIGAMENT (HIGH ANKLE) ELBOW: OLECRANON WITH OR WITHOUT INTRA ARTICULAR EXTENSION SUBLUXATION OF ANKLE, -

Mandibular Fractures, Diagnostics, Postoperative Complications
Journal of Medical Sciences. March 23, 2020 - Volume 8 | Issue 13. Electronic-ISSN: 2345-0592 Medical Sciences 2020 Vol. 8 (13), p. 45-52 e-ISSN: 2345-0592 Medical Sciences Online issue Indexed in Index Copernicus Official website: www.medicsciences.com Mandibular fractures, diagnostics, postoperative complications Shahaf Givony1 1 Lithuanian University of Health Sciences. Academy of Medicine. Faculty of Odonthology. ABSTRACT Mandibular fractures usually happen among young males at the age of 16-30 years old. The mandible which has been rated as the second facial bone with the highest rate of injuries, tends to break much more often compared to any other bone of the cranium and represent up to 70% of the cases. This tendency to fracture may be explained by the protruded position, mobility and particular shape of it. The tendency for a mandibular fracture may also be explained by the common risk factors such as vehicle accidents and physical violence that are part of our daily life. There are many other risk factors according to the literature which differ between individuals due to the different socio-economic status, culture, technology and environment. Before the clinical examination of the fracture, it is obligatory to make sure that a clear airway path presents with no other fatal injuries. The examination may be supported by imaging methods which together will approve the diagnosis and method of treatment. Patients with a fracture of the mandible may suffer from post-operative complications which may occur after a short or long duration of the treatment. Those complications may be malocclusion, infections, trismus, damaged teeth and soft tissue, esthetic disfiguration, functional problems, pain and many more. -

CASE REPORT Injuries Following Segway Personal
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature Permalink https://escholarship.org/uc/item/37r4387d Journal Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health, 16(5) ISSN 1936-900X Authors Ashurst, John Wagner, Benjamin Publication Date 2015 DOI 10.5811/westjem.2015.7.26549 License https://creativecommons.org/licenses/by/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California CASE REPORT Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature John Ashurst DO, MSc Conemaugh Memorial Medical Center, Department of Emergency Medicine, Benjamin Wagner, DO Johnstown, Pennsylvania Section Editor: Rick A. McPheeters, DO Submission history: Submitted April 20, 2015; Accepted July 9, 2015 Electronically published October 20, 2015 Full text available through open access at http://escholarship.org/uc/uciem_westjem DOI: 10.5811/westjem.2015.7.26549 The Segway® self-balancing personal transporter has been used as a means of transport for sightseeing tourists, military, police and emergency medical personnel. Only recently have reports been published about serious injuries that have been sustained while operating this device. This case describes a 67-year-old male who sustained an oblique fracture of the shaft of the femur while using the Segway® for transportation around his community. We also present a review of the literature. [West J Emerg Med. 2015;16(5):693-695.] INTRODUCTION no parasthesia was noted. In 2001, Dean Kamen developed a self-balancing, zero Radiograph of the right femur demonstrated an oblique emissions personal transportation vehicle, known as the fracture of the proximal shaft of the femur with severe Segway® Personal Transporter (PT).1 The Segway’s® top displacement and angulation (Figure). -

Pes Anserine Bursitis
BRIGHAM AND WOMEN’S HOSPITAL Department of Rehabilitation Services Physical Therapy Standard of Care: Pes Anserine Bursitis ICD 9 Codes: 726.61 Case Type / Diagnosis: The pes anserine bursa lies behind the medial hamstring, which is composed of the tendons of the sartorius, gracilis and semitendinosus (SGT) muscles. Because these 3 tendons splay out on the anterior aspect of the tibia and give the appearance of the foot of a goose, pes anserine bursitis is also known as goosefoot bursitis.1 These muscles provide for medial stabilization of the knee by acting as a restraint to excessive valgus opening. They also provide a counter-rotary torque function to the knee joint. The pes anserine has an eccentric role during the screw-home mechanism that dampens the effect of excessively forceful lateral rotation that may accompany terminal knee extension.2 Pes anserine bursitis presents as pain, tenderness and swelling over the anteromedial aspect of the knee, 4 to 5 cm below the joint line.3 Pain increases with knee flexion, exercise and/or stair climbing. Inflammation of this bursa is common in overweight, middle-aged women, and may be associated with osteoarthritis of the knee. It also occurs in athletes engaged in activities such as running, basketball, and racquet sports.3 Other risk factors include: 1 • Incorrect training techniques, or changes in terrain and/or distanced run • Lack of flexibility in hamstring muscles • Lack of knee extension • Patellar malalignment Indications for Treatment: • Knee Pain • Knee edema • Decreased active and /or passive ROM of lower extremities • Biomechanical dysfunction lower extremities • Muscle imbalances • Impaired muscle performance (focal weakness or general conditioning) • Impaired function Contraindications: • Patients with active signs/symptoms of infection (fever, chills, prolonged and obvious redness or swelling at hip joint). -

Pattern of Skeletal Injuries in Child Physical Abuse
1 Bahrain Medical Bulletin, Vol. 33, No. 2, June 2011 Pattern of Skeletal Injuries in Physically Abused Children Fadheela Al-Mahroos, MD, MHPE* Eshraq A Al-Amer, MD, ABMS (Ped)** Nabar J Umesh, MD, DMRE*** Ali I Alekri, FRCSI, CABS (Ortho)**** Objective: The aim of this study is to identify the frequency and patterns of skeletal injuries among victims of child abuse in Bahrain. Design: Retrospective. Setting: Child Protection Unit at Salmaniya Medical Complex. Method: Child’s characteristics, type of skeletal injuries, location, pattern, radiological findings, and associated other injuries of 36 children were reviewed. Data management and analysis was done using SPSS for Windows, version 18. Result: Thirty-six children with skeletal injuries resulting from child physical abuse were seen from 1991 to 2009. Twenty-three (64%) were males and 13 (36%) were females; the mean age was 3.8 years. Twenty-three (64%) were ≤ 3 years old. Multiple fractures were documented in 19 (53%) children. Bone fracture types and frequency were as follow: 10 (28%) affecting the femur, 9 (25%) skull, 8 (22%) humerus, 6 (17%) rib, 4 (11%) radius, 4 (11%) ulna and 2 (6%) tibia. Other bones less frequently affected were mandible, nasal bone, vertebral, metatarsals, and calcaneus fractures. In addition, other injuries included slipped femoral epiphysis, large bilateral hematoma in vastus lateralis, and full thickness tendon Achilles tear. Hundred percent of rib, ulnar, radial and tibial fractures were in children under one year old. In addition, 7 (78%) of skull fractures, 5 (62%) of humerus fractures, and 5 (50) of femur fractures were under one year old. -

Pediatric MSK Protocols
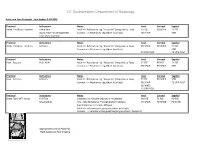
UT Southwestern Department of Radiology Ankle and Foot Protocols - Last Update 5-18-2015 Protocol Indications Notes Axial Coronal Sagittal Ankle / Midfoot - Routine Ankle Pain Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD SPAIR T1 FSE Injury, Internal Derangement Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR STIR Talar OCD, Coalition Protocol Indications Notes Axial Coronal Sagittal Ankle / Midfoot - Arthritis Arthritis Axial = In Relation to Leg "Footprint" (Long Axis to Foot) PD SPAIR PD SPAIR T1 FSE Coronal = In Relation to Leg (Short Axis Foot) STIR T1 SPIR POST T1 SPIR POST Protocol Indications Notes Axial Coronal Sagittal Foot - Routine Pain, AVN Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD FSE T1 FSE Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR PD SPAIR STIR Protocol Indications Notes Axial Coronal Sagittal Foot - Arthritis Arthritis Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD SPAIR STIR Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR T1 SPIR POST 3D WATS T1 SPIR POST Protocol Indications Notes Axial Coronal Sagittal Great Toe / MTP Joints Turf Toe Smallest Coil Possible (Microcoil if Available) PD FSE T1 FSE PD FSE Sesamoiditis FoV = Mid Metatarsal Through Distal Phalanges PD SPAIR PD SPAIR PD SPAIR Slice thickness = 2-3 mm, 10% gap Axial = In relation to the great toe (short axis foot) Coronal = In relation to the great toe (long axis foot / footprint) Appropriate Coronal Plane for Both Ankle and Foot Imaging UT Southwestern Department