Common Procedures in IR Kristiann Kinsman MD Disclosures
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Gastrostomy Feeding Tubes
Gastrostomy feeding tubes With Dr Anastasia Volovets, Gastroenterologist and Hepatologist, Royal Prince Alfred Hospital, Sydney, Australia Introduction In patients with prolonged inadequate or absent oral intake gastrostomy tubes can be used to provide a route for enteral feeding, hydration, and medication administration. Case 1 - You are a junior doctor on the wards and you’re called to see a 65 year old male, who is day 5 post- stroke with an impaired swallow he is unable to tolerate oral feed and his family is worried he will starve to death. 1. Management of this patient IV fluids do not provide the caloric support or nutrients needed by patients, after 48 hours of impaired oral feeding, enteral feeding should be considered. • Short term this would be a nasogastric tube • Longer term (greater than 6 weeks) a gastrostomy or jejunostomy should be considered 2. Indications for enteral feeding • Neurological disorders causing impaired swallowing and aspiration of food o Stroke (most common) o Traumatic brain injury o Parkinson’s disease • Structural problems o Malignancy obstructing the gastrointestinal tract, this can include upper GI, head, nose or throat. Gastrostomy insertion can be done prophylactically prior to treatment that will impair the functioning or path of the tract such as surgery or radiotherapy 3. Contraindications to gastric feeding tubes • Absolute o High bleeding risk - uncorrected coagulopathy, thrombocytopenia o Chronic liver disease - varies and ascites o Peritonitis or abdominal perforation o Cellulitis at selected -

Pancreaticogastrostomy
eCommons@AKU Section of General Surgery Department of Surgery October 2017 Pancreaticogastrostomy - an alternate for dealing with pancreatic remnant after pancreaticoduodenectomy - experience from a tertiary care center of Pakistan Tabish Chawla Aga Khan University, [email protected] Hassaan Bari Aga Khan University Shahrukh Effendi Follow this and additional works at: https://ecommons.aku.edu/pakistan_fhs_mc_surg_gen Part of the Surgery Commons Recommended Citation Chawla, T., Bari, H., Effendi, S. (2017). Pancreaticogastrostomy - an alternate for dealing with pancreatic remnant after pancreaticoduodenectomy - experience from a tertiary care center of Pakistan. Journal of Pakistan Medical Association, 67(10), 1621-1624. Available at: https://ecommons.aku.edu/pakistan_fhs_mc_surg_gen/76 1621 CASE SERIES Pancreaticogastrostomy — an alternate for dealing with pancreatic remnant after pancreaticoduodenectomy — experience from a tertiary care center of Pakistan Tabish Chawla, Hassaan Bari, Shahrukh Effendi Abstract as part of PD. Therefore it was associated with high Whipple's pancreaticoduodenectomy has been refined morbidity and mortality resulting from high rates of over the years to be a safe operation though the leakage from pancreatic stump. morbidity rate still remains high (30-50%). Pancreatic Pancreatcogastrostomy is a repopularized technique fistula is the most important cause of mortality which has been described previously in literature. 3 This following pancreaticoduodenectomy. To prevent it, study was done to review the experience of PG being surgeons have used two anastomotic techniques: done as an alternate to PJ after PD. pancreaticojejunostomy and pancreaticogastrostomy. Recent studies found that pancreaticogastrostomy is Material and Methods associated with fewer overall complications than It is a case series collected at the Department of Surgery of pancreaticojejunostomy. -

High Risk Percutaneous Endoscopic Gastrostomy Tubes: Issues to Consider
NUTRITIONINFLAMMATORY ISSUES BOWEL IN GASTROENTEROLOGY, DISEASE: A PRACTICAL SERIES APPROACH, #105 SERIES #73 Carol Rees Parrish, M.S., R.D., Series Editor High Risk Percutaneous Endoscopic Gastrostomy Tubes: Issues to Consider Iris Vance Neeral Shah Percutaneous endoscopy gastrostomy (PEG) tubes are a valuable tool for providing long- term enteral nutrition or gastric decompression; certain circumstances that complicate PEG placement warrant novel approaches and merit review and discussion. Ascites and portal hypertension with varices have been associated with poorer outcomes. Bleeding is one of the most common serious complications affecting approximately 2.5% of all procedures. This article will review what evidence exists in these high risk scenarios and attempt to provide more clarity when considering these challenging clinical circumstances. INTRODUCTION ince the first Percutaneous Endoscopic has been found by multiple authors to portend a poor Gastrostomy tube was placed in 1979 (1), they prognosis in PEG placement (3,4, 5,6,7,8). This review Shave become an invaluable tool for providing will endeavor to provide more clarity when considering long-term enteral nutrition (EN) and are commonly used these challenging clinical circumstances. in patients with dysphagia following stroke, disabling motor neuron diseases such as multiple sclerosis and Ascites & Gastric Varices amyotrophic lateral sclerosis, and in those with head The presence of ascites is frequently viewed as a and neck cancer.They are also used for patients with relative, if not absolute, contraindication to PEG prolonged mechanical intubation, as well as gastric placement. Ascites adds technical difficulties and the decompression in those with severe gastroparesis, risk for potential complications (see Table 1). -
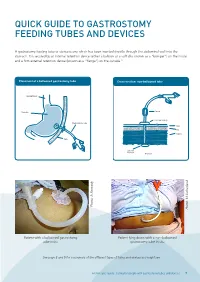
Quick Guide to Gastrostomy Feeding Tubes and Devices
QUICK GUIDE TO GASTROSTOMY FEEDING TUBES AND DEVICES A gastrostomy feeding tube or device is one which has been inserted directly through the abdominal wall into the stomach. It is secured by an internal retention device (either a balloon or a soft disc known as a “bumper”) on the inside and a firm external retention device (known as a “flange”) on the outside.11 Placement of a ballooned gastrostomy tube Cross-section: non-ballooned tube Oesophagus Stomach Clamp External Flange Gastrostomy tube Skin Fat Muscle Skin Internal Bumper Stomach Photo: APhoto: Kennedy Photo: MPhoto: Sutherland Patient with a ballooned gastrostomy Patient lying down with a non-ballooned tube insitu gastrostomy tube in situ See page 8 and 9 for a summary of the different types of tubes and devices you might see. A Clinician’s Guide: Caring for people with gastrostomy tubes and devices 7 Common features of gastrostomy feeding tubes and devices include, but are not limited to: Refer to manufacturer’s guidelines for advice on brand specific tube and device features Ballooned Gastrostomy Tube Ballooned Gastrostomy Tube With side port Without side port Feeding Port Feeding Port (Enteral Dispenser (Enteral Dispenser and Feed Bag and Feed Bag connect here) connect here) ml/cc Balloon Port Balloon Port ml/cc Side Port (X ml/cc) (X ml/cc) French (size) [For example:16/18/20] French (size) [For example:16/18/20] FR FR cm markings cm markings External External Flange Flange Balloon Balloon Non-ballooned Gastrostomy Tube Non-ballooned Gastrostomy Tube with collapsible internal -

Canadian Surgery Forum Canadien De Chirurgie
Vol. 44, Suppl., August / août 2001 ISSN 0008-428X ABSTRACTS RÉSUMÉS of presentations to the des communications présentées Annual Meetings of the aux congrès annuels de la Canadian Society of Colon Société canadienne and Rectal Surgeons des chirurgiens du côlon et du rectum Canadian Association of General Surgeons Association canadienne des chirurgiens généraux Canadian Association of Thoracic Surgeons Association canadienne des chirurgiens thoraciques CANADIAN SURGERY FORUM CANADIEN DE CHIRURGIE Québec, QC September 6 to 9, 2001 Québec (QC) du 6 au 9 septembre 2001 Abstracts Résumés Canadian Surgery Forum canadien de chirurgie 2001 Canadian Society of Colon and Rectal Surgeons Société canadienne des chirurgiens du côlon et du rectum 1 2 ARTIFICIAL BOWEL SPHINCTER IMPLANTATION COMPARISON OF DELORME AND ALTEMEIER IN THE MANAGEMENT OF SEVERE FECAL IN- PROCEDURES FOR RECTAL PROLAPSE. E.C. McKe- CONTINENCE — EXPERIENCE FROM A SINGLE vitt, B.J. Sullivan, P.T. Phang. Department of Surgery, St. INSTITUTION. A.R. MacLean, G. Stewart, K. Sabr, M. Paul’s Hospital, University of British Columbia, Vancou- Burnstein. Department of Surgery, St Michael’s Hospital, ver, BC University of Toronto, Toronto, Ont. We wish to compare the outcomes of 2 perineal operations for The purpose of this study was to evaluate the safety and effi- rectal prolapse: rectal mucosectomy (Delorme’s operation) cacy of artificial bowel sphincter (ABS) implantation in the and perineal rectosigmoidectomy (Altemeier’s operation). management of severe fecal incontinence (FI). We reviewed all 34 patients who had a perineal repair of Ten patients (6 males), with a mean age of 40.6 years, un- rectal prolapse at our hospital from July 1997 to June 2000. -

The Place of Laparoscopic Gastrostomy in the Surgical Armamentarium
6 The Place of Laparoscopic Gastrostomy in the Surgical Armamentarium Philip Ng Cheng Hin Department Of Surgery, University Hospital Lewisham, London UK 1. Introduction Historically, gastrostomy has been performed for centuries and recently with the advent of Laparoscopic surgery, laparoscopic gastrostomy (ref 1) has been added to the options available to surgeons. Laparoscopic gastrostomy can be considered when other minimally invasive methods such as PEG (Percutaneous Endoscopic Gastrostomy) is not feasible or fails. PEG can be come impossible if the endoscope cannot be introduced, because of physical or functional obstruction. The alternative is to consider PRG (Percutaneous Radiologically Guided) insertion prior to considering open gastrostomy via laparotomy, (LG) Laparoscopic gastrostomy has carved itself an important niche in that respect. 2. Indications of gastrostomy a. Patients requiring Medium or long term feeding - Starvation - Swallowing problems, long term neurological conditions - Chronic problems in children e.g. mucoviscidosis, reflux - Impassable benign or malignant stricture b. Decompression of the stomach c. Gastric access d. Failure of PEG e. Failure of PRG 3. Contra indications a. Unfit patients who cannot lie flat. b. Abdominal access not possible due to previous operations or gross obesity, fixed flexion deformity. 4. Techniques a. Double puncture laparoscopic assisted gastrostomy (ref 2, 4) Once the abdomen prepped, entry into the peritoneal cavity is performed using any preferred technique through a periumbilical port and the pneumoperitoneum is www.intechopen.com 84 Gastrostomy established, the anterior wall of the stomach is identified with certainty, and a second port (10mm) is inserted at a convenient point on the anterior abdominal wall. This operative step is greatly assisted by changing the position of the operating table 20 degrees head up. -

Gastrostomy Allows Removal of Obstructive Pancreatic Duct Stones
Original article Antegrade pancreatoscopy via EUS-guided pancreatico- gastrostomy allows removal of obstructive pancreatic duct stones Authors Theodore W. James, Todd H. Baron Institution pancreaticolithiasis, including use of pancreatoscopy for in- Division of Gastroenterology and Hepatology, University of traductal electrohydraulic lithotripsy (IEHL). Pancreatosco- North Carolina, Chapel Hill, North Carolina, United States py is often limited by a small-caliber downstream pancreat- ic duct as well as an unstable pancreatoscope position submitted 8.3.2018 within the pancreatic head. Endoscopic ultrasound-guided accepted after revision 11.4.2018 pancreaticogastrostomy (EUS-PG) has been developed as a method to relieve ductal obstruction when retrograde ac- Bibliography cess fails. The current study describes pancreatoscopy via DOI https://doi.org/10.1055/a-0607-2484 | EUS-PG, a novel method for managing obstructing pancrea- Endoscopy International Open 2018; 06: E735–E738 ticolithiasis. © Georg Thieme Verlag KG Stuttgart · New York Patients and methods From September 2017 to January ISSN 2364-3722 2018, patients who underwent EUS-PG followed by ante- grade pancreatoscopy via PG were identified. Endoscopy re- Corresponding author ports, medical charts and relevant laboratory data were re- Todd Huntley Baron, MD, Division of Gastroenterology and viewed and recorded. Hepatology, University of North Carolina School of Results Five patients underwent EUS-PG and antegrade Medicine, 101 Manning Drive, Chapel Hill, NC 27599 pancreatoscopy via PG during the study period; clinical suc- Fax: +1-984-974-0744 cess rate was 100%. There were no significant adverse [email protected] events during the procedure or follow up period. Conclusions Pancreatoscopy via PG for IEHL is safe and ef- fective for treating obstructing pancreaticolithiasis in pa- ABSTRACT tients who have previously failed ERCP or in clinical scenar- Background and study aims Endoscopic retrograde cho- ios were ERCP is not possible. -

Laparoscopic Intracorporeal Pancreaticogastrostomy in Total Laparoscopic Pancreaticoduodenectomy—A Novel Anastomotic Technique
Indian Journal of Surgical Oncology (June 2019) 10(2):274–279 https://doi.org/10.1007/s13193-018-0829-4 ORIGINAL ARTICLE Laparoscopic Intracorporeal Pancreaticogastrostomy in Total Laparoscopic Pancreaticoduodenectomy—A Novel Anastomotic Technique Shailesh P. Puntambekar1 & Mehul J. Mehta1 & Manoj M. Manchekar1 & Mihir Chitale1 & Mangesh Panse1 & Advait Jathar1 & Rohan Umalkar1 Received: 8 March 2018 /Accepted: 13 November 2018 /Published online: 2 January 2019 # Indian Association of Surgical Oncology 2019 Abstract Novel pancreaticogastric anastomosis technique in laparoscopic pancreaticoduodenectomy which is simple, feasible to perform, provides secure fixation between stomach and pancreas. The aim of our article is to describe our technique of intracorporeal pancreaticogastrostomy as a promising approach for future widespread application. Keywords PD-pancreaticoduocenectomy . PJ-pancreaticojejunostomy . PG-pancreaticogastrostomy Introduction aim of our article is to describe our technique of intracorporeal pancreaticogastrostomy as a promising approach for future Laparoscopic pancreatic surgery has emerged as one of the widespread application. most advanced applications of minimal invasive surgery. Gagner and Pomp were the first to describe the laparoscopic pancreaticoduodenectomy in 1994. Prolonged operative time Methods and technical difficulty of pancreatic resection and reconstruc- tion procedures were the reasons for initial reluctance to ac- We have used our technique in five patients since May 2015 to cept the laparoscopic technique. Pancreatic anastomotic leak- March 2016. The inclusion criteria were medically fit, non- age carries an increased risk of intraabdominal haemorrhage obese patients with periampullary tumours and without any and high mortality rate. Many surgeons avoid intracorporeal previous abdominal surgery. Preoperatively, all patients were pancreatic reconstruction to increase the safety of anastomo- thoroughly evaluated for operability and resectability. -

The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute Cholecystitis with Gallbladder Perforation 담낭천공을 동반한 급성담낭염 환자에서 수술 전 경피적담낭배액술의 효용성에 관한 연구
Original Article pISSN 1738-2637 / eISSN 2288-2928 J Korean Soc Radiol 2017;77(6):372-381 https://doi.org/10.3348/jksr.2017.77.6.372 The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute Cholecystitis with Gallbladder Perforation 담낭천공을 동반한 급성담낭염 환자에서 수술 전 경피적담낭배액술의 효용성에 관한 연구 Bo Ra Kim, MD, Jeong-Hyun Jo, MD, Byeong-Ho Park, MD* Department of Radiology, Dong-A University Hospital, Dong-A University College of Medicine, Busan, Korea Purpose: Treatment of acute cholecystitis with gallbladder perforation remains Index terms controversial. We aimed to determine the feasibility of percutaneous cholecystosto- Cholecystostomy my (PC) in these patients. Cholecystitis, Acute Materials and Methods: We retrospectively reviewed patients who had acute Cholecystectomy cholecystitis with gallbladder perforation at a single institution. Group 1 (n = 27; M:F = 18:9; mean age, 69.9 years) consisted of patients who received PC followed Received May 12, 2017 by cholecystectomy, and group 2 (n = 16; M:F = 8:8; mean age 57.1 years) consisted Revised June 3, 2017 of patients who were treated with cholecystectomy only. Preoperative details, in- Accepted June 26, 2017 cluding sex, age, underlying medical history, signs of systemic inflammatory re- *Corresponding author: Byeong-Ho Park, MD Department of Radiology, Dong-A University Hospital, sponse syndrome (SIRS), laboratory findings, body mass index, presence of gallstone, Dong-A University College of Medicine, 26 Daesingong- and type of perforation; treatment-related variables, including laparoscopic or open won-ro, Seo-gu, Busan 49201, Korea. cholecystectomy, conversion to laparotomy, blood loss, surgical time and anesthesia Tel. 82-51-240-5371 Fax. -

Percutaneous Endoscopic Gastrostomy Versus Nasogastric Tube Feeding: Oropharyngeal Dysphagia Increases Risk for Pneumonia Requiring Hospital Admission
nutrients Article Percutaneous Endoscopic Gastrostomy versus Nasogastric Tube Feeding: Oropharyngeal Dysphagia Increases Risk for Pneumonia Requiring Hospital Admission Wei-Kuo Chang 1,*, Hsin-Hung Huang 1, Hsuan-Hwai Lin 1 and Chen-Liang Tsai 2 1 Division of Gastroenterology, Department of Internal Medicine, Tri-Service General Hospital, National Defense Medical Center, Taipei 114, Taiwan; [email protected] (H.-H.H.); [email protected] (H.-H.L.) 2 Division of Pulmonary and Critical Care, Department of Internal Medicine, Tri-Service General Hospital, National Defense Medical Center, Taipei 114, Taiwan; [email protected] * Correspondence: [email protected]; Tel.: +886-2-23657137; Fax: +886-2-87927138 Received: 3 November 2019; Accepted: 4 December 2019; Published: 5 December 2019 Abstract: Background: Aspiration pneumonia is the most common cause of death in patients with percutaneous endoscopic gastrostomy (PEG) and nasogastric tube (NGT) feeding. This study aimed to compare PEG versus NGT feeding regarding the risk of pneumonia, according to the severity of pooling secretions in the pharyngolaryngeal region. Methods: Patients were stratified by endoscopic observation of the pooling secretions in the pharyngolaryngeal region: control group (<25% pooling secretions filling the pyriform sinus), pharyngeal group (25–100% pooling secretions filling the pyriform sinus), and laryngeal group (pooling secretions entering the laryngeal vestibule). Demographic data, swallowing level scale score, and pneumonia requiring hospital admission were recorded. Results: Patients with NGT (n = 97) had a significantly higher incidence of pneumonia (episodes/person-years) than those patients with PEG (n = 130) in the pharyngeal group (3.6 1.0 ± vs. 2.3 2.1, P < 0.001) and the laryngeal group (3.8 0.5 vs. -

The Role of Interventional Radiology in the Management of Pancreatic Pathologies
Published online: 2020-01-10 THIEME Review Article 99 The Role of Interventional Radiology in the Management of Pancreatic Pathologies Ghali Salahia1 Sook Cheng Chin2 Ian Zealley2 Richard D. White1 1Department of Radiology, University Hospital of Wales, Cardiff, Address for correspondence Ghali Salahia, MD, MBA, Department United Kingdom of Radiology, University Hospital of Wales, Heath Park Way, Cardiff, 2Department of Radiology, Ninewells Hospital, Dundee, United CF14 4XW, United Kingdom (e-mail: [email protected]). Kingdom J Gastrointestinal Abdominal Radiol ISGAR 2020;3:99–114 Abstract Pancreatic pathologies are varied and wide-ranging, and a multidisciplinary approach is essential for effective diagnosis and management. We describe image-guided percutaneous (nonendoscopic) interventions in the management of pancreatic dis- ease, with emphasis on inflammatory and neoplastic pancreatic pathologies and on the transplanted pancreas. Image-guided treatments for the complications of pan- Keywords creatitis include percutaneous interventions on simple and complex peripancreatic ► interventional collections, pseudocysts, and fistulas. Vascular interventions predominantly focus on radiology the treatment of pseudoaneurysms, hemorrhagic pseudocysts, and arteriovenous ► pancreatic cancer malformations. Emerging ablative techniques for pancreatic cancer are promising ► pancreatic transplant and include percutaneous radiofrequency ablation, microwave ablation, irreversible ► pancreatitis electroporation, and electrochemotherapy. Image-guided -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular