Statistical Analysis Plan
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Sports Medicine Examination Outline
Sports Medicine Examination Content I. ROLE OF THE TEAM PHYSICIAN 1% A. Ethics B. Medical-Legal 1. Physician responsibility 2. Physician liability 3. Preparticipation clearance 4. Return to play 5. Waiver of liability C. Administrative Responsibilities II. BASIC SCIENCE OF SPORTS 16% A. Exercise Physiology 1. Training Response/Physical Conditioning a.Aerobic b. Anaerobic c. Resistance d. Flexibility 2. Environmental a. Heat b.Cold c. Altitude d.Recreational diving (scuba) 3. Muscle a. Contraction b. Lactate kinetics c. Delayed onset muscle soreness d. Fiber types 4. Neuroendocrine 5. Respiratory 6. Circulatory 7. Special populations a. Children b. Elderly c. Athletes with chronic disease d. Disabled athletes B. Anatomy 1. Head/Neck a.Bone b. Soft tissue c. Innervation d. Vascular 2. Chest/Abdomen a.Bone b. Soft tissue c. Innervation d. Vascular 3. Back a.Bone b. Soft tissue c. Innervation 1 d. Vascular 4. Shoulder/Upper arm a. Bone b. Soft tissue c. Innervation d. Vascular 5. Elbow/Forearm a. Bone b. Soft tissue c. Innervation d. Vascular 6. Hand/Wrist a. Bone b. Soft tissue c. Innervation d. Vascular 7. Hip/Pelvis/Thigh a. Bone b. Soft tissue c. Innervation d. Vascular 8. Knee a. Bone b. Soft tissue c. Innervation d. Vascular 9. Lower Leg/Foot/Ankle a. Bone b. Soft tissue c. Innervation d. Vascular 10. Immature Skeleton a. Physes b. Apophyses C. Biomechanics 1. Throwing/Overhead activities 2. Swimming 3. Gait/Running 4. Cycling 5. Jumping activities 6. Joint kinematics D. Pharmacology 1. Therapeutic Drugs a. Analgesics b. Antibiotics c. Antidiabetic agents d. Antihypertensives e. -

Surgical Treatment of Traumatic Cervical Facet Dislocation
DOI: 10.1590/0004-282X20160078 VIEW AND REVIEW Surgical treatment of traumatic cervical facet dislocation: anterior, posterior or combined approaches? Deslocamentos facetários cervicais traumáticos: abordagem anterior, posterior ou combinada? Catarina C. Lins1, Diego T. Prado2, Andrei F. Joaquim1,3 ABSTRACT Surgical treatment is well accepted for patients with traumatic cervical facet joint dislocations (CFD), but there is uncertainty over which approach is better: anterior, posterior or combined. We performed a systematic literature review to evaluate the indications for anterior and posterior approaches in the management of CFD. Anterior approaches can restore cervical lordosis, and cause less postoperative pain and less wound problems. Posterior approaches are useful for direct reduction of locked facet joints and provide stronger fixation from a biomechanical point of view. Combined approaches can be used in more complex cases. Although both anterior and posterior approaches can be used interchangeably, there are some patients who may benefit from one of them over the other, as discussed in this review. Surgeons who treat cervical spine trauma should be able to perform both procedures as well as combined approaches to adequately manage CFD and improve patients’ final outcomes. Keywords: spine; dislocations; bones fractures; surgery. RESUMO O tratamento dos deslocamentos facetários cervicais traumáticos (DFC) é preferencialmente cirúrgico, conforme a literatura pertinente, mas há dúvidas quanto a melhor forma de abordagem da coluna: anterior, posterior ou combinada. Realizamos revisão sistemática para avaliar as indicações da abordagem anterior e da posterior nos DFC. A abordagem anterior permite restaurar a lordose cervical, com menor dor no pós-operatório e menos problemas relacionados a ferida cirúrgica. -

S41598-020-78754-9.Pdf
www.nature.com/scientificreports OPEN Acromioclavicular and sternoclavicular joint dislocations indicate severe concomitant thoracic and upper extremity injuries in severely injured patients M. Sinan Bakir1,2*, Rolf Lefering3, Lyubomir Haralambiev1,2, Simon Kim1, Axel Ekkernkamp1,2, Denis Gümbel1,2 & Stefan Schulz‑Drost2,4,5 Preliminary studies show that clavicle fractures (CF) are known as an indicator in the severely injured for overall injury severity that are associated with relevant concomitant injuries in the thorax and upper extremity. In this regard, little data is available for the rarer injuries of the sternoclavicular and acromioclavicular joints (SCJ and ACJ, respectively). Our study will answer whether clavicular joint injuries (CJI), by analogy, have a similar relevance for the severely injured. We performed an analysis from the TraumaRegister DGU (TR‑DGU). The inclusion criterion was an Injury Severity Score (ISS) of at least 16. In the TR‑DGU, the CJI were registered as one entity. The CJI group was compared with the CF and control groups (those without any clavicular injuries). Concomitant injuries were distinguished using the Abbreviated Injury Scale according to their severity. The inclusion criteria were met by n = 114,595 patients. In the case of CJI, n = 1228 patients (1.1%) were found to be less severely injured than the controls in terms of overall injury severity. Compared to the CF group (n = 12,030; 10.5%) with higher ISS than the controls, CJI cannot be assumed as an indicator for a more severe trauma; however, CF can. Concomitant injuries were more common for severe thoracic and moderate upper extremity injuries than other body parts for CJI. -

Dislocation of the Proximal Tibiofibular Joint, Do Not Miss It
BMJ Case Reports: first published as 10.1136/bcr-2014-207875 on 1 December 2015. Downloaded from Rare disease CASE REPORT Dislocation of the proximal tibiofibular joint, do not miss it Alexander FY van Wulfften Palthe, Linda Musters, Remko JA Sonnega, Hans A van der Sluijs Department of Orthopaedic SUMMARY TREATMENT Surgery, VU University Medical We present a case of a 45-year-old woman with a right After intra-articular infiltration of anaesthetic in the Center, Amsterdam, fi fi fi The Netherlands proximal tibio bular dislocation she sustained after a fall proximal tibio bular joint, the bular head was during roller skating. Anteroposterior and lateral reduced by direct manipulation in anterior to pos- Correspondence to radiographs confirmed the diagnosis; there were no terior direction with the knee in 90° of flexion. Dr Hans A van der Sluijs, other injuries. The dislocation was reduced by direct A radiograph following reduction showed an [email protected] manipulation after intra-articular infiltration, in our anatomical proximal tibiofibular joint (figure 2). Accepted 4 November 2015 emergency department. The patient was treated with a The patient was discharged with a long leg cast, long, non-weight bearing leg cast for 1 week. After non-weight bearing. 4 weeks, she had no pain and a full range of motion of the knee. OUTCOME AND FOLLOW-UP After 1 week, the cast was removed and the patient started with protected weight bearing. After BACKGROUND 4 weeks, she was able to bear full weight, and had a fi A traumatic dislocation of the proximal tibio bular full range of motion and no pain. -

Bilateral Carpometacarpal Joint Dislocations of the Thumb Changhoon Jeong, MD, Hyoung-Min Kim, MD, Sang-Uk Lee, MD, Il-Jung Park, MD
Case Report Clinics in Orthopedic Surgery 2012;4:246-248 • http://dx.doi.org/10.4055/cios.2012.4.3.246 Bilateral Carpometacarpal Joint Dislocations of the Thumb Changhoon Jeong, MD, Hyoung-Min Kim, MD, Sang-Uk Lee, MD, Il-Jung Park, MD Department of Orthopaedic Surgery, Bucheon St. Mary’s Hospital, The Catholic University of Korea School of Medicine, Bucheon, Korea A traumatic carpometacarpal joint dislocation of the thumb accounts for less than 1% of all hand injuries. Optimal treatment strategies for this injury are still a subject of debate. In this article, we report a case of bilateral thumb carpometacarpal joint dis- locations: a unique combination of injuries. We believe our case is the second report of bilateral carpometacarpal joint dislocation regarding the thumb in English literature. It was successfully treated with closed reduction and percutaneous K-wires fixation on one side, and an open reduction and reconstruction of the ligament on the other side. Keywords: Bilateral, Carpometacarpal joint, Dislocation, Thumb A carpometacarpal joint (CMCJ) of the thumb is impor- a result of a motorbike accident. At the time of impact, tant for the function of the thumb and in the performance he was firmly grasping the handlebars with both hands. regarding strong pinch and grasp. The dislocation of the A physical examination revealed severe tenderness and CMCJ in the thumb accounts for less than 1% of all hand dorsal prominence at the CMCJ regarding both thumbs. injuries.1) Mechanical instability for the CMCJ of the There were no neurovascular injuries or skin lesions. The thumb is an important factor, which may lead to articu- radiographs showed dorsal dislocation of the CMCJ for lar degeneration of the joint and thus interfere with the both thumbs with a tiny fracture fragment in the right normal function of the hand. -

Degloving and Severe Upper Extremity Injuries in Motor Vehicle Crashes Involving Partial Ejection"
"Degloving and Severe Upper Extremity Injuries in Motor Vehicle Crashes Involving Partial Ejection" Seattle CIREN University of Washington, Harborview Medical Center, Seattle WA Kaufman R., Blanar L., Bulger E. –Seattle CIREN, UW, HMC Lipira A., Friedrickson J. – Harborview Medical Center Mastrioanni S., Nelson M. –Seattle CIREN Upper Extremity (UE) Partial Ejection in Motor Vehicle Crashes (MVC) • Noted as an ‘arm‐ or hand‐out‐ window’ phenomenon • Upper extremity partial ejection in MVCs can result in contact to exterior objects, including the ground in rollovers, which can result in severe degloving type injuries • These severe injuries result in devastating and long‐lasting consequences J Trauma Acute Care Surg. 2013 Feb;74(2):687‐91. Vehicle factors and outcomes associated with hand‐out‐window motor vehicle collisions. Bakker A1, Moseley J, Friedrich J. Partial Ejection Mitigation • Seatbelts are 99.8% effective at preventing complete ejections, but only 38% effective in preventing partial ejections in rollover crashes • Side‐curtain airbags (SABs) can reduced and mitigated risk of partial ejection • BUT, most partial ejection research focuses on head or thoracic injuries • Partial ejection of the upper extremity (UE) remains a highly morbid mechanism of upper extremity injury in motor vehicle collisions References: 1. Bakker, A., Moseley, J. & Friedrich, J. Vehicle factors and outcomes associated with hand‐out‐window motor vehicle collisions. Journal of Trauma and Acute Care Surgery 74, 687–691 (2013). 2. Ball, C. G., Rozycki, G. S. & Feliciano, D. V. Upper Extremity Amputations After Motor Vehicle Rollovers. The Journal of Trauma: Injury, Infection, and Critical Care 67, 410–412 (2009). 3. Nikitins, M. -
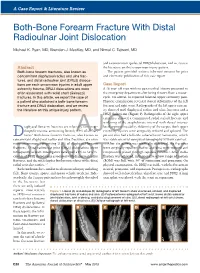
Both-Bone Forearm Fracture with Distal Radioulnar Joint Dislocation
A Case Report & Literature Review Both-Bone Forearm Fracture With Distal Radioulnar Joint Dislocation Michael K. Ryan, MD, Brendan J. MacKay, MD, and Nirmal C. Tejwani, MD and a concomitant ipsilateral DRUJ dislocation, and we review Abstract the literature on this uncommon injury pattern. Both-bone forearm fractures, also known as The patient provided written informed consent for print concomitant diaphyseal radius and ulna frac- and electronic publication of this case report. tures, and distal radioulnar joint (DRUJ) disloca- tions are each uncommon injuries in adult upper Case Report extremity trauma. DRUJ dislocations are more A 38-year-old man with no past medical history presented to often associated with radial shaft (Galeazzi) the emergency department after being thrown from a motor- fractures. In this article, we report the case of cycle. On arrival, he reported bilateral upper extremity pain. a patient who sustained a both-bone forearm Physical examination revealed closed deformities of the left fracture and DRUJ dislocation, and we review forearm and right wrist. Radiographs of the left upper extrem- the literature on this unique injury pattern. ity showed mid-diaphyseal radius and ulna fractures and a DRUJ dislocation (Figure 1). Radiographs of the right upper extremity showed a comminuted radial styloid fracture and widening of the scapholunate interval with dorsal interca- iaphyseal forearm fractures are relatively rare in or- lated segment instability deformity of the carpus. Both upper thopedic trauma, accounting for only 0.9% of all frac- extremity injuries were acceptably reduced and splinted. The 1 AJO Dtures. Both-bone forearm fractures, also known as patient also had a left-side subarachnoid hematoma, which concomitant diaphyseal radius and ulna fractures, are even was stable on serial computed tomography without contrast. -

Cervical Spine Injury Guest Lecture Delivered During the International Conference on Cervical Spine Held at NIMHANS on September 12, 1986
Article NIMHANS Journal Cervical Spine Injury Guest lecture delivered during the international Conference on Cervical Spine held at NIMHANS on September 12, 1986. Volume: 05 Issue: 01 January 1987 Page: 1-12 Phillip Harris, - Department of Surgical Neurology, Western General Hospital, Edinburgh, Scotland There is no doubt that serious injuries to the cervical spine is one of the major and most devastating health care problems that besets man, affecting so many body systems and necessitating the involvement of many public services and medical and other specialists. The patient's whole life may quite suddenly become disrupted, with permanent personal, family and employment problems. Maximal vertebral column deformity and associated neural and vascular damage usually occurs at the time of the injury. The appreciation, organisation and harnessing of proper resources for traumatic tetraplegic patients is indeed a challenge. The study and management of traumatic tetraplegia is a microcosm of the overall scientific and humanitarian progress of man [1], [2], [3], [4], [5], [6]. As noted by Edwin Smith in the medical writings of the Egyptians some 6,000 years ago, there is a phrase concerning spinal cord injuries: "an ailment not to be treated". This was understandable, because death was the immediate or the early outcome of such injuries - how times have changed! My aim today is to highlight some of the current medical aspects of patients with severe cervical spinal injury. Our interest and responsibility is firstly to try to prevent such injuries from occurring, but having occurred, to ensure that the patient is expertly managed, and this includes maintaining the cervical spinal cord, nerves and vessels in an optimal environment to allow neurological functions to recover maximally, to prevent complications and to permit the best possible future life for the patient. -

Spinal Cord Injury and Compression
Page 1 of 10 View this article online at: patient.info/doctor/spinal-cord-injury-and-compression Spinal Cord Injury and Compression See also the separate article on Whiplash and Cervical Spine Injury. Acute spinal cord compression is a neurosurgical emergency. Rapid diagnosis and management are essential to have the highest chances of preventing permanent loss of function. The spinal cord extends from the base of the skull and terminates near the lower margin of the L1 vertebral body. Below L1, the spinal canal contains the lumbar, sacral and coccygeal spinal nerves that comprise the cauda equina. Therefore, injuries below L1 involve the segmental spinal nerves and/or cauda equina. Injuries above the termination of the spinal cord at L1 often involve both spinal cord lesions and segmental root or spinal nerve injuries. The incidence of traumatic spinal cord injury in Western Europe is about 16 per million.[1] Spinal cord injury in children is relatively rare.[2] A traumatic spinal cord injury is a lesion of neural elements of the spinal cord that can result in any degree of sensory and motor deficit, and autonomic or bowel dysfunction.[3] Spinal cord injuries may be primary or secondary: Primary injuries arise from a variety of mechanisms, including mechanical disruption, transection, penetrating injuries due to bullets or weapons, vertebral fracture/subluxation or displaced bony fragments causing penetrating spinal cord and/or segmental spinal nerve injuries. The primary traumatic impact initiates vascular and chemical processes leading to oedema and ischaemia which can lead to secondary injuries. Further cord insult can occur through subsequent inappropriate manual handling following trauma. -

STABILISATION of POSTERIOR STERNOCLAVICULAR Clinical Anatomy.2002.15.139-142 Repaired in Childhood Have Been Reported As Associated 5
East African Orthopaedic Journal Original article East African Orthopaedic Journal be marvelous. This case displayed associated congenital 4. Boon JM: Potgieter D: Van Jaarsveld Z et al. Congential anomalies. The congenital cleft lip and palate that were Undescended Scapula (Sprengel Deformity): A case study. STABILISATION OF POSTERIOR STERNOCLAVICULAR Clinical Anatomy.2002.15.139-142 repaired in childhood have been reported as associated 5. Dilli A, Ayaz, U. Y., Damar, C., et al. Sprengel Deformity: JOINT DISLOCATION USING PALMARIS LONGUS TENDON before(4).The utilized modalities of investigating this Magnetic Resonance Imaging Findings in two Pediatric AUTOGRAFT: A CASE REPORT case were plain X-rays and a 3D CT scan. The information Cases. Journal of Clinical Imaging Sci. 2011. 1. 1. 17-20 6. Cavendish, M. E. Congenital Elevation of the Scapula. J. obtained from these was deemed adequate for the V.M. Mutiso*, MBChB(UON), MMed(Surg) (UON), Fellow (arthroscopy and arthroplasty) (UK), Fellow AO-International (Ger), Bone joint Surg. Br. 1972. 54B. 3.395-408 V. M. Mutiso*, Department of Orthopaedic Surgery, College of Health Sciences, University of Nairobi, (P.O. Box FCS (ecsa), Department of Orthopaedic Surgery, College of Health Sciences, University of Nairobi, P.O. Box 19681 - 00202, treatment planning of this case. No new information 7. Green, W. T. The surgical correction of congenital elevation Nairobi,19681 – Kenya 00202, and Nairobi, J. Chigumbura, Kenya and MBChB J. Chigumbura (UK), GPST1 (UK), GPST1 - University – University Hospital Hospital of North of Stanffordshire, North Stafford UK shire, UK would have been availed by conducting an MRI of the scapula (Sprengel’s deformity). -

SELF ASSESSMENT ANSWERS Congenital Renal Anomaly in A
Postgrad Med J 2003;79:359–362 359 to 10 years. The mode of spread of intramed- Postgrad Med J: first published as 10.1136/pmj.79.932.359 on 1 June 2003. Downloaded from SELF ASSESSMENT ANSWERS ullary cysticercosis is either haematogenous or ventriculoependymal.2 MRI studies help in diagnosing and correctly correlating the Congenital renal anomaly number of cases the band of renal tissue may 4 pathological diagnosis of neurocysticercosis evade ultrasonic detection. Computed tom- 3 in a patient with situs ography may be necessary to confirm the (including intramedullary cysticercosis). inversus diagnosis. Treatment modalities like drug therapy Intervention is required because of obstruc- (cysticidal drug)/surgery, or both, can be Q1: Name the congenital renal tion or calculi. The combination of horseshoe planned according to the pathological stage kidney with an aortic aneurysm presents a and location of the cyst as seen on MRI. Since anomaly identified in fig 1 (see p 355) the cysticidal drugs albendazole and Horseshoe kidney. The lower poles of the kid- diagnostic and therapeutic challenge to the vascular surgeon.5 praziquental were shown to be effective in ney being displaced towards the midline, parenchymal brain cysticercosis, these drugs joined by either functioning renal tissue or a Final diagnosis have been considered potentially useful in fibrous band. patients with intramedullary cysticercosis. Horseshoe kidney with situs inversus. Successful management of intramedullary Q2: What is the incidence and sex cysticercosis by cysticidal drugs alone has also ratio of this anomaly? References been reported in the literature.4 Incidence is one in 400. It is more commonly 1 Bauer SB, Perlmutter AD, Retik AB. -

Missed and Mismanaged Injuries of the Spinal Cord Pradeep Matthew Poonnoose, MS(Orth), Ganapathiraju Ravichandran, FRCS, and Martin Raymond Mcclelland, FRCS
The Journal of TRAUMA Injury, Infection, and Critical Care Missed and Mismanaged Injuries of the Spinal Cord Pradeep Matthew Poonnoose, MS(Orth), Ganapathiraju Ravichandran, FRCS, and Martin Raymond McClelland, FRCS Objective: The purpose of this study tients with no neurologic deficits were ex- associated injuries, and radiographic was to determine the incidence of missed cluded from the study. errors. and mismanaged injuries of the spinal Results: Of the 569 patients, the di- Conclusion: Despite a greater aware- cord, to identify factors contributing to a agnosis of spinal cord injury was missed in ness of the potential for spinal injury after failure to recognize such injuries, and to 52 instances (9.1%). The patients were road traffic accidents, failure to recognize assess the consequences of such failures. mismanaged in 34 instances, and the a spinal cord injury in the acute care set- Methods: Missed and mismanaged treatment offered to 30 was considered ting appears to be increasing. Injuries are injuries were defined using previously val- negligent. In 26 of 52 (50%), mismanage- seldom missed because of an isolated idated statements. All medical records ment resulted in neurologic deterioration. cause, but rather because of a combina- and radiographs of patients with acute The study identified several factors that tion of several factors. Increased vigilance traumatic spinal cord injury admitted to contributed to a failure to recognize a spi- on the part of the primary care physicians the Regional Spinal Cord Injury Unit in nal cord injury. These include ambience and careful documentation may reduce al- Sheffield, United Kingdom, over a period and circumstances surrounding the in- legations of medical negligence.