Summarized by © Lakhasly.Com • Remove the Cloth When Bleeding
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The National Drugs List
^ ^ ^ ^ ^[ ^ The National Drugs List Of Syrian Arab Republic Sexth Edition 2006 ! " # "$ % &'() " # * +$, -. / & 0 /+12 3 4" 5 "$ . "$ 67"5,) 0 " /! !2 4? @ % 88 9 3: " # "$ ;+<=2 – G# H H2 I) – 6( – 65 : A B C "5 : , D )* . J!* HK"3 H"$ T ) 4 B K<) +$ LMA N O 3 4P<B &Q / RS ) H< C4VH /430 / 1988 V W* < C A GQ ") 4V / 1000 / C4VH /820 / 2001 V XX K<# C ,V /500 / 1992 V "!X V /946 / 2004 V Z < C V /914 / 2003 V ) < ] +$, [2 / ,) @# @ S%Q2 J"= [ &<\ @ +$ LMA 1 O \ . S X '( ^ & M_ `AB @ &' 3 4" + @ V= 4 )\ " : N " # "$ 6 ) G" 3Q + a C G /<"B d3: C K7 e , fM 4 Q b"$ " < $\ c"7: 5) G . HHH3Q J # Hg ' V"h 6< G* H5 !" # $%" & $' ,* ( )* + 2 ا اوا ادو +% 5 j 2 i1 6 B J' 6<X " 6"[ i2 "$ "< * i3 10 6 i4 11 6! ^ i5 13 6<X "!# * i6 15 7 G!, 6 - k 24"$d dl ?K V *4V h 63[46 ' i8 19 Adl 20 "( 2 i9 20 G Q) 6 i10 20 a 6 m[, 6 i11 21 ?K V $n i12 21 "% * i13 23 b+ 6 i14 23 oe C * i15 24 !, 2 6\ i16 25 C V pq * i17 26 ( S 6) 1, ++ &"r i19 3 +% 27 G 6 ""% i19 28 ^ Ks 2 i20 31 % Ks 2 i21 32 s * i22 35 " " * i23 37 "$ * i24 38 6" i25 39 V t h Gu* v!* 2 i26 39 ( 2 i27 40 B w< Ks 2 i28 40 d C &"r i29 42 "' 6 i30 42 " * i31 42 ":< * i32 5 ./ 0" -33 4 : ANAESTHETICS $ 1 2 -1 :GENERAL ANAESTHETICS AND OXYGEN 4 $1 2 2- ATRACURIUM BESYLATE DROPERIDOL ETHER FENTANYL HALOTHANE ISOFLURANE KETAMINE HCL NITROUS OXIDE OXYGEN PROPOFOL REMIFENTANIL SEVOFLURANE SUFENTANIL THIOPENTAL :LOCAL ANAESTHETICS !67$1 2 -5 AMYLEINE HCL=AMYLOCAINE ARTICAINE BENZOCAINE BUPIVACAINE CINCHOCAINE LIDOCAINE MEPIVACAINE OXETHAZAINE PRAMOXINE PRILOCAINE PREOPERATIVE MEDICATION & SEDATION FOR 9*: ;< " 2 -8 : : SHORT -TERM PROCEDURES ATROPINE DIAZEPAM INJ. -

Classification of Medicinal Drugs and Driving: Co-Ordination and Synthesis Report
Project No. TREN-05-FP6TR-S07.61320-518404-DRUID DRUID Driving under the Influence of Drugs, Alcohol and Medicines Integrated Project 1.6. Sustainable Development, Global Change and Ecosystem 1.6.2: Sustainable Surface Transport 6th Framework Programme Deliverable 4.4.1 Classification of medicinal drugs and driving: Co-ordination and synthesis report. Due date of deliverable: 21.07.2011 Actual submission date: 21.07.2011 Revision date: 21.07.2011 Start date of project: 15.10.2006 Duration: 48 months Organisation name of lead contractor for this deliverable: UVA Revision 0.0 Project co-funded by the European Commission within the Sixth Framework Programme (2002-2006) Dissemination Level PU Public PP Restricted to other programme participants (including the Commission x Services) RE Restricted to a group specified by the consortium (including the Commission Services) CO Confidential, only for members of the consortium (including the Commission Services) DRUID 6th Framework Programme Deliverable D.4.4.1 Classification of medicinal drugs and driving: Co-ordination and synthesis report. Page 1 of 243 Classification of medicinal drugs and driving: Co-ordination and synthesis report. Authors Trinidad Gómez-Talegón, Inmaculada Fierro, M. Carmen Del Río, F. Javier Álvarez (UVa, University of Valladolid, Spain) Partners - Silvia Ravera, Susana Monteiro, Han de Gier (RUGPha, University of Groningen, the Netherlands) - Gertrude Van der Linden, Sara-Ann Legrand, Kristof Pil, Alain Verstraete (UGent, Ghent University, Belgium) - Michel Mallaret, Charles Mercier-Guyon, Isabelle Mercier-Guyon (UGren, University of Grenoble, Centre Regional de Pharmacovigilance, France) - Katerina Touliou (CERT-HIT, Centre for Research and Technology Hellas, Greece) - Michael Hei βing (BASt, Bundesanstalt für Straßenwesen, Germany). -

Tranexamic Acid in the Treatment of Residual Chronic Subdural Hematoma: a Single-Centre, Observer-Blinded, Randomized Controlled Trial (Trace)
TRANEXAMIC ACID IN THE TREATMENT OF RESIDUAL CHRONIC SUBDURAL HEMATOMA: A SINGLE-CENTRE, OBSERVER-BLINDED, RANDOMIZED CONTROLLED TRIAL (TRACE) by Adriana Micheline Workewych A thesis submitted in conformity with the requirements for the degree of Master of Science Institute of Medical Science University of Toronto © Copyright by Adriana Micheline Workewych 2018 TRANEXAMIC ACID IN THE TREATMENT OF RESIDUAL CHRONIC SUBDURAL HEMATOMA: A SINGLE-CENTRE, OBSERVER-BLINDED, RANDOMIZED CONTROLLED TRIAL (TRACE) Adriana Micheline Workewych Master of Science Institute of Medical Science University of Toronto 2018 ABSTRACT Chronic subdural hematoma (CSDH) is a frequent consequence of head trauma, particularly in older individuals. Given the aging of populations globally, its incidence is projected to increase substantially. Hyperfibrinolysis may be central to CSDH enlargement by causing excessive clot degradation and liquefaction, impeding resorption. The only current standard treatment for CSDH is surgery, however, up to 31% of residual hematomas enlarge, requiring reoperation. Tranexamic acid (TXA), an antifibrinolytic medication that prevents excessively rapid clot breakdown, may help prevent CSDH enlargement, potentially eliminating the need for repeat surgery. To evaluate the feasibility of conducting a trial investigating TXA efficacy in residual CSDH, we conducted an observer-blinded, pilot randomized controlled trial (RCT). We showed this trial was feasible and safe, reporting only minor to moderate AEs, and an attrition rate of 4%. The results from this study will inform the conduct of a double-blinded RCT investigating TXA efficacy in post-operative CSDH management. ii ACKNOWLEDGEMENTS First, I would like to thank my supervisor Dr. Michael Cusimano, my mentor for nearly six years. You have always given me more opportunity than I could have ever hoped for – I could not ask for a more dedicated teacher. -

No Benefit of Hemostatic Drugs on Acute Upper Gastrointestinal Bleeding in Cirrhosis
Hindawi BioMed Research International Volume 2020, Article ID 4097170, 11 pages https://doi.org/10.1155/2020/4097170 Research Article No Benefit of Hemostatic Drugs on Acute Upper Gastrointestinal Bleeding in Cirrhosis Yang An,1,2 Zhaohui Bai,1,2 Xiangbo Xu,1,2 Xiaozhong Guo ,1 Fernando Gomes Romeiro ,3 Cyriac Abby Philips,4 Yingying Li,5 Yanyan Wu,1,6 and Xingshun Qi 1 1Department of Gastroenterology, General Hospital of Northern Theater Command (formerly General Hospital of Shenyang Military Area), Shenyang 110840, China 2Postgraduate College, Shenyang Pharmaceutical University, Shenyang 110016, China 3Department of Internal Medicine, Botucatu Medical School, UNESP-Univ Estadual Paulista. Av. Prof. Mário Rubens Guimarães Montenegro, s/n Distrito de Rubião Jr, Botucatu, Brazil 4The Liver Unit and Monarch Liver Lab, Cochin Gastroenterology Group, Ernakulam Medical Center, Kochi, 682028 Kerala, India 5Department of Gastroenterology, The First People’s Hospital of Huainan, Huainan 232007, China 6Postgraduate College, Jinzhou Medical University, Jinzhou 121001, China Correspondence should be addressed to Xingshun Qi; [email protected] Received 28 February 2020; Revised 25 May 2020; Accepted 1 June 2020; Published 27 June 2020 Academic Editor: Hongqun Liu Copyright © 2020 Yang An et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Background and Aims. Acute upper gastrointestinal bleeding (AUGIB) is one of the most life-threatening emergency conditions. Hemostatic drugs are often prescribed to control AUGIB in clinical practice but have not been recommended by major guidelines and consensus. -

Blood Modifier Agents Policy #: Rx.01.208
Pharmacy Policy Bulletin Title: Blood Modifier Agents Policy #: Rx.01.208 Application of pharmacy policy is determined by benefits and contracts. Benefits may vary based on product line, group, or contract. Some medications may be subject to precertification, age, quantity, or formulary restrictions (ie limits on non-preferred drugs). Individual member benefits must be verified. This pharmacy policy document describes the status of pharmaceutical information and/or technology at the time the document was developed. Since that time, new information relating to drug efficacy, interactions, contraindications, dosage, administration routes, safety, or FDA approval may have changed. This Pharmacy Policy will be regularly updated as scientific and medical literature becomes available. This information may include new FDA-approved indications, withdrawals, or other FDA alerts. This type of information is relevant not only when considering whether this policy should be updated, but also when applying it to current requests for coverage. Members are advised to use participating pharmacies in order to receive the highest level of benefits. Intent: The intent of this policy is to communicate the medical necessity criteria for eltrombopag olamine (Promacta®), fostamatinib disodium (Tavalisse™), avatrombopag (Doptelet®), lusutrombopag (Mulpleta®) as provided under the member's prescription drug benefit. Description: Idiopathic thrombocytopenia purpura (ITP): ITP is an immune disorder in which the blood doesn't clot normally. ITP can cause excessive bruising and bleeding and can be characterized as an unusually low level of platelets, or thrombocytes, in the blood results in ITP. Thrombocytopenia in patients with hepatitis C: Thrombocytopenia can occur in patients with chronic hepatitis C virus (HCV) infection. -

Drug Name Plate Number Well Location % Inhibition, Screen Axitinib 1 1 20 Gefitinib (ZD1839) 1 2 70 Sorafenib Tosylate 1 3 21 Cr
Drug Name Plate Number Well Location % Inhibition, Screen Axitinib 1 1 20 Gefitinib (ZD1839) 1 2 70 Sorafenib Tosylate 1 3 21 Crizotinib (PF-02341066) 1 4 55 Docetaxel 1 5 98 Anastrozole 1 6 25 Cladribine 1 7 23 Methotrexate 1 8 -187 Letrozole 1 9 65 Entecavir Hydrate 1 10 48 Roxadustat (FG-4592) 1 11 19 Imatinib Mesylate (STI571) 1 12 0 Sunitinib Malate 1 13 34 Vismodegib (GDC-0449) 1 14 64 Paclitaxel 1 15 89 Aprepitant 1 16 94 Decitabine 1 17 -79 Bendamustine HCl 1 18 19 Temozolomide 1 19 -111 Nepafenac 1 20 24 Nintedanib (BIBF 1120) 1 21 -43 Lapatinib (GW-572016) Ditosylate 1 22 88 Temsirolimus (CCI-779, NSC 683864) 1 23 96 Belinostat (PXD101) 1 24 46 Capecitabine 1 25 19 Bicalutamide 1 26 83 Dutasteride 1 27 68 Epirubicin HCl 1 28 -59 Tamoxifen 1 29 30 Rufinamide 1 30 96 Afatinib (BIBW2992) 1 31 -54 Lenalidomide (CC-5013) 1 32 19 Vorinostat (SAHA, MK0683) 1 33 38 Rucaparib (AG-014699,PF-01367338) phosphate1 34 14 Lenvatinib (E7080) 1 35 80 Fulvestrant 1 36 76 Melatonin 1 37 15 Etoposide 1 38 -69 Vincristine sulfate 1 39 61 Posaconazole 1 40 97 Bortezomib (PS-341) 1 41 71 Panobinostat (LBH589) 1 42 41 Entinostat (MS-275) 1 43 26 Cabozantinib (XL184, BMS-907351) 1 44 79 Valproic acid sodium salt (Sodium valproate) 1 45 7 Raltitrexed 1 46 39 Bisoprolol fumarate 1 47 -23 Raloxifene HCl 1 48 97 Agomelatine 1 49 35 Prasugrel 1 50 -24 Bosutinib (SKI-606) 1 51 85 Nilotinib (AMN-107) 1 52 99 Enzastaurin (LY317615) 1 53 -12 Everolimus (RAD001) 1 54 94 Regorafenib (BAY 73-4506) 1 55 24 Thalidomide 1 56 40 Tivozanib (AV-951) 1 57 86 Fludarabine -

Multiple Technology Appraisal Avatrombopag and Lusutrombopag
Multiple Technology Appraisal Avatrombopag and lusutrombopag for treating thrombocytopenia in people with chronic liver disease needing an elective procedure [ID1520] Committee papers © National Institute for Health and Care Excellence 2019. All rights reserved. See Notice of Rights. The content in this publication is owned by multiple parties and may not be re-used without the permission of the relevant copyright owner. NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE MULTIPLE TECHNOLOGY APPRAISAL Avatrombopag and lusutrombopag for treating thrombocytopenia in people with chronic liver disease needing an elective procedure [ID1520] Contents: 1 Pre-meeting briefing 2 Assessment Report prepared by Kleijnen Systematic Reviews 3 Consultee and commentator comments on the Assessment Report from: • Shionogi 4 Addendum to the Assessment Report from Kleijnen Systematic Reviews 5 Company submission(s) from: • Dova • Shionogi 6 Clarification questions from AG: • Questions to Shionogi • Clarification responses from Shionogi • Questions to Dova • Clarification responses from Dova 7 Professional group, patient group and NHS organisation submissions from: • British Association for the Study of the Liver (BASL) The Royal College of Physicians supported the BASL submission • British Society of Gastroenterology (BSG) 8 Expert personal statements from: • Vanessa Hebditch – patient expert, nominated by the British Liver Trust • Dr Vickie McDonald – clinical expert, nominated by British Society for Haematology • Dr Debbie Shawcross – clinical expert, nominated by Shionogi © National Institute for Health and Care Excellence 2019. All rights reserved. See Notice of Rights. The content in this publication is owned by multiple parties and may not be re-used without the permission of the relevant copyright owner. MTA: avatrombopag and lusutrombopag for treating thrombocytopenia in people with chronic liver disease needing an elective procedure Pre-meeting briefing © NICE 2019. -
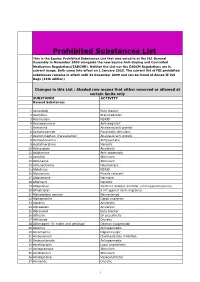
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

Management of Flood Syndrome: What Can We Do Better? Strainiene S, Peciulyte M, Strainys T, Stundiene I, Savlan I, Liakina V, Valantinas J
ISSN 1007-9327 (print) ISSN 2219-2840 (online) World Journal of Gastroenterology World J Gastroenterol 2021 August 28; 27(32): 5297-5459 Published by Baishideng Publishing Group Inc World Journal of W J G Gastroenterology Contents Weekly Volume 27 Number 32 August 28, 2021 OPINION REVIEW 5297 Management of Flood syndrome: What can we do better? Strainiene S, Peciulyte M, Strainys T, Stundiene I, Savlan I, Liakina V, Valantinas J REVIEW 5306 Radiomics and machine learning applications in rectal cancer: Current update and future perspectives Stanzione A, Verde F, Romeo V, Boccadifuoco F, Mainenti PP, Maurea S 5322 Could the burden of pancreatic cancer originate in childhood? Diaconescu S, Gîlcă-Blanariu GE, Poamaneagra S, Marginean O, Paduraru G, Stefanescu G MINIREVIEWS 5341 Application of artificial intelligence in preoperative imaging of hepatocellular carcinoma: Current status and future perspectives Feng B, Ma XH, Wang S, Cai W, Liu XB, Zhao XM 5351 Artificial intelligence application in diagnostic gastrointestinal endoscopy - Deus ex machina? Correia FP, Lourenço LC 5362 Faecal microbiota transplantation enhances efficacy of immune checkpoint inhibitors therapy against cancer Kang YB, Cai Y 5376 Immune checkpoint inhibitor-related hepatotoxicity: A review Remash D, Prince DS, McKenzie C, Strasser SI, Kao S, Liu K ORIGINAL ARTICLE Basic Study 5392 Therapeutic effect of Cistanche deserticola on defecation in senile constipation rat model through stem cell factor/C-kit signaling pathway Zhang X, Zheng FJ, Zhang Z 5404 Recombinant angiopoietin-like -

Drug and Medication Classification Schedule
KENTUCKY HORSE RACING COMMISSION UNIFORM DRUG, MEDICATION, AND SUBSTANCE CLASSIFICATION SCHEDULE KHRC 8-020-1 (11/2018) Class A drugs, medications, and substances are those (1) that have the highest potential to influence performance in the equine athlete, regardless of their approval by the United States Food and Drug Administration, or (2) that lack approval by the United States Food and Drug Administration but have pharmacologic effects similar to certain Class B drugs, medications, or substances that are approved by the United States Food and Drug Administration. Acecarbromal Bolasterone Cimaterol Divalproex Fluanisone Acetophenazine Boldione Citalopram Dixyrazine Fludiazepam Adinazolam Brimondine Cllibucaine Donepezil Flunitrazepam Alcuronium Bromazepam Clobazam Dopamine Fluopromazine Alfentanil Bromfenac Clocapramine Doxacurium Fluoresone Almotriptan Bromisovalum Clomethiazole Doxapram Fluoxetine Alphaprodine Bromocriptine Clomipramine Doxazosin Flupenthixol Alpidem Bromperidol Clonazepam Doxefazepam Flupirtine Alprazolam Brotizolam Clorazepate Doxepin Flurazepam Alprenolol Bufexamac Clormecaine Droperidol Fluspirilene Althesin Bupivacaine Clostebol Duloxetine Flutoprazepam Aminorex Buprenorphine Clothiapine Eletriptan Fluvoxamine Amisulpride Buspirone Clotiazepam Enalapril Formebolone Amitriptyline Bupropion Cloxazolam Enciprazine Fosinopril Amobarbital Butabartital Clozapine Endorphins Furzabol Amoxapine Butacaine Cobratoxin Enkephalins Galantamine Amperozide Butalbital Cocaine Ephedrine Gallamine Amphetamine Butanilicaine Codeine -

Nutrition and Blood
Greater Manchester Joint Formulary Chapter 9: Nutrition and Blood For cost information please go to the most recent cost comparison charts Contents 9.1. Anaemias and some other blood disorders 9.2 Fluids and electrolytes 9.3 Not listed 9.4. Oral nutrition 9.5 Minerals 9.6 Vitamins Key Red drug see GMMMG RAG list Click on the symbols to access this list Amber drug see GMMMG RAG list Click on the symbols to access this list Green drug see GMMMG RAG list Click on the symbols to access this list If a medicine is unlicensed this should be highlighted in the template as follows Drug name Not Recommended OTC Over the Counter In line with NHS England guidance, GM do not routinely support prescribing for conditions which are self-limiting or amenable to self-care. For further details see GM commissioning statement. Order of Drug Choice Where there is no preferred 1st line agent provided, the drug choice appears in alphabetical order. Return to contents Chapter 9 – page 1 of 16 V5.2 Greater Manchester Joint Formulary BNF chapter 9 Nutrition and Blood Section 9.1. Anaemias and some other blood disorders Subsection 9.1.1 Iron-deficiency anaemias Subsection 9.1.1.1 Oral iron First choice Ferrous fumarate 322 mg tabs (100 mg iron) Ferrous fumarate 305 mg caps (100 mg iron) Alternatives Ferrous fumarate 210 mg tabs (68 mg iron) Ferrous sulphate 200 mg tabs (65 mg iron) Ferrous fumarate 140 mg sugar free syrup (45 mg of iron/5 mL) Sodium feredetate 190 mg sugar free elixir (27.5 mg of iron/5 mL) Grey drugs Ferric maltol capsules Items which Criterion 2 (see RAG list) are listed as For treatment of iron deficiency anaemia in patients with Grey are intolerance to, or treatment failure with, two oral iron deemed not supplements. -

Doptelet® (Avatrombopag) (Oral) Document Number: IC-0369 Last Review Date: 02/04/2020 Date of Origin: 07/03/2018 Dates Reviewed: 07/2018, 02/2019, 08/2019, 02/2020
Doptelet® (avatrombopag) (Oral) Document Number: IC-0369 Last Review Date: 02/04/2020 Date of Origin: 07/03/2018 Dates Reviewed: 07/2018, 02/2019, 08/2019, 02/2020 I. Length of Authorization Thrombocytopenia due to CLD Coverage is provided for one 5-day course of therapy and may not be renewed. Chronic ITP Coverage is provided for three months and may be renewed. II. Dosing Limits A. Quantity Limit (max daily dose) [NDC unit]: 20 mg tablets: 3 tablets per day B. Max Units (per dose and over time) [HCPCS Unit]: Thrombocytopenia 60 mg daily Chronic ITP 40 mg daily III. Initial Approval Criteria1 Coverage is provided in the following conditions: Universal Criteria Patient age 18 years or older; AND Patient is not on any other thrombopoietin receptor agonist or mimetic (e.g., romiplostim, eltrombopag, lusutrombopag, etc.) or fostamtinib; AND Avatrombopag is not being used to attempt to normalize platelet count; AND Laboratory values are current (i.e., drawn within the previous 28 days); AND Thrombocytopenia due to Chronic Liver Disease (CLD) † Proprietary & Confidential © 2020 Magellan Health Inc. Patient is scheduled to undergo a procedure with a risk of bleeding which would necessitate a platelet transfusion; AND Patient will not be undergoing any of the following procedures: Neurosurgical intervention; Thoracotomy; Laparotomy; Organ resection; AND The patient is at increased risk for bleeding as indicated by platelet count of less than < 50 x 109/L Chronic Immune Thrombocytopenia (ITP) † Patient has had chronic ITP for